Bipedal edema in old age
Reading File
Finding Sources
Finding Sources
Searching PubMed
"bilateral leg edema" AND "elderly" AND causes
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Finding Sources
Reading File
Reading File
Finding Sources
Reading File
Reading File
Reading File
Reading File
Loading Image
I now have comprehensive content from Harrison's and Guyton to provide a thorough answer. Let me compile everything.
Bipedal (Bilateral Lower Extremity) Edema in Old Age
Bilateral lower extremity (bipedal) edema is extremely common in the elderly. It results from accumulation of interstitial fluid and is almost always a sign of an underlying systemic or local condition rather than a normal aging change.
Pathophysiology
Edema forms when the balance between Starling forces favors fluid movement out of capillaries into the interstitium:
- Raised capillary hydrostatic pressure (heart failure, venous obstruction)
- Reduced plasma oncotic pressure (hypoalbuminemia)
- Increased capillary permeability (inflammation, drugs)
- Impaired lymphatic drainage (lymphedema)
In chronic heart failure specifically, the key mechanism is renal fluid retention driven by:
- Reduced glomerular filtration rate (from low cardiac output)
- Renin–angiotensin–aldosterone system activation → sodium and water retention
- Increased aldosterone secretion → tubular sodium reabsorption
- Increased ADH secretion → water reabsorption
This raises the mean systemic filling pressure, elevates right atrial pressure, and ultimately causes bilateral pitting edema. — Guyton and Hall, p. 282
Causes in the Elderly
Bilateral (Symmetric) Edema
| Cause | Key Features |
|---|---|
| Chronic heart failure | Elevated JVP, pitting, symmetric, sacral edema in bedridden patients; S3 gallop, displaced apex |
| Chronic venous insufficiency | Most common cause in ambulatory elderly; varicosities, hyperpigmentation, lipodermatosclerosis, stasis ulcers |
| Hypoalbuminemia — nephrotic syndrome, hepatic cirrhosis, protein malnutrition | Absent elevated JVP; low serum albumin |
| Drug-induced | Dihydropyridine calcium channel blockers (amlodipine, nifedipine), thiazolidinediones, NSAIDs, steroids |
| Hypothyroidism / myxedema | Non-pitting, doughy; pretibial myxedema in Graves' disease |
| Cor pulmonale / pulmonary hypertension | Right heart failure from COPD or pulmonary vascular disease |
| Constrictive pericarditis | Elevated JVP, Kussmaul's sign, pericardial knock |
| Immobility / dependency edema | Common in bedbound elderly; no JVP elevation |
"Dependent lower extremity edema is common in chronic HF and is typically symmetric and pitting. Over time, chronic edema may cause reddening and induration of the skin, become weeping, or lead to cellulitis." — Harrison's Principles of Internal Medicine, 22e, p. 2027
Unilateral Edema (consider before assuming bilateral cause)
- Deep vein thrombosis (DVT)
- Cellulitis
- Ruptured Baker's (popliteal) cyst
- Prior trauma / vein harvest surgery
- Lymphedema (though can be bilateral)
Key Clinical Features of Venous Insufficiency Edema
The most common cause of bilateral leg edema in mobile older adults is chronic venous insufficiency (CVI). Features include:
- Pitting edema greatest at ankles, worse after prolonged standing, relieved by elevation
- Stasis dermatitis: hyperpigmentation (hemosiderin deposition), eczema, lipodermatosclerosis
- Venous (stasis) ulcers: typically medial malleolus location
- Varicose veins; may have atrophie blanche
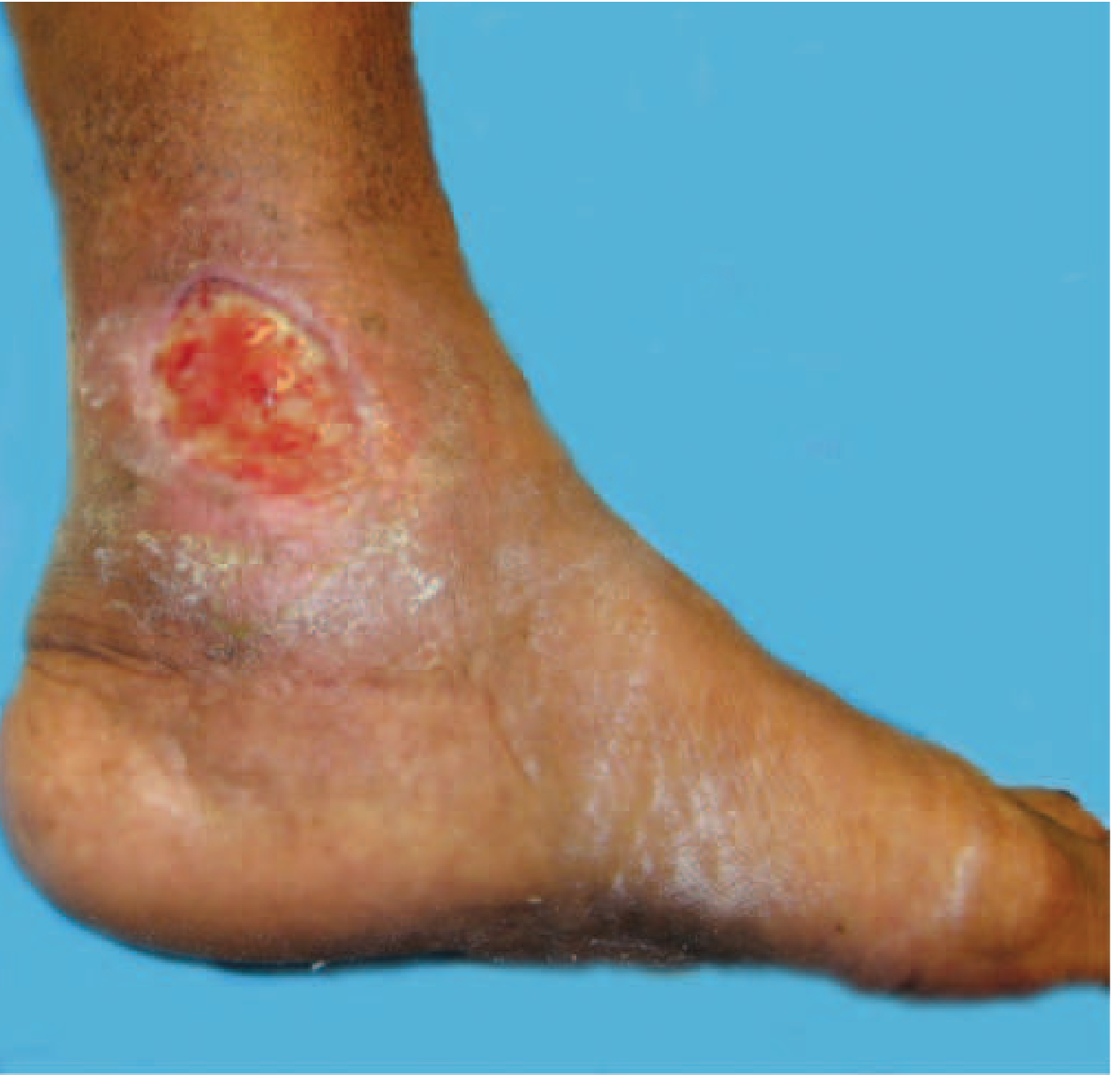
Venous ulcer with surrounding stasis changes — Harrison's Fig. 293-1
Over time, CVI can impair lymphatic drainage, leading to combined phlebo-lymphedema, where edema becomes less pitting and more indurated. — Harrison's, p. 2224
Diagnostic Approach
History:
- Duration and progression (acute → DVT; chronic → CVI or heart failure)
- Positional variation (worse on standing → venous; worse lying down → cardiac)
- Drug history (especially CCBs, thiazolidinediones)
- Dyspnea, orthopnea (→ heart failure)
- Systemic symptoms (fatigue, cold intolerance → hypothyroidism)
Examination:
- Jugular venous pressure (JVP): elevated → cardiac/constrictive; normal → venous/local/hypoalbuminemia
- Pitting vs. non-pitting: pitting → cardiac, renal, hepatic; non-pitting → lymphedema, myxedema
- Skin changes: hemosiderin, lipodermatosclerosis, ulcers → CVI
- Ascites: hepatic cirrhosis or right heart failure
Investigations:
| Test | Rationale |
|---|---|
| BNP / NT-proBNP | Elevated in heart failure |
| Serum albumin | Low → nephrotic, hepatic, malnutrition |
| Urine protein (spot protein:creatinine) | Nephrotic syndrome |
| TSH | Hypothyroidism |
| Renal function, LFTs | CKD, cirrhosis |
| Venous duplex ultrasound | CVI / DVT — first-line imaging |
| Echocardiogram | Confirms HF, pericardial disease, valvular etiology |
Management Principles
General
- Leg elevation above heart level for several hours daily — essential for both cardiac and venous edema
- Compression stockings (20–30 mmHg or higher) — cornerstone for CVI; contraindicated in significant PAD
- Mobility — calf muscle pump activation reduces venous pooling
- Salt and fluid restriction — for cardiac and renal causes
- Treat the underlying cause
Drug-Induced Edema
- Substitute dihydropyridine CCB (e.g., switch amlodipine to a non-DHP CCB or ACE-I/ARB if appropriate)
- Stop or reduce offending drugs (thiazolidinediones, NSAIDs)
Heart Failure
- Loop diuretics (furosemide) for symptomatic relief
- GDMT: ACE-I/ARB/ARNI + beta-blocker + MRA + SGLT2 inhibitor in HFrEF
Venous Insufficiency
- Compression therapy (first line)
- Wound care for stasis ulcers
- Avoid prolonged standing/sitting; frequent leg elevation
- Pentoxifylline for refractory venous ulcers
Aging-Specific Considerations
- Reduced muscle pump activity (sarcopenia, mobility limitation) contributes to venous pooling
- Polypharmacy: CCBs (extremely common in hypertensive elderly) are a frequently overlooked cause
- Multiple simultaneous causes are the rule rather than the exception in geriatric patients (e.g., CVI + heart failure + CCBs)
- Non-pitting edema in a bed-bound patient with sacral edema suggests anasarca from advanced heart failure or hypoalbuminemia
- Bilateral non-pitting edema that fails to respond to diuretics should prompt evaluation for lymphedema
Sources:
- Harrison's Principles of Internal Medicine, 22e — Chapters 246, 264, 293
- Guyton and Hall Textbook of Medical Physiology — Chapter 22
This is a shared conversation. Sign in to Orris to start your own chat.