Rheumatoid arthritis
Reading File
Asking for Preferences
Finding Sources
Searching PubMed
"rheumatoid arthritis"[MeSH Terms] AND "drug therapy"[MeSH Terms]
Finding Sources
Searching PubMed
"rheumatoid arthritis" AND treatment
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Loading Image
Reading File
I now have comprehensive, high-quality content from Goldman-Cecil Medicine and Textbook of Family Medicine. I can compile a thorough answer.
Rheumatoid Arthritis: Management & Treatment
Treatment Goals
The primary goal is clinical remission (or at minimum low disease activity), assessed by ACR/EULAR criteria. When treated early, remission is achievable in >50% of patients and low disease activity in at least another 35%. Therapy must be escalated rapidly — if insufficient improvement (<50% reduction in disease activity) is seen after 3 months, the plan should be changed. Sustained remission is defined as ≥6 months.
All RA patients should receive a DMARD — this is non-negotiable. Three categories of drugs are used:
- NSAIDs (symptom relief only)
- Glucocorticoids (bridge/adjunct)
- DMARDs — conventional (csDMARDs), biologic (bDMARDs), and targeted synthetic (tsDMARDs)
Management Algorithm
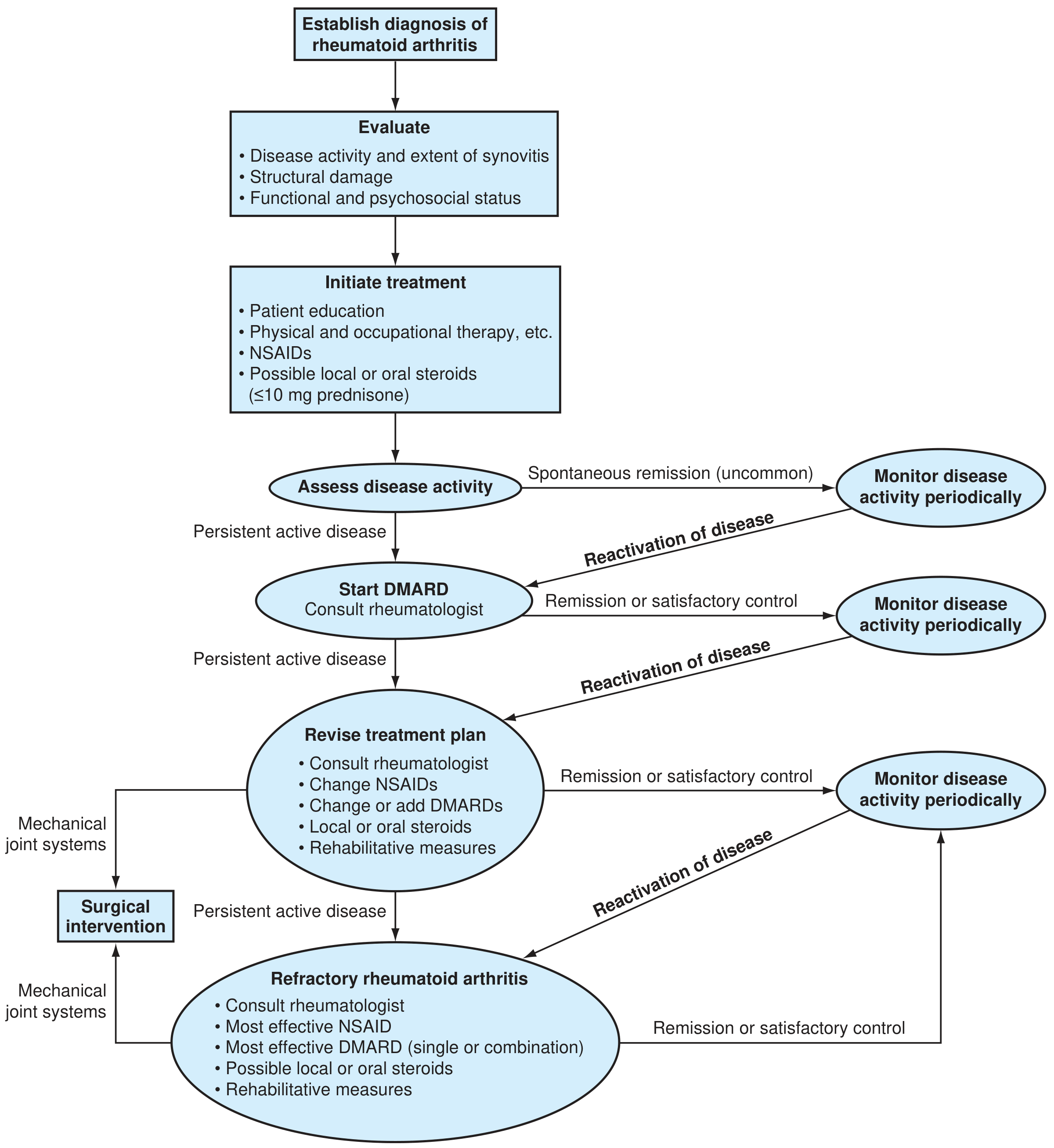
Figure: Algorithm for management of rheumatoid arthritis (ACR guidelines)
1. NSAIDs
NSAIDs provide symptomatic relief only — they have minimal or no effect on the underlying disease process, cannot halt joint erosion, and should never be used as sole therapy without a DMARD.
- COX-2 selective agents (e.g., celecoxib): less GI bleeding risk, but potential cardiovascular toxicity is a concern since RA patients already have elevated CV risk. Keep at low dose.
- Add a proton pump inhibitor in all RA patients taking NSAIDs.
- Monitor for reduced renal blood flow and elevated blood pressure.
2. Glucocorticoids
Glucocorticoids provide rapid, dramatic symptomatic and anti-inflammatory effect, and significantly reduce radiographic progression — but long-term toxicity is extensive:
- ≥25% increased risk of serious infection at doses as low as 5 mg/day
- Risk doubles at 5–10 mg/day
Key principles:
- Use as bridge therapy while slower-acting DMARDs take effect (2–6 months onset)
- Prednisone ≤10 mg/day — rarely exceed this for articular manifestations
- Starting prednisone at DMARD initiation reduces erosive damage, disease activity, disability, and the need for biologic escalation at 2 years
- Taper to the lowest effective dose as soon as possible
- Intramuscular depot injections and intra-articular injections (ultrasound-guided for difficult joints) are useful for flares
- Always prescribe osteoporosis prophylaxis (bisphosphonates, unless childbearing age)
3. Conventional DMARDs (csDMARDs)
| Drug | Key Points |
|---|---|
| Methotrexate | First-line anchor DMARD for most patients. Economical, rare serious toxicity, enhances all other DMARDs. Start 7.5–15 mg/week PO, can escalate to 25 mg/week SC/IM. Add folic acid 1 mg/day to reduce mouth sores. Monitor CBC + AST/ALT every 8–12 weeks. Contraindicated in pregnancy. Avoid alcohol. |
| Hydroxychloroquine | Keep dose <5.0 mg/kg/day. Annual ophthalmology exam after 5 years of therapy (retinal toxicity). |
| Sulfasalazine | 2–3 g/day in two divided doses. Check CBC + LFTs monthly for 1 month, then every 4–6 weeks. Sulfa allergy must be excluded. Widely used in Europe/Asia. |
| Leflunomide | CBC + AST/ALT every 4–8 weeks. Long half-life — cholestyramine washout needed if stopped. Contraindicated in pregnancy. |
| Azathioprine | Second- or third-line; causes bone marrow suppression. |
| Triple therapy | Methotrexate + sulfasalazine + hydroxychloroquine — most frequently used csDMARD combination per EULAR. |
The critical issue is not which DMARD to start first, but starting it early. — Goldman-Cecil Medicine
4. Biologic DMARDs (bDMARDs)
Used when csDMARDs provide inadequate response. Mandatory pre-treatment TB screening before starting any biologic.
| Class | Drugs |
|---|---|
| TNF inhibitors | Adalimumab, etanercept, infliximab, certolizumab, golimumab |
| IL-6 receptor inhibitors | Tocilizumab, sarilumab |
| T-cell co-stimulation blocker | Abatacept |
| B-cell depletion | Rituximab (anti-CD20; especially under certain conditions) |
Important caveats:
- Biologics must not be combined with each other — significantly increases infection risk
- If fever or infectious symptoms develop, stop biologic until resolved
- TNF inhibitors can precipitate CHF, demyelinating syndromes, or lupus-like syndromes
- Biosimilars (bsDMARDs) approved by EMA/FDA are interchangeable options
5. Targeted Synthetic DMARDs — JAK Inhibitors (tsDMARDs)
Oral small molecules targeting the JAK-STAT signaling pathway. Used after inadequate DMARD response.
| Drug | Dose | Notes |
|---|---|---|
| Tofacitinib | 5 mg twice daily | Effective with methotrexate; also after TNF inhibitor failure |
| Baricitinib | Varies | Superior to placebo and adalimumab in MTX-inadequate responders |
| Upadacitinib | 15 mg daily | Selective JAK1 inhibitor; effective as monotherapy or add-on |
| Filgotinib | 100–200 mg daily | Effective in MTX-inadequate or intolerant patients |
Shared toxicity concerns (all JAK inhibitors): infections (including TB), malignancies, cardiovascular events, herpes zoster reactivation. Monitor CBC and LFTs.
⚠️ Efficacy and safety of bDMARDs after JAK inhibitor failure, or JAK inhibitor after another JAK inhibitor, are not fully established.
6. Order of Therapy (EULAR 2019 Framework)
Step 1: Early RA → Start methotrexate ± short-term glucocorticoid bridge
↓ (reassess at 3 months; change if <50% improvement)
Step 2: csDMARD inadequate → Add/switch to another csDMARD (triple therapy)
OR
Add a bDMARD (TNF inhibitor, IL-6Ri, abatacept, rituximab)
OR
Add a tsDMARD (JAK inhibitor)
↓ (reassess; target remission by 6 months)
Step 3: Refractory RA → Most effective DMARD single or combination
Consider surgical intervention for mechanical joint problems
7. Non-Pharmacological Measures
- Patient education — essential at diagnosis
- Physical therapy — preserve joint function, prevent deformity
- Occupational therapy — adaptive equipment, joint protection
- Rehabilitative measures — throughout the disease course
- Surgical intervention — for persistent active disease with mechanical joint failure (synovectomy, joint replacement)
Monitoring Summary
| Drug | Key Monitoring |
|---|---|
| Methotrexate | CBC + AST/ALT every 8–12 weeks (stable dose) |
| Hydroxychloroquine | Annual ophthalmology after 5 years |
| Sulfasalazine | CBC monthly × 1 month, then every 4–6 weeks |
| Leflunomide | CBC + AST/ALT every 4–8 weeks |
| TNF inhibitors | Screen for TB; stop if any infectious symptoms |
| JAK inhibitors | CBC + LFTs; screen for TB and zoster |
| Glucocorticoids | Osteoporosis prophylaxis; taper to lowest dose |
Sources: Goldman-Cecil Medicine (International Edition) | Textbook of Family Medicine, 9e | Katzung's Basic & Clinical Pharmacology, 16e
This is a shared conversation. Sign in to Orris to start your own chat.