Orbital cellulitis
Reading File
Finding Sources
Searching PubMed
"orbital cellulitis" AND management
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Loading Image
Loading Image
Here is a comprehensive overview of orbital cellulitis based on multiple ophthalmology and emergency medicine textbooks.
Orbital Cellulitis (Postseptal Cellulitis)
Definition
Orbital cellulitis is an infection of the soft tissues posterior to the orbital septum — a critical anatomical landmark separating the eyelid (preseptal) from the true orbit (postseptal). It is a sight- and life-threatening emergency.
Clinical Presentation
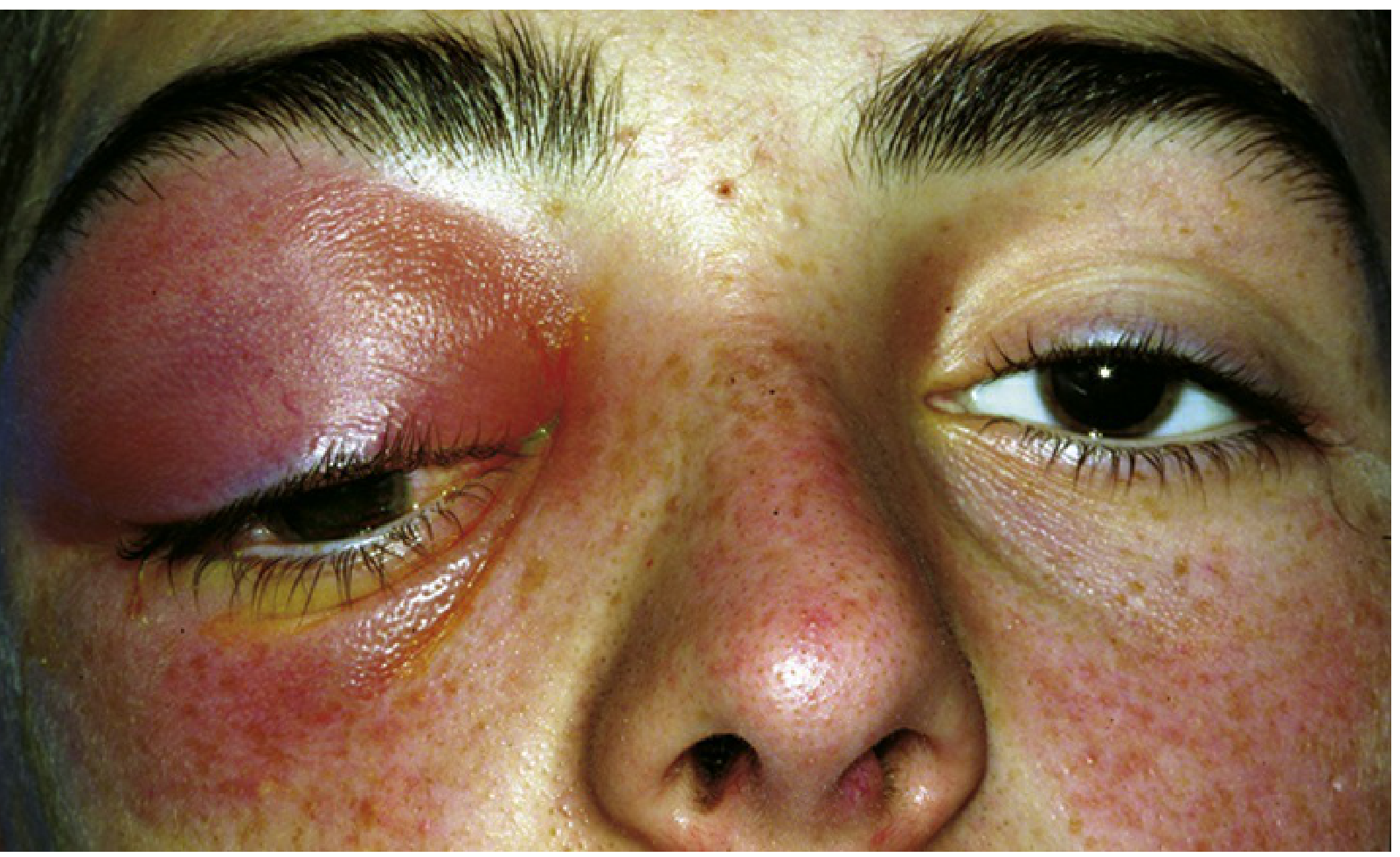
Symptoms
- Pain (worsened by eye movement)
- Eyelid and periorbital swelling
- Blurred/double vision
- Nasal congestion, sinus pressure/headache
- Fever, malaise
- Tooth pain (if dental source)
Signs (Critical)
- Eyelid edema, erythema, warmth, tenderness
- Conjunctival chemosis and injection
- Proptosis (often obscured by lid swelling; may be non-axial if abscess present)
- Painful ophthalmoplegia — restriction of extraocular movements
- Signs of optic neuropathy: RAPD, reduced VA, dyschromatopsia
- Retinal venous congestion, disc edema (on fundoscopy)
- Fever (often marked)
- Subconjunctival hemorrhage (sometimes)
Red flag — Cavernous Sinus Thrombosis
Headache + fever + CN III, IV, or VI deficits → suspect cavernous sinus thrombosis.
Preseptal vs. Postseptal: Key Distinction
| Feature | Preseptal (Periorbital) | Postseptal (Orbital) |
|---|---|---|
| Location | Anterior to orbital septum | Posterior to septum |
| Proptosis | Absent | Present |
| Ophthalmoplegia | Absent | Present |
| Pain on eye movement | Absent | Present |
| Visual change | Absent | May be present |
| Management | Oral antibiotics (mild), close follow-up | Mandatory hospitalization + IV antibiotics |
Etiology & Source
Most common source: paranasal sinusitis (ethmoid sinus most frequent — perforation of the thin lamina papyracea). Other sources:
- Dacryocystitis, dacryoadenitis, hordeolum
- Orbital/facial trauma, retained foreign body, ocular/sinus surgery
- Dental abscess (aggressive — may spread to cavernous sinus)
- Hematogenous spread / bacteremia
- Extension from preseptal cellulitis
Causative Organisms
| Population | Organisms |
|---|---|
| Adults | S. aureus, Streptococcus spp., Bacteroides (anaerobes) |
| Children (unvaccinated) | H. influenzae |
| Post-trauma | Gram-negative rods |
| Dental abscess | Mixed aerobes + anaerobes |
| Diabetics / immunocompromised | Mucor (zygomycosis), Aspergillus |
| General | S. pneumoniae, S. pyogenes, S. aureus |
Infection is frequently polymicrobial.
Investigations
- CT scan (orbits + paranasal sinuses + brain, with contrast) — vital: confirms diagnosis, identifies subperiosteal abscess (SPA), intracranial extension, or retained foreign body
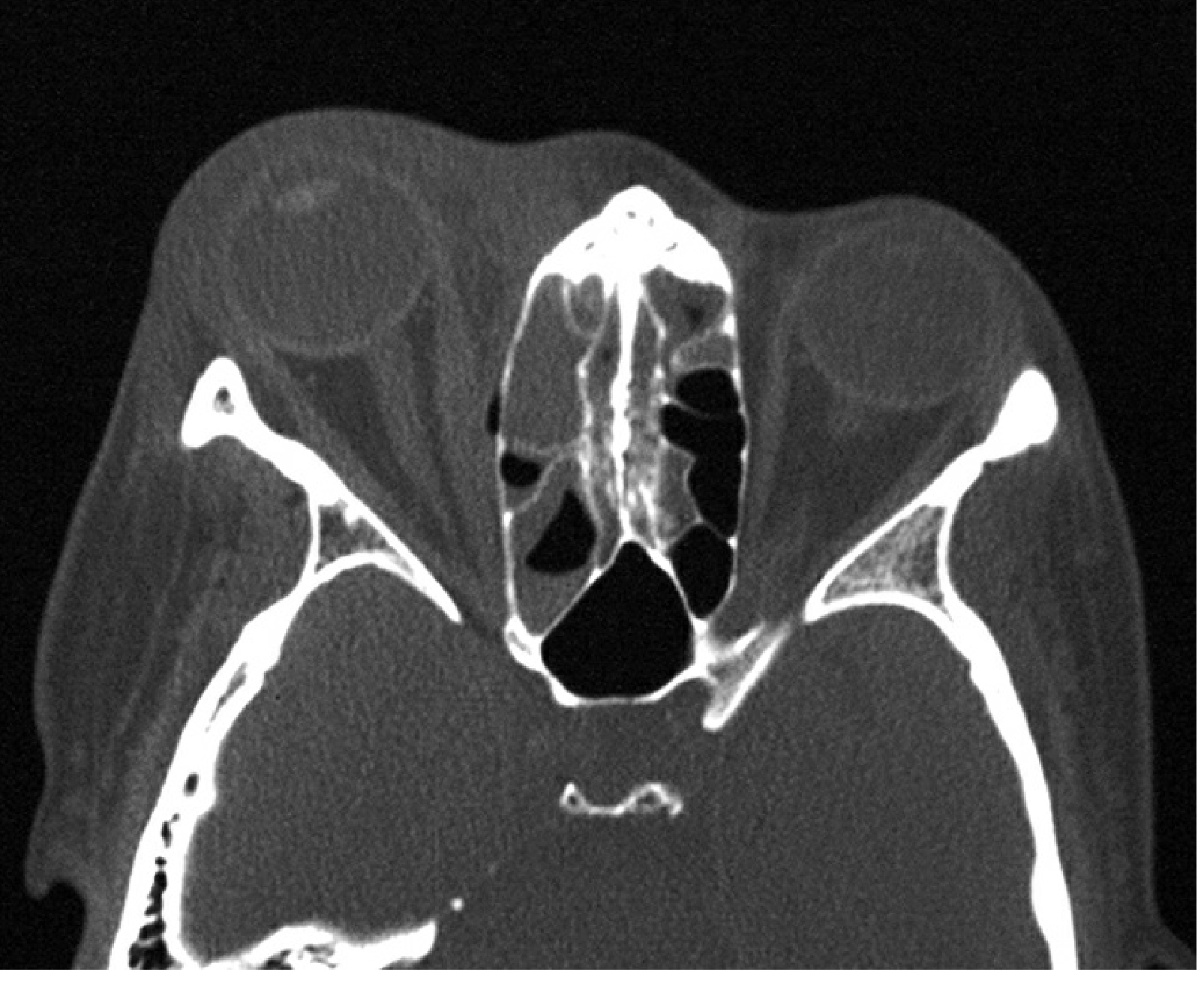
- CBC with differential
- Blood cultures
- Nasal discharge culture
- MRI — sometimes performed, especially if intracranial extension suspected
- Lumbar puncture — if meningeal or cerebral signs develop
- Gram stain + culture of any wound drainage
Management
Immediate Steps
- Hospitalize — mandatory
- Immediate ophthalmology consultation
- Otorhinolaryngology consultation (for sinus drainage if needed)
- Consider infectious disease, neurosurgery (if meningitis/abscess), oral-maxillofacial surgery (dental source) consultations
- Mark the extent of skin erythema with a surgical marker to monitor progress
Antibiotic Therapy
Broad-spectrum IV antibiotics covering Gram-positives, Gram-negatives, and anaerobes:
Community-acquired (no recent hospitalization):
- Ampicillin-sulbactam 3 g IV q6h (adults) — or —
- Piperacillin-tazobactam 4.5 g IV q8h (adults)
If MRSA coverage needed (skin source, severe, failed therapy, high CA-MRSA prevalence area, or hospital-acquired):
- Add vancomycin (target trough 15–20 mcg/mL)
Alternative broad-spectrum options:
- Vancomycin + third-generation cephalosporin ± metronidazole
- Imipenem or meropenem
- Ticarcillin-clavulanate
Anaerobic coverage: Add metronidazole or clindamycin when not covered by the primary agent.
IV antibiotics continued until afebrile for ~4 days → followed by 1–3 weeks of oral therapy.
Adjunctive Treatment
- Nasal decongestant spray (e.g., oxymetazoline) for up to 3 days
- Nasal corticosteroid spray to quicken sinusitis resolution
- Erythromycin/bacitracin ointment qid for corneal exposure/chemosis
- Systemic corticosteroids — controversial; if used, wait 24–48 h after IV antibiotics started (studies suggest they shorten hospital stay in pediatric orbital cellulitis)
Surgical Indications
- Orbital abscess → operative drainage + debridement
- Subperiosteal abscess → usually requires drainage (especially if large, medial wall)
- Tight orbit, optic neuropathy, severely elevated IOP → emergency lateral canthotomy/cantholysis
- Lack of antibiotic response or very severe sinus disease → surgical sinus drainage
Monitoring & Follow-Up
- Re-evaluate at least twice daily for the first 48 h; severe infections may need multiple daily exams
- Clinical improvement may lag 24–36 hours after starting IV antibiotics
- Monitor: temperature, WBC, VA, color vision, pupillary response, EOM, proptosis, globe displacement
- CRP is a useful clinical marker for monitoring progress
- If deterioration after 3–4 doses of IV antibiotics → repeat CT to rule out abscess formation
Complications
| Ocular | Intracranial |
|---|---|
| Optic neuropathy / visual loss | Cavernous sinus thrombosis |
| Exposure keratopathy | Meningitis |
| Elevated IOP | Brain abscess |
| Endophthalmitis | Subdural empyema |
| Central retinal artery/vein occlusion | Epidural abscess |
| Subperiosteal abscess | Frontal bone osteomyelitis |
Intracranial complications occur in ~3–4% of cases but are life-threatening.
Differential Diagnosis of Acutely Inflamed Orbit
- Preseptal (periorbital) cellulitis
- Subperiosteal abscess
- Orbital abscess
- Cavernous sinus thrombosis
- Dacryocystitis / dacryoadenitis
- Thyroid eye disease (acute)
- Orbital hemorrhage
- Carotid-cavernous fistula
- Neoplasia (rhabdomyosarcoma in children, metastases, lymphoma)
- Idiopathic orbital inflammation (orbital pseudotumor)
Sources: Wills Eye Manual 6e | Kanski's Clinical Ophthalmology 10e | Tintinalli's Emergency Medicine
This is a shared conversation. Sign in to Orris to start your own chat.