Bell Magendie law
Reading File
Finding Sources
Finding Sources
Searching the Web
Bell Magendie law spinal cord dorsal ventral roots anatomy physiology
Finding Sources
Finding Sources
Reading File
Reading File
Searching Images
Bell Magendie law spinal nerve roots dorsal ventral motor sensory
Here is a comprehensive overview of the Bell–Magendie Law:
Bell–Magendie Law
Definition
The Bell–Magendie law states that:
The anterior (ventral) roots of spinal nerves contain only motor (efferent) fibers, while the posterior (dorsal) roots contain only sensory (afferent) fibers.
It is the foundational principle of spinal nerve root functional segregation.
Historical Background
The law is named after two scientists who independently made the same discovery in the early 19th century:
- Sir Charles Bell (Scottish anatomist, ~1811) — described the functional distinction between anterior and posterior spinal roots, though his early work was partly unpublished.
- François Magendie (French physiologist, ~1822) — experimentally demonstrated the law in animals, famously using unanesthetized puppies (for which he was later criticized by Bell for animal cruelty). Magendie's systematic, experimental approach gave the law wider scientific recognition.
This led to a long-standing priority dispute between the two, and ultimately both names were attached to the principle.
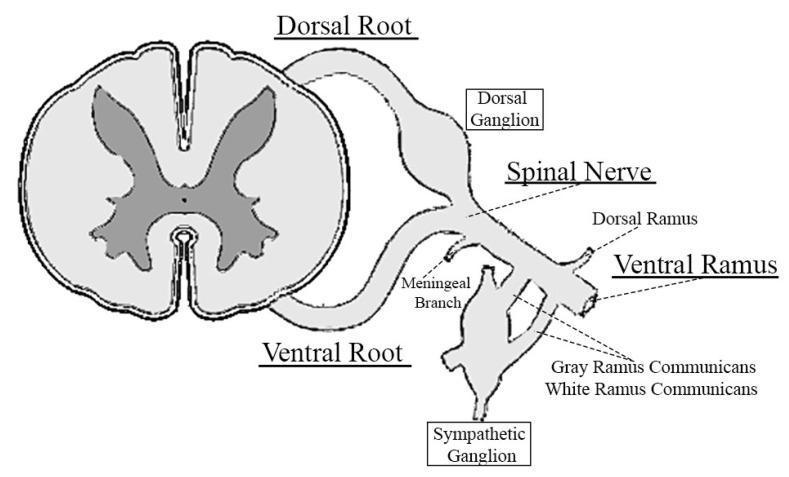
Anatomy
| Root | Direction | Function | Cell Body Location |
|---|---|---|---|
| Posterior (dorsal) root | Afferent (toward CNS) | Sensory | Dorsal root ganglion (DRG), outside the spinal cord |
| Anterior (ventral) root | Efferent (away from CNS) | Motor | Anterior (ventral) horn of spinal cord gray matter |
- Sensory neurons in the dorsal root ganglia have bifurcating axons: one branch collects sensory input from the periphery (skin, muscles, joints), the other enters the spinal cord via the dorsal root filaments into the dorsal horn.
- Motor neurons in the ventral horn send their axons out via ventral root filaments.
- The two roots fuse in or near the intervertebral foramen to form a mixed spinal nerve, which then divides into dorsal and ventral rami — both of which carry both sensory and motor fibers.
- The sensory (dorsal) root is approximately twice as thick as the motor (ventral) root. — Goldman-Cecil Medicine
Clinical Relevance
The Bell–Magendie law is the anatomical basis for distinguishing:
- Dorsal root / sensory radiculopathy: Damage to the posterior root → loss of sensation, pain, paresthesias in a dermatomal distribution. Motor power is preserved.
- Ventral root / motor radiculopathy: Damage to the anterior root → lower motor neuron (LMN) signs — weakness, hypotonia, hyporeflexia, fasciculations, muscle atrophy in a myotomal distribution. Sensation is preserved.
- Mixed spinal nerve or plexus lesions: Both sensory and motor deficits occur together (since the mixed nerve carries both).
This distinction is fundamental in differentiating:
- Root avulsions (preganglionic) vs. peripheral nerve injuries (postganglionic)
- Pure sensory vs. pure motor neuropathies
- Dorsal root ganglionopathies (sensory neuronopathies) — which spare motor function entirely
— Neuroanatomy through Clinical Cases, 3rd Ed.; Goldman-Cecil Medicine; Gray's Anatomy for Students
Important Nuance / Limitation
The "pure" separation is not absolute. Research has shown that:
- The ventral roots contain a small number of unmyelinated C-fiber afferents (~30% of ventral root fibers may carry pain sensations) — this may explain why dorsal rhizotomy alone does not always abolish pain.
- This finding prompted the statement: "The law of Magendie…was recently questioned. It turned out that ventral roots contain unmyelinated fibres…" — (PubMed 2674573)
Despite this refinement, the Bell–Magendie law remains the core teaching principle of spinal root functional organization.
This is a shared conversation. Sign in to Orris to start your own chat.