Which drug is better for abdominal pain in pregnancy dicyclomine or anafortan?
Reading File
Checking Date & Time
Finding Sources
Finding Sources
Searching PubMed
dicyclomine pregnancy safety abdominal pain
Reading File
Finding Sources
Finding Sources
Reading File
Searching the Web
anafortan camylofin pregnancy safety abdominal pain obstetrics
I now have enough information to give a clear, evidence-based answer. Here's a comprehensive comparison:
Dicyclomine vs. Anafortan (Camylofin) for Abdominal Pain in Pregnancy
TL;DR
Neither drug is ideal, but if a spasmolytic is truly necessary, dicyclomine has better-established human safety data for pregnancy. Anafortan (camylofin) is labeled "not recommended unless absolutely necessary" in pregnancy.
Dicyclomine
Mechanism: Anticholinergic (antimuscarinic) antispasmodic
Pregnancy status: ✅ "May be used in pregnancy. No known embryo-fetal risk based on human studies"
Pregnancy status: ✅ "May be used in pregnancy. No known embryo-fetal risk based on human studies"
- Historical data exists from its use in the Bendectin formulation (used by ~30% of American pregnant women for nausea/vomiting of pregnancy in the 1970s–80s), which provided substantial human safety data.
- Classified as relatively acceptable for use in pregnancy when indicated.
- ⚠️ Contraindicated in breastfeeding — associated with infant apnea risk.
- One important caveat: Yamada's Gastroenterology also notes antispasmodics as a class "should be avoided in pregnancy as their safety has not been fully established" — reflecting that use should still be justified clinically.
— Yamada's Textbook of Gastroenterology, 7th ed., Table 40.6: Pharmacological treatment of abdominal pain in pregnancy
Anafortan (Camylofin Dihydrochloride)
Mechanism: Smooth muscle relaxant with dual action — anticholinergic + direct musculotropic (papaverine-like)
Pregnancy status: ⚠️ "Not recommended for use in pregnant women unless absolutely necessary. All risks and benefits should be discussed."
Pregnancy status: ⚠️ "Not recommended for use in pregnant women unless absolutely necessary. All risks and benefits should be discussed."
- Used in obstetric practice primarily for cervical ripening and labor augmentation (shortening active labor duration) — not as a routine analgesic for abdominal pain during pregnancy.
- Evidence for its use in obstetrics is largely from Indian literature in the context of labor, not for pain relief during early/mid pregnancy.
- No large, controlled human teratogenicity/safety data comparable to dicyclomine.
- It is not absent from pregnancy contexts — but its role is labor management, not analgesia.
Head-to-Head Summary
| Feature | Dicyclomine | Anafortan (Camylofin) |
|---|---|---|
| Mechanism | Anticholinergic | Anticholinergic + musculotropic |
| Human pregnancy safety data | ✅ Available — no known embryo-fetal risk | ⚠️ Limited — "use only if necessary" |
| Approved obstetric use | Abdominal spasm / IBS | Labor augmentation / cervical ripening |
| Breastfeeding | ❌ Contraindicated (infant apnea) | Use with caution |
| Overall pregnancy recommendation | Preferred if antispasmodic needed | Reserve for labor use; avoid for general abdominal pain |
Practical Guidance
- For spasmodic abdominal pain in pregnancy (e.g., IBS, uterine round ligament pain, GI spasm): Dicyclomine is the better-supported choice when an antispasmodic is deemed necessary.
- Non-pharmacological options (heat, rest, positioning) and acetaminophen/paracetamol (for pain) should always be tried first.
- NSAIDs (including diclofenac) are contraindicated after 20 weeks gestation.
- Hyoscine/buscopan is another option but also has limited human data ("caution advised").
- Always assess the underlying cause of abdominal pain in pregnancy before treating symptomatically — surgical causes (appendicitis, ectopic, placental abruption) must be ruled out.
Sources: Yamada's Textbook of Gastroenterology, 7th ed.; Goodman & Gilman's Pharmacological Basis of Therapeutics; Camylofin in Obstetrics – IJRCOG; Practo: Anafortan Injection
Dichorionic monoamniotic twins
Checking Date & Time
Asking for Preferences
Finding Sources
Finding Sources
Reading File
Reading File
Finding Sources
Reading File
Finding Sources
Finding Sources
Reading File
I now have comprehensive information to answer this. Importantly, the research reveals a critical conceptual point about the query itself.
⚠️ Important Clarification: "Dichorionic Monoamniotic" Twins — Does This Exist?
"Dichorionic monoamniotic" is embryologically impossible under the standard fission model of twinning. This is a conceptually contradictory term, and likely represents either a trick question or a common source of confusion. Here's why:
Twin Classification: Chorionicity and Amnionicity
Chorionicity (number of placentas/chorions) and amnionicity (number of amniotic sacs) are both determined by the timing of zygote division in monozygotic (MZ) twinning:
| Timing of Division (after fertilization) | Chorionicity | Amnionicity | Frequency |
|---|---|---|---|
| Day 0–3 (before chorion forms) | Dichorionic | Diamniotic | ~70% of MZ twins |
| Day 3–9 (after chorion, before amnion) | Monochorionic | Diamniotic | ~25% of MZ twins |
| Day 8–12 (after both chorion & amnion) | Monochorionic | Monoamniotic | ~2% of MZ twins |
| Day 13–16 (incomplete splitting) | Monochorionic | Monoamniotic | Conjoined twins (1:100,000) |
— Creasy & Resnik's Maternal-Fetal Medicine, 9th ed., Chapter on Zygosity and Chorionicity
The key rule: For twins to share one amniotic sac (monoamniotic), they must already be sharing one chorion (monochorionic). You cannot have two separate chorions (dichorionic) yet share a single amnion — the amnion forms after the chorion during embryological development.
"Dichorionic monoamniotic" = does not occur naturally and is not a recognised twin type.
The Four Valid Twin Placentation Types
| Type | Chorions | Amnions | Zygosity |
|---|---|---|---|
| Dichorionic diamniotic (DCDA) | 2 | 2 | All DZ twins; 70% of MZ |
| Monochorionic diamniotic (MCDA) | 1 | 2 | MZ only (~25%) |
| Monochorionic monoamniotic (MCMA) | 1 | 1 | MZ only (~2%) |
| Conjoined twins | 1 | 1 | MZ only (rare) |
Monochorionic Monoamniotic (MCMA) Twins — Full Overview
Since this is the likely intended topic, here is the complete clinical picture:
Definition
Twins sharing one placenta + one amniotic sac, with no dividing membrane.
Pathogenesis
Division of the inner cell mass 8–12 days after fertilization, after both chorion and amnion have already formed. Occurs in ~1% of monozygotic gestations.
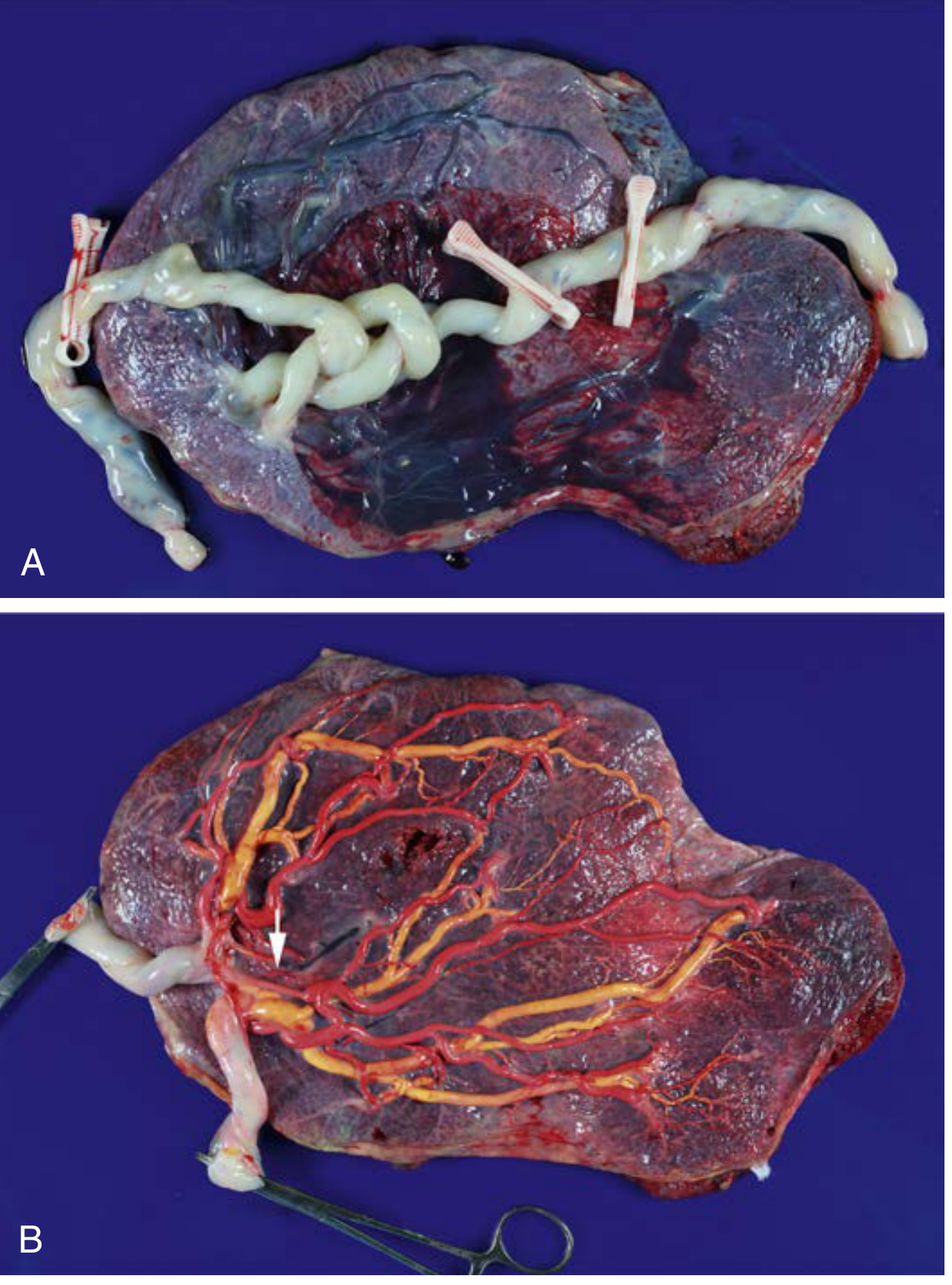
Placental Features
- Cord insertions are typically very close together on the chorionic plate
- Universal artery-to-artery (AA) and vein-to-vein (VV) anastomoses — large caliber, superficial
- Cords are almost always entangled (complex patterns)
- Cord abnormalities: single umbilical artery, furcate insertion, abnormal peripheral insertion
Prenatal Diagnosis
- No dividing membrane visualised on ultrasound by an experienced sonographer
- Cord entanglement confirmed by colour Doppler — detectable as early as 10 weeks' gestation (pathognomonic)
- Single yolk sac before 10 weeks (less specific; requires follow-up)
Complications
| Complication | Detail |
|---|---|
| Cord entanglement / cord accidents | Primary cause of fetal death — cord prolapse, cord compression |
| Perinatal mortality | Historically >50%; modern series 6% overall fetal loss; 2% at some centres |
| Twin-to-twin transfusion syndrome (TTTS) | Can occur; presents with polyhydramnios (common sac) + discordant bladder sizes |
| TRAP sequence | 1% of MZ twins; acardiac/acephalic perfused twin via AA anastomosis |
| Fetal growth restriction | Common |
| Congenital anomalies | Higher incidence than in dichorionic twins |
| Preterm delivery | Major source of morbidity |
Antenatal Management
- Intensive fetal surveillance from viability (~24 weeks), because cord accidents are unpredictable
- Daily NSTs from 24–26 weeks to monitor variable decelerations
- If variable decelerations increase → continuous CTG monitoring
- Inpatient vs. outpatient: The MONOMONO study (multicenter, retrospective) found a trend toward lower fetal demise with inpatient management (3.3% vs. 10.8%), but this was not significant on cluster analysis — evidence remains inconclusive
- Sulindac (prostaglandin inhibitor to reduce AFV and stabilise fetal lie) has been proposed theoretically but has no proven safety or efficacy
Delivery
- Timing: Elective caesarean section at 32–34 weeks after antenatal corticosteroids — recommended by ACOG
- Continuing beyond 34 weeks is difficult to justify given ongoing stillbirth risk and high neonatal survival at this gestational age
- Mode: Caesarean delivery is the standard once viability is reached; vaginal delivery is possible but high CS conversion rate
- Cord precautions: Case reports of cutting the nuchal cord of the second twin after first twin's head delivery
— Creasy & Resnik's Maternal-Fetal Medicine, 9th ed., Chapter 37: Monoamniotic Twins
Summary Points for Exam/Clinical Use
- "Dichorionic monoamniotic" — does not exist (common distractor in MCQs)
- Monoamniotic twins are always monochorionic (MCMA)
- Division occurs day 8–12 after fertilization
- Diagnostic hallmark on ultrasound: cord entanglement on colour Doppler
- Biggest risk: cord accidents (not TTTS — though TTTS can occur)
- Deliver at 32–34 weeks by caesarean section
- MCMA mortality was historically >50%; modern intensive surveillance has reduced this to ~2–6%
Diamniotic monochorionic twins
Finding Sources
Finding Sources
Reading File
Finding Sources
Finding Sources
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Finding Sources
Your credits are exhausted. Your daily credits reset tomorrow, or you can purchase a top-up for more.
This is a shared conversation. Sign in to Orris to start your own chat.