Frozen shoulder history and examination orthopaedics
Reading File
Finding Sources
Finding Sources
Searching the Web
frozen shoulder adhesive capsulitis history examination orthopaedics clinical features
Reading File
Reading File
Reading File
Reading File
Finding Sources
Finding Sources
Searching Images
frozen shoulder adhesive capsulitis examination range of motion
Reading File
Reading File
Loading Image
I now have comprehensive content from multiple authoritative orthopaedic textbooks. Let me compile a thorough answer.
Frozen Shoulder (Adhesive Capsulitis) — History & Examination
Definition
Frozen shoulder (adhesive capsulitis) is characterized by pain and restricted glenohumeral joint motion — both active and passive — due to inflammation and fibrosis of the joint capsule, particularly the coracohumeral ligament (CHL) and the rotator interval capsule. Histologically, there is a dense matrix of type III collagen containing fibroblasts and myofibroblasts, resembling findings in Dupuytren disease.
— Miller's Review of Orthopaedics, 9th Ed.
Epidemiology / Risk Factors
| Factor | Detail |
|---|---|
| Age | 40–70 years; rare before age 40 |
| Sex | More common in females |
| Side | Nondominant side more frequently affected |
| Associations | Diabetes mellitus, thyroid disease (disproportionately affected) |
| Secondary causes | Prolonged immobilization, post-mastectomy, Colles fracture, post-breast/chest surgery, stroke |
| Psychiatric | Depression and anxiety adversely affect symptoms and function |
Pathophysiology & Stages
The condition passes through four stages (not necessarily linear):
| Stage | Name | Timing | Key Features |
|---|---|---|---|
| 1 | Acute / Painful | 0–3 months | Acute synovial inflammation; pain limits movement |
| 2 | Freezing | 3–9 months | Capsular thickening and scarring; chronic pain; decreased ROM |
| 3 | Frozen | 9–15 months | Less pain but dense fibrotic capsule; maximum ROM restriction |
| 4 | Thawing | >15 months | Progressive ROM improvement; significant pain reduction |
Resolution typically occurs within 1–3 years, though many patients are left with residual limitation.
— Tintinalli's Emergency Medicine; Goldman-Cecil Medicine
History
Key points to elicit:
- Onset — insidious, gradual onset of diffuse shoulder pain (weeks to months). Sometimes rapid progression.
- Character of pain — diffuse, aching, poorly localized; radiates down the upper arm over the deltoid area.
- Night pain — characteristically worse at night, interfering with sleep; also worse at rest in early stages.
- Stiffness — progressive restriction of all shoulder movements. The patient notices difficulty with activities of daily living (e.g., reaching behind the back to fasten a bra, combing hair, reaching overhead).
- Dominant / non-dominant — clarify which arm is affected (nondominant more common).
- Precipitating factors — prior shoulder injury, immobilization, recent surgery, sling use.
- Relevant medical history — diabetes (ask about glucose control/HbA1c), thyroid disorders, autoimmune conditions, pulmonary history.
- Psychosocial — depression/anxiety (relevant to prognosis).
- Previous treatment — physiotherapy, injections, NSAIDs, and their response.
Examination
Inspection
- Muscle wasting (deltoid, supraspinatus, infraspinatus) — from disuse
- No gross deformity; shoulder contour usually normal
- Observe scapular compensatory movement during attempted arm elevation
Palpation
- Diffuse tenderness around the shoulder joint
- No specific point tenderness (unlike rotator cuff tendinopathy, where supraspinatus insertion is tender)
Range of Motion — THE KEY FINDING
The hallmark of frozen shoulder is globally restricted ROM — equally in active and passive testing (active = passive, because restriction is mechanical/capsular, not muscular):
| Movement | Finding |
|---|---|
| External rotation | Most restricted first — classic early finding (capsular pattern) |
| Abduction | Significantly limited |
| Internal rotation | Restricted (patient cannot reach mid-thoracic level behind the back) |
| Forward flexion | Restricted — typically <100° in full frozen stage |
"Diagnosis is clinical — typically an insidious onset of pain followed by selective loss of external rotation; in later stages, global ROM loss occurs; classically, active ROM and passive ROM are equivalent." — Miller's Review of Orthopaedics, 9th Ed.
Important: On passive external rotation testing, a mechanical restriction / hard end-feel (capsular end-feel) is felt — not a pain-limited end-feel.
Special Tests / Functional Assessment
- Apley scratch test — limited internal rotation; patient cannot reach dorsal midline on affected side
- External rotation (arms at sides) — compare bilateral ER; restriction is pathognomonic in early disease
- Impingement tests (Hawkins-Kennedy, Neer) — difficult to perform and interpret due to global ROM restriction
- Cervical spine exam — must be performed to exclude cervical radiculopathy as a cause of shoulder pain/stiffness
Neurovascular
- Normal sensation and power in myotomal distribution (rules out cervical pathology, brachial plexopathy)
- Normal distal pulses
Clinical Photograph — ROM Restriction
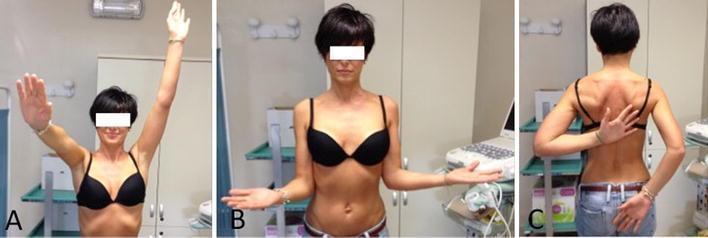
Panels A–C: Asymmetric ROM in frozen shoulder — restricted elevation (A), bilateral external rotation assessment (B), and the Apley scratch test showing significant internal rotation deficit on the affected side (C).
Investigations
| Investigation | Findings |
|---|---|
| Plain radiograph (X-ray) | Usually normal — but mandatory to exclude glenohumeral OA and locked posterior dislocation (which also cause ER loss) |
| Arthrography | Loss of the normal axillary recess — confirms capsular contracture; decreased joint volume |
| MRI | Thickening of GHJ capsule at axillary pouch, thickening of CHL, obliteration of subcoracoid fat triangle, rotator interval synovitis — none pathognomonic |
| Ultrasound | Increased vascular flow, thickening of rotator cuff structures — supportive |
"Two other causes of selective loss of external rotation are glenohumeral osteoarthritis and a locked posterior shoulder dislocation — for this reason, radiographs must be obtained before a diagnosis of frozen shoulder is made." — Miller's Review of Orthopaedics, 9th Ed.
Differential Diagnosis
- Glenohumeral osteoarthritis — bony crepitus, X-ray changes
- Locked posterior dislocation — history of seizure/trauma, X-ray abnormal
- Rotator cuff tear — passive ROM preserved, active restricted; positive lag signs
- Calcific tendinitis — acute severe pain, calcification on X-ray
- Cervical radiculopathy — dermatomal/myotomal distribution, neck movements reproduce pain
- Shoulder impingement — ROM less globally restricted; positive Hawkins-Kennedy/Neer
Key Diagnostic Criterion
Adhesive capsulitis is a clinical diagnosis based on history and examination, and by excluding other causes of shoulder pain and stiffness. There are no pathognomonic imaging findings.
Sources: Miller's Review of Orthopaedics 9th Edition; Goldman-Cecil Medicine; Harrison's Principles of Internal Medicine 22E; Tintinalli's Emergency Medicine; Rosen's Emergency Medicine
This is a shared conversation. Sign in to Orris to start your own chat.