21 female
Reading File
Finding Sources
Finding Sources
Searching Images
molluscum contagiosum skin papules umbilicated
Reading File
Reading File
Based on the image and textbook sources, here is a clinical assessment:
Likely Diagnosis: Molluscum Contagiosum
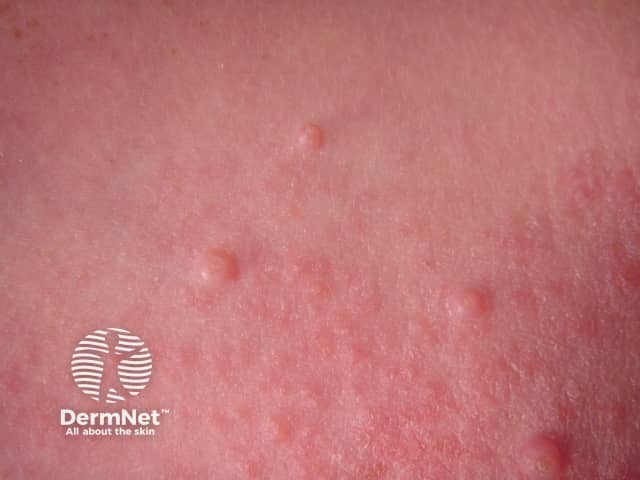
The image shows two lesions on what appears to be the shoulder/upper arm area:
- A pearly, dome-shaped papule with a central umbilication (the characteristic "dimple" or pit in the center)
- A smaller adjacent lesion with a white core visible
- Mild surrounding erythema on one lesion (consistent with irritation or early inflammatory resolution)
This morphology — smooth, flesh-colored to pearly papules with central umbilication — is the hallmark of molluscum contagiosum.
What Is It?
Molluscum contagiosum is a benign viral skin infection caused by a poxvirus (MCV types 1–4). In sexually active young adults like yourself, it is commonly transmitted by skin-to-skin contact, including sexual contact. The lesions typically appear on the lower abdomen, thighs, and genital region in adults, but can also appear on the trunk or arms.
Key Features
- Small, firm, pearly papules 1–10 mm in diameter
- Central umbilication (the defining feature — a central dimple or white core)
- Lesions cluster due to autoinoculation (spreading by scratching)
- An irritated/inflamed lesion (as seen in your image) may precede spontaneous resolution
What To Expect
- Self-limiting: Most cases resolve spontaneously within 6 months to 4 years without treatment
- Contagious: Spread by direct skin contact and fomites (shared towels, razors, etc.)
- Avoid shaving over affected areas — this spreads the virus
Treatment Options (if desired)
| Option | Notes |
|---|---|
| Watchful waiting | Preferred if lesions are few and not bothersome |
| Cantharidin (topical, clinic-applied) | Very effective; may need multiple sessions |
| Cryotherapy (liquid nitrogen) | Freezes and destroys lesions |
| Curettage | Physical removal under local anesthesia |
| Electrodesiccation | Burns off lesions |
When to See a Doctor
You should see a GP or dermatologist if:
- Lesions are spreading rapidly or numbering more than 20
- You want them treated for cosmetic or comfort reasons
- You're unsure if a lesion is MC (biopsy can confirm with molluscum bodies on Giemsa stain)
- You have any concern about concurrent sexually transmitted infections (other STIs can coexist)
⚠️ Important: This is an AI-assisted assessment for informational purposes only and is not a substitute for an in-person clinical diagnosis. Please see a healthcare provider for confirmation and treatment if needed.
Sources: Tintinalli's Emergency Medicine; Andrews' Diseases of the Skin (Clinical Dermatology)
Single lesion on breast
The location on the breast in a sexually active 21-year-old is actually very consistent with molluscum contagiosum — it's one of the classic sites for sexually transmitted MC in adults, spread by close skin-to-skin contact.
Updated Assessment: Still Molluscum Contagiosum
A single umbilicated papule on the breast in a sexually active young adult fits perfectly:
- In adults, MC via sexual/close contact commonly involves the chest, breast, lower abdomen, groin, and thighs
- A solitary lesion is a recognized presentation — not all cases are multiple
- The one lesion with a visible white core/central dimple and the second smaller adjacent lesion (possibly very early) match classic MC morphology
What This Means for You
Single lesions can still spread via autoinoculation (touching the lesion then touching other skin) or to a partner, so:
- Don't squeeze, pick, or scratch it — this spreads the virus
- Avoid skin-to-skin contact over the area with partners until resolved/treated
- Consider whether a sexual partner may also need to be checked
Practical Next Steps
- See a GP or sexual health clinic — they can confirm the diagnosis visually (no tests usually needed) and offer same-visit treatment
- Cryotherapy or cantharidin works well for a single lesion — quick and effective
- If you want to wait, a single lesion may resolve on its own within months, but treating it early prevents spread
⚠️ This remains an AI-assisted assessment — not a formal diagnosis. A clinician visit is recommended to confirm and treat.
She didn't hv sexual contact??? Early period, high stress time, sudden eruption of acne on forehead and bridge of nose and small pimple on breast
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Good — that context gives a much clearer picture. Here's the revised assessment:
Revised Assessment: Hormonal / Stress-Triggered Acne Vulgaris
The full clinical picture now fits acne vulgaris triggered by hormonal fluctuation and stress, NOT molluscum contagiosum:
| Feature | Fits Acne Vulgaris |
|---|---|
| 21-year-old female | ✅ Peak age group |
| Early in period | ✅ Premenstrual hormone surge (progesterone/androgens ↑ sebum) |
| High stress | ✅ Cortisol stimulates androgen production → more sebum |
| Forehead + bridge of nose | ✅ Classic T-zone acne distribution |
| Sudden eruption | ✅ Consistent with hormonal flare |
| Single pimple on breast | ✅ Chest involvement is common — sebaceous follicles exist on the breast |
What's Happening Physiologically
Stress → ↑ cortisol → ↑ androgens → ↑ sebum production by sebaceous glands → follicular plugging by Cutibacterium acnes → comedones, papules, pustules
The premenstrual phase specifically causes a well-known acne flare in many women due to hormonal shifts.
The lesion on the breast in this context is almost certainly just an inflamed follicular papule or comedone — breast skin has sebaceous follicles and can absolutely develop acne, especially with hormonal triggers.
What To Do
Right Now (over-the-counter)
- Benzoyl peroxide 2.5–5% wash or gel on affected areas — kills C. acnes and reduces inflammation
- Salicylic acid cleanser — unblocks pores, good for T-zone
- Don't scrub — mechanical friction worsens comedone rupture
- Non-comedogenic moisturiser — stress and cleansers can over-dry the skin
Lifestyle
- Manage stress (this directly affects hormone levels)
- Sleep, hydration, avoid touching the face
- Avoid heavy or oily cosmetics/hair products on the forehead
If It Recurs Every Cycle (see a doctor for):
- Combined oral contraceptive pill — reduces androgenic drive to sebaceous glands (several formulations are FDA-approved specifically for acne)
- Spironolactone — anti-androgen, very effective for hormonal acne in women
- Topical retinoids (tretinoin) — normalise follicular keratinisation
Bottom Line
This is very likely cyclical hormonal acne — a common, benign, and very treatable condition in young women. The breast lesion is part of the same process, not a separate concern. No action needed beyond standard acne care unless it becomes persistent or severe.
⚠️ AI-assisted assessment only — not a formal clinical diagnosis.
Source: Harrison's Principles of Internal Medicine, 22nd Ed.
Period came 20 days early
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Now the full picture is becoming clearer. Here's the updated clinical assessment:
Putting It All Together
| Symptom | Significance |
|---|---|
| Period 20 days early | Significantly disrupted cycle — not normal variation |
| High stress | Major trigger for HPA-HPG axis disruption |
| Sudden acne on forehead + nose | Androgenic/hormonal surge |
| Pimple on breast | Hormonal acne extending to chest |
| 21-year-old female | Peak age for hormonal dysregulation |
Most Likely Cause: Stress-Induced Hormonal Disruption
Severe psychological stress disrupts the hypothalamic-pituitary-gonadal (HPG) axis:
- ↑ Cortisol → suppresses/disrupts normal GnRH pulsing → abnormal LH/FSH release → disordered ovulation → cycle comes early, late, or is skipped entirely
- ↑ Androgens (from stress-driven adrenal activation) → ↑ sebum → acne flare
A period arriving 20 days early is called polymenorrhea (cycle shorter than 21 days) and in this context is most likely anovulatory bleeding — the uterine lining sheds abnormally because ovulation didn't happen on schedule, not because a true menstrual cycle completed.
However — Rule Out PCOS
The combination of:
- Acne
- Menstrual irregularity (abnormal cycle timing)
- Young female
...also fits Polycystic Ovary Syndrome (PCOS), which affects 4–10% of premenopausal women. PCOS features acne (in ~25% of cases), oligomenorrhea/irregular bleeding (40%), and androgen excess. Stress can also unmask underlying PCOS.
What She Should Do
See a doctor — this warrants evaluation
A GP or gynaecologist should check:
| Test | Why |
|---|---|
| Pregnancy test | Must exclude — irregular bleeding can be implantation bleeding |
| LH, FSH, oestradiol | Assess HPG axis function |
| Total + free testosterone, DHEAS | Screen for androgen excess (PCOS, adrenal) |
| Prolactin | Elevated prolactin disrupts cycles and can cause acne |
| Thyroid function (TSH) | Thyroid dysfunction commonly disrupts menstrual cycles |
| Pelvic ultrasound | If PCOS suspected — look for polycystic ovaries |
Keep a menstrual diary
Track cycle length, flow, and symptoms (acne, mood, pain) for the next 2–3 months. One abnormal cycle under stress may self-correct. Two or more in a row needs investigation.
Bottom Line
One episode of a very early period during a high-stress period is likely stress-induced hormonal disruption and may self-resolve when stress settles. However, the combination with acne means PCOS should be actively excluded with basic blood tests. A pregnancy test is the first thing to do at home.
⚠️ AI-assisted assessment only — not a substitute for clinical evaluation. Please see a doctor, especially if cycles remain irregular.
Sources: Tietz Textbook of Laboratory Medicine 7th Ed.; Harrison's Principles of Internal Medicine 22nd Ed.
This is a shared conversation. Sign in to Orris to start your own chat.