Distal radius fracture in orthopedic
Reading File
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Searching PubMed
"distal radius fracture" AND treatment
Reading File
Searching Images
distal radius fracture classification radiograph volar plate ORIF
Loading Image
Loading Image
I now have comprehensive content from Rockwood & Green and Miller's Review. Here is the complete clinical overview:
Distal Radius Fracture — Orthopedic Overview
Epidemiology
Distal radius fractures are the most common fracture of the upper extremity, accounting for at least one-sixth of fractures seen in the emergency department. Annual prevalence in the US exceeds 600,000 cases. There is a bimodal distribution:
- Young men: high-energy mechanisms (MVAs, falls from height, industrial injuries)
- Elderly women: low-energy falls; incidence in females is 2–3× that of males; second most common fracture in the elderly
— Rockwood and Green's Fractures in Adults, 10th ed., p. 1823
Mechanism of Injury
| Fracture Type | Wrist Position at Impact |
|---|---|
| Dorsally displaced (Colles) | Outstretched hand in 40–90° dorsiflexion |
| Volarly displaced (Smith) | Wrist in volar flexion |
| Volar shear (Barton) | High-energy axial/shear load |
Poor bone quality (low DXA T-scores) correlates with greater fracture severity and risk of early instability.
Applied Anatomy
Key anatomic facts relevant to fracture management:
- Volar surface: concave and smooth → ideal for volar plate application; covered by pronator quadratus (PQ)
- Dorsal surface: convex with extensor tendon grooves; Lister tubercle forms pulley for EPL
- Sigmoid notch: ulnar border of radius; articulates with distal ulna at DRUJ
- Articular surface: two concave facets — scaphoid facet (radial) and lunate facet (ulnar)
- Lunate facet: projects ~3 mm volarly; prone to shear forces; difficult to repair
- Brachioradialis: only tendinous insertion on distal radius; acts as deforming force in fractures
- TFCC: primary soft tissue stabilizer of the DRUJ
— Rockwood and Green's, p. 1826
Normal Radiographic Parameters ("11:11:22 Rule")
| Parameter | Normal Value | Acceptable Postreduction Limit |
|---|---|---|
| Radial height | ~11 mm | < 5 mm shortening |
| Volar tilt | ~11° | < 10° dorsal angulation |
| Radial inclination | ~22° | < 5° change |
| Intra-articular step-off | 0 mm | < 2 mm |
Ulnar variance (neutral, positive, or negative) should be assessed with forearm in neutral rotation compared to the contralateral side.
— Miller's Review of Orthopaedics, 9th ed., p. 650
Associated Injuries
| Injury | Frequency / Notes |
|---|---|
| TFCC injury | 39–82%; most are peripheral avulsions with ulnar styloid fractures |
| Scapholunate ligament | 4.7–46% (arthroscopic studies); true clinical significance debated |
| Lunotriquetral ligament | 12–34% |
| Acute carpal tunnel syndrome | Less common; characterized by progressive pain and neurologic deficit → urgent release |
| Chondral injuries | Present in comminuted/articular patterns |
The carpal stretch test (traction to accentuate Gilula lines) has ~78% sensitivity and ~72% specificity for grade 3–4 interosseous ligament tears.
Classification
Eponyms (pre-radiographic; still widely used)
| Eponym | Pattern |
|---|---|
| Colles | Dorsally angulated, apex volar extra-articular metaphyseal fracture |
| Smith | Volarly angulated, apex dorsal metaphyseal fracture ("reverse Colles") |
| Barton | Intra-articular fracture with dorsal cortex involvement + radiocarpal subluxation/dislocation |
| Reverse (Volar) Barton | Intra-articular fracture with volar extension + volar subluxation |
| Chauffeur's (Hutchinson) | Isolated intra-articular radial styloid fracture |
AO/OTA Classification (most widely used)
| Group | Description |
|---|---|
| A | Extra-articular |
| B | Partial articular (one cortex remains intact) |
| C | Complete articular (articular surface fully separated from diaphysis) |
Each group has 3 subgroups with 3 further subtypes = 27 total patterns.
Historical systems (rarely used clinically)
- Gartland & Werley: 3 groups based on articular involvement and comminution
- Frykman: Based on articular involvement ± ulna fracture
- Melone: Emphasizes "medial complex" (dorsomedial + palmar medial fragments) and lunate facet impaction
None of the existing systems reliably predict treatment or prognosis. — Rockwood and Green's, p. 1828
Instability Predictors
Lafontaine Criteria (≥3 of 5 = high risk of secondary displacement)
- Dorsal angulation > 20°
- Dorsal comminution
- Intra-articular radiocarpal fracture
- Associated ulnar fracture
- Age > 60 years
Note: A larger study (MacKenney ~4,000 fractures) found that age, ulnar variance, and metaphyseal comminution were the most consistent predictors; dorsal angulation alone was not significant. Risk of displacement increases linearly with age.
Treatment
Goals
- Maintain reduction until union
- Restore function
- Prevent symptomatic post-traumatic radiocarpal arthritis
Nonoperative Treatment
Indications: Extra-articular minimally displaced fractures; low-demand patients
Technique of closed reduction:
- Dorsal hematoma block with local anesthetic; finger traps for traction
- Volar translation of lunate with traction and ulnar deviation
- Re-create deformity → manipulate distal fragment
- Sugar-tong plaster splint with three-point mold (hook volar cortex)
- MCP and IP joints must be kept free
Immobilization: 6–8 weeks
Post-reduction benchmarks (AAOS guideline):
- Radial shortening < 5 mm
- Dorsal articular tilt < 5–10°
- Intra-articular step-off < 2 mm
Operative Treatment
| Method | Indications / Key Points |
|---|---|
| CRPP (Closed reduction, percutaneous pinning) | Extra-articular fractures in younger patients without osteoporosis; Kapandji intrafocal or arthroscopically assisted technique; less used since volar plating advent |
| External fixation | Unstable fractures with soft tissue compromise; combination with CRPP; articular alignment difficult; overdistraction → risk of CRPS |
| ORIF — Volar locking plate | Most commonly performed; stable fixation for most dorsally displaced fractures; plate must be proximal to watershed line to avoid flexor tendon irritation |
| ORIF — Dorsal plate | Used for dorsal shearing, die-punch, and severely comminuted articular fractures; concurrent SL ligament injuries; higher tendon irritation rate |
| Bridge/distraction plate | Alternative to external fixation in highly comminuted unstable fractures or severe osteoporosis; allows weight-bearing through the extremity |
| Fragment-specific fixation | Best for certain intra-articular patterns including volar-ulnar ("critical corner") fragment; hook plate for volar-ulnar fragment |
AAOS 2020 CPG: Appropriate to treat isolated, low-energy AO/OTA type A fractures in high-functioning, healthy patients with ORIF.
Post-operative Radiographs: Volar Locking Plate
AP view — post ORIF volar locking plate (left wrist):
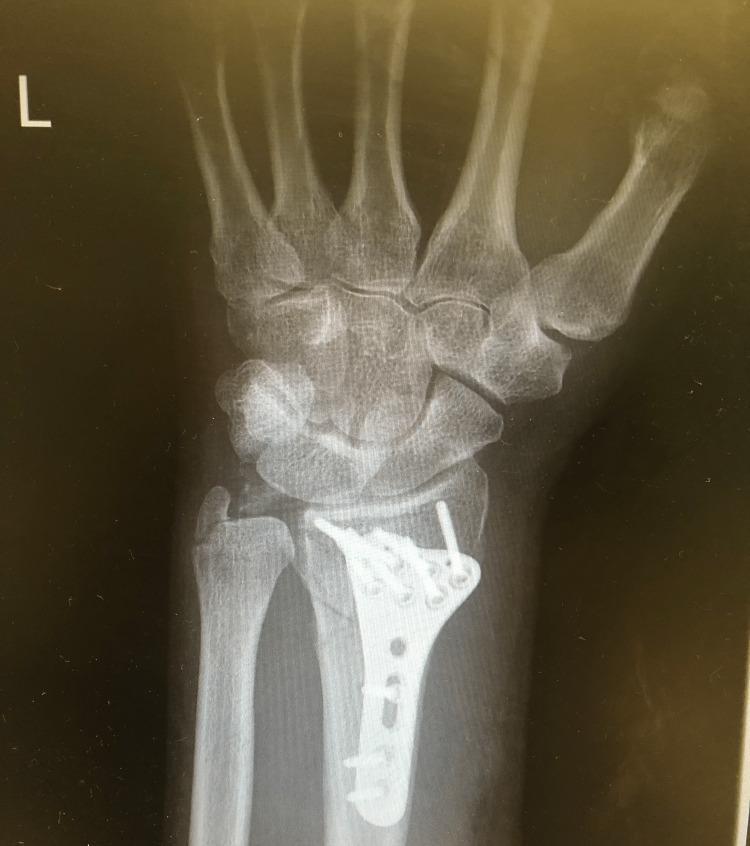
Lateral view — post ORIF volar locking plate (right wrist):
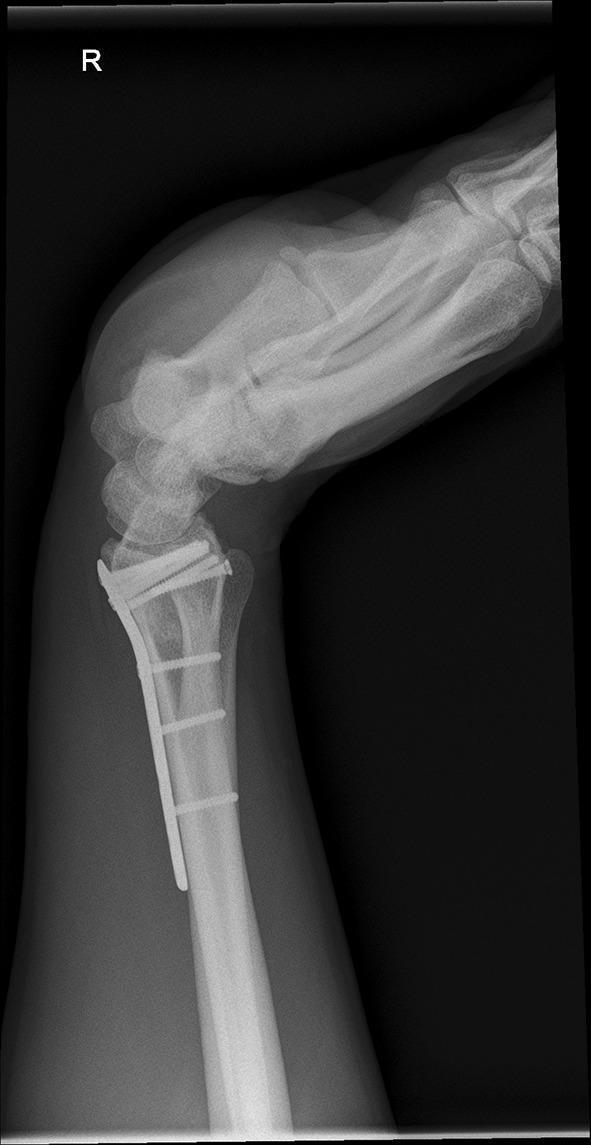
Complications
| Complication | Key Details |
|---|---|
| Acute CTS | Progressive paresthesias + disproportionate pain → emergent carpal tunnel release. Mild non-progressive sensory dysfunction is NOT acute CTS. |
| EPL tendon rupture | Most common tendon rupture, both operative and non-operative; late complication (hematoma, attrition at Lister tubercle); treat with EIP transfer |
| FPL rupture | After volar plating; occurs when plate is distal to the watershed line; most common flexor tendon injured |
| Extensor tendon irritation (EPL) | From volar plate dorsal screw too long; check on fluoroscopy |
| Malunion | Common in elderly managed nonoperatively; treatment should target symptomatic patients |
| Ulnar nerve palsy | After high-energy displaced fractures; most often neuropraxia |
| CRPS | Risk increased with overdistraction via external fixation |
| Hardware removal | Complication rate up to 13% with locking plates |
Malunion Criteria
- Radial inclination < 10°
- Volar tilt > 20° or dorsal tilt > 20°
- Radial height < 10 mm
- Ulnar variance > +2 mm
- Intra-articular incongruity > 2 mm
Distal Ulna Fractures (Associated)
- Ulnar styloid fracture: Concurrent treatment is not routinely necessary — no additional clinical benefit if DRUJ is stable after radial fixation
- DRUJ instability/painful nonunion occurs in < 10% of cases after radial reduction
- Unstable DRUJ: indicated for fixation; options include tension band construct or mini-fragment T-plate
Controversies & Special Topics
- Arthroscopy: Aids articular reduction and confirms screws do not penetrate radiocarpal joint
- Bone grafting: Used for structural defects from impaction; calcium phosphate or coralline hydroxyapatite
- Post-operative motion: Evidence does not support early over late motion recovery
- Osteoporosis: Should prompt evaluation and treatment in low-energy fractures (DXA screening)
- Rehabilitation: Recent 2024 systematic review (Mehta et al., JOSPT, PMID 39213418) provides evidence-based rehabilitation guidelines
Recent Evidence (2024)
| Study | Key Finding |
|---|---|
| Mehta et al. 2024 (Syst. Review) [PMID 39213418] | Evidence-based rehabilitation guidelines for distal radius fractures |
| Gruisen et al. 2024 (Syst. Review) [PMID 38849773] | Patient-reported outcomes after surgical salvage for post-traumatic radiocarpal OA |
| Lister et al. 2024 (Syst. Review) [PMID 37269124] | Spontaneous EPL rupture — relevant complication after distal radius fixation |
Sources: Rockwood and Green's Fractures in Adults, 10th ed. (2025); Miller's Review of Orthopaedics, 9th ed.
This is a shared conversation. Sign in to Orris to start your own chat.