Neurocysticercosis
Reading File
Finding Sources
Searching PubMed
neurocysticercosis diagnosis treatment
Reading File
Reading File
Reading File
Searching Images
neurocysticercosis MRI brain cyst scolex
Reading File
Reading File
Reading File
Loading Image
Loading Image
Here is a comprehensive review of neurocysticercosis (NCC):
Neurocysticercosis (NCC)
Definition & Etiology
Neurocysticercosis is a CNS infection caused by the larval stage (cysticercus) of Taenia solium, the pork tapeworm. It is the most common parasitic disease of the human CNS and the most common cause of symptomatic/acquired epilepsy worldwide.
Humans become infected by ingesting T. solium eggs (not larvae) via:
- Fecal-oral contamination from a tapeworm carrier (including auto-infection)
- Contaminated food or water
The ingested eggs hatch in the intestine → oncospheres penetrate the intestinal wall → disseminate hematogenously → lodge in the CNS, muscles, eye, and subcutaneous tissue → develop into cysticerci over 2–3 months.
Epidemiology
- Endemic in Latin America, sub-Saharan Africa, South and Southeast Asia, Eastern Europe
- Most common cause of adult-onset epilepsy in endemic regions
- Estimated 0.45–1.35 million epilepsy cases due to NCC in Latin America; ~1 million in India; 0.31–4.6 million in Africa
- Increasingly important in the US due to immigration: estimated 1,320–5,050 new cases/year; 33,060 cysticercosis-related hospitalizations from 1998–2011
Life Cycle and Pathophysiology
| Step | Detail |
|---|---|
| Ingestion of eggs | T. solium eggs in contaminated food/water/fecal matter |
| Oncosphere penetration | Hatches in small intestine, crosses intestinal wall |
| Hematogenous spread | Oncospheres travel to CNS, muscle, eye, subcutaneous tissue |
| Cyst formation | Develop into cysticerci (~1 cm) over months |
| Host immune response | Intact cysts cause little inflammation; dying cysts trigger intense edema and seizures |
| Resolution | Degenerating cyst calcifies over 1–2 years |
The BBB normally shields viable cysts from immune attack — when the cyst dies (spontaneously or with treatment), antigen release provokes a perilesional inflammatory response that is the principal cause of symptoms.
Classification by Location
1. Parenchymal NCC (most common)
- Cysts in brain parenchyma, predominantly at the gray-white junction
- Seizures are the dominant presentation
- Over 1–2 years, cysts degenerate → fibrosis → calcification
2. Extraparenchymal NCC
| Form | Characteristics |
|---|---|
| Intraventricular | Most commonly 4th ventricle; causes obstructive hydrocephalus; highly symptomatic |
| Subarachnoid (racemose) | Cysts grow without scolex in the subarachnoid space; aggressive form; arachnoiditis, hydrocephalus, vasculitis, stroke |
| Spinal | Intra- or extramedullary; rare |
| Ocular | Subretinal or vitreous; visual symptoms |
Stages of Cyst Evolution (Critical for Imaging Interpretation)
| Stage | Pathology | CT | MRI | Symptoms |
|---|---|---|---|---|
| Vesicular (viable) | Viable cyst, intact BBB, minimal inflammation | Hypodense cyst, ± scolex dot | CSF-isointense cyst, hypointense scolex | Often asymptomatic |
| Colloidal (degenerating) | Scolex disintegrating, intense edema | Ring-enhancing lesion, edema | Heterogeneous signal, ring enhancement, perilesional edema | Seizures, headache |
| Granular-nodular | Fibrotic retraction | Nodular enhancement | Small enhancing nodule | Seizures decreasing |
| Calcified | Complete involution | Dense calcification | Hypointense nodule on T2* | May still cause seizures via perilesional gliosis |
Clinical Manifestations
Seizures are the most common presentation (50–70%), typically focal with or without secondary generalization, occurring most often during the colloidal (degenerating) stage.
Other features:
- Headache — most common non-seizure symptom
- Increased intracranial pressure — from intraventricular cysts or communicating hydrocephalus
- Focal neurological deficits — depending on cyst location
- Meningitis — subarachnoid NCC; chronic basilar meningitis pattern
- Stroke — vasculitis from subarachnoid cysts
- Cysticercotic encephalitis — rare; massive cyst burden with diffuse cerebral edema; can be fatal if antiparasitics are given prematurely
- Psychiatric symptoms — cognitive decline, dementia (in heavy infection)
- Hydrocephalus — obstructive (intraventricular) or communicating (arachnoiditis)
In 80–90% of parenchymal cases, lesions resolve within 3–6 months; ~20% of patients continue to have seizures requiring ongoing antiepileptic therapy.
Diagnosis
Diagnosis relies on a combination of neuroimaging, serology, clinical history, and exposure context. No single test is pathognomonic, but the "hole-with-dot" sign on MRI (cyst + eccentric scolex) is highly specific.
Neuroimaging
CT findings:
- 1–2 cm cystic lesion with thin walls and a 1–3 mm mural nodule (scolex)
- Ring-like enhancement with surrounding edema
- Calcified lesion (chronic stage)
- Hydrocephalus
MRI findings (more sensitive):
- Vesicular stage: CSF-isointense cyst, hypointense scolex ("hole-with-dot")
- Colloidal stage: ring enhancement, perilesional edema on FLAIR
- Calcified stage: hypointense on T2/GRE; may have perilesional FLAIR signal in seizure-causing calcifications
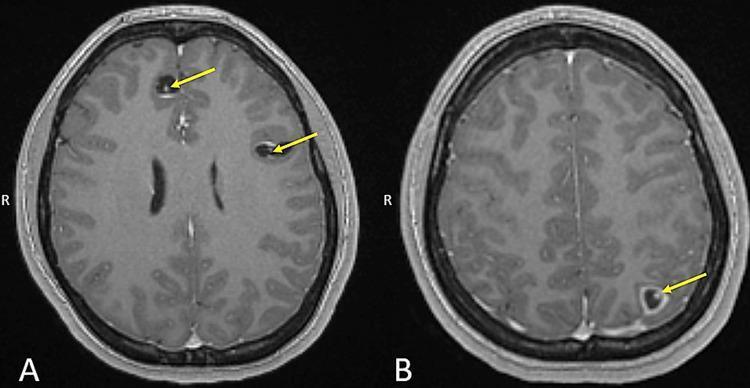
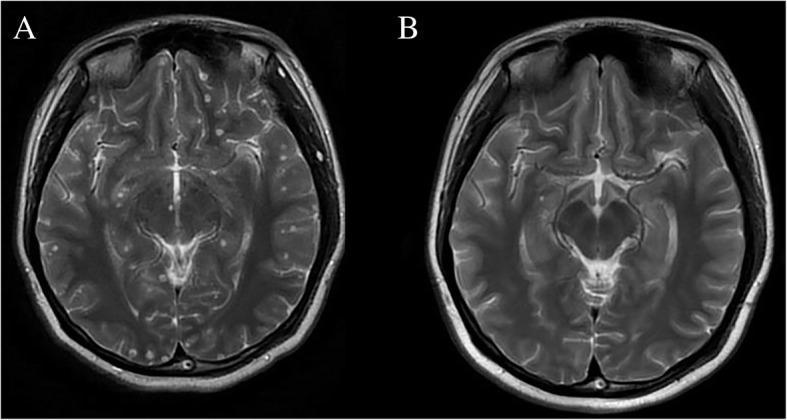
Serology
- EITB (enzyme-linked immunoelectrotransfer blot) — most specific serologic test; sensitivity ~94–98% with ≥2 cysts, but only ~50–70% with single cyst or calcified lesion
- ELISA (CSF or serum) — less specific
- CSF pleocytosis (lymphocytic/eosinophilic) with elevated protein in subarachnoid NCC
Del Brutto Diagnostic Criteria
Combines absolute, major, minor, and epidemiological criteria to classify diagnosis as definitive or probable.
Treatment
Treatment must be individualized based on number, location, viability of cysts, and presence of hydrocephalus.
Treatment Table (IDSA/ASTMH 2017 Guidelines)
| Form | Subgroup | Recommendation |
|---|---|---|
| Parenchymal — viable or enhancing (1–2 cysts) | — | Albendazole monotherapy + steroids |
| Parenchymal — viable or enhancing (>2 cysts) | — | Albendazole + praziquantel + steroids |
| Parenchymal — calcified | Any number | No antiparasitic treatment |
| Cysticercotic encephalitis (diffuse edema) | — | No antiparasitic; steroids only |
| Intraventricular — removal feasible | Lateral/3rd ventricle | Neuroendoscopic removal; no medical therapy if successful |
| Intraventricular — removal feasible | 4th ventricle | Neuroendoscopic or microsurgical removal |
| Intraventricular — removal not feasible | — | Ventricular shunt → then antiparasitic + steroids |
| Subarachnoid | ± Hydrocephalus | Shunt if hydrocephalus → prolonged albendazole ± praziquantel |
| Hydrocephalus, no visible cysts | — | Ventricular shunt; no antiparasitic |
| Spinal cysticercosis | — | Surgical removal or antiparasitic + steroids (individualized) |
| Ocular cysticercosis | — | Surgical resection |
Antiparasitic Drugs
Albendazole (drug of choice over praziquantel):
- Dose: 400 mg twice daily for up to 21 days (or 15 mg/kg/day in two divided doses)
- Advantages over praziquantel: shorter course, lower cost, better subarachnoid penetration, drug levels increased (not decreased) by dexamethasone
- Contraindicated in pregnancy, children <2 years, and hepatic cirrhosis
- Drug interactions: dexamethasone and praziquantel increase albendazole levels; phenytoin, phenobarbital, carbamazepine, and ritonavir decrease levels
Praziquantel:
- Used in combination with albendazole for patients with >2 cysts (improves efficacy)
- Levels decreased by dexamethasone and antiepileptic drugs (carbamazepine, phenytoin)
Corticosteroids
- Essential adjunct to antiparasitics to blunt inflammatory response from dying cysts
- Dexamethasone or prednisone; duration tailored to clinical response
- Mandatory when treating subarachnoid/intraventricular NCC (antiparasitics can precipitate acute hydrocephalus)
Antiepileptic Drugs (AEDs)
- All patients with seizures require AEDs
- Monotherapy controls seizures in most
- Duration: typically continued until cyst resolution on imaging; long-term AEDs needed in ~20% who have persistent seizures
Surgery
- Neuroendoscopy: standard approach for intraventricular NCC — avoids need for medical therapy if cyst successfully removed
- VP shunt: for hydrocephalus when cysts are not surgically accessible
- Microsurgery: for fourth-ventricular cysts or selected cases
Prognosis
- Most parenchymal NCC has a favorable prognosis: cysts resolve in 80–90% within 3–6 months; seizures remit in most patients
- Subarachnoid and intraventricular NCC carry higher morbidity and mortality (hydrocephalus, stroke, arachnoiditis)
- Cysticercotic encephalitis is life-threatening; antiparasitics are contraindicated until edema resolves
Prevention
- Access to clean water and sanitation
- Cooking pork thoroughly (cysticerci in muscle killed at 56°C for >5 min)
- Good hand hygiene (to prevent fecal-oral transmission of eggs)
- Treating tapeworm carriers (intestinal taeniasis) in endemic communities
Key sources: Bradley and Daroff's Neurology in Clinical Practice; Tintinalli's Emergency Medicine; Katzung's Basic and Clinical Pharmacology, 16th ed.; Washington Manual of Medical Therapeutics
Recent evidence (2025–2026):
- A 2025 systematic review and meta-analysis (PMID 40381508) supports neuroendoscopic management as the preferred approach for intraventricular NCC, consistent with the IDSA guidelines above.
- A 2026 systematic review (PMID 42087630) on NCC-associated meningitis highlights the aggressive course of subarachnoid/racemose NCC with meningitic complications.
- A 2025 systematic review (PMID 40822429) documents a range of movement disorders as uncommon but recognized manifestations of NCC.
This is a shared conversation. Sign in to Orris to start your own chat.