Varicose vein in surgery in detail
Reading File
Finding Sources
Searching PubMed
"varicose veins"[MeSH Terms] AND "surgical treatment"[MeSH Terms]
Finding Sources
Searching PubMed
"varicose veins" AND surgery
Reading File
Reading File
Reading File
Reading File
Reading File
Searching Images
varicose vein surgery stripping endovenous ablation
Loading Image
Loading Image
Reading File
Reading File
Reading File
I now have thorough, detailed content from multiple authoritative surgical textbooks. Let me compile the comprehensive answer:
Varicose Veins — Surgical Perspective
1. Definition & Epidemiology
Varicose veins are dilated, tortuous, elongated superficial veins resulting from venous wall incompetence and valvular dysfunction. By age 65, prevalence in Western populations exceeds 55% (Edinburgh Vein Study). They are present in at least 10% of the general population. More time is lost from work due to vein-related pathology than from all arterial diseases combined, including coronary artery disease.
Risk factors: Female sex, family history, obesity, prolonged standing/inactivity, occupation.
2. Anatomy & Pathophysiology
The lower extremity venous system has three components:
- Deep veins (enclosed in muscle fascia, driven by the calf pump)
- Superficial veins (great saphenous vein [GSV], small saphenous vein [SSV], and accessory systems)
- Perforators (connect superficial to deep, contain valves preventing backflow)
Normal Physiology
Calf muscle contraction generates up to 300 cm H₂O pressure, forcing blood proximally through competent valves. During relaxation, blood refills the superficial system via perforators. The superficial system functions as an "atrium" and the deep veins as a "ventricle."
Pathological Mechanism
When vein walls dilate, valve leaflets lose coaptation → valvular incompetence → blood refluxes distally under gravity → ambulatory venous pressure (AVP) rises. Skin manifestations are uncommon when AVP <35 mmHg but are almost certain when AVP >90 mmHg.
Primary varicose veins arise from intrinsic venous wall abnormalities.
Secondary varicose veins follow deep vein thrombosis, compression syndromes (May-Thurner, Nutcracker), or congenital conditions (Klippel-Trenaunay, Ehlers-Danlos, clonal trisomies).
3. Clinical Features
| Feature | Detail |
|---|---|
| Dilated/tortuous veins | Visible, palpable superficial vessels |
| Aching, heaviness, pruritus | Worse with prolonged standing, relieved by leg elevation |
| Edema | Mild ankle/leg swelling |
| Thrombophlebitis | Painful red cord |
| Hyperpigmentation | Hemosiderin deposition |
| Lipodermatosclerosis | Fibrosis/induration of lower leg skin |
| Venous ulceration | Typically medial gaiter area (C6) |
| Bleeding | From attenuated vein clusters |
4. Classification — CEAP System (Revised 2020)
The Clinical-Etiology-Anatomy-Pathophysiology (CEAP) classification (introduced 1994, revised 2004, updated 2020) is the global standard:
| Class | Description |
|---|---|
| C0 | No visible or palpable signs |
| C1 | Telangiectasias or reticular veins |
| C2 | Varicose veins |
| C2r | Recurrent varicose veins |
| C3 | Edema |
| C4a | Pigmentation or eczema |
| C4b | Lipodermatosclerosis or atrophie blanche |
| C4c | Corona phlebectatica |
| C5 | Healed venous ulcer |
| C6 | Active venous ulcer |
The revised Venous Clinical Severity Score (r-VCSS) supplements CEAP for outcomes assessment. The Aberdeen Varicose Vein Score is a validated QoL instrument.
5. Diagnosis
Duplex Ultrasonography
The cornerstone of evaluation. Protocol-driven scanning performed with the patient standing or in steep reverse Trendelenburg. Key assessments:
- Pathological reflux: Reversal of flow >500 ms in superficial truncal veins, >500 ms in perforators, >1000 ms in deep veins
- Vein diameter: >5 mm in saphenous trunks (>3.5 mm in perforators) correlates with symptomatic reflux
- Identify the most proximal (central) source of reflux before any intervention
- Crucially: failure to recognize deep vein compromise before superficial ablation "can be a catastrophic mistake"
6. Non-Surgical (Conservative) Management
- Elastic compression stockings: 20–30, 30–40, or 40–50 mmHg; knee-high to waist-high; must cover the varices — sufficient for many symptomatic patients
- Leg elevation above heart level
- Weight loss, activity improvement
- Management of deep reflux (if present): External compression (20–30 mmHg), elevation, activities that enhance the calf muscle pump
7. Interventional & Surgical Management
Indications for Intervention
- Symptoms worsening or unrelieved despite compression therapy
- Lipodermatosclerosis
- Venous ulcer (C5/C6)
- Thrombophlebitis
- Cosmetic concern with documented reflux
Overview of Techniques
All techniques share one fundamental principle: eliminate the source of symptomatic venous hypertension by functionally removing the refluxing segment. Treatment proceeds from most central to most peripheral — truncal veins first (GSV, SSV), then accessory systems, then branch varicosities.
A. Injection Sclerotherapy
Sclerosants destroy the venous endothelium, provoking fibrosis and obliteration. Used for telangiectasias, reticular veins, and smaller varicosities.
Sclerosing agents (FDA-approved in US):
| Agent | Concentration for Telangiectasias | Concentration for Larger Varices | Notes |
|---|---|---|---|
| Sodium tetradecyl sulfate (STS/Sotradecol) | 0.125–0.25% | 0.5–1% | Painless; can cause extravascular necrosis |
| Hypertonic saline | 11.7% | 23.4% | No anaphylaxis, inexpensive; some injection discomfort |
| Polidocanol (Aethoxysklorol) | 0.25–1% | 0.75–1% | Painless; less extravascular necrosis |
Technique:
- Inject sclerosant directly into the vein
- Wrap elastic bandages continuously for 3–5 days (appose inflamed walls, prevent thrombus)
- Wear compression stockings ≥2 weeks after bandage removal
Complications: Allergic reaction, local hyperpigmentation, superficial thrombophlebitis, DVT, skin necrosis
Foam sclerotherapy: Sclerosant mixed with air/gas to form foam; increases surface contact with endothelium. A multicenter RCT demonstrated significant symptom relief and improved cosmetic appearance vs. placebo.
Ultrasound-guided foam sclerotherapy (UGFS): Allows treatment of truncal veins under real-time ultrasound visualization; effective but lower long-term QoL and higher recurrence vs. thermal ablation or surgery for GSV/SSV.
B. Endovenous Thermal Ablation
i. Radiofrequency Ablation (RFA)
Introduced in 2003. Radiofrequency energy delivered through catheter tip causes endothelial and collagen damage → lumen closure → in situ vein wall degeneration.
Catheter systems: ClosureFast (Medtronic) — 3-cm and 7-cm thermal tip lengths; dedicated stylet for perforator veins.
Step-by-step technique (GSV/SSV):
- Sterile prep of the leg
- Duplex scan: map saphenous system, assess for occlusion, aneurysm, superficial location, webbing
- Percutaneous ultrasound-guided access below popliteal fossa (medial calf for GSV; mid-to-lower calf for SSV)
- Thread microwire, place 7Fr introducer sheath
- Advance RFA catheter to 2–2.5 cm below the epigastric vein, distal to the saphenofemoral junction (SFJ); for SSV, stop 3 cm from the saphenopopliteal junction (SPJ)
- Tumescent anesthesia perivenously: 1000 mg 1% lidocaine + 20 cc 8.4% NaHCO₃ in 1000 cc NS; creates halo in saphenous fascia extending ≥2 cm proximal to catheter tip (anesthesia + thermal barrier protecting deep structures)
- Trendelenburg position to collapse vein
- Apply compression over heating element; treat segment
- Each 7-cm segment treated sequentially as catheter is withdrawn (index to shaft marks); segment at junction treated twice (three times if vein >10 mm)
- Apply compression foot to thigh; review postprocedure instructions
Key safety point: If wattage does not fall below 14W during a cycle, increase compression or reassess catheter tip position; if patient has pain, stop immediately and inject more tumescence.
ii. Endovenous Laser Ablation (EVLA)
Introduced by Carlos Boné in 1999. Thermal energy delivered via laser fiber causes endothelial destruction and vein wall contraction.
Wavelengths: 810 nm and 1470 nm diode lasers
- 1470 nm: 40 J/cm energy delivery
- 810 nm: 80 J/cm energy delivery
Technique (key differences from RFA):
- Access and tumescent anesthesia identical to RFA
- Laser fiber advanced to SFJ position under ultrasound guidance
- Machine set to 5–7 W; foot pedal used to deliver continuous energy
- Fiber and sheath withdrawn 1 cm every 3–5 seconds
- Stop when fiber is 1–3 cm proximal to entry site
- Apply compression foot to thigh
Outcomes: EVLA and RFA result in durable ablation of the GSV with rates of recurrence and clinical severity scores comparable to open surgery, but with more rapid postprocedure recovery.
Both thermal techniques carry risks of DVT, ecchymosis, saphenous nerve injury (GSV) / sural nerve injury (SSV).
C. Nonthermal Endovenous Techniques
i. Mechanochemical Ablation (MOCA) — ClariVein® System
A rotating wire creates mechanical spasm in the vein wall, combined with concurrent injection of a sclerosant (typically 1% polidocanol or 1–3% STS).
Key advantage: No tumescent anesthesia required (no thermal injury risk); can access the vein more distally than thermal techniques without nerve injury risk.
Long-term durability appears equivalent to thermal ablation but remains under active investigation.
ii. Cyanoacrylate Adhesive Closure (VenaSeal™)
Proprietary cyanoacrylate glue injected into the vein lumen to permanently seal it. No tumescent anesthesia, no thermal energy. Demonstrates promising early results with good closure rates.
iii. Novel Combined Devices
Newer catheter systems combine mechanical endoluminal injury with sclerotherapy (nonthermal ablation) — e.g., MOCA devices.
D. Surgical Techniques
i. High Ligation and Stripping (HL&S) — Saphenous Vein Stripping
Still the preferred technique when:
- GSV diameter is very large (>2 cm)
- Technology or expertise for endovenous techniques is unavailable
- Anatomy precludes endovenous treatment (strong 1B guideline recommendation)
Technique:
- Small incisions medially in the groin (saphenofemoral junction) and just below the knee
- GSV ligated flush at SFJ with ligation of all SFJ tributaries
- GSV removed using a blunt-tip catheter or invagination pin stripper (pulled through the vein)
- Bleeding controlled with compression
Complications: Ecchymosis, hematoma, lymphocele, DVT, wound infection, saphenous nerve injury
Important: GSV stripping has a lower recurrence rate and better QoL than saphenofemoral junction ligation alone — stripping of the infragenicular GSV is essential.
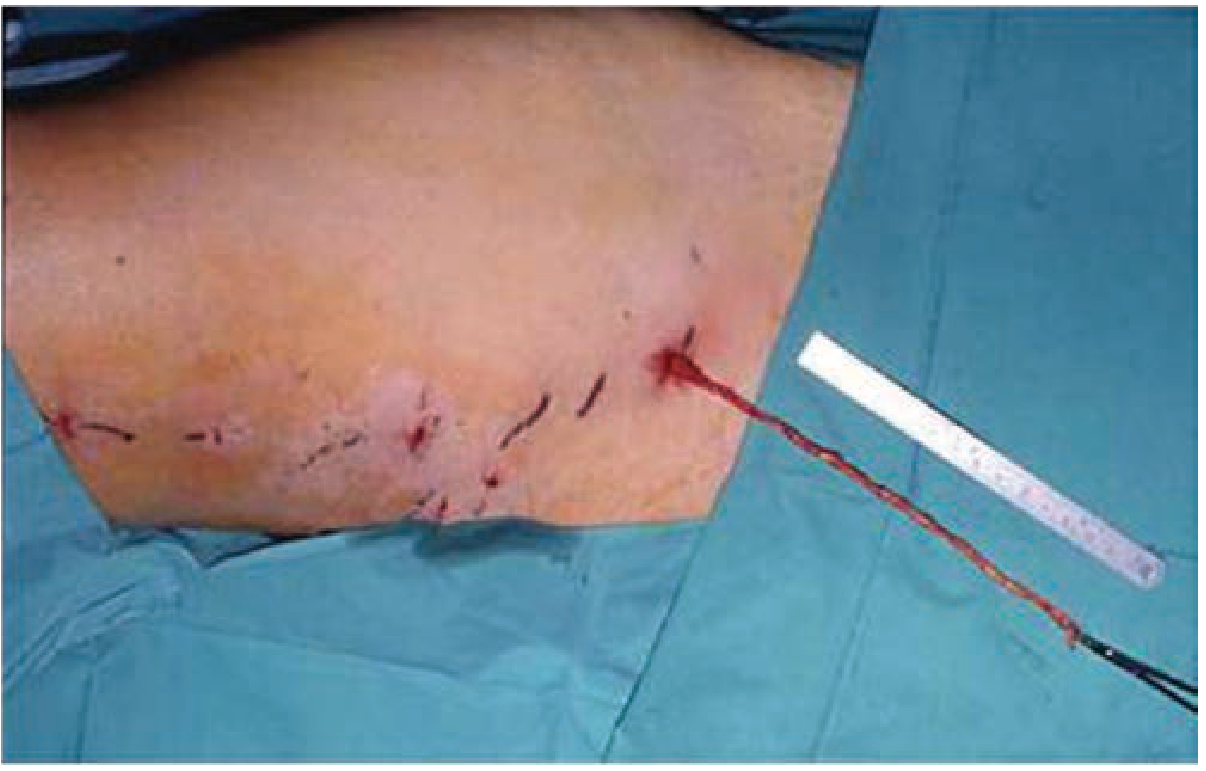
ii. Stab (Micro-)Avulsion Phlebectomy (Ambulatory Phlebectomy)
Used for larger branch varicosities not amenable to ablation alone. Can be performed alongside endovenous ablation or as a staged procedure.
Technique:
- 2 mm stab incisions made directly over marked branch varicosities
- Vein dissected bluntly from subcutaneous tissue through the small incision as far proximally and distally as possible
- Vein avulsed without ligation in most cases
- Bleeding controlled by leg elevation + manual compression + tumescent anesthesia
- No sutures needed for 2 mm incisions
E. Management of Deep Vein Reflux
Deep vein valve transplantation and valvuloplasty are available but uncommon and restricted to specialty centers. Current mainstream recommendations are nonsurgical for isolated deep reflux.
8. Clinical Results — Before vs. After
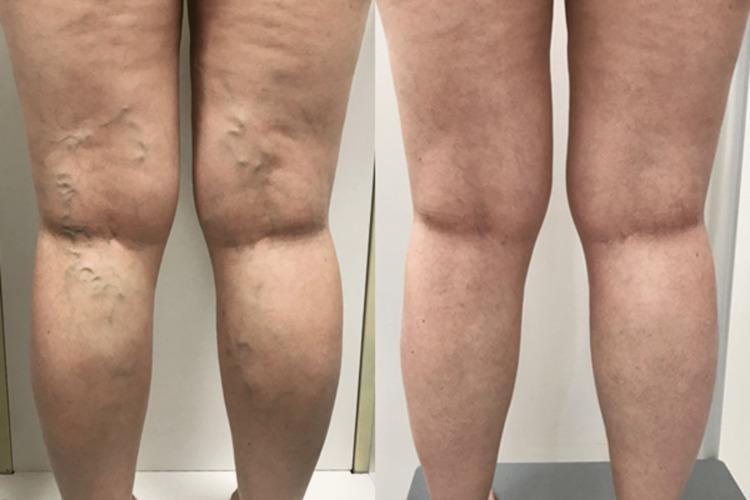
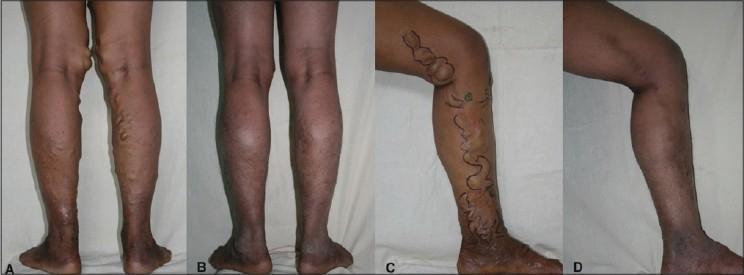
9. 2023 SVS/AVF/AVLS Clinical Practice Guidelines (PMID: 37652254)
The most current major guidelines recommend:
| Recommendation | Grade |
|---|---|
| Endovenous ablation preferred over HL&S for GSV/SSV | 1 (Strong) |
| HL&S if endovenous not available/feasible (GSV/SSV) | 1 (Strong), Level B |
| Either thermal or nonthermal ablation for symptomatic GSV axial reflux (groin to below knee) | 1 (Strong), Level B |
| EVLA, RFA, or HL&S preferred over UGFS for long-term QoL and reduced recurrence | 2 (Weak), Level B |
| Isolated SFJ incompetence alone does NOT justify ablation of a competent GSV | Consensus |
| Procedures can be performed in office, surgery center, or OR; office setting shows better patient experience and lower cost | Consensus |
10. Complications Summary
| Complication | Thermal Ablation | Stripping | Sclerotherapy |
|---|---|---|---|
| DVT | + | + | + |
| Nerve injury (saphenous/sural) | + | + | – |
| Ecchymosis/hematoma | + | ++ | + |
| Skin necrosis | – | – | + |
| Lymphocele | – | + | – |
| Infection | + | + | – |
| Hyperpigmentation | – | – | + |
| Recurrence | Low | Low | Higher (truncal) |
11. Special Considerations
- Recurrent varicose veins (C2r): Require repeat duplex mapping to identify neovascularization at previous SFJ ligation site, perforator incompetence, or untreated tributary reflux
- Venous ulcers (C6): Address superficial reflux urgently; concomitant compression therapy with wound care; early intervention reduces ulcer recurrence
- Pregnancy: Conservative management with compression; defer intervention until after delivery
- Bilateral disease: Treat the more symptomatic side first; reassess before treating contralateral side
Sources:
- Schwartz's Principles of Surgery, 11th Ed., Chapter 24
- Current Surgical Therapy, 14th Ed. — Treatment of Varicose Veins (Schulick & Whittaker)
- Pfenninger and Fowler's Procedures for Primary Care, 3rd Ed., Chapter 92
- 2023 SVS/AVF/AVLS Clinical Practice Guidelines [PMID: 37652254]
This is a shared conversation. Sign in to Orris to start your own chat.