Bechets disease
Reading File
Finding Sources
Searching PubMed
"Behcet disease"[MeSH Terms] AND management
Reading File
Reading File
Searching Images
Behcet disease oral ulcers skin lesions pathergy
Finding Sources
Reading File
Reading File
Reading File
Loading Image
Loading Image
Here is a comprehensive overview of Behçet Disease:
Behçet Disease (Adamantiades–Behçet Disease)
Definition & Overview
Behçet disease (BD) is a multisystem inflammatory disorder of unknown etiology, classified as a systemic vasculitis involving all types and sizes of blood vessels. It is characterized by recurrent oral aphthous ulcers, genital ulcers, skin lesions, uveitis, and arthritis, with variable involvement of vascular, GI, and neurologic systems. — Fitzpatrick's Dermatology, Ch. 141
Epidemiology
- Prevalent along the "Silk Road" — highest rates in Turkey (80–420 per 100,000), followed by the Middle East and East Asia (Japan 14–31, Korea 35, Iran 17 per 100,000)
- Rare in Northern Europe (0.27–1.18 per 100,000) and the USA (0.75 per 100,000)
- Peak onset: 20s and 30s
- Gender: largely equal overall, though male predominance persists in Arab populations; female predominance in Korea and USA
Pathogenesis
- Genetically determined with probable environmental triggers
- Strongly associated with HLA-B51 (especially in endemic regions)
- Fundamental lesion: neutrophilic vascular reaction / vasculitis
- Lymphocytic perivasculitis is also seen (often in older lesions)
- Autoimmune dysregulation with T-cell and neutrophil hyperactivation
Clinical Features
1. Mucocutaneous (most common, usually first)
| Feature | Details |
|---|---|
| Oral aphthous ulcers | Recurrent, painful; often the presenting sign; minor, major, or herpetiform types |
| Genital ulcers | Scrotum, penis, vulva, cervix; painful; often leave scars (unlike oral ulcers) |
| Papulopustular lesions | Acneiform; on face, neck, chest |
| Erythema nodosum–like lesions | Tender nodules, typically on legs |
| Pseudofolliculitis | Sterile pustules at hair follicles |
2. Ocular
- Uveitis (iridocyclitis / posterior uveitis) — may appear years after oral ulcers
- Risk of blindness if untreated
- Patients may initially report seeing spots
3. Neurological (~20%)
- Aseptic meningitis / meningoencephalitis
- Focal/multifocal neurological deficits — small vessel inflammatory disease; brainstem frequently involved
- Cerebral venous sinus thrombosis
- CSF: mild pleocytosis, elevated protein
- Peripheral neuropathy (rare): polyneuropathy or mononeuropathy multiplex
4. Vascular
- Venous thrombosis (DVT, Budd-Chiari)
- Arterial aneurysms (pulmonary, aorta)
- Pulmonary arterial aneurysm → arterio-bronchial fistula → massive hemoptysis
- Post-anastomotic aneurysms (pathergy phenomenon)
5. Gastrointestinal
- Abdominal pain, GI bleeding, perforation
- Ileocecal ulcers most common (can mimic Crohn disease)
6. Articular
- Non-destructive, asymmetric oligoarthritis of large joints (knees, ankles)
Clinical Images
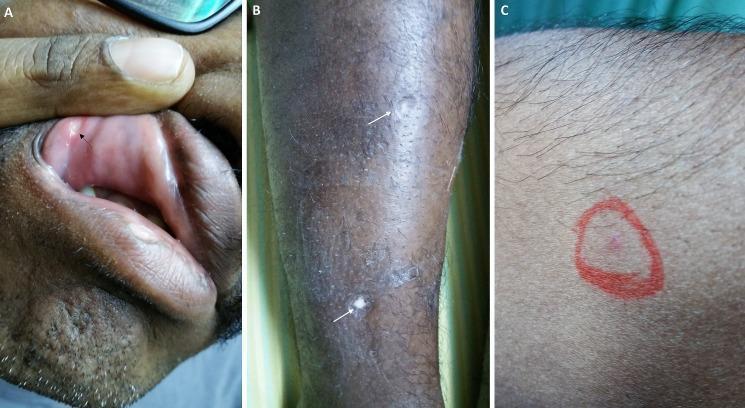
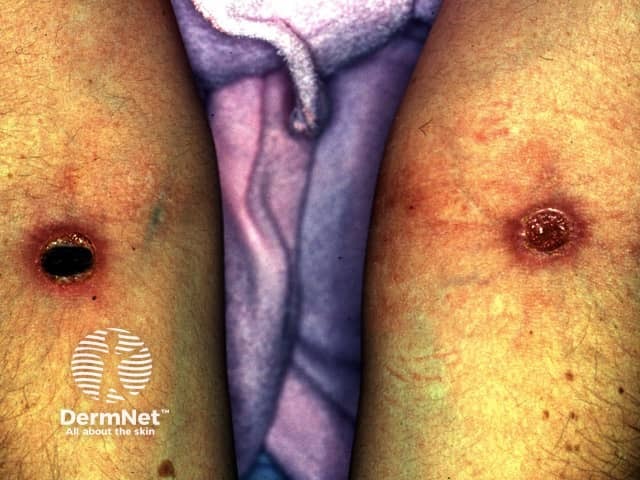
Diagnosis
International Criteria for Behçet Disease (ICBD Scoring System)
| Feature | Points |
|---|---|
| Ocular lesions (recurrent) | 2 |
| Oral aphthosis (recurrent) | 2 |
| Genital aphthosis (recurrent) | 2 |
| Skin lesions (recurrent) | 1 |
| CNS involvement | 1 |
| Vascular manifestations | 1 |
| Positive pathergy test | 1 |
Score ≥4 = Behçet Disease — Fitzpatrick's Dermatology, Table 141-1
Pathergy Test
- Needle prick or 0.1 mL intradermal saline injection on volar forearm
- Positive: erythematous papule/pustule >2 mm within 48 hours
- Not pathognomonic — also seen in pyoderma gangrenosum, Crohn's, rheumatoid arthritis
Other Investigations
- No specific serologic test; HLA-B51 supports diagnosis in appropriate context
- Cranial MRI: hypodense/atrophic brain changes in neuro-Behçet
- Angiography for vascular lesions
- CSF analysis when CNS involvement suspected
Differential Diagnosis
| Category | Conditions |
|---|---|
| Oculocutaneous/mucocutaneous | Stevens-Johnson syndrome, Reiter syndrome, Sweet syndrome, pemphigus |
| GI/systemic | Crohn disease (most important — also has aphthae, uveitis, skin lesions), ulcerative colitis |
| Infectious | HSV, syphilis, HIV |
| Other vasculitides | Systemic lupus, polyarteritis nodosa |
Differentiating from Crohn disease is particularly challenging as both share aphthous ulceration, skin lesions, and uveitis.
Treatment
| Manifestation | Treatment |
|---|---|
| Oral/genital ulcers | Topical corticosteroids, colchicine (first-line for mucocutaneous) |
| Skin lesions | Colchicine, dapsone |
| Uveitis / retinal disease | Systemic glucocorticoids + azathioprine; cyclosporine for refractory cases |
| CNS involvement | Systemic corticosteroids ± azathioprine; anticoagulation for cerebral venous thrombosis |
| Severe systemic disease | Azathioprine, cyclophosphamide, interferon-α, anti-TNF agents (infliximab, adalimumab) |
| Vascular disease | Immunosuppression + anticoagulation; surgical/endovascular for aneurysms |
The primary goal in primary care is early recognition and prompt referral to ophthalmology to prevent irreversible visual loss. — Textbook of Family Medicine, 9e
Prognosis
- Course: chronic, relapsing, progressive
- Worse prognosis in: males, early-onset disease, HLA-B51 positivity, recurrent erythema nodosum, systemic presentations (vascular, CNS)
- Mortality: 0–6% (mainly from vascular complications — pulmonary hemorrhage, CNS disease)
- Mucocutaneous symptoms may improve with age; ocular disease most feared for permanent disability
Sources: Fitzpatrick's Dermatology (Ch. 141), Textbook of Family Medicine 9e, Bradley & Daroff's Neurology in Clinical Practice
This is a shared conversation. Sign in to Orris to start your own chat.