Neuroretinitis findings are seen in
Reading File
Finding Sources
Reading File
Finding Sources
Reading File
Here is a comprehensive answer on the causes and findings of neuroretinitis:
Neuroretinitis — Causes
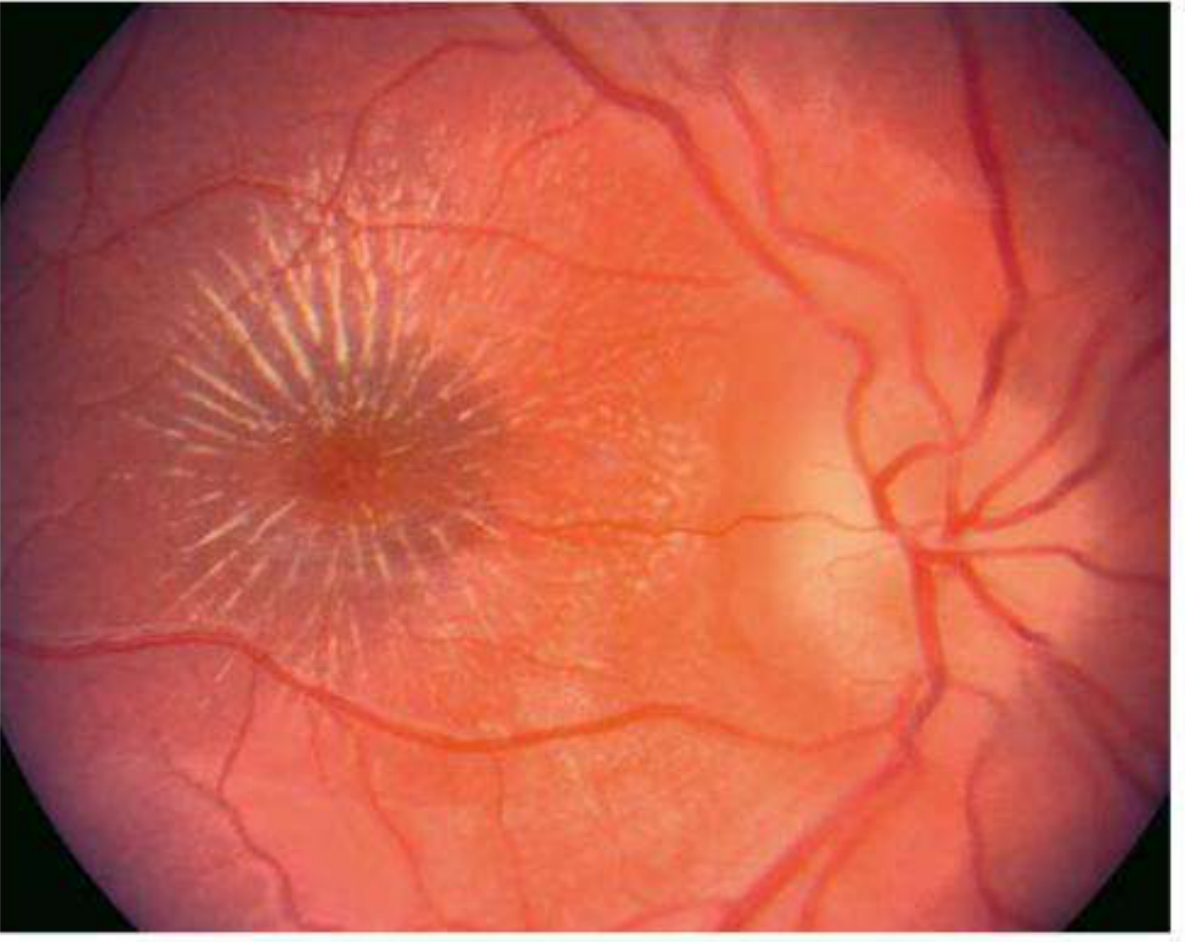
Neuroretinitis refers to the combination of optic disc inflammation (papillitis) and macular/retinal inflammation, classically producing a macular star figure.
Causes (in order of frequency)
| Cause | Notes |
|---|---|
| Cat-scratch disease (Bartonella henselae) | Most common — responsible for ~60% of cases |
| Idiopathic (Leber idiopathic stellate neuroretinitis) | ~25% of cases |
| Syphilis | Occurs during primary or secondary stages |
| Lyme disease (Borrelia burgdorferi) | Tick-borne spirochaetal infection |
| Mumps | Viral cause |
| Leptospirosis | Bacterial cause |
| Tuberculosis | Optic neuropathy including neuroretinitis |
| Toxoplasmosis | Rare association |
| Viral infections (measles, chickenpox, rubella, glandular fever) | More common in children |
Classic Findings
Symptoms:
- Painless unilateral visual impairment, gradually worsening over ~1 week
Signs:
- Papillitis with peripapillary and macular oedema
- Macular star — pathognomonic appearance; lipid exudates deposited radially in the Henle fiber layer around the fovea (appears 1–2 weeks after onset as disc swelling settles)
- Signs of optic nerve dysfunction are usually mild or absent (visual loss is largely from macular involvement)
- Venous engorgement and splinter haemorrhages in severe cases
- Occasional fellow eye involvement
Investigations:
- OCT: sub- and intraretinal fluid
- FA: diffuse leakage from superficial disc vessels
- Serology: Bartonella titres and other targeted tests
Prognosis: The macular star resolves with return to normal or near-normal vision over 6–12 months.
Key Distinguishing Point
Unlike typical optic neuritis (demyelinating), neuroretinitis carries NO increased risk of multiple sclerosis — an important clinical distinction.
The macular star is essentially never seen in demyelinating optic neuritis; its presence redirects the workup toward infectious and inflammatory causes. — Kanski's Clinical Ophthalmology, 10th ed.
Can this be seen in tension type headache
Checking Date & Time
No. Neuroretinitis is not a finding in tension-type headache (TTH).
Here's why:
-
Tension-type headache is a primary headache disorder — it is a purely functional condition with no structural, vascular, or inflammatory pathology in the eye or optic nerve. It does not cause any optic disc, retinal, or macular changes.
-
Neuroretinitis requires an underlying infectious or inflammatory process affecting the optic nerve and retina (as listed above — Bartonella, syphilis, Lyme, etc.). It is a secondary optic neuropathy, not related to headache syndromes.
-
The causes of headache in the differential that can produce optic disc/retinal changes are:
- Idiopathic intracranial hypertension (pseudotumor cerebri) → papilloedema (bilateral disc swelling), but not a macular star
- Giant cell arteritis → anterior ischaemic optic neuropathy
- Malignant hypertension → disc swelling, flame haemorrhages, exudates
None of these produce the classic disc swelling + macular star picture of neuroretinitis, and tension-type headache produces none of these findings at all.
Bottom line: Neuroretinitis is not seen in tension-type headache. If a patient with headache has neuroretinitis findings, an infectious cause (particularly Bartonella henselae) must be actively sought.
This is a shared conversation. Sign in to Orris to start your own chat.