Here is a full clinical analysis of this case:
Clinical Case Analysis
Diagnosis: Mumps (Epidemic Parotitis) complicated by Aseptic (Viral) Meningitis
Clinical Reasoning
Phase 1 — Parotitis (Days 1–4)
| Feature | Significance |
|---|
| Fever 38°C | Systemic viral infection |
| Right parotid swelling → bilateral (day 3) | Classic sequential bilateral parotitis of mumps |
| Pain on chewing | Parotid gland enlargement |
| Pain on tragus pressure, retromandibular fossa tenderness | Parotid gland involvement (the parotid lies anterior to the tragus and fills the retromandibular fossa) |
| Mastoid process tenderness | Referred pain from adjacent parotid swelling |
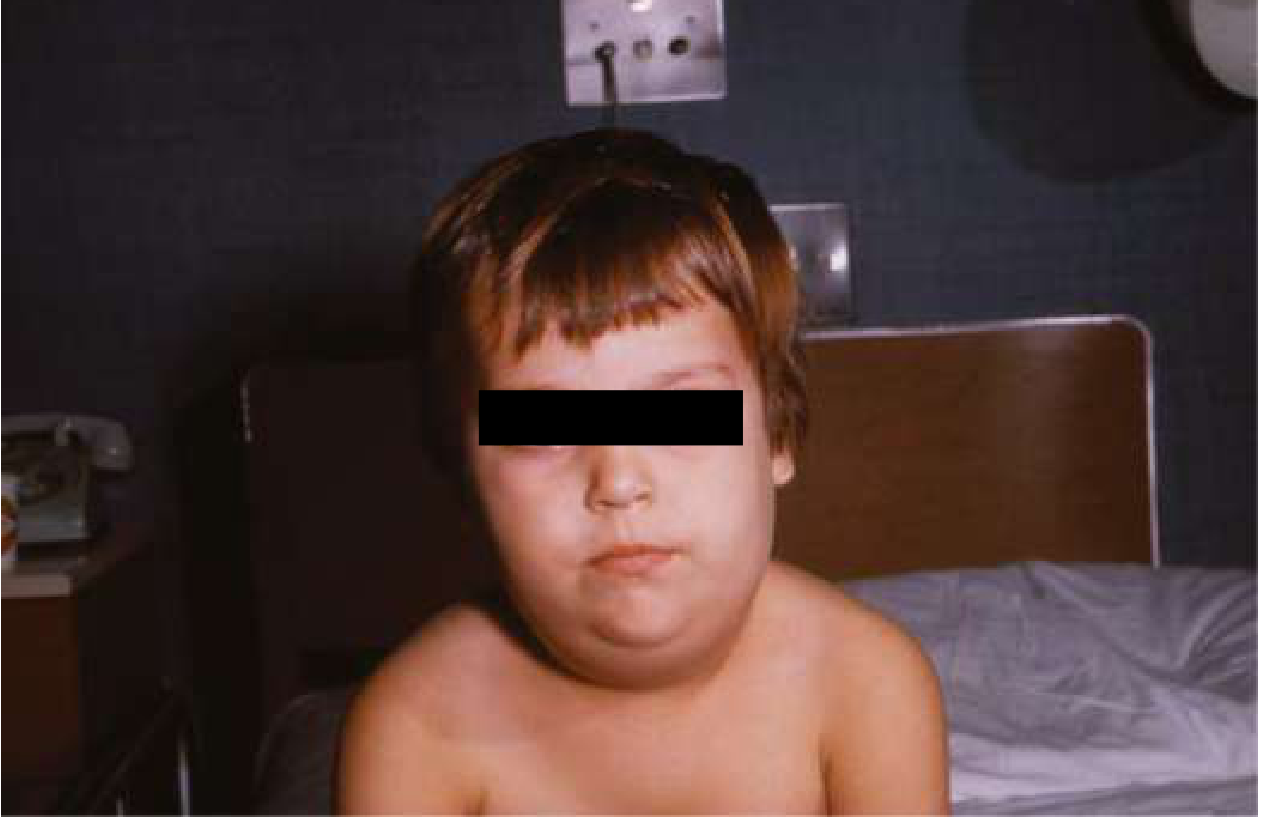
Sequential bilateral parotitis is the hallmark of mumps. The bilateral involvement over 2 days is characteristic.
Bilateral parotid swelling due to mumps parotitis — CDC Public Health Image Library
Phase 2 — Meningeal Complication (Day 5)
| Feature | Significance |
|---|
| Return of fever | Second febrile phase typical of CNS complication |
| Headache + vomiting | Classic meningeal irritation symptoms |
| Nuchal rigidity (2.5 finger-widths) | Meningismus |
| Positive Kernig's sign (bilateral) | Meningeal irritation |
| Positive upper Brudzinski's sign | Meningeal irritation |
| HR 102/min | Tachycardia from fever/pain |
This sequence — parotitis on day 1 → meningeal signs on day 5 — is textbook for mumps meningitis, which typically appears 4–5 days after onset of parotitis in up to 10% of unvaccinated patients.
"In up to 10% of unvaccinated persons with mumps, symptomatic aseptic meningitis can occur and be manifested as headache, neck stiffness, vomiting, and lethargy, usually about 4 to 5 days after onset of parotitis."
— Goldman-Cecil Medicine, p. 3570
CSF Analysis Interpretation
| Parameter | This Patient | Typical Mumps Meningitis |
|---|
| Appearance | Transparent, clear | Clear (viral) |
| Pressure | Flows in frequent drops (↑) | Mildly elevated |
| Total cells | 385 cells/mL | ~400–500 cells/µL |
| Lymphocytes | 353/mL (91%) | Predominantly mononuclear |
| Neutrophils | 52/mL (9%) | May have early PMN predominance |
The CSF profile is classic for aseptic (viral) meningitis: clear fluid, lymphocytic pleocytosis, normal glucose (implied by non-bacterial appearance). Early in mumps meningitis, a mixed neutrophil/lymphocyte picture can occur before it shifts to predominantly lymphocytic.
"CSF examination usually shows about 400 to 500 cells/µL, usually monocellular cells but sometimes polymorphonuclear cells early in the course. The CSF protein may be mildly elevated, and the glucose level is usually normal but can be low."
— Goldman-Cecil Medicine, p. 3570
Blood Count Interpretation
| Value | This Patient | Interpretation |
|---|
| Hb 120 g/L | Normal for age | |
| RBC 4.5×10¹² | Normal | |
| CP (colour index) 0.89 | Normal | |
| WBC 4.0×10⁹/L | Low-normal | Leukopenia — typical of viral infections |
| Band neutrophils 3% | Normal | |
| Segmented neutrophils 37% | Slightly low | Relative lymphocytosis |
| Lymphocytes 60% | Elevated | Lymphocytosis — classic for viral infection (mumps) |
| ESR 7 mm/hr | Normal | Argues against bacterial infection |
Lymphocytosis with leukopenia is the expected peripheral blood picture in mumps. Bacterial meningitis would show leukocytosis with neutrophilia.
Pathophysiology
Mumps virus (a Paramyxovirus) replicates initially in the upper respiratory tract → spreads hematogenously → seeds the parotid glands and CNS. The virus enters the CNS via choroidal and ependymal epithelial cells. This explains the viremic second phase with meningeal involvement after initial parotitis.
Differential Diagnosis (to consider and exclude)
| Condition | Against it |
|---|
| Bacterial meningitis | Clear CSF, lymphocytic pleocytosis, leukopenia, low ESR, no CSF PMN predominance |
| Bacterial parotitis | Typically unilateral, purulent, no meningitis |
| Other viral meningitis (enterovirus, HSV-2) | No parotitis; seasonality and epidemiology differ |
| Lymphadenitis | Swelling not in salivary gland territory |
Diagnostic Confirmation
- Mumps-specific PCR from buccal swab (most sensitive within 8–10 days of parotitis onset; massage parotid 30 sec before swab)
- Mumps IgM serology (may be absent in vaccinated individuals)
- CSF PCR for mumps virus
- Serum amylase/lipase — often elevated in mumps (pancreatic and parotid involvement)
Treatment
There is no specific antiviral therapy for mumps. Management is supportive:
- Antipyretics/analgesics (paracetamol/ibuprofen)
- Adequate hydration
- Bed rest
- Analgesia for parotid pain (cold compresses)
- Monitor for complications: encephalitis, hearing loss, orchitis (if pubertal), pancreatitis
For meningitis: close neurological observation; the prognosis is generally excellent — mumps meningitis is self-limiting and rarely causes permanent sequelae.
Isolation: Droplet precautions for at least 5 days after onset of parotitis.
Prevention (Public Health)
- MMR vaccine (measles-mumps-rubella): 2 doses — first at 12–15 months, second at 4–6 years
- No post-exposure prophylaxis exists; vaccinating contacts after exposure does not prevent disease from the current exposure but protects against future exposures
- Mumps is a nationally notifiable disease — report to public health authorities
Summary
This child presents with mumps (epidemic parotitis) complicated by aseptic viral meningitis, occurring in the classic sequence: bilateral sequential parotitis days 1–3, followed by meningeal syndrome on day 5. The CSF (lymphocytic pleocytosis, clear fluid, ~385 cells/mL) and peripheral blood (lymphocytosis, leukopenia) are entirely consistent. No specific treatment exists; management is supportive with an excellent prognosis.
— Goldman-Cecil Medicine, pp. 3569–3571; Bradley and Daroff's Neurology in Clinical Practice