Why oral cancer by tobacco leads to death
Reading File
Finding Sources
Finding Sources
Searching PubMed
"oral cancer" AND tobacco AND mortality
Reading File
Reading File
Reading File
Reading File
Finding Sources
Finding Sources
Loading Image
Finding Sources
Finding Sources
I now have comprehensive information from multiple textbooks to give a thorough answer. Let me compile this.
How Tobacco-Related Oral Cancer Leads to Death
Oral cancer is predominantly oral squamous cell carcinoma (OSCC) — over 90–95% of all oral malignancies — and tobacco is one of its primary causes. Here's the full chain from exposure to death:
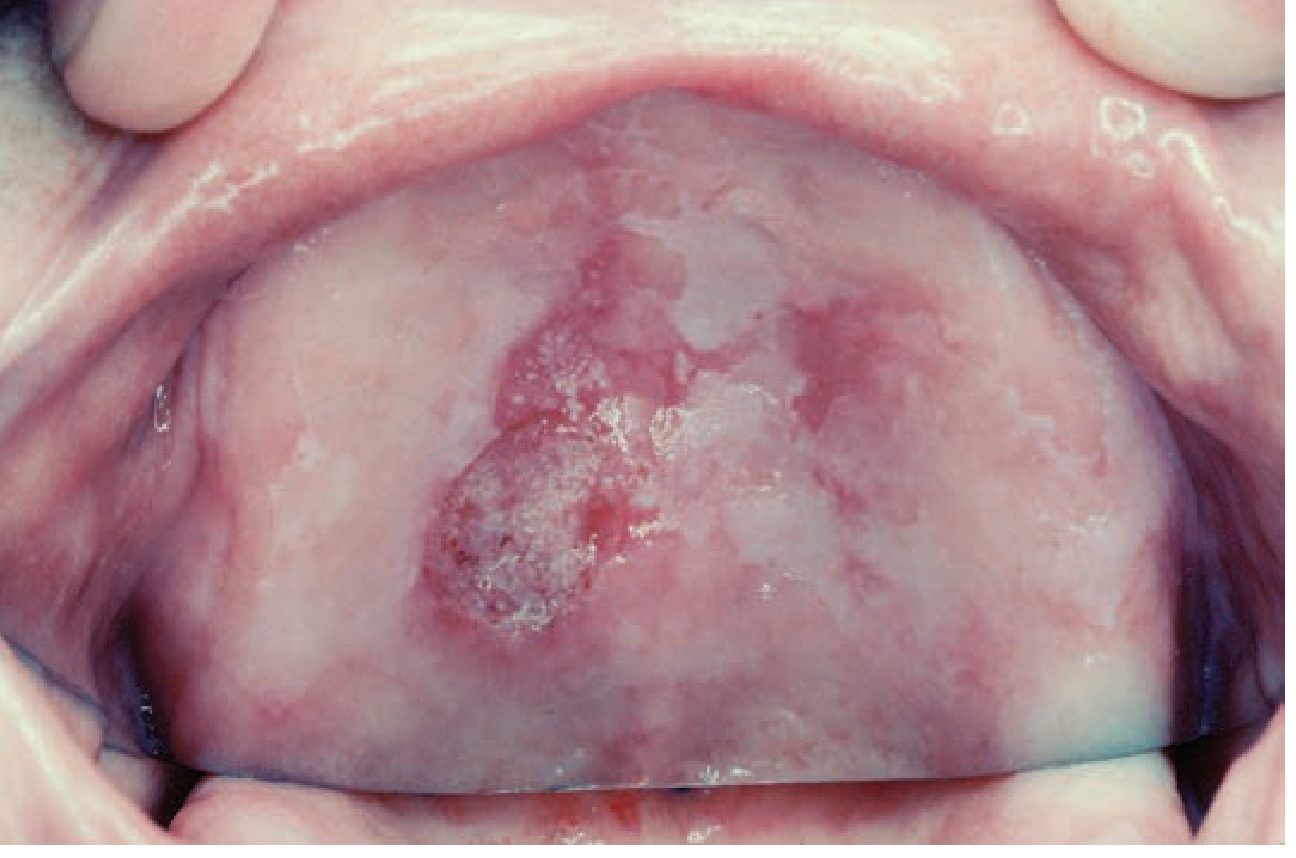
1. How Tobacco Causes Oral Cancer
Carcinogens in Tobacco
Tobacco (smoked and smokeless) contains potent chemical carcinogens:
- N-nitrosonornicotine (NNN) and 4-methylnitrosamino-1-(3-pyridyl)-1-butanone (NNK) — tobacco-specific nitrosamines found especially in smokeless tobacco (chewing tobacco, snuff). These are directly implicated in oral tumor induction in animal models and in humans.
- Polycyclic aromatic hydrocarbons (PAHs) from combustion in smoked tobacco.
These chemicals bind to DNA, forming DNA adducts (permanent mutations), particularly affecting tumor suppressor genes (e.g., p53) and cell cycle regulators (e.g., INK4 family). Smokeless tobacco users have a fourfold increased risk of oral cavity carcinoma compared to non-users.
Synergy with Alcohol
When tobacco is combined with alcohol, the risk increases synergistically by 45 times — far more than either substance alone. Alcohol acts as a solvent that enhances mucosal penetration of tobacco carcinogens.
Premalignant Progression
Chronic tobacco exposure produces a stepwise transformation:
- Leukoplakia (white patches) → risk of malignant transformation ~2–3% per year
- Erythroplakia (red patches) → 5–7× higher malignant risk than leukoplakia
- Dysplasia → Carcinoma in situ → Invasive OSCC
2. Why the Cancer Goes Undetected Until Advanced
"Oral cancer is generally painless, and patients are often unaware of the presence of a mass until it is advanced." — Tintinalli's Emergency Medicine
Because early lesions are painless, patients often present with locally advanced or metastatic disease, which dramatically worsens prognosis. By this stage, the tumor has already invaded deep tissues.
3. How Advanced Oral Cancer Kills — Mechanisms of Death
A. Local Invasion and Structural Destruction
OSCC invades deeply into adjacent structures:
- Floor of mouth and tongue (most common sites — 50% tongue, 35% floor of mouth): invasion destroys muscles of swallowing and speech
- Mandible and maxilla: tumor erodes bone, requiring segmental mandibulectomy or partial maxillectomy
- Depth of invasion is a key independent prognostic factor — deeper invasion = higher mortality
- As the tumor destroys the airway anatomy, patients develop dysphagia (inability to swallow), leading to malnutrition, aspiration, and respiratory compromise
B. Regional Lymph Node Metastasis (Cervical Spread)
OSCC spreads predictably through cervical lymphatics:
- Tongue/floor of mouth → levels IA, IB, II lymph nodes
- Extranodal extension (tumor breaking through lymph node capsule) is a particularly lethal finding — directly worsens survival and is now a separate staging criterion in AJCC 8th edition
Once nodal disease is extensive or involves bilateral nodes, surgical cure becomes very difficult or impossible.
C. Distant Metastasis
When oral cancer spreads beyond the head and neck:
- Lungs — by far the most common distant site (hematogenous spread)
- Liver
- Bone
Pulmonary metastases cause progressive respiratory failure. Once distant metastases are present (Stage IVb/IVc), disease is rarely curable.
D. Starvation and Cachexia
- Tumors of the oral cavity directly prevent eating and swallowing
- Progressive weight loss and cancer cachexia (systemic wasting syndrome) from both the tumor's metabolic demands and treatment toxicity weakens the patient
- Inability to maintain adequate nutrition leads to immune failure and organ dysfunction
E. Hemorrhage
- Oral tumors are highly vascular and prone to bleeding from ulceration
- Invasion of major neck vessels (carotid artery) can cause catastrophic, fatal hemorrhage
F. Airway Obstruction
- Large tumors of the tongue base and floor of mouth can physically obstruct the oropharyngeal airway
- Infiltration into the larynx or trachea leads to asphyxiation if untreated
G. Sepsis
- Oral tumors are chronically infected, given the bacterial environment of the mouth
- Tumor necrosis, poor oral hygiene, and aspiration pneumonia (from dysphagia) can lead to systemic sepsis
H. Treatment Complications
Even when treatment is attempted:
- High-dose radiotherapy causes osteoradionecrosis (bone death), xerostomia, and severe dysphagia
- Major surgical resections carry significant perioperative risk
- Chemotherapy-related toxicity can be fatal in already-debilitated patients
4. Survival Statistics
| Stage | 5-Year Disease-Specific Survival |
|---|---|
| Stage I–III | ~90% |
| Stage IVa | ~75% |
| Stage IVb | ~50% |
| Overall (historical) | 59% (1990) → 70% (2011) — improved but still poor for late-stage |
- Locoregional disease-free survival for T2-T4 OSCC: ~60%
- Overall disease-free survival (including distant metastases): ~50%
The reason survival remains poor compared to many other cancers is the late stage at diagnosis, driven by the painless early course of the disease.
Summary
Tobacco kills through oral cancer via this chain:
Tobacco carcinogens (nitrosamines, PAHs) → DNA mutations in oral mucosa → squamous cell carcinoma → silent growth until advanced → local destruction of airway/swallowing/bone → lymph node spread → distant metastasis (lung/liver/bone) → cachexia, hemorrhage, airway obstruction, sepsis, organ failure → death
Early detection remains the single most important factor in survival. Any oral ulcer or white/red patch not resolving within 10–14 days in a tobacco user warrants urgent biopsy.
Sources: Sabiston Textbook of Surgery (19th ed.), Tintinalli's Emergency Medicine, Cummings Otolaryngology Head and Neck Surgery
This is a shared conversation. Sign in to Orris to start your own chat.