Treatment for myositis ossificans
Reading File
Finding Sources
Searching PubMed
"myositis ossificans" treatment management
Reading File
Reading File
Reading File
Reading File
Finding Sources
Finding Sources
Loading Image
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
I now have comprehensive information from multiple authoritative textbooks. Here is a complete summary:
Treatment of Myositis Ossificans
Myositis ossificans (MO) refers to heterotopic ossification — pathologic bone formation within muscle or soft tissue. Treatment strategy depends on whether the disease is localized/traumatic or progressive/generalized (fibrodysplasia ossificans progressiva, FOP).
Radiographic appearance (mature MO)
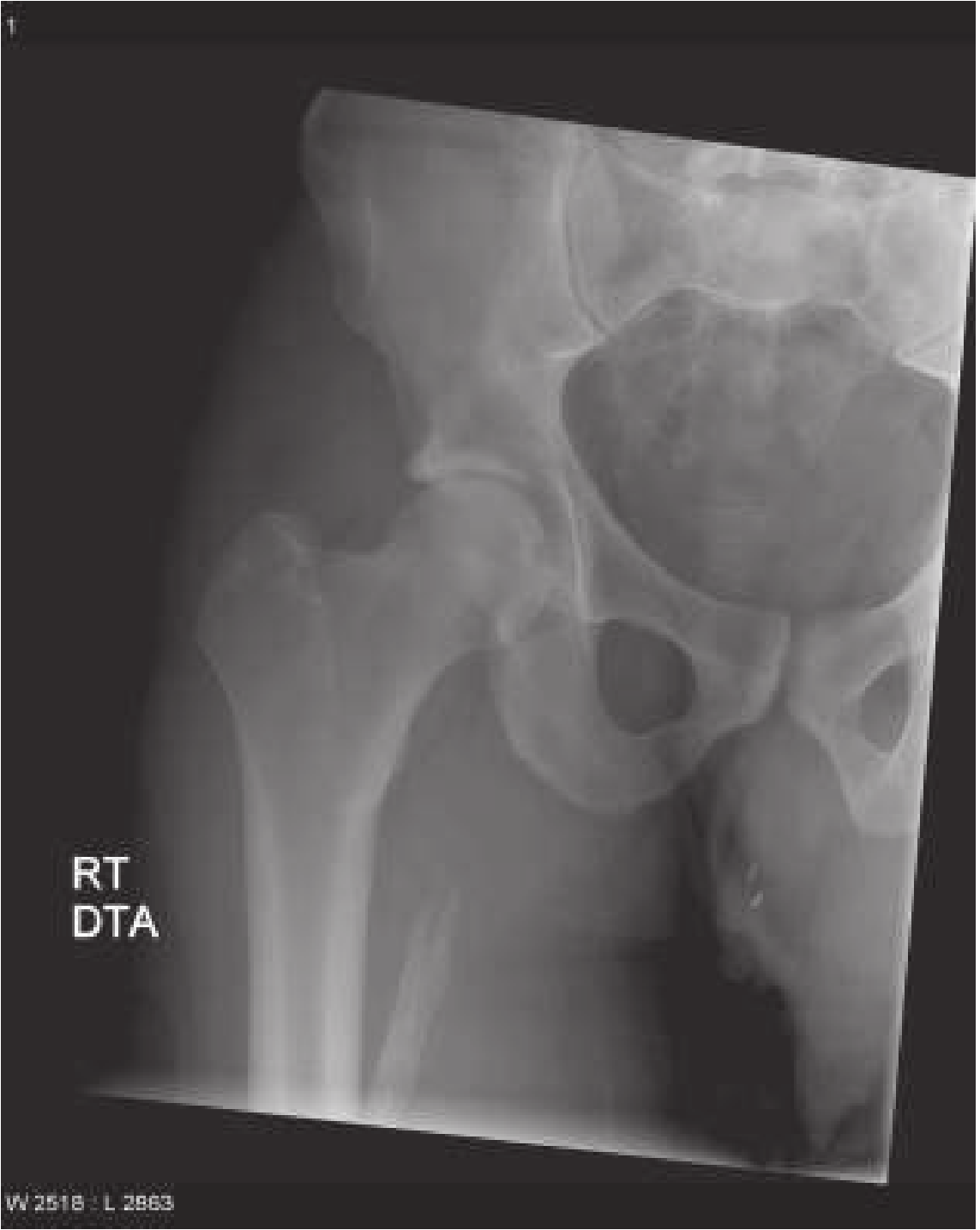
1. Localized (Traumatic) Myositis Ossificans
This form follows a single blow, muscle tear, or repetitive minor trauma. The key principle is conservative management.
Conservative (First-line)
- Activity modification / rest: The mass tends to subside spontaneously over several months if the causative activity is stopped. — Adams & Victor's Principles of Neurology, 12th ed.
- Observation is the primary recommended treatment in most orthopaedic references. — Miller's Review of Orthopaedics, 9th ed.
- NSAIDs (especially Indomethacin): Used prophylactically after high-risk trauma or surgery.
- Indomethacin 25 mg orally three times daily, or SR 75 mg once daily for 6 weeks is the standard regimen.
- Efficacy is debatable and it may increase the fracture nonunion rate — use cautiously in perioperative settings. — Miller's Review of Orthopaedics, 9th ed.
Prophylactic Radiation Therapy
For high-risk situations (e.g., post-hip arthroplasty, acetabular fractures, elbow injuries):
- 600–800 cGy (6–8 Gy) as a single fraction, given 24 hours before or up to 72 hours after surgery
- Prevents proliferation/differentiation of mesenchymal cells into osteoprogenitor cells
- Equal to indomethacin in effectiveness, with better compliance
- Preoperative radiation is preferred for patients at very high risk (e.g., Paget disease, prior MO; incidence of HO after THA in Paget disease ~50%) — Miller's Review of Orthopaedics, 9th ed.
Surgical Excision
Reserved for lesions causing specific functional disability:
- Indicated only when the lesion is mature — confirmed by radiographic evidence of sharp demarcation and trabecular pattern
- Timing: Wait at least 6–12 months after injury; for THA-related HO, delay at least 6 months
- For patients with traumatic brain injury, timing is critical: wait 3–6 months with evidence of bone maturation; recurrence after resection is likely if neurologic compromise is severe
- Treatment is excision of "problematic" HO once no further growth is evident (stable on serial radiographs, "quiet" bone scan, or >1 year from injury) — Miller's Review of Orthopaedics, 9th ed.
- Adjuvant radiation therapy after excision helps prevent recurrence — Miller's Review of Orthopaedics, 9th ed.
2. Generalized (Progressive) Myositis Ossificans — FOP
This is a rare autosomal dominant disorder (ACVR1/ALK2 activating mutation) distinct from traumatic MO.
Pharmacological
- Bisphosphonates (diphosphonates): Etidronate (EHDP, 10–20 mg/kg orally) inhibits calcium phosphate deposition; has been reported to cause regression of new swellings and prevent calcification. — Adams & Victor's Principles of Neurology, 12th ed.
- Prednisone: Useful in calcinosis universalis (closely related condition); worth attempting given the unclear relationship. — Adams & Victor's Principles of Neurology, 12th ed.
- Palovarotene (RAR-γ agonist): Reduces new heterotopic ossification by ~60% vs. historical controls. FDA-approved in 2023 for females ≥8 years and males ≥10 years. Note: risk of premature epiphyseal closure in younger children. — Harrison's Principles of Internal Medicine, 22nd ed. (2025)
- Garetosumab (REGN2477): Anti-activin A monoclonal antibody — currently in clinical trials. — Harrison's, 22nd ed.
What NOT to do in FOP
- Surgical removal of ectopic bone is contraindicated — trauma from surgery precipitates formation of new areas of heterotopic bone
- Local anesthetic injections can trigger frozen jaw (trismus)
- Low-calcium diet, glucocorticoids, and bisphosphonates have largely been ineffective in halting progression of established ossification in FOP. — Harrison's, 22nd ed.
Key Differentiating Point for Imaging
CT helps distinguish MO from osteosarcoma:
- MO: calcification begins at the periphery, progresses inward
- Osteosarcoma: calcification begins centrally first — ROSEN's Emergency Medicine
Recent Evidence
A 2023 scoping review (PMID 38161430) on pediatric MO and a 2022 review on heterotopic ossification (PMID 35866484) provide contemporary perspectives but do not overturn the above management principles. The approval of palovarotene for FOP (2023) is the most significant recent development.
This is a shared conversation. Sign in to Orris to start your own chat.