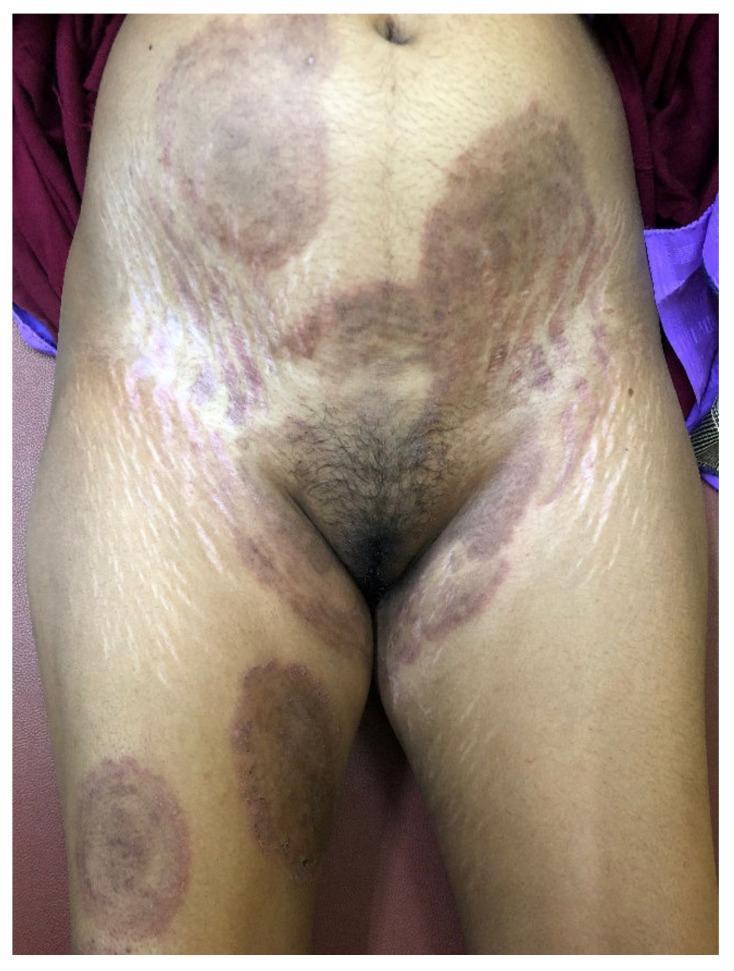
Lesions in an 22 year old male using a clobetasol neomycin based topical cream and previously treated with terbinafine for tenia infection in the groin region
Reading File
Finding Sources
Finding Sources
Finding Sources
Searching PubMed
tinea incognito corticosteroid modified tinea cruris
Finding Sources
Finding Sources
Finding Sources
Searching Images
tinea incognito groin steroid modified dermatophytosis
Reading File
Reading File
Finding Sources
Finding Sources
Reading File
Loading Image
Searching PubMed
Trichophyton indotineae terbinafine resistance India
I now have a comprehensive picture. Let me synthesize the full clinical analysis.
Clinical Assessment: Tinea Incognito (Steroid-Modified Tinea Cruris / Majocchi Granuloma)
What the Images Show
Across all four images, the lesions demonstrate:
- Large, hyperpigmented, lichenified plaques in the groin/inner thigh region
- Loss of the classic annular/raised scaly border — the active edge is blurred and ill-defined
- Dark central hyperpigmentation with overlying fine white scale/crust
- Follicular pustules and papules within and around the plaques
- Scattered erythematous papules and small erosions at the periphery
- No clear central clearing — unlike classic tinea cruris where the center heals
This appearance is not classic tinea cruris. It is a textbook presentation of Tinea Incognito with likely Majocchi Granuloma — a direct complication of applying clobetasol (a superpotent Class I corticosteroid) to a fungal infection.
Primary Diagnosis: Tinea Incognito
Tinea Incognito is a clinically altered dermatophytosis caused by inappropriate application of topical corticosteroids to a fungal infection. The steroid:
- Suppresses the host inflammatory/immune response, allowing uncontrolled fungal proliferation
- Abolishes the characteristic raised scaly active border
- Causes extensive spread of the lesion
- Produces hyperpigmentation and lichenification from chronic inflammation
- Promotes deep follicular invasion → Majocchi granuloma
"An altered appearance known as tinea incognito can occur in patients who have been treated erroneously with topical corticosteroids, which includes diminished erythema and absence of typical scaling borders. Such patients also can develop Majocchi granuloma when fungi invade the hair shaft and surrounding dermis, causing a granulomatous dermal reaction that can extend into the surrounding subcutaneous fat." — Red Book 2021, Report of the Committee on Infectious Diseases, p. 1173
The follicular papules and dark punctate lesions visible in images 3 and 4 are consistent with Majocchi granuloma — perifollicular granulomatous inflammation from dermatophyte invasion of the hair follicle.
Reference Image for Comparison
The image below shows a similar case of steroid-modified tinea cruris/corporis with corticosteroid misuse:
The Drug Problem: Clobetasol + Neomycin Combination
Clobetasol propionate is a Class I (superpotent) topical corticosteroid — the most potent class. Applied to the groin (an occluded, thin-skinned area with high percutaneous absorption), it rapidly:
- Immunosuppresses the skin, allowing the dermatophyte to proliferate unchecked
- Masks symptoms (itch, redness), giving a false impression of improvement
- Drives the infection into the hair follicle → Majocchi granuloma
- Causes skin atrophy, striae, and secondary bacterial colonization (the neomycin component addresses this surface bacterial issue but does nothing for the fungus)
Clobetasol is absolutely contraindicated in the groin/intertriginous regions and should never be applied to a fungal infection.
Causative Organism Consideration: T. indotineae
Given that terbinafine was previously tried and failed, a critical consideration is Trichophyton indotineae (formerly T. mentagrophytes var. VIII):
"Terbinafine-resistant T. indotineae... emerged in India with subsequent global spread. One theory for its emergence is the misuse of potent topical corticosteroids in settings where they are available without a prescription." — Dermatology 2-Volume Set 5e, p. 1605
This organism is particularly prevalent in India and South Asia, causes recalcitrant groin infections in young males, and has intrinsic/acquired terbinafine resistance via SQLE gene mutation (squalene epoxidase). Oral terbinafine failure in a young male with groin tinea is a red flag for T. indotineae.
Management Plan
Step 1: Immediately Stop Clobetasol
Cessation is non-negotiable. Continuing will worsen the infection further.
Step 2: Confirm Diagnosis
- KOH microscopy of scrapings from the active border — will show abundant hyphae (often more numerous than in classic tinea due to steroid-driven proliferation)
- Fungal culture on Sabouraud's dextrose agar — essential for species identification
- Antifungal susceptibility testing (MIC) — critical if T. indotineae is suspected (terbinafine MIC ≥4 µg/mL = resistant)
- Skin biopsy with PAS/GMS staining — for suspected Majocchi granuloma (shows hyphae in dermis/perifollicular tissue)
Step 3: Systemic Antifungal Therapy
For tinea incognito with likely Majocchi granuloma, topical therapy alone is insufficient — systemic treatment is required:
| Drug | Dose | Duration | Notes |
|---|---|---|---|
| Itraconazole | 200 mg/day or 200 mg BD (pulse) | 4–8 weeks | Drug of choice if T. indotineae suspected; good activity against terbinafine-resistant strains |
| Oral terbinafine | 250 mg/day | — | Avoid if prior failure — likely resistant |
| Fluconazole | 150–300 mg/week | 6–8 weeks | Alternative, though less potent for dermatophytes |
| Voriconazole | 200 mg BD | 4–6 weeks | Reserved for proven resistant cases |
| Griseofulvin | 500–1000 mg/day | 8–12 weeks | An option; less convenient |
Current evidence (PMID 38574764) supports itraconazole as the preferred systemic agent in the era of T. indotineae, given reliable susceptibility even in terbinafine-resistant strains.
Step 4: Supportive Measures
- Keep the area dry; use absorbent powder (tolnaftate, miconazole)
- Loose-fitting cotton underwear
- Treat concurrent tinea pedis/unguium if present (reservoir for reinfection)
- Avoid reapplication of any steroid-containing combination cream
Summary Table
| Feature | Finding |
|---|---|
| Diagnosis | Tinea incognito (steroid-modified tinea cruris) ± Majocchi granuloma |
| Causative agent | T. rubrum or T. indotineae (suspect given terbinafine failure) |
| Drug implicated | Clobetasol propionate (superpotent CS — contraindicated here) |
| Neomycin role | Addresses secondary bacterial colonization only; irrelevant to fungal cause |
| Key investigation | KOH smear + fungal culture + MIC testing |
| Treatment | Stop clobetasol immediately; systemic itraconazole 200 mg/day × 4–8 weeks |
| Biopsy | If Majocchi granuloma confirmed → mandatory systemic therapy |
Dermatology referral is recommended for formal culture, MIC testing, and supervised systemic therapy.
Which topical antifungal and emollient cream to be used along with systemic therapy
Finding Sources
Finding Sources
Finding Sources
Searching PubMed
topical antifungal tinea cruris adjunct systemic therapy
Reading File
Finding Sources
Finding Sources
Reading File
Finding Sources
Searching PubMed
luliconazole sertaconazole tinea cruris India treatment
Here is a structured answer covering both the topical antifungal and the emollient/barrier care for this specific case.
Topical Antifungal + Emollient in Tinea Incognito (Groin)
Important Caveat First
In confirmed tinea incognito with Majocchi granuloma, systemic therapy is the backbone of treatment. Topical antifungals have limited penetration into the dermis/follicle where Majocchi granuloma resides. However, topical agents are still useful adjunctively to reduce surface fungal burden, prevent reseeding, and manage the chronic skin damage from clobetasol.
1. Topical Antifungal: Best Choice in This Case
Why NOT terbinafine cream?
Given the prior oral terbinafine failure, T. indotineae with squalene epoxidase (SQLE) mutation is suspected. Terbinafine cream should be avoided — resistance affects both topical and oral formulations at the target-enzyme level.
"In some geographic regions (e.g. India), isolates of Trichophyton with increasing resistance to terbinafine have been observed due to mutations in the gene that encodes squalene epoxidase." — Dermatology 2-Volume Set 5e, p. 2695
Preferred Topical Options
| Drug | Form | Application | Why Preferred |
|---|---|---|---|
| Luliconazole 1% cream | Cream | Once daily × 2–4 weeks | Highest potency topical azole; excellent T. rubrum & T. indotineae activity; low MIC even for terbinafine-resistant strains; once-daily dosing improves adherence |
| Sertaconazole 2% cream | Cream | Twice daily × 2–4 weeks | Broad-spectrum azole + anti-inflammatory effect; particularly useful where lichenification/itch is prominent; good tolerability on intertriginous skin |
| Clotrimazole 1% cream | Cream | Twice daily × 4 weeks | Widely available, inexpensive, well-tolerated; first-line option if cost is a concern |
| Ciclopirox olamine 1% cream | Cream | Twice daily × 4 weeks | Distinct mechanism (chelates metal ions essential to fungal enzymes) — active regardless of SQLE or CYP51 mutations; also has anti-inflammatory and antibacterial properties |
"Topical azoles are indicated for tinea corporis, tinea pedis, tinea cruris... Cyclopirox olamine is active against dermatophytes [and] also anti-inflammatory due to its inhibition of prostaglandin and leukotriene synthesis." — Dermatology 2-Volume Set 5e, p. 2695
Top recommendation: Luliconazole 1% cream OD — it combines the highest in vitro potency against dermatophytes with once-daily convenience and lacks cross-resistance with terbinafine (it is an azole, not an allylamine).
Alternative: Ciclopirox 1% cream BD — mechanistically unrelated to both azoles and allylamines, so fully active regardless of resistance profile.
2. Emollient/Barrier Cream
The skin here has suffered chronic damage from:
- Long-term clobetasol → epidermal atrophy, disrupted skin barrier
- Chronic fungal inflammation → lichenification, scale, fissuring
- Friction + maceration in the groin
An emollient serves to restore the impaired skin barrier, reduce lichenification, relieve itch, and improve drug penetration of the antifungal.
Key Principles for the Groin Region
- Use light, non-occlusive emollients — heavy petrolatum-based products trap moisture and worsen maceration in intertriginous areas
- Avoid fragrance, preservatives (e.g. parabens) — the skin barrier is already compromised
- Apply after the antifungal cream has been absorbed (space by 15–20 minutes), not mixed together
Recommended Emollients
| Product type | Examples | Why suitable |
|---|---|---|
| Ceramide-containing cream | CeraVe Moisturizing Cream, Sebamed, DermaB | Directly replenishes ceramides depleted by steroid atrophy and fungal infection; restores lamellar bilayer structure |
| Urea 5–10% cream | Nutradeep 5%, Eucerin Urea | Mild keratolytic + humectant — softens lichenification; penetration-enhancing (helps antifungal penetrate); 5% for moist areas, 10% for drier lichenified patches |
| Glycerin-based light lotion | Simple Kind to Skin, Lacto Calamine lotion | Very light; non-occlusive; soothing on inflamed intertriginous skin |
| Zinc oxide paste (barrier) | Calamine lotion (during wet phase) | If active oozing or maceration is present — zinc has mild antifungal and astringent properties; apply as a thin barrier layer |
Top recommendation: Ceramide + hyaluronic acid cream (e.g. CeraVe or equivalent) — directly targets the clobetasol-induced barrier disruption; non-comedogenic, fragrance-free, light enough for groin use.
If significant lichenification is present (as seen in images 3 and 4): Urea 10% cream on lichenified areas to soften plaques while aiding antifungal penetration.
Practical Application Schedule
| Time | Product |
|---|---|
| After bath (pat dry) | Luliconazole 1% cream — thin layer over affected area |
| 15–20 min later | Ceramide cream (light layer) — or urea 10% on thickened areas |
| Evening only if needed | Calamine lotion if maceration/oozing is present |
What to Strictly Avoid
| Avoid | Reason |
|---|---|
| Any steroid-containing cream (including hydrocortisone) | Will worsen tinea incognito further |
| Steroid-antifungal combinations (e.g. clotrimazole + betamethasone, Panderm, Quadriderm) | Remain widely misused; re-exposure will cause relapse |
| Terbinafine cream | Likely resistant organism |
| Heavy occlusive petrolatum in the groin fold | Traps moisture, worsens maceration and secondary candidiasis |
| Neomycin-containing products | Risk of contact sensitization on already-damaged barrier skin |
Summary: Luliconazole 1% cream once daily (or ciclopirox 1% cream BD if resistance is a concern) + ceramide-based light emollient, applied separately, for the duration of systemic itraconazole therapy (4–8 weeks). Reassess at 4 weeks with KOH to confirm mycological cure.
This is a shared conversation. Sign in to Orris to start your own chat.