Rheumatic fever
Reading File
Finding Sources
Searching PubMed
"rheumatic fever"[MeSH Terms] AND diagnosis
Reading File
Reading File
Reading File
Finding Sources
Reading File
Finding Sources
Searching Images
rheumatic fever erythema marginatum skin rash
Reading File
Finding Sources
Reading File
I now have comprehensive information. Let me compile the full answer.
Acute Rheumatic Fever (ARF)
Definition & Overview
Acute rheumatic fever is a systemic inflammatory disease that follows pharyngeal infection with Group A β-hemolytic Streptococcus pyogenes (GAS), specifically mucoid types 3, 5, and 18. It is an immune-mediated, non-suppurative sequel of streptococcal pharyngitis — not skin infections. The disease affects connective tissue of the heart, joints, CNS, and skin.
Epidemiology
- Most common in children 5–15 years old
- Equal sex incidence in ARF; chronic rheumatic heart disease (RHD) is more common in women
- Incidence has fallen in developed countries over the past 50 years, but outbreaks with virulent GAS strains still occur
- Only ~1–3% of infected individuals develop ARF — genetic susceptibility likely plays a role
- ARF remains a major cause of acquired heart disease in the developing world, with RHD prevalence peaking in the 3rd and 4th decades of life
Pathobiology
The mechanism is molecular mimicry: M-protein antigens on certain GAS strains share structural homology with human cardiac proteins (myosin, valvular tissue, basal ganglia). This triggers cross-reactive T cells and antibodies that attack host tissues:
| Manifestation | Mechanism |
|---|---|
| Carditis | Antibody binding + T-cell infiltration of the heart |
| Arthritis | Immune complex deposition in joints |
| Chorea | Antibody binding to basal ganglia |
| Skin findings | Delayed hypersensitivity |
The hallmark 2–3 week delay between throat infection and ARF onset reflects the time required to mount this immune response — by this point, streptococci are absent from lesions.
Clinical Manifestations
Symptoms develop approximately 2–6 weeks after pharyngitis and usually persist 2–4 weeks.
| Feature | Frequency |
|---|---|
| Fever | >90% |
| Migratory polyarthritis (large joints) | 60–75% |
| Carditis (pancarditis) | >50% |
| Sydenham chorea | ~30% |
| Subcutaneous nodules | <10% |
| Erythema marginatum | <10% |
Key Features:
Arthritis: Migratory, fleeting, affecting large joints (knees, ankles, hips, elbows). Sterile synovial fluid with lymphocyte predominance. Responds rapidly to NSAIDs — lack of response should prompt reconsideration.
Carditis (Pancarditis): Affects all three layers of the heart:
- Pericardium: fibrinous exudate (resolves without sequelae)
- Myocardium: scattered Aschoff bodies in interstitial connective tissue
- Endocardium/Valves: fibrinoid necrosis + 1–2 mm verrucous vegetations along valve closure lines; mitral valve most affected, aortic valve less frequently
Sydenham Chorea (St. Vitus Dance): Involuntary, non-rhythmic, purposeless movements of body, limbs, and face. More pronounced on one side. Stops during sleep — a distinguishing feature.
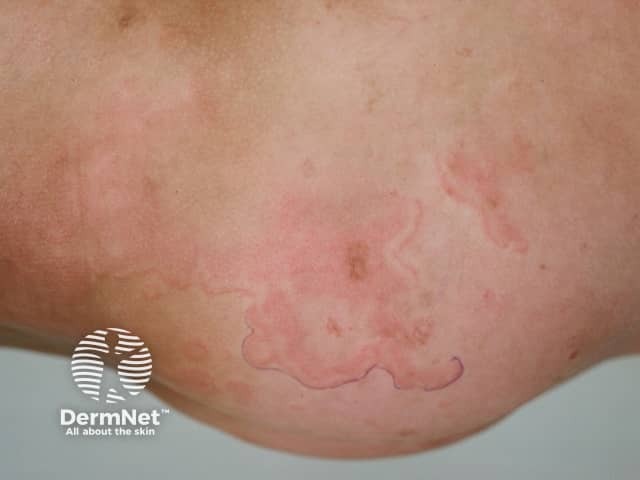
Erythema Marginatum: Pink, non-pruritic, blanching macules or papules spreading in a serpiginous pattern on the trunk and proximal limbs (spares the face). Evanescent and migratory.
Subcutaneous Nodules: 0.5–2 cm, painless, over bony prominences or extensor tendons.
Pathology (Histology)
Aschoff bodies are pathognomonic for rheumatic carditis:
- Collections of lymphocytes (primarily T cells), plasma cells, and plump activated macrophages (Anitschkow cells)
- Anitschkow cells have centrally condensed, wavy-ribbon chromatin → "caterpillar cells"
- Associated with zones of fibrinoid necrosis
- Seen in all three cardiac layers during acute disease; replaced by fibrous scar in chronic disease
Chronic RHD features: leaflet thickening, commissural fusion, shortened/fused chordae tendineae → classic "fishmouth" or "buttonhole" mitral stenosis with calcification.
Diagnosis — Revised Jones Criteria (2015 AHA)
No definitive test exists. Diagnosis is clinical, requiring evidence of a preceding GAS infection (throat culture, ASO titer, anti-DNase B) plus criteria below.
Definition:
- Initial ARF: 2 major OR 1 major + 2 minor criteria
- Recurrent ARF: 2 major, OR 1 major + 2 minor, OR 3 minor criteria
Major Criteria:
| Low-Risk Populations | Moderate/High-Risk Populations |
|---|---|
| Carditis (clinical ± subclinical echocardiographic valvulitis) | Carditis (clinical ± subclinical) |
| Polyarticular arthritis | Mono- or polyarticular arthritis |
| Chorea | Chorea |
| Erythema marginatum | Erythema marginatum |
| Subcutaneous nodules | Subcutaneous nodules |
Note: In moderate/high-risk populations, monoarthritis and monoarthralgia are upgraded (major and minor, respectively), reflecting higher pre-test probability.
Minor Criteria:
| Low-Risk | Moderate/High-Risk |
|---|---|
| Polyarthralgia | Monoarthralgia |
| Fever ≥38.5°C | Fever ≥38.5°C |
| ESR ≥60 mm/hr and/or CRP ≥3.0 mg/dL | ESR ≥30 mm/hr and/or CRP ≥3.0 mg/dL |
| Prolonged PR interval (if carditis not a major criterion) | Prolonged PR interval |
Low-risk = ARF incidence <2/100,000 school-aged children/year OR RHD prevalence ≤1/1,000/year.
Supporting Labs:
- Elevated ESR, CRP
- Normochromic normocytic anemia, leukocytosis
- ECG: prolonged PR interval
- Echocardiography: to assess subclinical valvulitis
- Rising ASO or anti-DNase B titers
Treatment
1. Eradication of GAS (Primary Treatment)
- Benzathine penicillin G 1.2 million units IM (600,000 U if <27 kg) — single dose
- Penicillin V 250 mg PO twice daily × 10 days
- Erythromycin or azithromycin for penicillin-allergic patients
2. Anti-inflammatory Therapy
- Arthritis: Aspirin 80–100 mg/kg/day (max 4–8 g/day) — first-line; OR naproxen 10–20 mg/kg/day divided BID. Continue 1–2 weeks until all symptoms resolve.
- Carditis with heart failure: Diuretics, ACE inhibitors/ARBs, fluid restriction, bed rest. Systemic glucocorticoids in severe cases (high-quality evidence lacking).
- Chorea: Usually self-limiting (weeks–months); treatment rarely needed.
3. Hospitalization
Admission is generally advised early to confirm the diagnosis.
Secondary Prophylaxis (Prevention of Recurrence)
Recurrences cause cumulative valve damage. Long-term prophylaxis is mandatory.
| Category | Duration |
|---|---|
| ARF without carditis | 5 years after last episode OR until age 21, whichever is longer |
| ARF with carditis, no residual valve disease | 10 years after last episode OR until age 21, whichever is longer |
| ARF with carditis + residual valvular disease | 10 years after last episode OR until age 40, whichever is longer; consider lifelong prophylaxis for severe valvular disease or high-exposure settings |
Preferred Regimens (AHA):
| Drug | Dose | Route |
|---|---|---|
| Benzathine penicillin G (preferred) | 1.2 million U every 4 weeks (every 3 weeks in high-risk settings) | IM |
| Penicillin V | 250 mg BID | PO |
| Sulfadiazine | 0.5 g/day (<27 kg), 1 g/day (>27 kg) | PO |
| Macrolide (azithromycin) | 250 mg/day | PO (penicillin-allergic) |
Prognosis
- Despite treatment, 35–70% of patients progress to chronic rheumatic heart disease
- The greatest risk of carditis recurrence is in the first year after acute carditis
- RHD produces predominantly mitral stenosis (and, less commonly, aortic stenosis/regurgitation)
Recent Evidence
Two 2024 systematic reviews are relevant:
- A Cochrane review on long-term antibiotic prophylaxis (PMID 39312290) evaluated secondary prevention and progression to RHD — still supports benzathine penicillin G as the mainstay.
- A meta-analysis on adherence to secondary prophylaxis (PMID 39542478) highlighted poor adherence as a major barrier to prevention — supporting IM over oral regimens in high-burden settings.
Sources: Goldman-Cecil Medicine, 26e; Robbins & Kumar Basic Pathology; Tintinalli's Emergency Medicine; Red Book 2021 (AAP); Fuster and Hurst's The Heart, 15e
This is a shared conversation. Sign in to Orris to start your own chat.