Role of pediatrician in anc
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Loading Image
Reading File
Now I have enough to provide a comprehensive answer. The textbooks confirmed that antenatal counseling is the first step in neonatal resuscitation planning. Let me now synthesize a thorough answer from my medical knowledge combined with textbook evidence.
Role of the Pediatrician in Antenatal Care (ANC)
The pediatrician — or neonatologist — has a distinct and important role during the antenatal period that is separate from obstetric care. This role centers on preparing for the newborn, counseling the family about anticipated fetal/neonatal conditions, and coordinating delivery-room readiness.
1. Antenatal Counseling (the Primary Role)
As shown in the Neonatal Resuscitation Algorithm, antenatal counseling is the first step before any delivery:
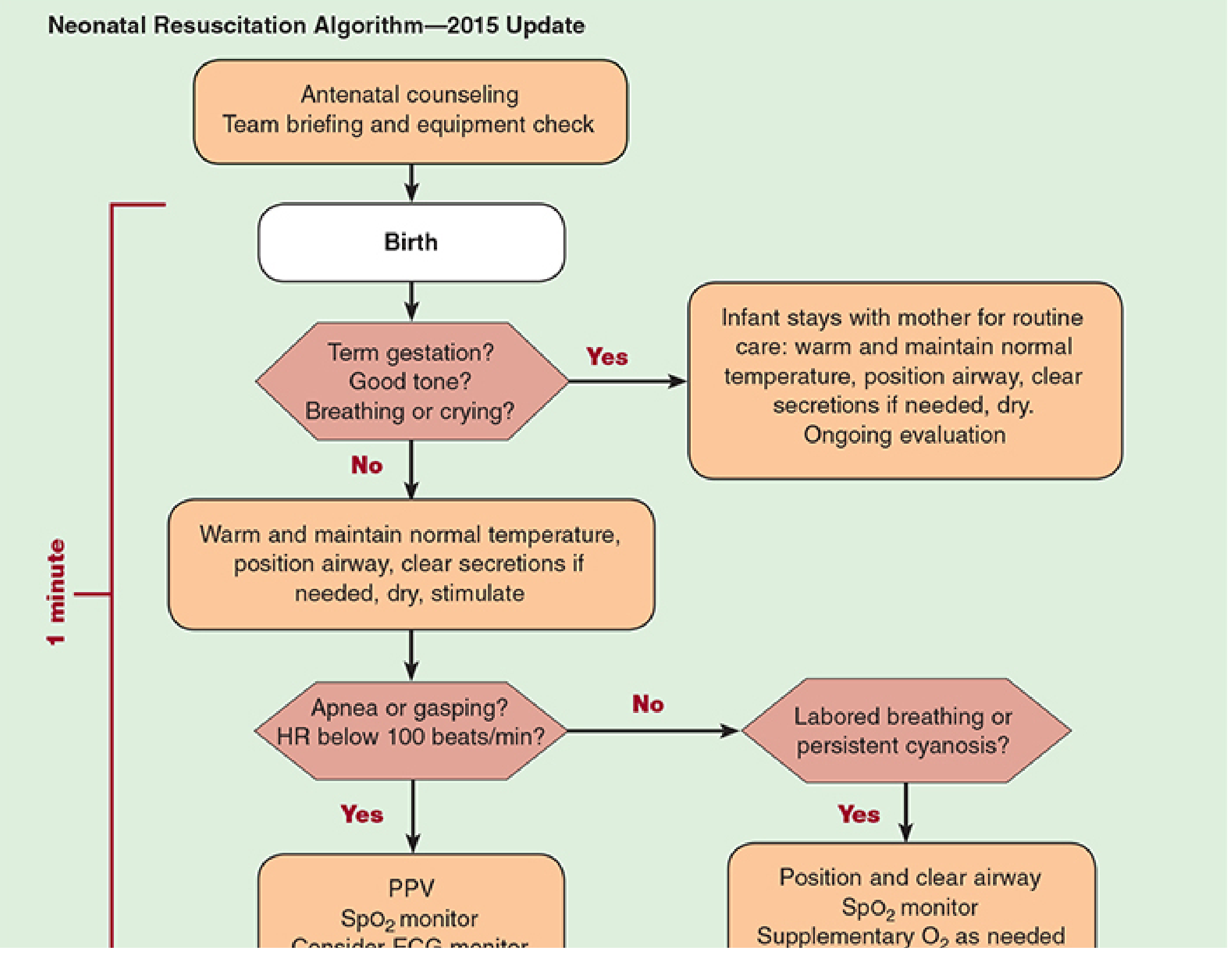
This involves:
- Team briefing and equipment check prior to every high-risk delivery
- Reviewing maternal history, gestational age, fetal anomalies detected on antenatal ultrasound, and expected complications
2. High-Risk Pregnancy Consultation
A pediatrician/neonatologist is specifically called for antenatal consultation when the obstetrician anticipates:
| Maternal Condition | Neonatal Risk Requiring Pediatric Input |
|---|---|
| Pregestational/gestational diabetes | Macrosomia, hypoglycemia, RDS, congenital anomalies |
| Maternal thyroid disease (Graves') | Neonatal hyperthyroidism/hypothyroidism |
| Hypertension / Pre-eclampsia | Preterm birth, IUGR, thrombocytopenia |
| Infections (TORCH, GBS, HIV) | Congenital infection, prophylaxis planning |
| Polyhydramnios/oligohydramnios | GI atresias, renal anomalies |
| Multiple pregnancy | Prematurity, TTTS |
| Substance abuse / medications | Neonatal abstinence syndrome |
3. Counseling Regarding Resuscitation at the Limits of Viability
One of the most critical roles is counseling parents when delivery is anticipated before 25 weeks of gestation. The American Academy of Pediatrics (AAP) recommends:
- Discussion of prognosis at each gestational age (22–25 weeks)
- Parent-centered decision making regarding resuscitation vs. comfort care
- Documentation of antenatal consultation in the chart
- Per Mulholland & Greenfield's Surgery: "Antenatal counseling regarding resuscitation and intensive care before 25 weeks of gestation" is an established standard of care (Cummings J, Committee on Fetus and Newborn. Pediatrics 2015;136(3):588–595)
4. Fetal Anomaly Counseling
When structural anomalies are detected on ultrasound or genetic diagnosis confirms a condition:
- The pediatric surgeon, neonatologist, or relevant subspecialist meets with the family antenatally
- Explains postnatal management plan (e.g., for CDH, orofacial clefts, cardiac defects, renal anomalies)
- Coordinates delivery at an appropriate level of care (tertiary center if needed)
- Example: "Most families find antenatal counseling helpful in planning for care of the child with an orofacial cleft" — Cummings Otolaryngology Head and Neck Surgery
5. Planning for Delivery Room Readiness
Based on the antenatal consultation, the pediatrician/neonatologist:
- Ensures appropriate resuscitation equipment is available and functional
- Assembles the resuscitation team (at least one provider whose sole responsibility is care of the newborn must be present at every delivery)
- Plans for surfactant therapy, intubation, umbilical line placement in anticipated preterm deliveries
- Arranges NICU bed and transport if necessary
6. Anticipatory Guidance to Parents
The pediatrician counsels expectant parents on:
- Breastfeeding preparation and lactation support
- Newborn screening (metabolic, hearing, critical CHD)
- Immunization schedule starting at birth (Hepatitis B, BCG)
- Safe sleep practices (back to sleep, avoiding co-sleeping)
- Neonatal jaundice recognition
- Vitamin K and eye prophylaxis at birth
- Signs of neonatal illness requiring urgent care
7. Antenatal Genetic Counseling (Collaborative)
When chromosomal or genetic conditions are diagnosed prenatally:
- The clinical geneticist and pediatric specialist jointly counsel the family
- Explain natural history, management options, recurrence risks, and prognosis
- Coordinate multidisciplinary team for delivery (Emery's Elements of Medical Genetics and Genomics)
Summary
| Domain | Pediatrician's Role in ANC |
|---|---|
| High-risk cases | Antenatal consultation and risk communication |
| Limits of viability | Counseling on resuscitation decisions (<25 weeks) |
| Fetal anomalies | Subspecialty counseling and delivery planning |
| Delivery room | Team briefing, equipment, resuscitation readiness |
| Parent education | Newborn care, feeding, immunization, safe sleep |
| Genetics | Collaborative counseling for chromosomal conditions |
The overarching principle is that the pediatrician's antenatal role is preventive and preparatory — anticipating neonatal complications, empowering parents with accurate information, and ensuring the team is ready to provide optimal care from the moment of birth.
References:
- Morgan and Mikhail's Clinical Anesthesiology, 7e — Neonatal Resuscitation
- Creasy & Resnik's Maternal-Fetal Medicine — Antenatal Monitoring
- Cummings Otolaryngology — Prenatal Diagnosis
- Mulholland & Greenfield's Surgery — citing AAP Committee on Fetus and Newborn, Pediatrics 2015
This is a shared conversation. Sign in to Orris to start your own chat.