APPENDICITIS
Reading File
Finding Sources
Searching PubMed
"appendicitis"[MeSH Terms] AND ("diagnosis" OR "management")
Searching Images
appendicitis anatomy pathology CT scan
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
I have excellent comprehensive coverage. Let me now compile the full, well-organized response on appendicitis.
APPENDICITIS
Overview & Epidemiology
Appendicitis is the most common intra-abdominal surgical emergency, affecting ~1 per 1,000 adults annually worldwide. Lifetime risk is 7–10% (8.7% men, 6.9% women). In the United States, ~400,000 cases are diagnosed per year, with 16–40% presenting with perforation. Peak incidence is ages 9–12 years; it is uncommon under age 5 but carries the highest perforation rate in that group (>50% ruptured at surgery).
- Current Surgical Therapy 14e | Goldman-Cecil Medicine | Rosen's Emergency Medicine
Anatomy
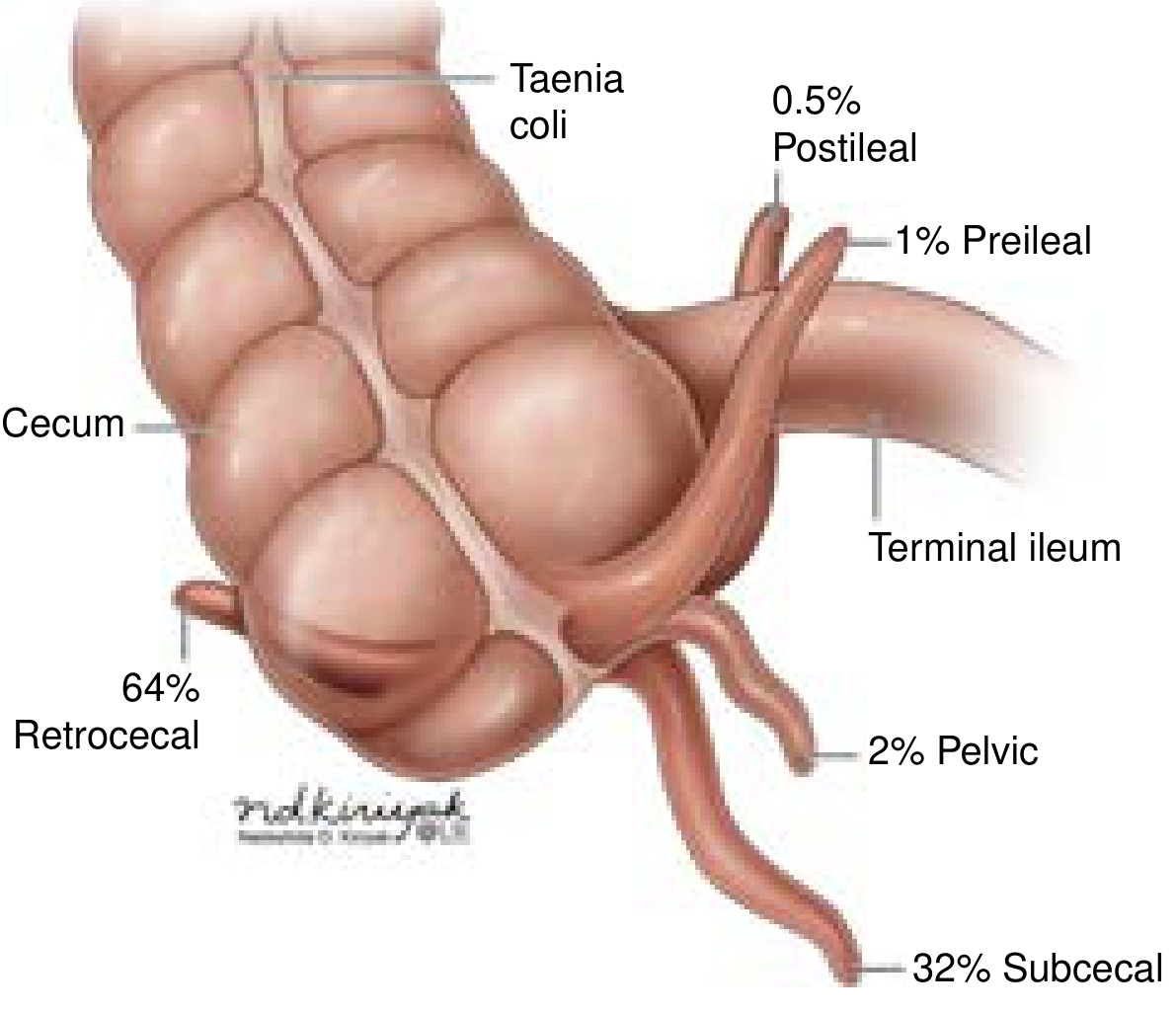
The appendix is an ~9 cm long, 0.6 cm wide vermiform ("worm-shaped") hollow structure arising from the terminal cecum, at the convergence of the three taenia coli. While the base is consistently cecal, the tip position varies widely:
- Retrocecal (most common, ~65%)
- Pelvic / subcecal
- Pre-ileal / post-ileal
This positional variability explains the diversity of clinical presentations. Blood supply: appendiceal artery, a branch of the ileocolic artery (branch of superior mesenteric artery).
Pathophysiology
The central mechanism is luminal obstruction → bacterial overgrowth → progressive ischemia → perforation.
Causes of obstruction:
| Cause | Notes |
|---|---|
| Fecalith / appendicolith | Most common |
| Lymphoid hyperplasia | Common in children (viral infections) |
| Neoplasm | Carcinoid, mucocele |
| Parasites | Enterobius, Ascaris |
| Foreign body | Less common |
Sequence of events:
- Obstruction → increased intraluminal pressure
- Mucus accumulation, bacterial overgrowth (E. coli, B. fragilis, Klebsiella, Streptococcus, Enterococcus, Pseudomonas)
- Venous congestion → distension → visceral pain (periumbilical)
- Arterial ischemia → necrosis → gangrene
- Perforation → local abscess or diffuse peritonitis
Children have thinner appendiceal walls and underdeveloped omentum → perforation occurs earlier and diffuse peritonitis develops more readily.
- Current Surgical Therapy 14e
Clinical Features
Classic Presentation
- Anorexia (often earliest symptom)
- Nausea and vomiting
- Periumbilical pain initially (visceral, colicky) → migrates to RLQ (McBurney's point) within hours as parietal peritoneum becomes involved
- Low-grade fever (develops later; high fever suggests perforation/abscess)
- Progressive worsening over 24–72 hours
McBurney's point: two-thirds of the distance from the umbilicus to the right anterosuperior iliac spine.
Physical Examination Signs
| Sign | How to Elicit | Significance |
|---|---|---|
| McBurney's tenderness | Direct palpation at McBurney's point | Most reliable |
| Rovsing's sign | Palpation of LLQ causes RLQ pain | Peritoneal irritation |
| Psoas sign | Pain with extension of right hip (patient prone) or flexion against resistance | Retrocecal appendix |
| Obturator sign | Pain with internal rotation of flexed right hip | Pelvic appendix |
| Dunphy's sign | Increased RLQ pain with coughing | Peritonitis |
| Heel-tap sign | RLQ pain when patient drops from tiptoes | Peritoneal irritation |
| Rebound tenderness | Sudden release of pressure causes pain | Peritoneal irritation |
| Guarding / rigidity | Involuntary muscle spasm | Peritonitis |
Important caveats: Rovsing, psoas, and obturator signs have poor sensitivity/specificity, especially in young children. Classic signs may be absent in retrocecal appendicitis, elderly patients, immunosuppressed patients, and pregnant women.
- Rosen's Emergency Medicine | Textbook of Family Medicine 9e
Differential Diagnosis
Surgical causes: Intestinal obstruction, intussusception, acute cholecystitis, Meckel's diverticulitis, mesenteric adenitis, ovarian torsion, ectopic pregnancy
Gynecological: Pelvic inflammatory disease, ovarian cyst (ruptured/torsion), endometriosis, mittelschmerz
Medical/other: Urinary tract infection, right ureteral stone, psoas abscess, right-sided pneumonia, Crohn's disease, gastroenteritis, constipation
- Goldman-Cecil Medicine, Table 128-1
Diagnostic Workup
Laboratory Tests
No single test is diagnostic. Typical findings:
- WBC >10,000/μL (in 87–92% of cases) but <18,000/μL unless perforation has occurred; left shift
- CRP elevated (>0.6 mg/dL sensitive; highly elevated suggests perforation/abscess)
- Procalcitonin: elevated with complicated appendicitis
- Urinalysis: mild sterile pyuria (<5–10 WBC/hpf) possible due to ureteral inflammation; does not exclude appendicitis
- β-hCG: mandatory in women of reproductive age to exclude ectopic pregnancy
Clinical Scoring Systems
Alvarado Score (MANTRELS):
| Feature | Points |
|---|---|
| Migration of pain to RLQ | 1 |
| Anorexia | 1 |
| Nausea/vomiting | 1 |
| RLQ tenderness | 2 |
| Rebound tenderness | 1 |
| Elevated temperature (>37.3°C) | 1 |
| Leukocytosis (WBC >10,000) | 2 |
| Left shift | 1 |
| Total | 10 |
Interpretation: ≤4 = unlikely; 5–6 = possible; 7–8 = probable; 9–10 = very likely.
Other validated systems: Pediatric Appendicitis Score (PAS), Adult Appendicitis Score, Appendicitis Inflammatory Response (AIR) score.
Imaging
| Modality | Sensitivity | Specificity | Notes |
|---|---|---|---|
| CT (multidetector, low-dose) | ≥94% | ≥94% | Preferred in adults and obese patients; can detect perforation and complications |
| Ultrasound | ~83% | ~93% | First-line in children and pregnant women; non-compressible appendix >6 mm is diagnostic; operator-dependent |
| MRI | Comparable to CT | Comparable to CT | Preferred in pregnancy (avoids radiation); good alternative |
| Plain X-ray | Low | Low | Not diagnostic; may show appendicolith, ileus, RLQ soft tissue density |
CT findings in appendicitis:
- Dilated appendix >6 mm diameter
- Appendiceal wall thickening and enhancement
- Periappendiceal fat stranding
- Appendicolith (seen in ~30%)
- Periappendiceal abscess (with perforation)
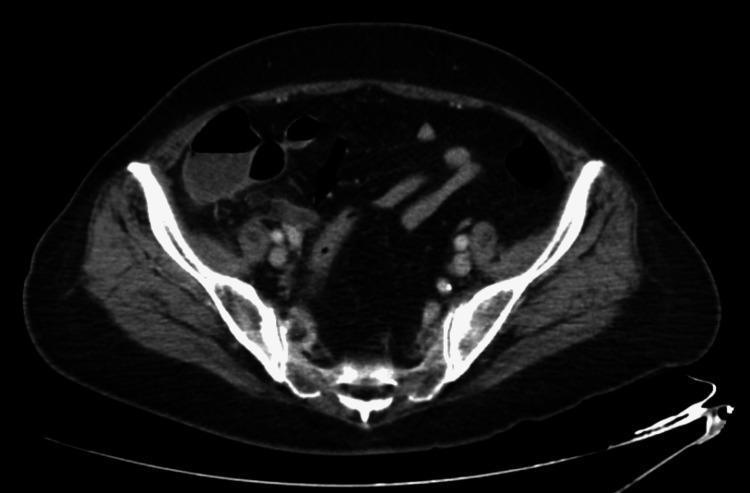
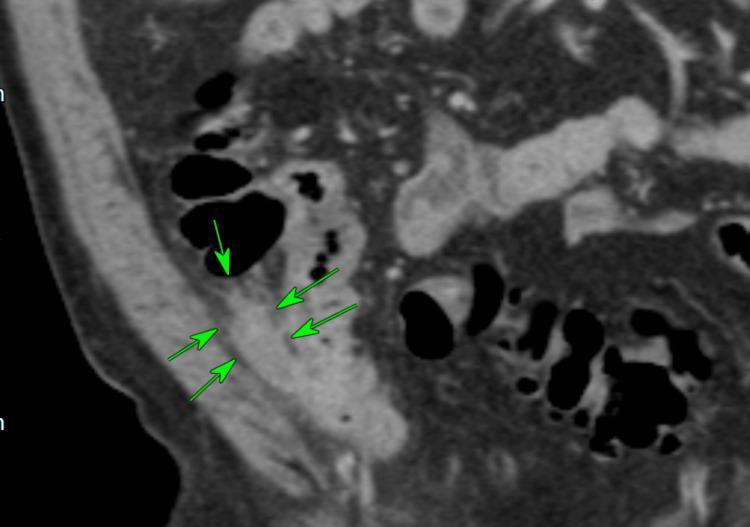
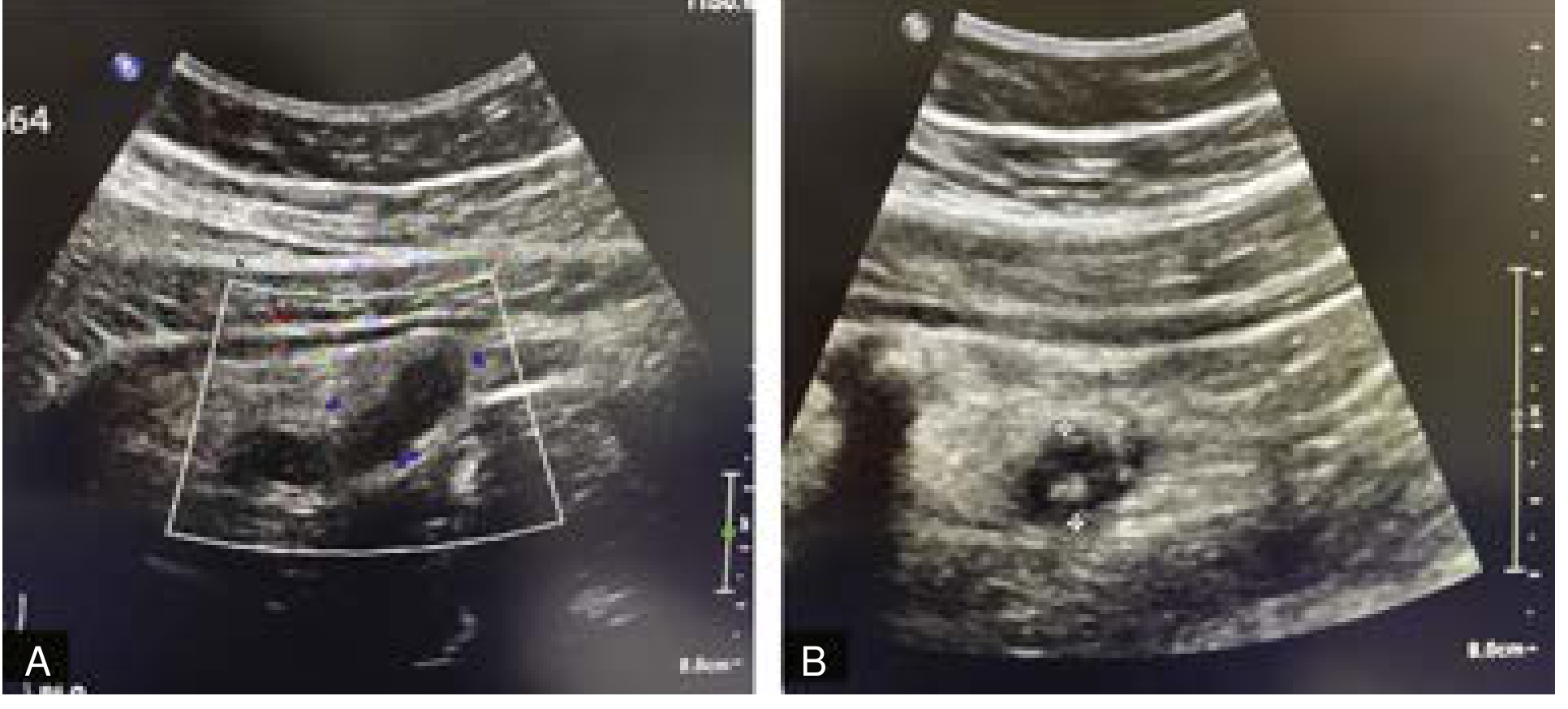
- Goldman-Cecil Medicine | Current Surgical Therapy 14e | Rosen's Emergency Medicine
Classification
| Type | Features |
|---|---|
| Simple (uncomplicated) | Inflamed but intact; no necrosis, perforation, or abscess |
| Gangrenous | Necrosis of appendiceal wall; almost always associated with luminal obstruction |
| Perforated | Full-thickness rupture; risk of peritonitis or abscess |
| Phlegmon / Abscess | Walled-off perforation; mass palpable in RLQ |
Management
Preoperative
- IV fluids and electrolyte correction
- NPO
- Preoperative antibiotics (reduce infectious complications in uncomplicated disease):
- Cefotetan 2 g IV, or Cefoxitin 2 g IV (3 postoperative doses for uncomplicated disease)
- Piperacillin-tazobactam or ticarcillin-clavulanic acid for complicated/perforated
- Target: E. coli, Bacteroides (gram-negative aerobes + anaerobes)
Operative Management
Laparoscopic appendectomy is now the standard of care for most cases:
- Lower rate of postoperative complications vs. open
- Faster return to normal activity and diet
- Appropriate for: uncomplicated and most complicated appendicitis
Open appendectomy (McBurney's / Gridiron incision):
- Preferred when perforation is evident preoperatively
- McBurney's incision: oblique through McBurney's point; muscle-splitting (gridiron)
- Remains essential skill for surgeons
Interval appendectomy: For patients who present with phlegmon/abscess after >5 days of symptoms → nonoperative management first (IV antibiotics ± percutaneous drainage by interventional radiology), followed by interval appendectomy at 6–8 weeks.
Nonoperative (Antibiotic-Only) Management
Growing evidence supports antibiotics alone for uncomplicated appendicitis:
-
~80–90% symptom resolution within 24–48 hours
-
2025 WSES Jerusalem Guidelines and 2024 SAGES Guidelines acknowledge this as a viable alternative
-
Recurrence rate ~25–40% at 5 years (higher in children)
-
Contraindicated if: fecalith/appendicolith present, perforation, immunocompromised, unable to comply with follow-up
-
Most surgeons still prefer operative management as definitive treatment
-
Current Surgical Therapy 14e | Goldman-Cecil Medicine | SAGES 2024 [PMID: 38740595] | WSES 2025 [PMID: 41604201]
Complications
| Complication | Features |
|---|---|
| Perforation | Increases mortality 0.0002% → 3%; morbidity 3% → 47% |
| Peritonitis | Diffuse or localized; requires broad-spectrum antibiotics + surgery |
| Periappendiceal abscess | Walled-off perforation; drain percutaneously if accessible |
| Wound infection | More common after open or contaminated surgery |
| Ileus / adhesions | Post-surgical bowel obstruction |
| Pylephlebitis | Septic portal vein thrombosis (rare but serious) |
| Stump appendicitis | Inflammation of residual appendiceal stump after appendectomy |
Special Populations
Children
- Perforation rate inversely correlates with age; >50% perforation rate in children <5 years
- US and MRI preferred (avoid radiation)
- Nonoperative management acceptable in select cases; recurrence up to 40%
- Same-day discharge possible after laparoscopic appendectomy in early disease
Pregnancy
- Most common surgical emergency in pregnancy (same incidence as non-pregnant)
- Diagnosis challenging: displaced appendix (tip moves to RUQ by third trimester in <25% of cases), physiologic leukocytosis and elevated ESR
- MRI preferred imaging (avoids fetal radiation)
- Perforation → increased risk of sepsis, fetal mortality, preterm labor
- Laparoscopic appendectomy safe throughout all trimesters
Elderly
- Atypical presentation common; diagnosis often delayed
- Higher perforation rate at presentation (~70%)
- Higher mortality and morbidity
Prognosis
- Uncomplicated appendicitis: mortality ~0.0002%; full recovery expected
- Perforated appendicitis: mortality ~3%; morbidity ~47%
- Laparoscopic vs. open: laparoscopic carries lower wound infection rate, shorter hospital stay
Recent Guidelines (2024–2025)
| Guideline | Key Recommendation |
|---|---|
| SAGES 2024 [PMID: 38740595] | Laparoscopic appendectomy preferred; antibiotics-first is a valid option for uncomplicated disease in selected patients |
| WSES Jerusalem Guidelines 2025 [PMID: 41604201] | Updated diagnostic and management algorithms; CT preferred for adults; nonoperative management supported for uncomplicated, fecalith-free appendicitis |
Sources: Current Surgical Therapy 14e | Rosen's Emergency Medicine | Goldman-Cecil Medicine | Textbook of Family Medicine 9e | Gray's Anatomy for Students | SAGES 2024 [PMID 38740595] | WSES 2025 [PMID 41604201]
Definition Etiology Pathophysiology ( chart form) Clinical features Types Diagnosis/ investigation Management ( table form) Medical management Surgical management Algorithm to approach appendicitis (chart form) with arrow Of appendicitis
Finding Sources
Finding Sources
Reading File
Reading File
Finding Sources
Reading File
Reading File
Reading File
I now have all the content needed. Let me compile the comprehensive, structured response exactly as requested.
APPENDICITIS — Structured Clinical Reference
1. DEFINITION
Appendicitis is an acute inflammation of the vermiform appendix — a blind-ended tubular structure arising from the cecum — resulting from luminal obstruction, bacterial overgrowth, and progressive ischemic injury to the appendiceal wall.
It is the most common intra-abdominal surgical emergency worldwide, responsible for ~300,000–400,000 hospitalizations annually in the United States, with a lifetime risk of 6–10% in the general population.
Sabiston Textbook of Surgery | Goldman-Cecil Medicine
2. ETIOLOGY
Primary Cause: Luminal Obstruction
| Cause | Details |
|---|---|
| Fecalith / Appendicolith | Most common; hardened stool or calcified concretion; ~1/3 of cases |
| Lymphoid hyperplasia | Common in children/adolescents following viral infections (adenovirus, EBV) |
| Neoplasms | Carcinoid tumor, mucinous adenocarcinoma, carcinoma |
| Parasites | Enterobius vermicularis (pinworm), Ascaris lumbricoides |
| Foreign body | Ingested material, vegetable seeds, barium |
| Fecal stasis | Low-fiber, high-fat (Western) diet implicated epidemiologically |
| Stricture / adhesion | Post-inflammatory scarring |
Bacteriology (polymicrobial)
- Escherichia coli
- Bacteroides fragilis
- Klebsiella pneumoniae
- Enterococcus spp.
- Pseudomonas aeruginosa
- Streptococcus spp.
Sabiston Textbook of Surgery | Current Surgical Therapy 14e
3. PATHOPHYSIOLOGY (Flow Chart)
LUMINAL OBSTRUCTION
(fecalith, lymphoid hyperplasia, neoplasm, parasite)
│
▼
INCREASED INTRALUMINAL PRESSURE
(mucus secretion + bacterial gas production continue)
│
▼
VENOUS CONGESTION & LYMPHATIC OBSTRUCTION
(visceral afferent nerve fibers stretched)
│
▼
VAGUE PERIUMBILICAL / EPIGASTRIC PAIN
(T10 dermatome, colicky, visceral)
│
▼
BACTERIAL OVERGROWTH & MUCOSAL ISCHEMIA
(E. coli, B. fragilis, Klebsiella, Pseudomonas)
│
▼
TRANSMURAL INFLAMMATION
(appendiceal wall becomes full-thickness inflamed)
│
▼
PARIETAL PERITONEUM INVOLVED
│
▼
LOCALIZED SOMATIC PAIN → RLQ (McBurney's point)
+ Fever, guarding, rigidity
│
▼
┌───────┴────────┐
▼ ▼
UNCOMPLICATED ARTERIAL ISCHEMIA
APPENDICITIS → FULL-THICKNESS NECROSIS
(inflamed but (Gangrenous appendicitis)
intact) │
▼
PERFORATION
┌──────┴──────┐
▼ ▼
LOCALIZED FREE PERFORATION
ABSCESS / (Diffuse peritonitis,
PHLEGMON sepsis, death)
Sabiston Textbook of Surgery | Current Surgical Therapy 14e
4. CLINICAL FEATURES
Symptoms
| Symptom | Description |
|---|---|
| Anorexia | Earliest and most consistent symptom |
| Periumbilical pain | Initial visceral pain — vague, colicky |
| Migration of pain to RLQ | Hallmark; occurs over 12–24 h as parietal peritoneum becomes involved |
| Nausea & vomiting | Usually follows pain onset |
| Low-grade fever | 37.5–38.5°C; high fever (>39°C) suggests perforation |
| Constipation / diarrhea | Variable; tenesmus possible with pelvic appendix |
Signs
| Sign | Method | Significance |
|---|---|---|
| McBurney's tenderness | Direct palpation 2/3 from umbilicus to ASIS | Most reliable RLQ finding |
| Guarding / rigidity | Involuntary abdominal wall spasm | Peritoneal irritation |
| Rebound tenderness (Blumberg's) | Sudden release of deep pressure → pain | Peritonitis |
| Rovsing's sign | LLQ palpation → RLQ pain | Refers peritoneal irritation |
| Psoas sign | Pain on right hip extension (patient prone) or active flexion against resistance | Retrocecal appendix |
| Obturator sign | Pain with internal rotation of flexed right hip | Pelvic appendix |
| Dunphy's (cough) sign | RLQ pain increased by coughing | Peritonitis |
| Heel-drop test | Patient drops from tiptoes → RLQ pain | Peritoneal irritation |
| Rigidity / Board-like abdomen | Involuntary muscle guarding | Perforated / diffuse peritonitis |
Rosen's Emergency Medicine | Textbook of Family Medicine 9e | Sabiston Textbook of Surgery
5. TYPES / CLASSIFICATION
By Acuity
| Type | Features |
|---|---|
| Acute appendicitis | Evolves over hours to days; most common presentation |
| Chronic / Recurrent appendicitis | Symptoms spanning weeks to months; low-grade, intermittent pain |
By Severity (most clinically important)
| Type | Pathology | Key Features |
|---|---|---|
| Simple (Uncomplicated) | Inflamed appendix, wall intact, no necrosis | RLQ pain, fever, leukocytosis; no perforation |
| Gangrenous | Full-thickness wall necrosis | More severe pain; almost always associated with fecalith; pre-perforation state |
| Perforated | Transmural rupture | High fever, peritonism, sepsis; two subtypes below |
| Appendiceal Phlegmon | Contained inflammatory mass | Palpable RLQ mass; present after ≥5 days of symptoms |
| Periappendiceal Abscess | Walled-off pus collection | Mass, swinging fever; amenable to percutaneous drainage |
| Diffuse Peritonitis | Free perforation, peritoneal soilage | Generalized rigidity, sepsis, high mortality |
Sabiston Textbook of Surgery | Current Surgical Therapy 14e
6. DIAGNOSIS / INVESTIGATIONS
Clinical Scoring: Alvarado Score (MANTRELS)
| Feature | Score |
|---|---|
| Migration of pain to RLQ | 1 |
| Anorexia | 1 |
| Nausea / vomiting | 1 |
| Tenderness in RLQ | 2 |
| Rebound tenderness | 1 |
| Elevated temperature (>37.3°C) | 1 |
| Leukocytosis (WBC >10,000) | 2 |
| Shift to left (neutrophilia) | 1 |
| Total | 10 |
Interpretation: ≤4 = Appendicitis unlikely | 5–6 = Possible | 7–8 = Probable | 9–10 = Highly likely
Other scores: Pediatric Appendicitis Score (PAS), Appendicitis Inflammatory Response (AIR) Score, Adult Appendicitis Score
Laboratory Investigations
| Test | Expected Finding | Notes |
|---|---|---|
| WBC count | >10,000/μL; usually <18,000 | Elevated in 87–92%; left shift (neutrophilia) |
| CRP | Elevated (>0.6 mg/dL) | Highly elevated → perforation/abscess |
| Procalcitonin | Elevated | Indicates complicated/perforated disease |
| Urinalysis | Mild sterile pyuria possible | ≤5–10 WBC/hpf; bacteria absent; from ureteral irritation |
| β-hCG (serum/urine) | Negative | Mandatory in all women of reproductive age |
| Blood cultures | Positive in sepsis | Needed if systemic infection suspected |
| Electrolytes / BMP | Disturbances with vomiting | Baseline for surgical planning |
| LFTs / Lipase | Normal (helps exclude biliary/pancreatic) | Part of differential workup |
Imaging Investigations
| Modality | Sensitivity | Specificity | When to Use |
|---|---|---|---|
| CT Abdomen/Pelvis (MDCT) | ≥94% | ≥94% | Gold standard in adults; low-dose (2 mSv); detects perforation, abscess, alternative diagnoses |
| Ultrasound (RLQ) | ~83% | ~93% | First-line in children and pregnant women; non-compressible appendix >6 mm diagnostic; operator-dependent |
| MRI Abdomen | ~95% | ~95% | Preferred in pregnancy (no radiation); safe, accurate |
| Plain X-ray (AXR) | Low | Low | Not routinely used; may show appendicolith, air-fluid levels, RLQ soft tissue density |
CT Diagnostic Criteria:
- Appendix diameter >6 mm
- Appendiceal wall thickening + enhancement
- Periappendiceal fat stranding
- Appendicolith (30% of cases)
- Periappendiceal fluid / abscess (with perforation)
- "Target sign": thickened, fluid-filled appendix (sagittal view)
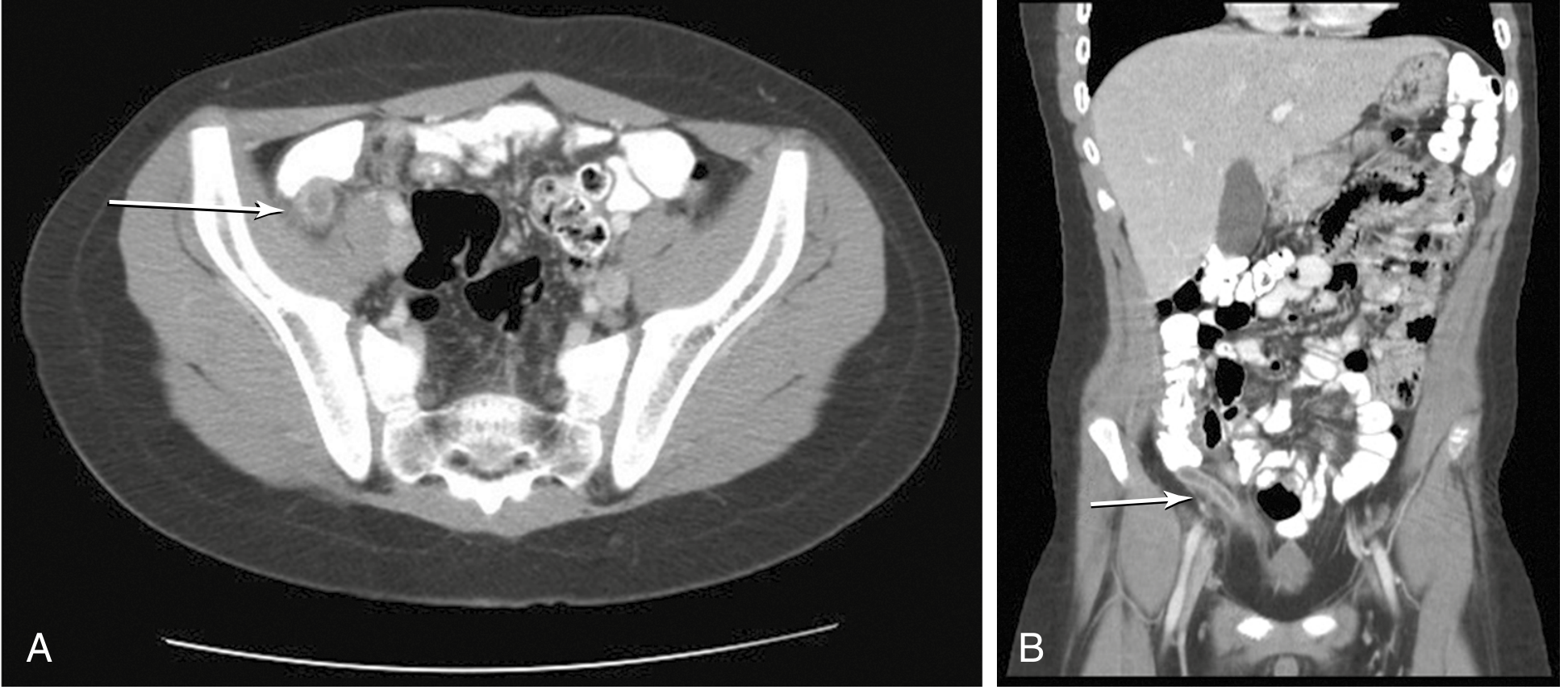

Goldman-Cecil Medicine | Sabiston Textbook of Surgery | Current Surgical Therapy 14e
7. MANAGEMENT (Table Form)
Overview by Type
| Type of Appendicitis | Management Strategy |
|---|---|
| Uncomplicated (simple) | Laparoscopic appendectomy OR antibiotics-first (shared decision making) |
| Gangrenous | Laparoscopic appendectomy (urgent) |
| Perforated with diffuse peritonitis | Emergency open or laparoscopic appendectomy + peritoneal lavage |
| Perforated with abscess (<5 days) | Laparoscopic appendectomy + drainage |
| Phlegmon / Abscess (>5 days symptoms) | Nonoperative: IV antibiotics ± percutaneous drain → Interval appendectomy 6–8 weeks |
| Chronic/recurrent | Elective laparoscopic appendectomy |
A. MEDICAL MANAGEMENT
| Component | Details |
|---|---|
| IV Fluid Resuscitation | Normal saline or Lactated Ringer's to correct dehydration and electrolyte imbalances |
| NPO | Nothing by mouth in anticipation of surgery or while monitoring |
| Analgesia | IV opioids (morphine, fentanyl) — does NOT mask diagnosis; provide adequate pain relief |
| Antiemetics | Ondansetron, metoclopramide for nausea/vomiting |
| Antipyretics | Paracetamol / NSAIDs for fever management |
| Preoperative antibiotics | Single dose within 60 min of incision (reduces surgical site infections) |
Antibiotic Regimens
| Setting | First-Line | Alternatives |
|---|---|---|
| Uncomplicated (prophylaxis) | Cefotetan 2 g IV OR Cefoxitin 2 g IV | Cefazolin + metronidazole |
| Complicated / Perforated | Piperacillin-tazobactam 3.375 g IV q6h | Ticarcillin-clavulanate; Meropenem (severe) |
| Antibiotics-only (nonoperative) | Ertapenem 1 g IV daily OR Ceftriaxone + metronidazole | Amoxicillin-clavulanate (oral step-down) |
| Penicillin allergy | Ciprofloxacin + metronidazole | Aztreonam + metronidazole |
Duration:
- Uncomplicated: single preoperative dose (3 doses post-op max)
- Complicated/perforated: 3–5 days IV then consider oral step-down based on clinical response
- Nonoperative (antibiotics-only): 7–10 days (IV 24–48 h → oral)
Nonoperative (Antibiotics-Only) — Indications & Criteria
| Factor | Suitable for Nonoperative | NOT Suitable |
|---|---|---|
| Appendicolith | No | Yes (higher failure/complication rate) |
| Imaging | Uncomplicated, no abscess | Perforation, free air, abscess |
| Age | Adults, select pediatric | Very young children |
| Recurrence risk | Counseled (~25–40% at 5 years) | Refused by patient |
| Comorbidities | Low surgical risk prefers nonop | High surgical risk |
Sabiston Textbook of Surgery (CODA trial, APPAC trial) | Current Surgical Therapy 14e
B. SURGICAL MANAGEMENT
Laparoscopic Appendectomy (Standard of Care)
| Step | Details |
|---|---|
| Position | Supine; left arm tucked; possible reverse Trendelenburg + right side up |
| Access | Veress needle (closed) or Hasson technique (open) through umbilicus |
| Insufflation | CO₂ to 12–15 mmHg |
| Port placement | Umbilical camera port (10–12 mm) + 2 working ports (5 mm) in LLQ / suprapubic |
| Procedure | Identify cecum → follow taenia coli to appendix base → divide mesoappendix (stapler/LigaSure) → staple/ligate appendix base → place in retrieval bag → remove |
| Irrigation | Pelvic irrigation if contamination present; consider cultures |
| Advantages | Lower wound infection rate, faster recovery, shorter hospital stay, diagnostic capability |
Open Appendectomy
| Step | Details |
|---|---|
| Incision | McBurney's (gridiron): oblique muscle-splitting incision at McBurney's point |
| Alternative | Lanz (transverse) incision for better cosmesis |
| Preferred when | Perforation with peritonitis; technical failure of laparoscopy; laparoscopy unavailable |
| Technique | Identify cecum → mesoappendix ligated and divided → appendix base doubly ligated → appendix excised → stump inverted (optional) |
Interval Appendectomy
| Indication | Timing | Route |
|---|---|---|
| Phlegmon or abscess (>5 days) managed nonoperatively | 6–8 weeks after resolution | Elective laparoscopic |
Percutaneous Drainage (IR-guided)
- For periappendiceal abscess amenable to drainage
- Performed by interventional radiology
- Followed by interval appendectomy at 6–8 weeks
- Not appropriate if no safe window, peritonitis, or free perforation
Sabiston Textbook of Surgery | Current Surgical Therapy 14e | Goldman-Cecil Medicine
8. ALGORITHM TO APPROACH APPENDICITIS
PATIENT PRESENTS WITH ACUTE ABDOMINAL PAIN
│
▼
HISTORY & PHYSICAL EXAMINATION
(Pain migration, anorexia, RLQ tenderness,
fever, guarding, Rovsing/Psoas/Obturator signs)
│
▼
CALCULATE ALVARADO SCORE
┌──────────┼──────────┐
▼ ▼ ▼
SCORE ≤4 SCORE 5–6 SCORE ≥7
(Unlikely) (Equivocal) (Probable)
│ │ │
▼ │ ▼
Consider IMAGING LABS + IMAGING
Alternatives │ (CBC, CRP, PCT)
Discharge if ┌────┴─────┐ │
well │ │ │
ULTRASOUND CT CT ABDOMEN
(children, (adults, /PELVIS
pregnant) obese)
│
┌───────┴────────┐
▼ ▼
CT NEGATIVE CT POSITIVE
(Appendix normal) (Appendicitis confirmed)
│ │
▼ ▼
Observe / Admit DETERMINE TYPE
Re-evaluate │
Consider alt Dx ┌────────┴─────────┐
▼ ▼
UNCOMPLICATED COMPLICATED
(No perforation, (Perforation / Abscess /
no gangrene) Phlegmon / Peritonitis)
│ │
┌─────────┴──────┐ ┌──────┴──────┐
▼ ▼ ▼ ▼
APPENDECTOMY ANTIBIOTICS DURATION FREE
(Laparoscopic, -ONLY OF Sx <5d PERFORATION
Gold standard) (selected, Appendectomy /PERITONITIS
│ no fecalith) ± Drainage │
▼ │ │ ▼
PREOP ABX Ertapenem DURATION Sx ≥5d EMERGENCY
+ Resuscitation IV 24–48h ┌────────────┐ OPEN / LAP
│ → Oral 7–10d │ IV ABX + │ APPENDECTOMY
▼ │ │Percutaneous│ + LAVAGE
SURGERY MONITOR │ Drainage │
│ (Failure? │ │
▼ → Surgery)└────────────┘
POST-OP CARE │
(Uncomplicated: ▼
same-day/next-day INTERVAL APPENDECTOMY
discharge; at 6–8 WEEKS
Complicated:
IV ABX 3–5 days)
Sources: Sabiston Textbook of Surgery | Current Surgical Therapy 14e | Rosen's Emergency Medicine | Goldman-Cecil Medicine | Textbook of Family Medicine 9e | SAGES Guidelines 2024 [PMID 38740595] | WSES Jerusalem Guidelines 2025 [PMID 41604201]
This is a shared conversation. Sign in to Orris to start your own chat.