pcos
Reading File
Asking for Preferences
Finding Sources
Searching PubMed
"polycystic ovary syndrome"[MeSH Terms] AND management
Reading File
Reading File
Reading File
Reading File
Reading File
Loading Image
Here is a comprehensive overview of PCOS:
Polycystic Ovary Syndrome (PCOS)
Definition & Epidemiology
PCOS is the most common endocrine disorder in women of reproductive age, affecting 5–10% of women worldwide. It is also the most common cause of hyperandrogenism (HA), hirsutism, and anovulatory infertility in developed countries. First described by Stein and Leventhal in 1935 (bilateral polycystic ovaries + obesity + amenorrhea), it is now understood as a heterogeneous syndrome with reproductive, metabolic, and cardiovascular consequences. Its genetic basis is likely polygenic and multifactorial.
Pathophysiology
Three interrelated disturbances drive the syndrome:
1. Hypothalamic-Pituitary Dysregulation
- Increased LH pulse frequency and amplitude, leading to a raised LH:FSH ratio (in ~⅔ of patients)
- Excess LH stimulates ovarian theca cells → excess androgen production
- Insufficient FSH → arrested follicular development → anovulation
2. Hyperandrogenism
- Elevated androgens (testosterone, androstenedione, DHEAS) arise from both the ovaries and adrenal glands
- Androgens are converted peripherally (especially in adipose tissue) to estrogens, which exerts positive feedback on LH — creating a self-perpetuating cycle
- Skin 5α-reductase converts testosterone → DHT, causing hirsutism and acne (activity varies by ethnicity, explaining why hirsutism appears in ~70% of US patients vs. only 10–20% in Japan)
3. Insulin Resistance & Hyperinsulinemia
- Present in the majority, independent of obesity
- Hyperinsulinemia directly stimulates ovarian androgen production and suppresses sex hormone-binding globulin (SHBG), increasing free androgen levels
- PCOS typically arises at puberty; obesity worsens the phenotype by amplifying hyperinsulinemia
Clinical Features
| Domain | Features |
|---|---|
| Menstrual | Oligomenorrhea, amenorrhea (rarely primary); irregular cycles from menarche |
| Androgen excess | Hirsutism (~70%), acne, male-pattern alopecia |
| Metabolic | Obesity (>50%, android/central distribution), insulin resistance, dyslipidemia |
| Ovarian | Polycystic ovary morphology on ultrasound |
| Reproductive | Anovulatory infertility, increased miscarriage risk |
| Psychological | Depression, anxiety (screen at diagnosis) |
Diagnosis
PCOS is a diagnosis of exclusion. The 2003 Rotterdam Criteria (most widely used) require 2 of 3:
- Oligo-ovulation or anovulation
- Clinical and/or biochemical hyperandrogenism (hirsutism, acne, alopecia; or elevated free testosterone)
- Polycystic ovarian morphology on ultrasound — ≥20 follicles (2–9 mm) in either ovary and/or ovarian volume >10 mL
In adolescents, diagnosis requires both persistent anovulation and clinical/biochemical HA (PCO morphology alone is insufficient).
Differential Diagnoses to Exclude:
- Non-classic congenital adrenal hyperplasia → 17-OHP (follicular phase) to screen
- Cushing syndrome → 24-hr urinary cortisol / overnight dexamethasone suppression
- Hyperprolactinemia → serum prolactin
- Androgen-secreting neoplasm → imaging if testosterone very high
- Thyroid disease → TSH
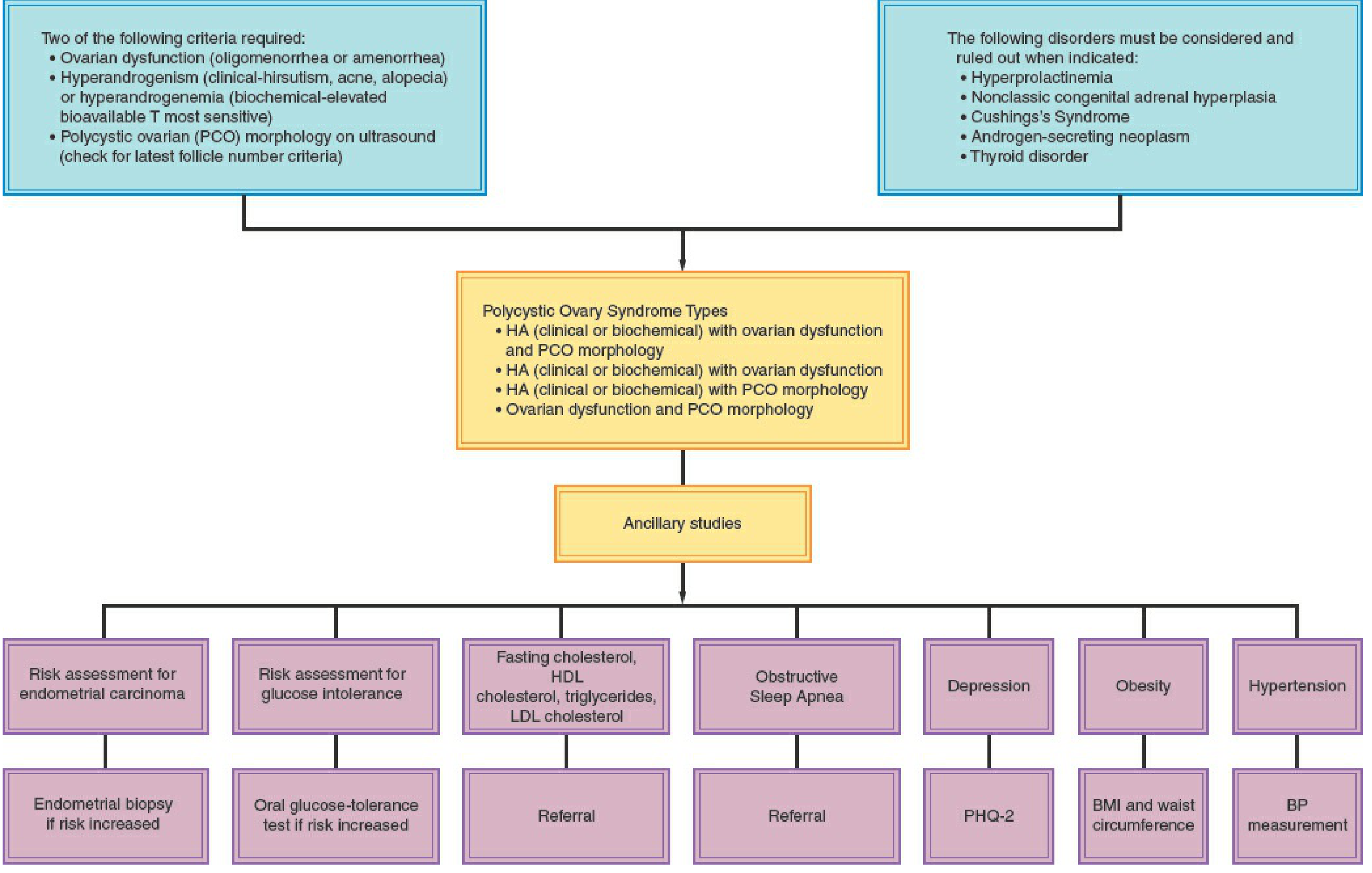
Ancillary Workup at Diagnosis:
- Fasting glucose / oral GTT (screen for impaired glucose tolerance/T2DM)
- Fasting lipid profile (overweight/obese women)
- BMI, waist circumference, blood pressure
- PHQ-2 (depression screen)
- Consider endometrial biopsy if prolonged anovulation (endometrial hyperplasia risk)
Management
Treatment is tailored to the patient's primary concern (menstrual irregularity, hyperandrogenism, infertility, or metabolic risk).
All Patients — Universal
- Lifestyle modification (diet + exercise): first-line for all women; even modest weight loss (5–10%) improves menstrual regularity, hyperandrogenism, and insulin sensitivity
- Screen and monitor: obesity, hypertension, glycemic control, depression, anxiety — at diagnosis and at regular intervals
Women Not Seeking Pregnancy
| Goal | Therapy |
|---|---|
| Menstrual regulation + androgen control | Combined oral contraceptive pill (COCP) — first-line; increases SHBG, suppresses LH/androgens |
| Inadequate response to COCP after 6 months | Add antiandrogens: spironolactone, flutamide |
| Endometrial protection (if OCP not used) | Cyclic progestin (MPA 10 mg or progesterone 200 mg × 10–14 days every ≥3 months) or levonorgestrel IUD |
| Cardiometabolic risk reduction | Metformin — especially for overweight/obese women |
Women Seeking Pregnancy (Ovulation Induction)
- Letrozole (aromatase inhibitor) — first-line for ovulation induction in PCOS
- Clomiphene citrate ± metformin — second-line
- Injectable gonadotropins — used judiciously (risk of ovarian hyperstimulation syndrome is higher in PCOS)
- Metformin — adjunct with diet/exercise in obese women; alone is not recommended for infertility treatment
Metformin is not recommended as monotherapy for endometrial protection, treatment of hyperandrogenic symptoms, prevention of pregnancy loss, or prevention of gestational diabetes.
Complications & Long-term Risks
Reproductive
- Anovulatory infertility — most common endocrine cause
- Increased risk of early miscarriage, gestational diabetes, gestational hypertension, preeclampsia, preterm birth
- Prepregnancy counseling and lifestyle management recommended before conception
Metabolic / Cardiovascular
- Type 2 diabetes and impaired glucose tolerance — screen with oral GTT
- Dyslipidemia (elevated LDL, triglycerides; low HDL) → increased long-term cardiovascular disease risk
- Obstructive sleep apnea — increased prevalence, refer if suspected
- Non-alcoholic fatty liver disease
Oncological
- Endometrial carcinoma — chronic anovulation leads to unopposed estrogen stimulation; endometrial biopsy if at increased risk
Psychiatric
- Higher rates of depression and anxiety — screen at diagnosis and regularly
Recent Evidence (2024–2025)
- Inositol (myo-inositol + D-chiro-inositol) was evaluated in a 2024 meta-analysis for the 2023 updated PCOS guidelines — modest evidence for improving metabolic and reproductive outcomes (PMID: 38163998)
- Lifestyle interventions remain foundational: a 2025 systematic review confirmed significant improvements in insulin resistance, androgen levels, and menstrual regularity with structured exercise and diet (PMID: 39861440)
- Pregnancy outcomes: A 2024 meta-analysis in Nature Communications quantified increased risks of gestational diabetes, preeclampsia, and preterm birth, reinforcing preconception counseling (PMID: 38965226)
Sources: Berek & Novak's Gynecology; Harrison's Principles of Internal Medicine, 22e; Goldman-Cecil Medicine
This is a shared conversation. Sign in to Orris to start your own chat.