Hi, I'm a year 4 mbbs student studying in Aimst university, Malaysia. Currently I'm in optal posting and having case presentation exam. I only have a rough history: Hasnah binti Ahmad 67 years SP0024086 Female, Malay DOA : 30/4/26, 9am Doc : 30/4 C/o Blurry vision HOPI 2 weeks a/w redness, LE glare Past History Thyroid disease 1 year diagnosis Dx : Graves ophthalmopathy, moderate to severe --- Physical Exam General Alert Sitting upright Oriented to tpp Prominent conjunctival redness Specific (thyroid) not done Ocular Lower lid retraction Injected conjunctiva Corneal haziness (exposure keratopathy) Periorbital swelling. Can you create a good presentation report for my exam please including the differentials, investigation and management
Graves ophthalmopathy management
CASE PRESENTATION REPORT
Opthalmology Posting — MBBS Year 4 | AIMST University
COVER PAGE
1. BIODATA
| Name | Hasnah binti Ahmad |
| Age | 67 years |
| Sex | Female |
| Race | Malay |
| Religion | Islam (presumed) |
| Hospital No. | SP0024086 |
| DOA | 30/04/2026 |
| Ward | Ophthalmology |
2. CHIEF COMPLAINT
3. HISTORY OF PRESENTING ILLNESS
- Redness of the left eye (LE)
- Glare/photophobia of the left eye
- Severity and progression of blurry vision (VA before vs. now)
- Any diplopia (double vision)?
- Any difficulty closing the eyes, especially during sleep (lagophthalmos)?
- Any sensation of grittiness or foreign body in the eye?
- Any colour vision changes (suggests optic nerve involvement)?
- Any proptosis noticed by patient or family?
4. PAST MEDICAL HISTORY
| Condition | Duration | Treatment |
|---|---|---|
| Thyroid disease (Graves' disease) | 1 year | Not documented — to be clarified |
- No known history of diabetes mellitus, hypertension, or ischaemic heart disease documented
- No prior ocular surgery or trauma
5. PAST SURGICAL HISTORY
6. DRUG & ALLERGY HISTORY
- Current thyroid medication: to be clarified (carbimazole / propylthiouracil / radioiodine / thyroxine?)
- No known drug allergy documented.
Note: If the patient underwent radioiodine therapy, this is a significant risk factor for worsening TED and must be documented.
7. FAMILY HISTORY
8. SOCIAL HISTORY
- Smoking history: Must be specifically elicited — smoking is the major modifiable risk factor for progression of TED. The greater the number of cigarettes smoked per day, the greater the risk; cessation reduces risk.
- Occupation, living situation, functional status — relevant given age 67.
9. SYSTEMIC REVIEW
- Thyrotoxic symptoms: weight loss despite good appetite, palpitations, heat intolerance, increased sweating, tremors, loose stools, irritability, menstrual irregularities
- Current thyroid status: Is patient euthyroid, hyperthyroid or hypothyroid?
10. PHYSICAL EXAMINATION
General Examination
- Alert, sitting upright, orientated to time, place, and person
- Prominent conjunctival redness noted on inspection
- To complete: Build (weight loss?), fine tremor of outstretched hands, pulse rate (tachycardia?), skin (warm, sweaty, palmar erythema), pre-tibial myxoedema, thyroid acropachy
Thyroid Examination
- Not performed (to be done — assess for goitre: diffuse enlargement, bruit, thrill)
Specific Ocular Examination
Visual Acuity (VA)
- Not documented — must be measured with Snellen chart (unaided and aided)
- Critical to determine if there is sight-threatening disease (optic neuropathy)
External Examination / Adnexa
| Sign | Findings |
|---|---|
| Lower lid retraction | Present |
| Periorbital swelling | Present |
- Upper lid signs to look for: Dalrymple sign (widened palpebral aperture), von Graefe sign (lid lag on down-gaze), Kocher sign (staring, frightened appearance)
- Proptosis: Assess with Hertel exophthalmometer — >20 mm or asymmetry >2 mm is significant
Anterior Segment
| Sign | Findings |
|---|---|
| Injected conjunctiva | Present — bilateral epibulbar hyperaemia (sensitive sign of inflammatory activity; may outline insertions of horizontal recti) |
| Corneal haziness | Present — exposure keratopathy secondary to incomplete lid closure |
- Further slit-lamp findings to assess: Corneal fluorescein staining (punctate epithelial erosions), corneal thinning/scarring, superior limbic keratoconjunctivitis
Extraocular Movements (EOM)
- Not documented — assess for restriction, especially upgaze (inferior rectus involvement) or diplopia
Fundoscopy / Posterior Segment
- Not documented — must be performed to rule out disc swelling or optic atrophy (signs of compressive optic neuropathy — the most serious complication)
11. CLINICAL ACTIVITY SCORE (CAS) — EUGOGO
| # | Feature | Present? |
|---|---|---|
| 1 | Spontaneous retrobulbar pain | ? |
| 2 | Pain on up- or down-gaze | ? |
| 3 | Redness of the eyelids | — |
| 4 | Redness of the conjunctiva | ✓ (injected conjunctiva) |
| 5 | Swelling of the eyelids | ✓ (periorbital swelling) |
| 6 | Inflammation of the caruncle or plica | ? |
| 7 | Chemosis | ? |
12. SEVERITY CLASSIFICATION — EUGOGO
| Severity | Criteria |
|---|---|
| Mild | Lid retraction <2 mm, mild soft tissue involvement, proptosis <3 mm above normal, no diplopia |
| Moderate-to-Severe | Lid retraction ≥2 mm, moderate-severe soft tissue signs, proptosis ≥3 mm above normal, intermittent or constant diplopia |
| Sight-Threatening | Compressive optic neuropathy ± corneal breakdown |
13. DIAGNOSIS
14. DIFFERENTIAL DIAGNOSES
| # | Differential | Supporting Features | Differentiating Features |
|---|---|---|---|
| 1. Orbital cellulitis | Periorbital swelling, redness, blurry vision | Fever, pain, proptosis, reduced EOM — acute presentation; no thyroid history | |
| 2. Idiopathic orbital inflammatory disease (orbital pseudotumour) | Periorbital oedema, injection, proptosis | Painful proptosis, unilateral, no thyroid disease association; responds well to steroids | |
| 3. Cavernous sinus thrombosis | Periorbital swelling, conjunctival injection | Severe headache, fever, bilateral signs, altered consciousness, CN III/IV/VI/V palsies | |
| 4. Conjunctivitis (bacterial/viral/allergic) | Redness, blurry vision, foreign body sensation | No lid retraction, no proptosis, no systemic thyroid disease; discharge often present | |
| 5. Ocular myasthenia gravis | Diplopia, ptosis, fatigable EOM | Ptosis rather than lid retraction, fatigability on sustained upgaze, positive edrophonium/ice test, anti-AChR antibodies | |
| 6. Superior ophthalmic vein thrombosis | Proptosis, chemosis, engorgement | Often secondary to cavernous sinus pathology; no thyroid disease | |
| 7. Orbital lymphoma / metastasis | Proptosis, periorbital mass | Firm mass on palpation, painless, no inflammatory features, CT/MRI shows discrete mass |
15. INVESTIGATIONS
A. Thyroid Function & Autoimmunity
| Investigation | Rationale |
|---|---|
| TSH (Thyroid Stimulating Hormone) | First-line; suppressed in hyperthyroidism |
| Free T3 & Free T4 | Confirm hyperthyroid state |
| TSH receptor antibodies (TRAb) / TSHR-Ab | Pathognomonic of Graves' disease; elevated in ~95% of TED |
| Anti-TPO antibody, Anti-Tg antibody | Associated autoimmune thyroid disease |
B. Ocular Investigations
| Investigation | Rationale |
|---|---|
| Snellen visual acuity (best corrected) | Baseline; monitor for optic neuropathy |
| Colour vision testing (Ishihara) | Desaturated colour vision = early optic nerve compression |
| Slit-lamp examination with fluorescein staining | Assess corneal epithelial defects (exposure keratopathy severity) |
| Hertel exophthalmometry | Measure proptosis quantitatively |
| Intraocular pressure (IOP) in primary and upgaze | Elevated IOP on upgaze suggests inferior rectus tethering |
| Visual fields (Humphrey perimetry) | Assess for field defects from optic nerve compression |
| Fundoscopy | Disc swelling, optic atrophy, choroidal folds |
C. Imaging
| Investigation | Rationale |
|---|---|
| CT orbit (axial + coronal, with contrast) | Gold standard — shows enlarged extraocular muscles (typically inferior and medial recti), orbital fat expansion, apical crowding |
| MRI orbit | Superior soft tissue detail; T2-weighted signal indicates muscle inflammation (active disease) |
| Thyroid ultrasound | Assess thyroid size, vascularity (hypervascular in Graves') |
D. General
| Investigation | Rationale |
|---|---|
| FBC | Baseline before starting steroids/immunosuppression; carbimazole can cause agranulocytosis |
| Fasting glucose / HbA1c | Rule out DM before steroid therapy; Graves' can cause glucose intolerance |
| LFTs | Baseline before steroid/immunosuppressive therapy; IV steroids contraindicated in significant hepatic dysfunction |
| Selenium level | Adjunct — selenium deficiency associated with TED; supplementation shown to slow progression |
| ECG | Thyrotoxicosis can cause AF; check before treatment |
16. MANAGEMENT
Immediate Priorities
- Refer to combined Ophthalmology + Endocrinology clinic
- Ensure euthyroid state — active TED is worsened by thyroid dysfunction in either direction
- Smoking cessation counselling — most important modifiable risk factor
A. Conservative (Supportive)
| Measure | Detail |
|---|---|
| Topical lubricants (artificial tears / lubricating ointment) | Relieve ocular surface symptoms from corneal exposure |
| Nocturnal eyelid taping | Prevents lagophthalmos and nocturnal corneal desiccation |
| Head elevation during sleep (3 pillows) | Reduces periorbital oedema |
| Sunglasses | Relieve photophobia/glare |
| Selenium supplementation | Sodium selenite 200 µg daily for 6 months in selenium-deficient patients — shown to improve quality of life and slow disease progression (double-blind RCT evidence) |
B. Medical — Moderate-to-Severe Active TED
- IV Methylprednisolone (preferred over oral — superior efficacy, better safety profile):
- 500 mg IV once weekly × 6 weeks, then 250 mg IV once weekly × 6 weeks
- Advantages: Higher treatment response, longer period to retreatment
- Contraindications: Significant hepatic dysfunction, cardiovascular disease, uncontrolled hypertension, uncontrolled diabetes
- Oral Prednisolone: 60–80 mg/day, tapered over months — used if IV not available; efficacy 33–63%
- IV methylprednisolone weekly + Mycophenolate sodium (0.72 g/day for 24 weeks) — superior to IV steroids alone; less disease reactivation
- Methotrexate — monotherapy if steroids not tolerated or patient is steroid-dependent
- Azathioprine — combined with radiotherapy or steroids (not effective alone)
- Teprotumumab (anti-IGF-1R antibody) — significant proptosis reduction; now first-line in some centres
- Tocilizumab (anti-IL-6R) — evidence of efficacy, especially steroid-refractory TED
- Rituximab (anti-CD20) — positive results in some trials; used in refractory cases
- Ensure and maintain euthyroid state (carbimazole / propylthiouracil / surgery)
- If radioiodine is planned, cover with a short course of oral steroids to prevent TED flare
C. Orbital Radiotherapy
- Second-line adjunct for soft tissue changes and EOM restriction
- 20 Gy in 10 fractions over 2 weeks
- Response evident at 6 weeks; maximal at 4 months (~40% non-responders)
- Used with steroids (not as sole treatment for acute optic neuropathy)
- Contraindicated in patients with diabetes (risk of radiation retinopathy)
D. Surgical Rehabilitation (Inactive Disease — Done in Sequence)
| Order | Procedure | Indication |
|---|---|---|
| 1st | Orbital decompression | Sight-threatening optic neuropathy; severe proptosis; cosmesis. Medial ± inferior ± lateral wall; endoscopic transnasal approach. Reduces proptosis 3.2–5.1 mm |
| 2nd | Strabismus surgery | Residual diplopia after decompression settles |
| 3rd | Eyelid surgery | Lid retraction correction (lower lid spacer graft, levator recession); exposure keratopathy |
E. Management of Exposure Keratopathy (This Patient)
- Intensive topical lubricants (preservative-free drops q1–2h + ointment at night)
- Eyelid taping at night
- Consider temporary tarsorrhaphy if keratopathy progresses despite conservative measures
- Urgent review if corneal staining worsens — risk of corneal ulceration/perforation
17. PROGNOSIS
- Most patients (>90%) with mild-moderate TED remain stable or improve over 1–3 years
- Moderate-to-severe disease may have residual soft tissue changes, proptosis, or diplopia even after treatment
- Smoking significantly worsens prognosis
- Sight-threatening complications (corneal ulceration, optic neuropathy) can cause permanent visual loss if untreated
18. PATIENT COUNSELLING POINTS
- TED is an autoimmune condition linked to her thyroid disease — managing the thyroid is essential
- Stop smoking — this is the single most important lifestyle modification
- Explain the natural history: active phase (6–24 months) followed by inactive/stable phase
- Surgery (if needed) is only done after the disease is stable — not during the active phase
- Regular follow-up with both ophthalmology and endocrinology is mandatory
- Side effects of steroid therapy must be discussed: weight gain, mood changes, glucose intolerance, peptic ulcer disease, osteoporosis, avascular necrosis of hip
SUMMARY STATEMENT (for oral presentation)
"Madam Hasnah binti Ahmad is a 67-year-old Malay female with a 1-year history of Graves' disease who presented with a 2-week history of blurry vision associated with left eye redness and glare. On examination, she was alert and orientated, with lower lid retraction, injected conjunctiva, corneal haziness consistent with exposure keratopathy, and periorbital swelling. These findings are in keeping with a diagnosis of Graves' Ophthalmopathy, moderate-to-severe severity, currently in the active phase. Management priorities include confirming thyroid status, quantifying ocular involvement with CAS scoring, initiating IV methylprednisolone with mycophenolate for active disease, intensive topical lubricants for corneal protection, and strict smoking cessation counselling. Combined ophthalmology-endocrinology follow-up is essential."
- Always state the CAS score — examiners love this scoring system
- The sequence of surgery (decompression → strabismus → eyelid) is a classic exam favourite
- Emphasise smoking cessation as the #1 modifiable risk factor
- Know the contraindications to IV steroids (hepatic dysfunction, uncontrolled DM/HPT, CV disease)
- For this patient, the corneal haziness needs urgent attention — mention tarsorrhaphy as an option
Can you give expected viva questions for this presentation and prepare me for the case
VIVA PREPARATION GUIDE
Graves' Ophthalmopathy | Hasnah binti Ahmad
HOW EXAMINERS BUILD THE VIVA
Diagnosis → Mechanism → Classification → Signs → Investigations → Management → Complications → Emergencies → Exam-specific traps
BLOCK 1 — DIAGNOSIS & DEFINITIONS
"My diagnosis is Graves' Ophthalmopathy, moderate-to-severe severity, in the active phase. I arrived at this based on:
- Known history of Graves' disease (thyroid disease diagnosed 1 year ago)
- Clinical triad of lid retraction, periorbital swelling, and injected conjunctiva
- Corneal haziness consistent with exposure keratopathy — a direct complication of lid retraction and proptosis
- Blurry vision and glare, indicating ocular surface compromise Severity is classified as moderate-to-severe because of the combination of lid retraction, significant soft tissue involvement, and corneal compromise."
"Graves' Ophthalmopathy, also called Thyroid Eye Disease (TED) or thyroid-associated orbitopathy, is an autoimmune inflammatory condition of the orbit and periorbital tissues. It is the most common cause of both unilateral and bilateral proptosis in adults. It is most commonly associated with Graves' disease but can occur in euthyroid patients and, rarely, in Hashimoto's thyroiditis."
"Yes. About 10% of TED patients are euthyroid at presentation. These individuals usually have anti-thyroid antibodies or autoimmune hypothyroidism. The onset of TED can precede, coincide with, or follow the diagnosis of thyrotoxicosis — in 75% of cases it occurs within 1 year of thyroid diagnosis."
BLOCK 2 — PATHOPHYSIOLOGY
"The underlying mechanism is autoimmune. TSH receptor antibodies (TRAb/TSHR-Ab) that drive Graves' hyperthyroidism also bind to TSH receptors expressed on orbital fibroblasts. This triggers:
- Proliferation of orbital fibroblasts → differentiate into adipocytes (fat expansion) or myofibroblasts
- Upregulation of IGF-1 receptor on fibroblasts (synergises with TSH receptor activation)
- Glycosaminoglycan (hyaluronic acid) accumulation → osmotic water retention → orbital oedema
- Extraocular muscle enlargement — primarily the muscle belly (spares tendons, unlike orbital myositis)
- The net result is increased orbital volume in a rigid bony orbit → proptosis, compressive optic neuropathy, venous congestion"
"Two mechanisms:
- Sympathetic overstimulation of Müller's muscle (smooth muscle) due to high circulating thyroid hormones — occurs in any thyrotoxic state
- Fibrotic contracture of the levator palpebrae and inferior rectus muscles with adhesion to overlying orbital tissues — specific to Graves' ophthalmopathy Lower lid retraction is caused by fibrosis and tethering of the inferior rectus to the lower lid retractors."
"The mnemonic is I'M SLow (in order of frequency):
- Inferior rectus — most commonly
- Medial rectus — second
- Superior rectus/levator complex
- Lateral rectus — least common
Importantly, the muscle belly is enlarged but tendons are spared — this helps distinguish TED from orbital myositis on CT/MRI."
BLOCK 3 — CLINICAL SIGNS
Lid signs:
- Dalrymple sign — lid retraction in primary gaze (widened palpebral fissure)
- von Graefe sign — lid lag on downgaze (upper lid fails to follow globe)
- Kocher sign — staring/frightened expression on attentive fixation
- Stellwag sign — infrequent blinking
Soft tissue signs:
- Periorbital oedema
- Conjunctival injection / epibulbar hyperaemia (especially overlying horizontal recti insertions)
- Chemosis
- Caruncular/plical swelling
Proptosis (exophthalmos)EOM restriction → diplopia (typically upgaze first, due to inferior rectus tethering)Corneal signs: Punctate epithelial erosions, exposure keratopathy, superior limbic keratoconjunctivitisOptic nerve signs: Disc swelling, optic atrophy, reduced acuity, colour vision loss, RAPD, field defects
"Dalrymple sign is lid retraction in primary gaze — the upper lid sits above the superior limbus, revealing scleral show. Von Graefe sign is lid lag on downgaze — the upper lid fails to descend at the same speed as the globe when the patient looks down."
"The corneal haziness is due to exposure keratopathy. Lower lid retraction (present in this patient) causes the lower cornea to be constantly exposed. Combined with incomplete lid closure (lagophthalmos), the corneal epithelium desiccates, breaks down, and can develop punctate erosions, corneal haze, and if severe — ulceration, secondary bacterial infection, and corneal scarring. This is a serious complication that can permanently affect vision."
BLOCK 4 — CLASSIFICATION SYSTEMS
"The preferred system is the EUGOGO (European Group on Graves' Orbitopathy) classification:
Severity Features Mild Lid retraction <2 mm, mild soft tissue signs, proptosis <3 mm above normal, no diplopia, normal VA Moderate-to-Severe Lid retraction ≥2 mm, moderate/severe soft tissue signs, proptosis ≥3 mm above normal, intermittent/constant diplopia Sight-Threatening Compressive optic neuropathy OR corneal breakdown This patient classifies as Moderate-to-Severe based on lid retraction, periorbital swelling, injected conjunctiva, and corneal compromise."
"The CAS is a 7-point scoring system to assess inflammatory activity — it tells us whether the disease is active (and will respond to immunosuppression) versus inactive (and requires surgical rehabilitation).One point is given for each:
- Spontaneous retrobulbar pain
- Pain on eye movement
- Eyelid redness
- Conjunctival injection ✓
- Periorbital/eyelid swelling ✓
- Chemosis
- Inflammation of caruncle/plica
CAS ≥ 3/7 = active disease → immunosuppressive treatment warrantedThis patient scores at least 2 from documented findings; further assessment needed for the full score."
"NO SPECS is a mnemonic for the 7 classes of TED:
- 0 = No signs or symptoms
- I = Only signs (lid retraction/lag)
- II = Soft tissue involvement (periorbital oedema, chemosis)
- III = Proptosis (>22 mm)
- IV = EOM involvement (diplopia)
- V = Corneal involvement
- VI = Sight loss (optic neuropathy)
It is now considered inadequate because patients don't necessarily progress sequentially. EUGOGO + CAS are preferred in modern practice."
BLOCK 5 — INVESTIGATIONS
"TSH receptor antibodies (TRAb/TSHR-Ab). They are elevated in ~95% of patients with TED and are pathognomonic of Graves' disease. They also correlate with disease activity and can be used to monitor treatment response."
"CT orbit (axial and coronal, with contrast) is the gold standard. Expected findings:
- Enlarged extraocular muscle bellies with tendon sparing (distinguishes from orbital myositis)
- Predominant enlargement of inferior and medial recti
- Increased orbital fat volume
- Apical crowding — muscles crowding the orbital apex, compressing the optic nerve at the orbital apex — this is the mechanism of compressive optic neuropathy
MRI orbit is preferred for soft tissue detail and uses T2-weighted signal to assess inflammation/activity — bright T2 = active, inflammatory muscles."
"Fluorescein staining under cobalt blue light on slit lamp reveals corneal epithelial defects. Punctate staining indicates superficial punctate keratopathy from exposure. Larger defects indicate epithelial erosions or frank ulceration. This determines the urgency of corneal protection — if large or central, urgent intervention (tarsorrhaphy) is needed to prevent vision-threatening corneal scarring."
BLOCK 6 — MANAGEMENT
"My management is based on Moderate-to-Severe, Active TED. I would approach it in three pillars:1. Supportive:
- Intensive topical lubricants (preservative-free, q1–2h during day + ointment at night)
- Nocturnal eyelid taping to prevent corneal desiccation
- Head elevation during sleep
- Smoking cessation counselling — the most important modifiable risk factor
2. Medical (Active Disease):
- First-line: IV Methylprednisolone 500 mg weekly × 6 weeks, then 250 mg weekly × 6 weeks
- Combined with Mycophenolate sodium 0.72 g/day for 24 weeks for superior outcomes
- Monitor LFTs, blood glucose, blood pressure
- Ensure and maintain euthyroid state throughout
3. Surgical (only when disease is inactive/stable — ≥6 months):
- Done in strict sequence: orbital decompression → strabismus surgery → eyelid surgery
For this patient specifically: The corneal haziness requires urgent attention — intensive lubricants, eyelid taping; if the cornea deteriorates, consider temporary tarsorrhaphy."
"IV methylprednisolone is superior to oral prednisolone in TED for three reasons:
- Better efficacy — higher response rate and longer time before needing retreatment
- Better safety profile — lower cumulative dose, fewer systemic side effects
- Faster onset of soft tissue response The oral route is used only when IV is unavailable or not tolerated. However, IV steroids are contraindicated in significant hepatic dysfunction, major cardiovascular disease, uncontrolled hypertension, or uncontrolled diabetes."
"Selenium supplementation — sodium selenite 200 µg/day for 6 months — has Level 1 evidence (double-blind RCT) showing:
- Improved quality of life
- Decreased soft tissue involvement
- Slowed disease progression in mild, active TED The benefit is greatest in selenium-deficient populations. It acts via selenoproteins, which regulate oxidative stress and T3 production. Serum levels should be monitored as excess selenium is associated with diabetes, neurotoxicity, and glaucoma."
"The sequence is strictly: Decompression → Strabismus → Eyelid
- Orbital decompression first — because it changes orbital anatomy, which can induce or change strabismus. If you do strabismus surgery first, the decompression will undo your correction.
- Strabismus surgery second — corrects diplopia after the orbit has been decompressed and stabilised.
- Eyelid surgery last — because strabismus surgery changes orbital and lid mechanics; lid surgery should be the final refinement.
All surgery is done only when the disease has been inactive and stable for ≥6 months."
"Teprotumumab is a monoclonal antibody targeting the IGF-1 receptor (IGF-1R) on orbital fibroblasts. Since IGF-1R synergises with TSH receptor signalling in TED pathogenesis, blocking it reduces orbital fibroblast activation. Clinical trials have shown significant reduction in proptosis and CAS. It is now approved by the FDA and used as first-line therapy for moderate-to-severe TED in some centres, particularly in the United States."
BLOCK 7 — COMPLICATIONS & EMERGENCIES
"Dysthyroid optic neuropathy (DON) — compression of the optic nerve at the orbital apex by enlarged extraocular muscles. It is sight-threatening and constitutes an ophthalmological emergency.Features to recognise:
- Reduced visual acuity (especially colour vision — use Ishihara plates)
- Relative afferent pupillary defect (RAPD)
- Visual field defects (central scotoma, inferior altitudinal defect)
- Disc swelling on fundoscopy
Management: IV methylprednisolone 1 g/day × 3 days — if no improvement in 2 weeks, urgent orbital decompression surgery."
"Red flags requiring urgent intervention:
- Large/central fluorescein staining defect
- Corneal ulceration — risk of perforation and endophthalmitis
- Secondary bacterial keratitis
- Corneal thinning/descemetocele
Action: Urgent temporary tarsorrhaphy (lateral or central), intensive topical lubricants + antibiotics if infected, admit the patient."
"Systemic: glucose intolerance, weight gain, mood changes/psychosis, peptic ulcer disease (cover with PPI), hypertension, osteoporosis (calcium + vitamin D supplementation), avascular necrosis of the femoral head.Hepatic: acute liver injury (rare but potentially fatal) — LFTs must be checked before and during treatment. Contraindicated if significant liver disease.Ophthalmological: posterior subcapsular cataract, raised intraocular pressure."
BLOCK 8 — RISK FACTORS & ASSOCIATIONS
"1. Smoking — the strongest modifiable risk factor; dose-dependent relationship; cessation reduces risk 2. Radioiodine therapy — can precipitate or worsen TED; cover with steroids if TED is pre-existing 3. Female sex — 5× more commonly affected (though largely reflects Graves' disease incidence) 4. High TRAb levels — correlate with TED severity 5. Thyroid dysfunction — both hyper- and hypothyroidism worsen TED; euthyroid state is protective"
"Smoking is the single most important modifiable risk factor for TED. It increases the risk of developing TED in Graves' patients, worsens severity, and reduces response to treatment (including radioiodine and immunosuppression). Smoking cessation should be the very first intervention offered, regardless of TED severity."
BLOCK 9 — CLASSIC EXAM TRAPS
"Yes, absolutely. In 75% of patients, TED onset occurs within 1 year before or after the diagnosis of thyrotoxicosis. The conditions are autoimmune siblings sharing the TSH receptor as the target antigen. TED can even precede thyroid disease by several years or appear in fully euthyroid patients."
"Lower lid retraction in TED is caused by fibrosis and adhesion of the inferior rectus muscle to the lower lid retractors (capsulopalpebral fascia). As the inferior rectus becomes fibrotic and tethered, it pulls the lower lid downward, revealing inferior scleral show. Upper lid retraction, on the other hand, is from levator/Müller's overaction."
"No. Normal VA at presentation does not exclude early dysthyroid optic neuropathy (DON). Colour vision loss, particularly red desaturation, is often the earliest sign of optic nerve compression — it may be abnormal before Snellen acuity drops. RAPD and visual field defects may also precede VA loss. This is why a full ocular assessment including colour vision, Humphrey fields, and fundoscopy is mandatory."
"Yes. Although TED is most commonly associated with Graves' disease (~95% of cases), it can occur with:
- Hashimoto's thyroiditis (rarely)
- Euthyroid Graves' (10%) — TED with normal thyroid function tests but positive TRAb
- Post-radioiodine hypothyroidism The diagnosis in euthyroid cases is primarily clinical, supported by TRAb positivity and orbital imaging."
"Clinically used interchangeably, but technically:
- Proptosis = any anterior displacement of the globe from any cause
- Exophthalmos = proptosis specifically due to endocrine/thyroid-related orbital disease
Measured with a Hertel exophthalmometer. Normal <20 mm; asymmetry >2 mm is significant. In TED, >20 mm constitutes proptosis."
"Any of the following:
- Reduced visual acuity unexplained by corneal or lens pathology
- Loss of colour vision (red desaturation)
- RAPD
- Visual field defects
- Disc swelling or optic atrophy on fundoscopy
- Corneal ulceration / descemetocele / perforation
These indicate either compressive optic neuropathy or corneal breakdown — both are ophthalmological emergencies requiring immediate IV methylprednisolone and/or urgent orbital decompression."
QUICK-FIRE SUMMARY TABLE
| Question | Key Answer |
|---|---|
| Most common cause of bilateral proptosis in adults | Graves' Ophthalmopathy |
| Autoantibody responsible | TSH receptor antibody (TRAb) |
| Most commonly enlarged EOM | Inferior rectus |
| Most important modifiable RF | Smoking |
| Activity scoring system | Clinical Activity Score (CAS) — ≥3/7 = active |
| Severity classification | EUGOGO (Mild / Moderate-Severe / Sight-threatening) |
| First-line treatment for moderate-severe active | IV Methylprednisolone + Mycophenolate |
| Surgical sequence | Decompression → Strabismus → Eyelid |
| Earliest sign of optic neuropathy | Colour vision loss (red desaturation) |
| Emergency management of DON | IV methylprednisolone 1g/day × 3 days → decompression |
| Selenium dose | 200 µg/day × 6 months (mild active TED) |
| IV steroid regimen (mod-severe) | 500 mg weekly × 6 weeks, then 250 mg × 6 weeks |
| Imaging of choice | CT orbit (axial + coronal) |
| CT hallmark finding | Muscle belly enlargement with tendon sparing |
Graves' Ophthalmopathy 101 please
Graves ophthalmopathy thyroid eye disease proptosis lid retraction clinical signs
Graves ophthalmopathy pathogenesis orbital fibroblast GAG mechanism diagram
GRAVES' OPHTHALMOPATHY 101
A Complete Visual Guide for the MBBS Student
1. WHAT IS IT?
- Thyroid Eye Disease (TED) ← most modern term
- Thyroid-Associated Orbitopathy (TAO)
"TED is the most common cause of both unilateral and bilateral proptosis in adults." — Kanski's Clinical Ophthalmology, 10th Ed.
2. WHO GETS IT?
| Factor | Detail |
|---|---|
| Most common association | Graves' disease (autoimmune hyperthyroidism) — ~95% |
| Can occur in euthyroid | ~10% — called "euthyroid Graves' ophthalmopathy" |
| Can occur in hypothyroid | Rarely — e.g. Hashimoto's thyroiditis |
| Sex | Females 5× more common (mirrors Graves' disease incidence) |
| Age | 4th–5th decade typical; but any age |
| Timing vs thyroid disease | 75% of cases: TED occurs within 1 year before or after thyroid diagnosis |
Risk Factors
🚬 Smoking ————————→ #1 modifiable risk factor (dose-dependent)
☢️ Radioiodine therapy → can precipitate/worsen TED
⬆️ High TRAb levels ——→ predicts TED severity
❌ Thyroid dysfunction —→ both hyper- AND hypo- worsen TED
3. PATHOGENESIS — HOW DOES IT HAPPEN?
STEP 1: AUTOIMMUNE TRIGGER
TSH receptor antibodies (TRAb) are produced
↓
STEP 2: ORBITAL FIBROBLAST ACTIVATION
TRAb binds TSH receptors (TSHR) on orbital fibroblasts
IGF-1 receptor (IGF-1R) is also upregulated — synergises
↓
STEP 3: TWO PARALLEL PROCESSES
(A) Fibroblasts → ADIPOCYTES → orbital FAT EXPANSION
(B) Glycosaminoglycan (hyaluronic acid) secretion
→ osmotic water retention → EXTRAOCULAR MUSCLE SWELLING
→ muscles can swell up to 8× their normal size
↓
STEP 4: CONSEQUENCES
Increased orbital volume in a RIGID BONY BOX
→ Proptosis (globe pushed forward)
→ Apical crowding → optic nerve compression
→ Lid retraction, EOM restriction, corneal exposure
Key teaching point: This is why we treat early (active phase) — once fibrosis sets in, anti-inflammatory treatment no longer works.
4. CLINICAL FEATURES — THE BIG PICTURE
| Phase | Also Called | Eyes Look | Duration | Treatment works? |
|---|---|---|---|---|
| Active (Congestive) | Inflammatory | Red, swollen, painful | 6 months – 3 years | ✅ YES — steroids/immunosuppression |
| Inactive (Fibrotic) | Quiescent | White, quiet | Permanent | ❌ Anti-inflammatory no longer helps → surgery |
5. CLINICAL SIGNS — HEAD TO TOE
Clinical Photo: Active TED Before & After Treatment
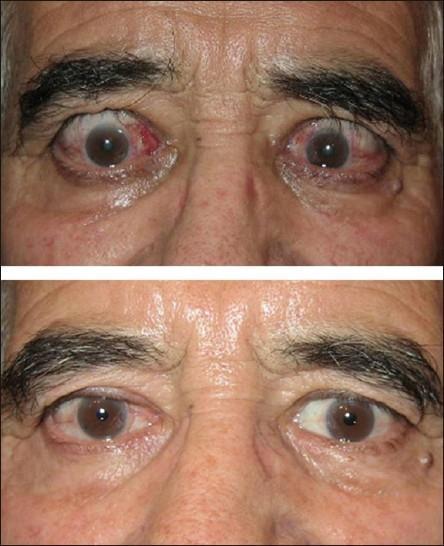
A. LID SIGNS
| Sign | What It Means | How to Elicit |
|---|---|---|
| Dalrymple sign | Lid retraction in primary gaze — upper lid sits above superior limbus (scleral show) | Look at patient in primary gaze |
| von Graefe sign | Lid lag on downgaze — lid doesn't descend with globe | Ask patient to follow your finger slowly downward |
| Kocher sign | Staring, frightened expression on attentive fixation | Observe patient looking at a target |
| Stellwag sign | Infrequent blinking | Count blinks per minute |
Memory tip: "Dalrymple = Daytime (primary gaze) | von Graefe = vertical downgaze"
- Sympathetic overstimulation of Müller's muscle (any thyrotoxic state)
- Fibrotic contracture of levator palpebrae adhesion to orbital tissues (specific to GO)
B. SOFT TISSUE SIGNS
- Periorbital oedema — caused by oedema and fat infiltration behind the orbital septum
- Conjunctival injection — especially epibulbar hyperaemia overlying the horizontal recti insertions (sensitive activity sign)
- Chemosis — conjunctival oedema/boggy appearance
- Caruncle/plica swelling
- Tear insufficiency — very common, causes grittiness
C. PROPTOSIS (EXOPHTHALMOS)
- Globe displaced anteriorly due to increased orbital volume
- Measured with Hertel exophthalmometer
- Normal: <20 mm | Significant asymmetry: >2 mm difference
- Check: visible sclera between inferior limbus and lower lid in primary gaze
- Axial proptosis (straight forward) = typical of TED (unlike eccentric proptosis seen in tumours)
D. EXTRAOCULAR MUSCLE (EOM) INVOLVEMENT
Inferior rectus ——→ Most common → upgaze restriction (diplopia on looking up)
Medial rectus ——→ 2nd → abduction restriction
Superior rectus ——→ 3rd
Lateral rectus ——→ Least common
CT hallmark: Muscle BELLY enlargement with TENDON SPARING — this distinguishes TED from orbital myositis (which involves tendons too)
E. CORNEAL SIGNS
- Exposure keratopathy — incomplete lid closure → corneal desiccation → haziness (as in Madam Hasnah)
- Superficial punctate keratopathy — fluorescein staining
- Superior limbic keratoconjunctivitis (SLK)
- Severe: corneal ulceration, thinning, scarring, perforation
F. OPTIC NERVE INVOLVEMENT (Sight-Threatening!)
- Caused by apical crowding — enlarged muscles compress optic nerve at orbital apex
- Occurs in 5–7% of TED patients — but must be excluded at EVERY visit
- Key: often occurs with mild or absent proptosis (the muscles are crowding inward, not pushing out)
6. INVESTIGATIONS
Blood Tests
| Test | Why |
|---|---|
| TSH | First line; suppressed in hyperthyroidism |
| Free T3 & Free T4 | Confirm thyroid status |
| TRAb (TSH receptor antibodies) | Elevated in ~95% of TED; pathognomonic; monitor activity |
| Anti-TPO / Anti-Tg | Associated autoimmune thyroid disease |
| FBC, LFTs, glucose | Before starting steroids/immunosuppression |
| Selenium levels | Adjunct in mild TED |
Ocular Assessments
| Test | Why |
|---|---|
| Snellen VA | Baseline and monitor |
| Colour vision (Ishihara) | Earliest sign of optic neuropathy — red desaturation |
| RAPD (swinging torch test) | Asymmetric optic nerve involvement |
| Humphrey visual fields | Field defects from optic compression |
| Hertel exophthalmometry | Quantify proptosis |
| IOP in primary + upgaze | Elevated IOP on upgaze = inferior rectus tethering |
| Slit lamp + fluorescein | Corneal staining — severity of exposure keratopathy |
| Fundoscopy | Disc swelling (early DON) or optic atrophy (late DON) |
Imaging
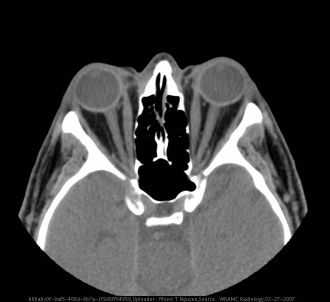
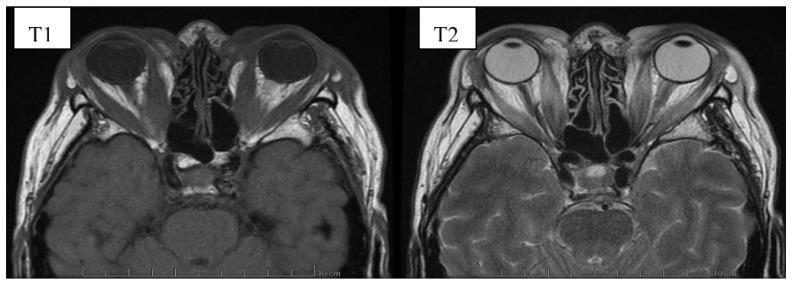
7. CLASSIFICATION SYSTEMS
A. EUGOGO Severity (What to Treat)
MILD ──────────────────────────────────────────────
• Lid retraction < 2 mm
• Mild soft tissue signs
• Proptosis < 3 mm above normal
• No diplopia / transient
• Corneal exposure responding to lubricants
• VA normal
MODERATE-TO-SEVERE ────────────────────────────────
• Lid retraction ≥ 2 mm
• Moderate-severe soft tissue signs
• Proptosis ≥ 3 mm above normal
• Intermittent or constant diplopia
SIGHT-THREATENING ─────────────────────────────────
• Dysthyroid optic neuropathy (DON)
• Corneal breakdown
→ EMERGENCY
B. Clinical Activity Score (CAS) — Is It Active?
1. Spontaneous retrobulbar pain
2. Pain on eye movement (up/down)
3. Redness of eyelids
4. Redness of conjunctiva ← Madam Hasnah ✓
5. Periorbital/eyelid swelling ← Madam Hasnah ✓
6. Conjunctival chemosis/plica swelling
7. Caruncle swelling
Score can extend to 10 during follow-up by adding: +1 for ≥2 mm proptosis increase, +1 for ≥8° EOM restriction decrease, +1 for ≥1 line VA decrease
C. Old NO SPECS (Harrison's) — Still Tested in Exams
| Class | Meaning |
|---|---|
| 0 | No signs or symptoms |
| I | Only signs (lid retraction/lag) |
| II | Soft tissue involvement |
| III | Proptosis >22 mm |
| IV | EOM involvement (diplopia) |
| V | Corneal involvement |
| VI | Sight loss (optic neuropathy) |
8. MANAGEMENT — THE FULL ALGORITHM
ALL PATIENTS
│
├─ Stop smoking (most important modifiable step)
├─ Maintain euthyroid state
├─ Topical lubricants + lid taping at night
└─ Head elevation (3 pillows)
│
├── MILD ACTIVE TED
│ Selenium 200 µg/day × 6 months
│ Topical lubricants / NSAIDs
│ Sunglasses
│
├── MODERATE-TO-SEVERE ACTIVE TED (CAS ≥ 3)
│ First line: IV Methylprednisolone
│ 500 mg weekly × 6 weeks
│ then 250 mg weekly × 6 weeks
│ + Mycophenolate sodium 0.72g/day × 24 weeks
│ (combined = better than steroids alone)
│
│ Orbital Radiotherapy (2nd line, adjunct)
│ 20 Gy / 10 fractions over 2 weeks
│ ⚠️ Contraindicated in diabetes
│
│ Biologics (specialist/refractory):
│ Teprotumumab (anti-IGF-1R) — FDA approved 2020
│ Tocilizumab (anti-IL-6R)
│ Rituximab (anti-CD20)
│
├── SIGHT-THREATENING (DON or corneal breakdown)
│ EMERGENCY
│ IV Methylprednisolone 1 g/day × 3 days
│ → No response in 2 weeks → URGENT decompression surgery
│
└── INACTIVE DISEASE — Surgical Rehabilitation
(In strict sequence — only when stable ≥6 months)
1st: Orbital decompression
2nd: Strabismus surgery
3rd: Eyelid surgery
9. THE SURGICAL SEQUENCE — WHY THIS ORDER?
WHY DECOMPRESSION FIRST?
→ Changes orbital anatomy → will alter/cause strabismus
→ Must do BEFORE strabismus surgery
WHY STRABISMUS SECOND?
→ Correct diplopia after orbit has settled
→ EOM surgery changes lid mechanics
WHY EYELID LAST?
→ Both decompression and strabismus surgery change lid position
→ Eyelid surgery is the final refinement
- Medial wall (lamina papyracea) and/or inferior wall most common
- Endoscopic transnasal approach preferred
- Reduces proptosis by 3.2–5.1 mm per wall
- Most common complication: new-onset diplopia (19–45%)
10. DYSTHYROID OPTIC NEUROPATHY (DON) — THE EMERGENCY
MECHANISM:
Enlarged muscle bellies → crowd orbital apex → compress optic nerve
(Note: proptosis is often ABSENT or MILD — the muscles push IN not OUT)
EARLIEST SIGN: Colour vision loss (red desaturation)
Test with Ishihara plates
OTHER SIGNS:
• Reduced VA (late sign)
• RAPD
• Central scotoma or inferior altitudinal field defect
• Disc swelling (early) → optic atrophy (late)
MANAGEMENT:
• IV methylprednisolone 1 g/day × 3 days
• If no improvement in 2 weeks → urgent posterior orbital decompression
• Do NOT delay — permanent visual loss if untreated
Key exam pearl: DON typically occurs WITHOUT significant proptosis — it's the apical crowding that matters, not how far the eye bulges out.
11. NATURAL HISTORY — RUNDLE'S CURVE
SEVERITY
▲
│ ╭──────╮ ← Peak of active phase
│ ╱ ╲
│ ╱ ╲──────────────→ Plateau (residual)
│ ╱
│────╱
└──────────────────────────────────→ TIME
Active inflammatory phase: 6 months – 3 years
After the peak: spontaneous partial improvement, then plateau at residual level
- Only ~10% develop serious long-term ocular problems
- Anti-inflammatory treatment is only effective during the active phase
- Surgery addresses residual deformity in the inactive plateau
12. ONE-PAGE CHEAT SHEET
| Topic | Key Point |
|---|---|
| Definition | Autoimmune orbital inflammation; most common cause of proptosis in adults |
| Antibody | TRAb (TSH receptor antibody) |
| Target | Orbital fibroblasts expressing TSHR + IGF-1R |
| Pathology | GAG accumulation + adipogenesis → muscle swelling + fat expansion → raised orbital pressure |
| Most common EOM | Inferior rectus (upgaze restricted first) |
| CT hallmark | Muscle belly enlargement + tendon sparing |
| MRI activity | T2 bright = active |
| Severity tool | EUGOGO (Mild / Moderate-Severe / Sight-Threatening) |
| Activity tool | CAS ≥ 3/7 = treat with immunosuppression |
| #1 risk factor | Smoking |
| Radioiodine | Worsens TED — cover with steroids |
| Mild treatment | Lubricants + Selenium 200 µg × 6 months |
| Mod-severe treatment | IV methylprednisolone + mycophenolate |
| Earliest DON sign | Colour vision loss (not VA!) |
| DON emergency | IV methylprednisolone 1g/day → decompression if no response |
| Surgical order | Decompression → Strabismus → Eyelid |
| New biologic | Teprotumumab (anti-IGF-1R, FDA 2020) |
Can you interpret it