Questions to ask pt who admitted for total knee replacement
Reading File
Checking Date & Time
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Based on the textbook content and comprehensive clinical knowledge for TKA admission assessment, here is a thorough question guide organized by domain:
Pre-Admission Assessment Questions: Total Knee Replacement (TKA)
1. Reason for Surgery / Knee History
- Which knee is being replaced? (laterality confirmation)
- How long have you had knee pain/arthritis?
- What makes the pain worse — walking, stairs, rest, at night?
- Rate your pain on a scale of 0–10.
- What non-surgical treatments have you tried? (PT, injections, bracing, medications)
- Have you had any prior knee surgeries on this knee?
- Do you use any assistive devices (cane, walker, brace)?
- How far can you walk before stopping due to pain?
2. Medical History / Comorbidities
- Do you have diabetes? If so, how well is it controlled? (last HbA1c)
- Do you have hypertension, heart disease, or heart failure?
- Any history of blood clots (DVT or pulmonary embolism)?
- Do you have kidney disease, liver disease, or COPD/asthma?
- Any history of stroke or TIA?
- Do you have obesity? (BMI is a key risk factor for complications)
- Any history of anemia or bleeding disorders?
- Any autoimmune or inflammatory conditions (RA, lupus)?
- Do you have any active infections anywhere in your body?
3. Medications
- What prescription medications are you currently taking?
- Do you take blood thinners? (warfarin, rivaroxaban, aspirin, clopidogrel — ask about last dose)
- Do you take NSAIDs regularly? (when did you last take them?)
- Are you on steroids or immunosuppressants?
- Do you take any diabetes medications or insulin?
- Any herbal supplements or over-the-counter medications?
- Have you been told to hold any medications before surgery?
4. Allergies
- Do you have any drug allergies? (especially antibiotics — cefazolin is standard prophylaxis)
- Any allergy to latex, iodine, or contrast dye?
- Any prior reactions to anesthesia?
5. Anesthesia & Surgical History
- Have you had surgery or anesthesia before?
- Any complications with past anesthesia? (nausea/vomiting, difficult airway, malignant hyperthermia family history)
- Do you have a personal or family history of problems with anesthesia?
- Have you had any prior joint replacements? Any complications?
6. Cardiovascular / Respiratory Assessment
- Any chest pain, shortness of breath, or palpitations?
- Can you climb a flight of stairs or walk on level ground without stopping?
- Do you get short of breath lying flat? (orthopnea)
- Do you snore heavily or have sleep apnea? Do you use a CPAP?
- Any recent cardiac workup or stress tests?
7. VTE Risk Assessment
- Any personal or family history of DVT or PE?
- Are you currently on anticoagulation?
- Are you on hormonal contraceptives or HRT?
- Are you a smoker?
TKA carries high VTE risk — this informs thromboprophylaxis choice postoperatively. — Morgan and Mikhail's Clinical Anesthesiology, 7e
8. Nutritional & Metabolic Status
- Have you lost weight recently without trying?
- Do you have a good appetite?
- Any difficulty swallowing?
- Do you drink alcohol? How much? How often?
- Do you smoke? How many pack-years?
- Do you use recreational drugs?
9. Functional / Social History
- Who will be caring for you at home after discharge?
- Do you live in a house with stairs? Can you manage them?
- Do you have a shower/tub setup that's safe for post-op?
- Have you arranged for home PT or rehab?
- What is your occupation and activity goals after surgery?
10. Preoperative Instructions Compliance
- Have you been NPO (nothing by mouth) since midnight / per instructions?
- Did you shower with chlorhexidine soap before admission?
- Did you complete preoperative blood work and imaging (X-rays)?
- Have you signed informed consent?
- Do you understand what to expect from the surgery and recovery?
11. Mental Health / Expectations
- Do you have a realistic expectation of recovery time and outcomes?
- Any history of anxiety, depression, or chronic pain conditions?
- Are you on any psychiatric medications?
- Do you have concerns about the surgery you'd like to discuss?
Key Clinical Notes
- Pain control: TKA produces more severe and longer-lasting pain than THA; multimodal analgesia and nerve blocks are key. — Morgan and Mikhail's Clinical Anesthesiology, 7e
- Anesthesia preference: Neuraxial (spinal/epidural) anesthesia is preferred over general anesthesia for TKA due to lower rates of infection, AKI, PE, and falls.
- Blood conservation: Ask about autologous donation or tranexamic acid use — standard protocol to reduce surgical bleeding.
- Active infection: Any active infection (even dental/skin) is a contraindication to proceeding with implant surgery.
Physical and specific examinations for the knee
Checking Date & Time
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Finding Sources
Reading File
Finding Sources
Finding Sources
Finding Sources
Searching Images
knee physical examination special tests Lachman McMurray valgus varus
Here is a comprehensive guide to the physical and specific examination of the knee, structured in the standard clinical sequence.
Physical Examination of the Knee
1. GENERAL INSPECTION (Patient Standing & Walking)
Standing
- Alignment: Look for varus (bow-legged) or valgus (knock-kneed) deformity — both are common findings in OA patients heading for TKA
- Limb length discrepancy
- Muscle wasting: Quadriceps atrophy (especially VMO)
- Skin changes: Scars from previous surgeries, erythema, sinuses
Gait Analysis
- Antalgic gait (shortened stance phase on affected side)
- Vaulting or circumduction suggesting stiffness
- Thrust: Varus/valgus thrust during weight-bearing
2. INSPECTION (Patient Supine on Bed)
- Swelling: Diffuse (effusion) vs. localized (bursitis)
- Deformity: Fixed flexion contracture, hyperextension
- Skin: Bruising, erythema, sinuses, scars
- Muscle bulk: Quadriceps wasting compared bilaterally
3. PALPATION
Temperature & Skin
- Increased warmth suggests inflammation or infection
- Compare with the contralateral knee
Effusion Tests
| Test | Technique | Positive Finding |
|---|---|---|
| Bulge (Stroke) Sign | Small effusion test — stroke fluid from medial to suprapatellar pouch, then tap lateral side; watch for medial bulge | Medial bulge returns = small effusion |
| Patellar Tap (Ballottement) | Compress suprapatellar pouch downward, tap patella sharply | Palpable tap/bounce = moderate–large effusion |
| Cross-Fluctuation | Compress one side of the joint and feel fluctuation on the other side | Large effusion |
Specific Tenderness Points
- Medial joint line → OA, medial meniscus tear, MCL injury
- Lateral joint line → OA, lateral meniscus, LCL injury
- Medial femoral condyle → OA, avascular necrosis
- Tibial tubercle → Osgood-Schlatter (young patients), patellar tendon insertion
- Patella margins → Patellofemoral OA
- Pes anserine bursa (anteromedial proximal tibia) → Bursitis, common in OA
- Popliteal fossa → Baker's cyst, DVT, popliteal aneurysm
4. RANGE OF MOTION (ROM)
| Movement | Normal | Note |
|---|---|---|
| Flexion (active & passive) | 0–135° | OA often limits to 90–110° |
| Extension | 0° (or up to 5–10° hyperextension) | Fixed flexion contracture is common in severe OA |
| Fixed Flexion Contracture | None | Measure the deficit with goniometer |
- Crepitus: Feel for during ROM — coarse crepitus suggests significant cartilage loss
- Pain arc: Note at which point in ROM pain is provoked
5. NEUROVASCULAR ASSESSMENT
- Distal pulses: Popliteal, posterior tibial, dorsalis pedis (critical pre-TKA)
- Capillary refill of toes
- Sensation: Light touch L3–S1 dermatomes
- Motor: Quadriceps (L3–L4), hamstrings (L5–S1), tibialis anterior (L4–L5)
6. SPECIFIC LIGAMENT TESTS
Anterior Cruciate Ligament (ACL)
Lachman Test (most accurate — high sensitivity & specificity)
- Patient supine, knee at 20–30° flexion
- Stabilize femur with one hand; pull tibia anteriorly with the other
- Positive: Increased anterior tibial translation or soft end-point
- Graded: 1+ (0–5 mm), 2+ (5–10 mm), 3+ (>10 mm)
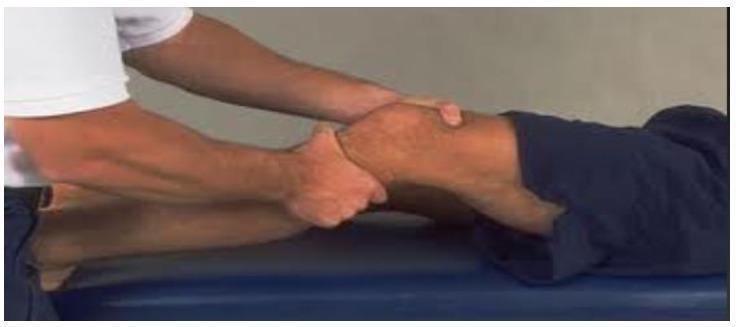
Anterior Drawer Test
- Hip at 45°, knee at 90° flexion, foot stabilized
- Pull tibia forward; compare with opposite knee
- Positive: Anterior translation > contralateral side
- Less sensitive than Lachman
Posterior Cruciate Ligament (PCL)
Posterior Drawer Test
- Knee at 90° flexion, foot stabilized
- Push tibia posteriorly with smooth backward force
- Positive: >5 mm posterior displacement or soft end-point
Posterior Sag Sign
- Hips and knees both flexed to 90° while supine
- Positive: Tibia visibly sags backwards relative to femur → PCL insufficiency
Collateral Ligaments
Valgus & Varus Stress Tests
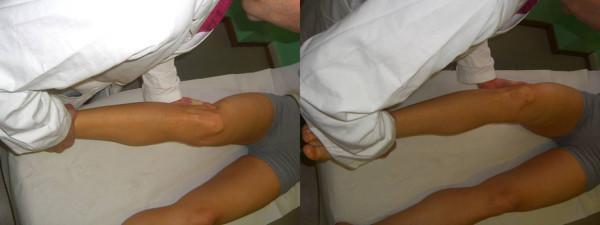
- Test at both 0° and 30° flexion
- Valgus stress (medial force) → tests MCL
- Varus stress (lateral force) → tests LCL
- At 30° flexion: isolated collateral injury
- Laxity in full extension = combined cruciate + collateral injury
Grading:
- Grade I: Pain, no laxity
- Grade II: Pain + marked laxity, firm end-point
- Grade III: Complete laxity, no end-point
— Rosen's Emergency Medicine, 10e
7. MENISCAL TESTS
McMurray Test (most commonly used)
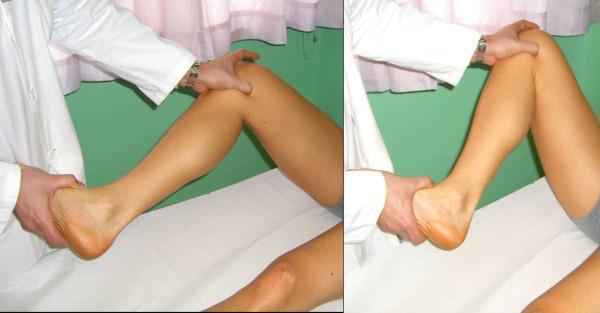
- Patient supine, knee hyperflexed
- Examiner: one hand on foot, one hand on knee palpating joint line
- Flex/extend knee while simultaneously rotating tibia internally (lateral meniscus) and externally (medial meniscus) + apply varus/valgus stress
- Positive: Palpable/audible click along the joint line, pain, or locking
— Rosen's Emergency Medicine, 10e
Apley Grind Test
- Patient prone, knee at 90° flexion
- Apply downward compression + internal/external rotation
- Positive: Pain with compression = meniscal pathology
- Compare: pain relieved with distraction = meniscal (not ligament) origin
- Relatively specific but not sensitive
Thessaly Test (more recent, functional)
- Patient stands on affected leg, knee at 20° flexion
- Rotates body medially and laterally three times
- Positive: Medial or lateral joint line pain, or sense of locking
8. PATELLOFEMORAL TESTS
| Test | Technique | Positive Finding |
|---|---|---|
| Patellar Grind / Clarke's Test | Press patella distally, ask patient to contract quads | Pain = patellofemoral OA/chondromalacia |
| Patellar Apprehension Test | Push patella laterally with knee slightly flexed | Apprehension/quad contraction = patellar instability |
| J-Sign | Observe patellar tracking during active knee extension | Patella deviates laterally in terminal extension = maltracking |
9. EXTENSOR MECHANISM
- Straight Leg Raise: If unable to actively lift leg with extended knee → extensor mechanism disruption (quad tendon, patellar, patellar tendon rupture)
- Palpate: Quad tendon, patella, patellar tendon for gaps/defects
10. HIP EXAMINATION (Never Forget)
Hip pathology commonly refers pain to the knee. Always assess:
- Hip ROM (especially internal rotation)
- FABER / FADIR tests to screen for hip joint pathology
- Thomas test for hip flexor contracture
Summary Table: Key Special Tests
| Test | Structure Tested | Position | Positive Sign |
|---|---|---|---|
| Lachman | ACL | 20–30° flexion | Soft end-point, anterior translation |
| Anterior Drawer | ACL | 90° flexion | Anterior tibial translation |
| Posterior Drawer | PCL | 90° flexion | Posterior tibial displacement >5 mm |
| Posterior Sag | PCL | 90° hip & knee flexion | Tibia sags posteriorly |
| Valgus Stress | MCL | 0° & 30° flexion | Medial joint opening |
| Varus Stress | LCL | 0° & 30° flexion | Lateral joint opening |
| McMurray | Menisci | Hyperflexed → extended | Click/pain at joint line |
| Apley Grind | Menisci | Prone, 90° flexion | Pain with compression |
| Clarke's/Grind | Patellofemoral | Supine | Pain with quad contraction |
| Patellar Tap | Effusion | Supine | Ballotteable patella |
| Bulge Sign | Effusion (small) | Supine | Medial fluid wave |
This is a shared conversation. Sign in to Orris to start your own chat.