70 year old man has shingles along the nerve on left part of the body in the abdominal region above the umbilicus
Reading File
Finding Sources
Finding Sources
Searching PubMed
herpes zoster treatment elderly
Reading File
Reading File
Reading File
Reading File
Finding Sources
Searching Images
herpes zoster dermatomal distribution thoracic abdomen shingles rash
Reading File
Finding Sources
Loading Image
Loading Image
I now have everything needed for a comprehensive answer. Here is the full clinical picture:
Herpes Zoster (Shingles) — Left Abdominal Region, Above the Umbilicus, in a 70-Year-Old Man
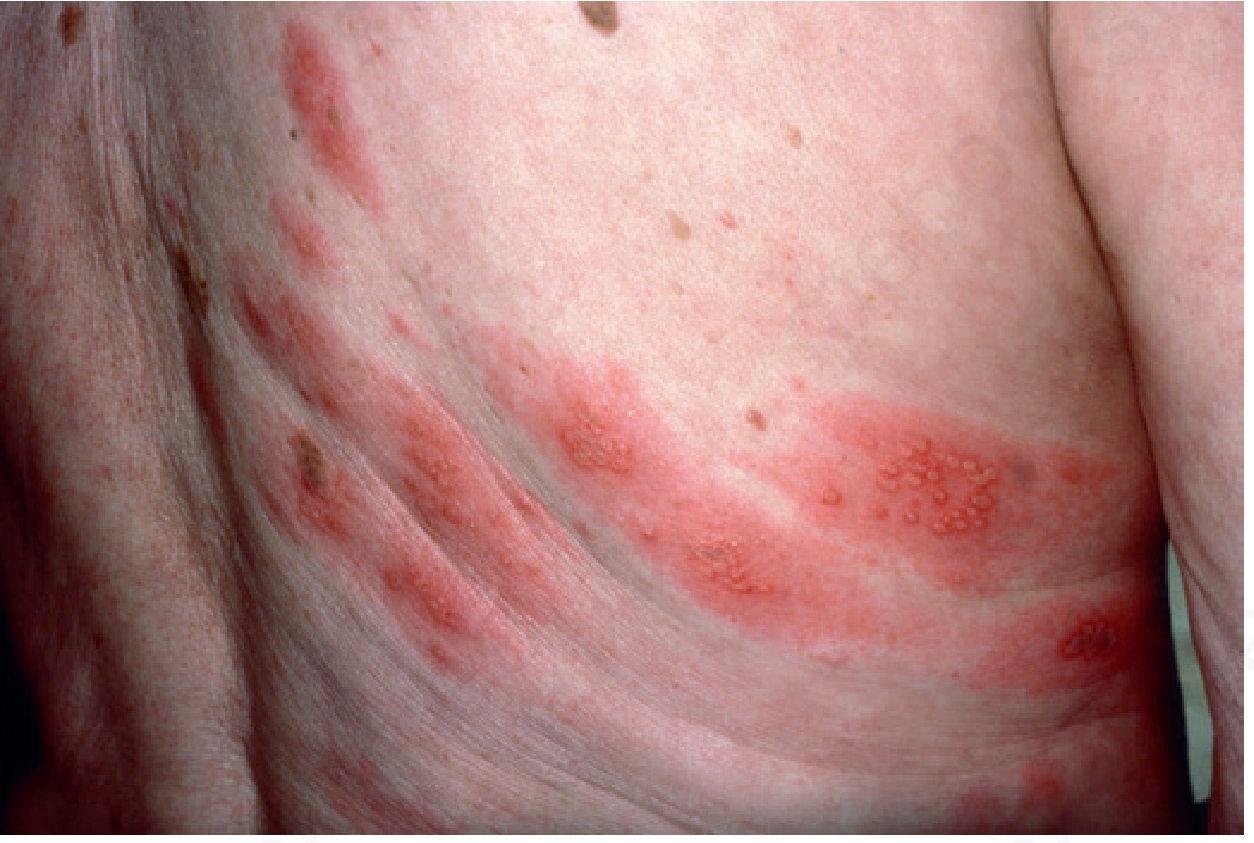
Dermatome Involved
Left-sided abdominal zoster above the umbilicus corresponds to the T8–T10 thoracic dermatomes (the umbilicus itself is at T10). The rash travels from the posterior dorsal root ganglion, around the left flank, to the anterior abdominal wall — following the intercostal/subcostal nerves. Thoracic dermatomes are the single most commonly affected region in herpes zoster, accounting for approximately 55% of all cases.
Pathophysiology
Herpes zoster results from reactivation of varicella-zoster virus (VZV / HHV-3), which lies latent in the dorsal root ganglion cells after primary chickenpox infection. With aging, cell-mediated immunity wanes — the principal reason this 70-year-old man is at high risk. Over age 75, the annual incidence is more than four times the rate in those under 45. The virus travels anterograde down the sensory nerve into skin, producing the characteristic unilateral, band-like vesicular eruption.
Additional risk factors in elderly patients include:
- Comorbidities (diabetes, COPD, autoimmune disease)
- Statin use (slightly increased risk)
- Hemodialysis
- Malignancy (especially hematologic) — zoster patients have a 0.7–1.8% absolute risk of a new cancer diagnosis within 1 year
Clinical Features
| Feature | Details |
|---|---|
| Prodrome | 1–several days of pain, burning, hyperesthesia in the dermatome before any rash |
| Rash evolution | Erythematous papules → vesicles → pustules → crusting (new lesions appear for 1–5 days) |
| Distribution | Strictly unilateral, does not cross the midline; left T8–T10 in this patient |
| Duration | Lesions may take up to 6 weeks to heal in elderly patients (vs. 2–3 weeks in young) |
| Pain | Severe; pain severity correlates with lesion extent and age |
| Rare variants | Zoster sine herpete (pain without rash); disseminated zoster (>20 lesions outside the dermatome) |
Complications — High Priority in a 70-Year-Old
1. Postherpetic Neuralgia (PHN) — Most Important
- Occurs in up to 40% of patients over age 60 (vs. <10% under age 60)
- Pain persists after skin lesions heal, driven by incomplete nerve injury creating a hyperpathic state
- Can last months to years; eventually subsides even in severe cases
2. Other Complications
- Disseminated zoster: >20 satellite lesions outside the dermatome → risk of visceral (lung, liver, CNS) spread; more common in immunosuppressed/elderly
- Bacterial superinfection of skin lesions
- Although not relevant here, ophthalmic (V1) and Ramsay Hunt syndrome (cranial nerve VII) are the most feared cranial nerve variants
Management
Antiviral Therapy (Start Immediately)
Initiate within 72 hours of rash onset — this is the critical window. Benefits are more pronounced in patients >50 years.
| Drug | Dose | Duration |
|---|---|---|
| Valacyclovir | 1000 mg PO TID | 7 days |
| Famciclovir | 500 mg PO TID | 7 days |
| Acyclovir | 800 mg PO 5×/day | 7 days |
- Antivirals hasten lesion resolution, reduce viral shedding, and decrease acute pain
- Treatment up to 7 days after onset is still beneficial if new vesicles are still forming
- IV acyclovir is reserved for disseminated disease, CNS involvement, or severely immunosuppressed patients
Pain Management
- Acetaminophen / NSAIDs for mild-moderate pain
- Opioid analgesia may be required for severe acute pain
- Corticosteroids (in combination with antivirals): modest reduction in acute pain; do not prevent PHN but can be considered in older individuals with severe pain without contraindications
- Cool compresses for local relief
Postherpetic Neuralgia Treatment (if it develops)
- Tricyclic antidepressants (amitriptyline 50–125 mg at bedtime) — well-established, first-line
- Gabapentin / Pregabalin — FDA-approved for PHN; particularly effective for lancinating-type pain
- Capsaicin ointment — topical, applied to the affected skin
- Carbamazepine, valproate, SSRIs — adjunctive options
- Nerve blocks — inconsistent benefit but may offer temporary relief
- Short-term narcotics are appropriate for severe persistent pain; patients with >1 year of symptoms often have a depressive component and respond to antidepressants
Vaccination — Prevention
- Shingrix (recombinant zoster vaccine, RZV) is the current preferred vaccine — recommended for all immunocompetent adults ≥50 years (2 doses)
- The older live vaccine (Zostavax) decreased burden of illness by 61% and PHN by 67% in clinical trials; Shingrix is substantially more effective
- The vaccine is not contraindicated in someone who has already had zoster
Red Flags to Rule Out in This Patient
- Disseminated zoster — check for >20 lesions outside the T8–T10 dermatome
- Visceral involvement — unexplained respiratory symptoms warrant a chest X-ray
- New underlying malignancy — consider workup given the 0.7–1.8% 1-year cancer risk post-zoster, especially hematologic malignancy
- CNS involvement — any encephalopathic features warrant MRI brain, lumbar puncture, and CSF VZV PCR
Sources: Andrews' Diseases of the Skin, 12e | Textbook of Family Medicine, 9e | Tintinalli's Emergency Medicine | Adams & Victor's Principles of Neurology, 12e
What to give for itching, and any ointment to be prescribed?
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Searching the Web
herpes zoster shingles itching treatment antihistamine calamine ointment guidelines
Finding Sources
Finding Sources
Here is a concise, practical prescribing guide for itching in this patient's shingles:
Managing Itch (Pruritus) in Herpes Zoster
Why It Itches
Itch in shingles comes from two sources: the vesicles/inflammatory rash (histamine-mediated) and nerve sensitization (neurogenic itch). Treatment should address both.
Oral Antihistamines (Systemic Itch Relief)
| Drug | Dose | Notes |
|---|---|---|
| Hydroxyzine (Atarax) | 25 mg TID–QID | Preferred in shingles — both antihistamine and mild anxiolytic/analgesic effect; helps with sleep |
| Cetirizine (Zyrtec) | 10 mg OD | Non-sedating; good daytime option |
| Loratadine (Claritin) | 10 mg OD | Non-sedating; OTC, once daily |
| Diphenhydramine (Benadryl) | 25–50 mg every 6 hrs | Effective but use with caution in a 70-year-old — significant sedation, anticholinergic effects (urinary retention, confusion in elderly) |
In a 70-year-old, hydroxyzine (low dose, 10–25 mg at bedtime) or cetirizine/loratadine during the day is the safest choice. Avoid diphenhydramine as the first-line choice in elderly patients.
Topical Treatments (Local Skin Relief)
For the Vesicular/Weeping Phase (Active Blisters)
| Preparation | How to Use | Purpose |
|---|---|---|
| Calamine lotion | Dab on with cotton ball, let dry; repeat 3–4×/day | Soothes itch, dries vesicles, cooling effect — first-line topical |
| Burrow's solution (Aluminium acetate 13%) | Wet compress, 15–20 min, 3–4×/day | Astringent, dries weeping lesions, antimicrobial |
| Colloidal oatmeal lotion (Aveeno) | Apply topically or soak in oatmeal bath | Gentle, anti-inflammatory, soothing |
Do NOT apply calamine or any lotion directly on open/broken skin erosions — use wet compresses (Burrow's) there instead.
Once Lesions Begin Crusting / Healing Phase
| Preparation | How to Use | Purpose |
|---|---|---|
| Lidocaine 2–5% gel or ointment | Apply sparingly to painful/itchy areas | Local anaesthetic; reduces both itch and pain |
| Capsaicin 0.025–0.075% cream | Apply 3–4×/day (use gloves) | Depletes substance P; better for postherpetic itch/pain than acute phase — causes initial burning |
| White soft paraffin / petrolatum | Thin layer over crusted lesions | Prevents cracking, aids healing of crusts |
What NOT to Apply
- Topical acyclovir cream — no benefit for shingles (it works systemically; topical preparations do not meaningfully penetrate)
- Topical steroids — avoid directly on vesicular/active lesions; can worsen infection
- Antibiotic ointments (e.g., neomycin, bacitracin) — only if secondary bacterial infection is suspected
Practical Prescription Summary for This Patient
1. Oral: Hydroxyzine 10–25 mg at bedtime (for itch + sleep)
+ Cetirizine 10 mg every morning (daytime itch)
2. Topical (acute/weeping phase):
- Calamine lotion — apply with cotton ball TID–QID to intact vesicles
- Burrow's solution compresses — for oozing/weeping areas, 15 min TID
3. Topical (healing/post-crusting phase):
- Lidocaine 2% gel — apply to painful itchy areas as needed
- White soft paraffin — over dried crusts to prevent cracking
4. General: Cool compresses (wet cloth, 20 min), loose cotton clothing,
colloidal oatmeal baths
Important Reminders
- Ensure the oral antiviral (valacyclovir/famciclovir) has been started — this is the primary treatment and will reduce the duration of itch along with the rash
- If itch is neurogenic (persists after lesions heal = PHN-related itch), gabapentin or pregabalin is the appropriate agent — antihistamines will not work for neurogenic itch
- Keep nails short and advise against scratching to prevent bacterial superinfection
This is a shared conversation. Sign in to Orris to start your own chat.