So while cannulating MHD patient for dialysis session many a times the needle gets clotted sometimes in a few moments sometimes when there's a delay in locating vein after inserting the needle. How to prevent that.
Reading File
Checking Date & Time
Finding Sources
Finding Sources
Searching PubMed
hemodialysis needle cannulation clotting prevention
Finding Sources
Finding Sources
Reading File
Finding Sources
Reading File
Reading File
Reading File
Reading File
The earlier read at line 3094 was cut off. Let me check where the anticoagulation-free strategies were described:
The snippet from earlier (line 3093-3094) said:
"During anticoagulation-free dialysis, several strategies may help prevent clotting, such as the following: (1) rinse the circuit before dial..."
That was the key passage. Combined with all the context I've gathered, I now have enough to give a comprehensive, practical answer.
Here's a practical breakdown of why needles clot during MHD cannulation and how to prevent it:
Why the Needle Clots During Cannulation
When you insert a needle and blood enters the needle hub but flow is not immediately established (either because connection to the tubing is delayed, or you're searching for the vessel lumen), blood stagnates. Uremic blood in MHD patients already has a pro-inflammatory, pro-thrombotic state on top of the foreign surface contact activation triggered by the metal needle — this combination causes rapid fibrin/clot formation in the needle dead space.
Prevention Strategies
1. Pre-fill the needle with heparinized saline before insertion
This is the single most effective step. Draw up 2–5 mL of heparinized normal saline (100–500 IU/mL depending on unit protocol) into a syringe and attach it to the needle before cannulating. Once blood flashback is confirmed, immediately flush — this prevents stasis-driven clotting in the hub and needle lumen. This is especially important when you anticipate any delay (difficult access, obese arm, poor fistula maturation).
2. Flush immediately upon flashback
The moment you see blood return in the needle chamber, flush slowly with the pre-attached syringe. Do not wait to cap, clamp, or connect tubing. Even a 15–30 second delay with blood sitting in the needle is enough to initiate clotting.
3. Minimise the search time inside the tissue
Blind probing with the needle causes trauma, haematoma, and blood oozing into tissue — all of which consume time and promote clotting. Strategies to reduce search time:
- Palpate and mark the fistula track before skin puncture — feel the thrill, mark entry and direction with a pen if needed.
- Use a tourniquet (or simply have the patient make a fist/elevate the fistula arm in a dependent position) to engorge the vessel before cannulation.
- Ultrasound guidance at the bedside has been shown to reduce failed cannulations, particularly for poorly palpable fistulae — many units now keep a portable US probe at chairside.
- Good lighting and positioning of the arm cannot be overstated.
4. Use the correct needle gauge and bevel orientation
Inserting the needle bevel-up at 20–35° ensures the tip enters the lumen cleanly. A bevel-down insertion or too-steep angle risks the tip abutting the posterior wall, giving partial or no blood return while blood accumulates and clots in the needle.
5. Start the blood pump quickly after both needles are inserted
Once both arterial and venous needles are placed and connected, start the blood pump promptly. Prolonged priming time with static blood in the circuit promotes clotting. Standard protocol is to start the pump at a low rate (100–150 mL/min) as soon as connection is established, then ramp up.
6. Ensure adequate systemic anticoagulation at session start
Per standard MHD protocol:
- Heparin bolus (1000–5000 U or 50 U/kg weight-based) should be given into the arterial line before blood reaches the dialyzer — ideally within 1–3 minutes of session start.
- In patients where heparin is contraindicated, the circuit should be pre-rinsed with heparinized saline (1000–5000 U in 1L NS run through the lines during priming) before blood is introduced.
- If using anticoagulation-free dialysis: pre-rinse with heparinized saline, use a biocompatible/heparin-coated dialyzer, and flush the circuit with 100–200 mL NS every 15–30 minutes during the session. — Brenner and Rector's The Kidney, 7th ed., p. 2731–2732
7. Avoid kinking or compression of the needle after insertion
After insertion, tape the needle securely but without angulating it. A kinked needle causes flow turbulence and stasis — both promote clotting.
8. Consider the patient's pre-dialysis state
- Hypotension at session start (common with over-ultrafiltration from the prior session) causes low fistula flow, which means sluggish blood in the needle — pre-load with 100–200 mL NS if needed.
- Hypercoagulable states (antiphospholipid syndrome, protein C/S deficiency, active inflammation) may require adjusted heparin dosing — flag these patients and discuss with the nephrologist.
Quick Reference Summary
| Situation | Fix |
|---|---|
| Delay in locating vein | Pre-fill needle with heparinized saline; flush immediately on flashback |
| Repeated probing | Palpate/mark fistula before inserting; use US guidance |
| Clot a few moments after insertion | Connect tubing and start pump promptly; don't leave blood static in needle |
| Fistula poorly engorged | Tourniquet or dependent positioning before cannulation |
| Recurrent clotting in a specific patient | Check heparin dose adequacy; rule out hypercoagulable state |
The core principle is: never let blood sit still in a needle. Pre-fill, flush on flashback, connect fast, start pump promptly.
Can you show and guide me how to elevate fistula arm
Checking Date & Time
Searching Images
AV fistula arm positioning hemodialysis cannulation
Loading Image
Loading Image
Good — the second image actually shows the dialysis session arm positioning well. Now let me give you the full corrected guidance with visuals.
Clarification: "Dependent" vs "Elevated" — Which One Engorges the Fistula?
✅ DEPENDENT arm = engorges the fistula (use this BEFORE cannulation)
The arm hangs below the level of the heart. Gravity causes venous blood to pool in the forearm and fistula, making the vessel distended, prominent, and easy to feel and cannulate.
Step-by-Step: Dependent Arm Positioning to Engorge the Fistula
Step 1 — Seat the patient in the dialysis chair
Have the patient sit upright or slightly reclined.
Step 2 — Let the fistula arm hang downward
The arm should hang off the side of the chair or rest low on the lap — clearly below the level of the heart. Do NOT prop it up on an armrest at this stage.
Step 3 — Ask the patient to open and close their fist 8–10 times
This "pumps" venous blood into the forearm and engorges the fistula further. The vessel should become visibly raised and pulsatile.
Step 4 — Apply a tourniquet if needed
Place it 5–10 cm proximal to the intended cannulation site. Tighten enough to obstruct venous outflow but NOT arterial flow (you should still feel the thrill distal to the tourniquet). Hold for 60–90 seconds.
Step 5 — Palpate and mark
Feel for the track of the fistula. Mark the entry point with a sterile pen or thumb-nail indent if you are a beginner.
Step 6 — Remove tourniquet and cannulate promptly
Remove the tourniquet just before inserting the needle. Cannulate with the bevel up at 20–35°, flush immediately on flashback.
❌ Why You Should NOT Elevate the Arm Before Cannulation
Raising the arm above heart level drains venous blood out of the fistula — the vessel deflates and becomes harder to palpate and cannulate. This is the opposite of what you want.
| Arm Position | Effect on Fistula | When to Use |
|---|---|---|
| Dependent (hanging down) | Engorges / distends vessel | Before cannulation |
| At heart level | Neutral | During dialysis session (standard resting position) |
| Elevated (above head) | Vessel collapses | Testing for venous outflow stenosis only |
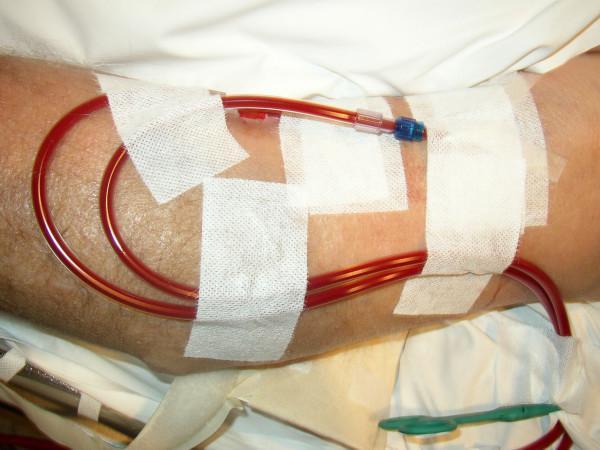
In Summary
Before cannulation: arm down (dependent) + fist pumping + tourniquet → vessel engorges → easier cannulation. During session: arm rested comfortably at chair level. "Elevate to check stenosis": arm raised above head → if fistula stays distended instead of collapsing, suspect outflow stenosis.
What if the patient is lying on a bed and there's only bed facility available not chair etc.
Checking Date & Time
Great practical question — bed-based dialysis is very common in ICU, ward settings, and resource-limited units. The principle is exactly the same (make the arm dependent relative to the heart), but the technique adapts to what's available.
Fistula Engorgement on a Flat Bed
The Core Problem
When a patient lies flat in bed, both arms are at roughly heart level — so neither arm is naturally dependent. The fistula won't be as engorged as when sitting upright.
Practical Adaptations (No Chair, Bed Only)
Option 1 — Head-end elevation + arm hanging off the side of the bed ✅ (Best option)
- Elevate the head end of the bed to 30–45° (semi-Fowler's position) if the patient's condition allows.
- Ask the patient to let the fistula arm hang off the side of the bed, pointing downward toward the floor.
- The arm is now below heart level — gravity engorges the fistula just as it would in a chair.
- Have the patient open and close the fist 8–10 times while the arm hangs down.
- Apply tourniquet if needed, palpate the track, mark, then cannulate.
⚠️ Make sure the bed side-rail is lowered on that side before hanging the arm — safety first.
Option 2 — Arm dangling off the foot-end or side of a flat bed ✅
If the bed cannot be raised (e.g., ICU flat positioning required):
- Move the patient slightly toward the edge of the bed on the fistula side.
- Let the fistula arm hang over the edge of the mattress toward the floor.
- Even a 20–30 cm drop below mattress level provides meaningful venous pooling.
- Fist pump + tourniquet as above, then cannulate.
Option 3 — Towel/roll under the opposite shoulder ✅ (Subtle tilt)
If hanging the arm is not possible:
- Place a folded towel or small pillow under the opposite shoulder — this tilts the patient slightly toward the fistula side, allowing the fistula arm to drop slightly lower than the rest of the body.
- Not as effective as a true dependent hang, but better than flat.
Option 4 — Tourniquet alone (if arm movement is restricted) ✅
When the patient cannot move the arm at all (post-op, paralysis, pain):
- Apply the tourniquet firmly proximal to the cannulation site.
- Wait 90–120 seconds — this alone will engorge the vessel by obstructing venous return.
- Palpate, cannulate, remove tourniquet.
What to Avoid on a Flat Bed
| ❌ Don't do this | Why |
|---|---|
| Prop the fistula arm on a pillow above bed level | This elevates the arm — vessel deflates |
| Leave arm lying flat alongside the body | Neutral position — minimal engorgement |
| Apply tourniquet for >3 minutes | Causes discomfort and access trauma |
Quick Decision Tree (Bed Setting)
Patient flat in bed
|
Can head-end be raised 30-45°?
YES → Raise head → hang fistula arm off side → fist pump → tourniquet → cannulate
NO → Slide patient to edge → hang arm over mattress side → tourniquet → cannulate
Still difficult? → Towel under opposite shoulder for tilt + tourniquet alone
Additional Tips Specific to Bed-Based Cannulation
- Warm the arm — wrap with a warm towel for 3–5 minutes if vessel is still not palpable. Warmth causes vasodilation and further engorges the fistula.
- Your height matters — when the arm is hanging off a bed, you may need to sit on a low stool or kneel to cannulate at the right angle. Cannulating at an awkward angle from above increases the chance of through-and-through puncture.
- Stabilise the arm — ask a colleague to hold the arm steady while you cannulate if the patient is restless or sedated.
- Pre-fill the needle with heparinized saline — even more important in bed settings because positioning is suboptimal and you may need a moment to adjust after flashback.
This is a shared conversation. Sign in to Orris to start your own chat.