child, 10 years old, complaints of headache, an increase in body temperature to 36.8 °C, hemorrhagic rashes on the shins, thighs, buttocks, swelling of the knee and ankle joints, soreness when moving. It is known from the history of the disease that 3 weeks ago he was ill with ARVI, his mother gave paracetamol to reduce the temperature. Against the background of taking medications, fine-spotted rash appeared on the skin of the shins, swelling of the knee fonts, soreness in them when moving. A pediatrician called from the polyclinic regarded the symptoms as an allergic reaction to drug therapy. The patient was advised to stop taking anti-inflammatory drugs. Antihistamines are prescribed. After 2-3 days, the rashes and swelling of the joints disappeared, arthralgia stopped. In dynamics, the condition worsened again: hemorrhagic rashes appeared on the lower extremities, thighs, buttocks, swelling and soreness in the knee and ankle joints when moving, headache and weakness increased. Objectively: the patient's condition is moderate, the body temperature is 36,8 °C. The skin is pale, dry. On the skin of the extensor surfaces of the feet, shins, thighs, hemorrhagic rashes, sometimes having a drain character. The knee and ankle joints are enlarged in volume, movements in them are painful. Acute cramping pain in the abdomen every 5-7 minutes, during which the patient rushes and moans. In the lungs, respiration is vesicular, BH-20 per minute. The boundaries of the heart are within the normal range, the tones are muted, tachycardia is 100 per minute, the rhythm is correct, blood pressure is 100/60 mm Hg. Data from laboratory research methods. Clinical blood test: Hb-90 g / 1, leukocytes-12.6 x109/l, rod-shaped 12 %, c-65. cog.1-23 ESR-34 mm / h, platelets-180x109/1. Clinical analysis of urine: relative density-1015, protein-0.33 mg/l, red blood cells-0-1 in the field of vision.
Henoch-Schonlein purpura IgA vasculitis children
Henoch-Schonlein purpura hemorrhagic rash lower extremities child
Diagnosis: IgA Vasculitis (Henoch-Schönlein Purpura — HSP)
Why This Diagnosis Fits
| Feature | This Patient | Classic HSP |
|---|---|---|
| Age | 10 years | Peak 3–15 years |
| Preceding URTI | ARVI 3 weeks prior | ~50% have preceding infection |
| Rash location | Shins, thighs, buttocks (extensor, gravity-dependent) | Extensor surfaces, lower extremities, buttocks |
| Rash character | Hemorrhagic, confluent | Palpable purpura, non-blanching |
| Joint involvement | Knee + ankle, bilateral, painful swelling | 70–85%, lower extremity predominance |
| Abdominal pain | Cramping, colicky, every 5–7 min | Colicky, present in ~50% |
| Recurrence | Resolved then relapsed | ~1/3 of patients relapse |
| Platelets | 180 × 10⁹/L (normal) | Normal (key: distinguishes from ITP) |
| Urine | Protein 0.33 mg/L, RBCs 0–1 | Hematuria/proteinuria = renal involvement |
"IgAV is the most common form of systemic vasculitis in children and is characterized by IgA deposition in affected blood vessels. The classic tetrad of symptoms is a palpable purpuric rash, arthritis/arthralgia, abdominal pain, and kidney disease." — National Kidney Foundation Primer on Kidney Diseases, 8e
Pathophysiology
Clinical Picture of This Case
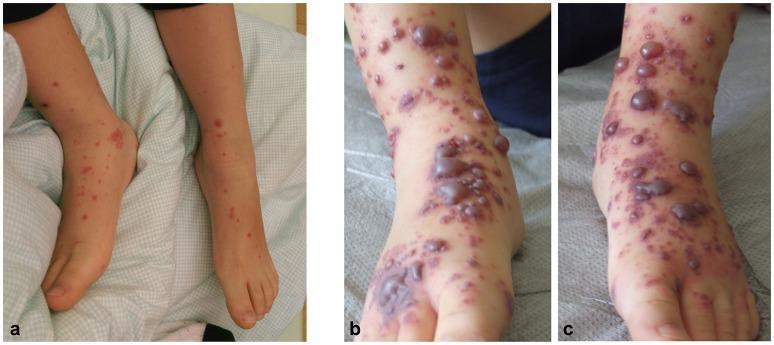
Lab Interpretation
| Lab | Value | Significance |
|---|---|---|
| Hb 90 g/L | Low | Anaemia — likely from GI blood loss and/or inflammatory state |
| Leukocytes 12.6 × 10⁹/L | Elevated | Inflammatory response |
| ESR 34 mm/h | Elevated | Active systemic inflammation |
| Platelets 180 × 10⁹/L | Normal | Critical: rules out ITP and TTP |
| Urine protein 0.33 mg/L | Positive | Early renal involvement |
| Urine RBC 0–1 | Borderline | Early microscopic haematuria |
Differential Diagnosis
| Condition | Why Less Likely |
|---|---|
| Drug allergy / urticaria | Non-palpable, blanching, urticarial — not purpuric; no systemic features |
| ITP | Thrombocytopenia expected; no joint or GI features |
| Septicaemia / meningococcaemia | High fever, toxic appearance, rapid deterioration; no colicky abdominal pain |
| Reactive arthritis | Joint-predominant, no purpura |
| Systemic lupus erythematosus | ANA/anti-dsDNA positive; butterfly rash, multi-system pattern differs |
| Kawasaki disease | Requires fever >5 days + specific mucocutaneous criteria |
Management
- Adequate hydration and rest
- NSAIDs (e.g., ibuprofen) for arthralgias and joint swelling — effective for pain
- Avoid nephrotoxic drugs
- Prednisone 1 mg/kg/day for 2 weeks, then 2-week taper — attenuates joint pain and GI symptoms
- Does not prevent the development of nephritis (confirmed by RCTs)
- Indicated when abdominal symptoms are severe (as in this child with colicky pain every 5–7 min)
- Urinalysis with protein and RBC at every visit
- Weekly for first 4–6 weeks, then monthly for 6 months
- If proteinuria worsens or GFR declines → nephrology referral and consider kidney biopsy
- Monitor for intussusception (ultrasound if worsening pain), GI bleeding
- This child's colicky pain every 5–7 minutes warrants abdominal ultrasound
- Pulsed methylprednisolone → oral prednisolone 3-month course
- Consider cyclophosphamide or azathioprine in refractory cases
Prognosis
- Typically self-limited, resolving in 3–4 weeks
- Recurrence in ~1/3 of patients (as seen in this child — initial episode "resolved," now relapsed)
- Renal prognosis: Most resolve spontaneously; ~10% of those with nephritis progress to CKD
- Long-term monitoring of blood pressure and proteinuria is warranted
"Most patients can be discharged to home from the ED with follow-up within 1 week for repeat urinalysis." — Tintinalli's Emergency Medicine, 9e
Key Takeaway on the Clinical Error
- Paracetamol (acetaminophen) rarely causes purpuric eruptions
- The rash was hemorrhagic and purpuric — not urticarial/maculopapular
- Joint swelling + colicky abdominal pain + normal platelets = HSP tetrad
- Recurrence after apparent resolution is characteristic of HSP, not drug allergy