1 Clinical anatomy of the organ of vision. Membranes of the organ of vision. Chambers of the eye. Accessory apparatus of the eye (eyelids, lacrimal
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Loading Image
Loading Image
I now have comprehensive textbook content. Let me compile the complete answer.
Clinical Anatomy of the Organ of Vision
Sources: Gray's Anatomy for Students; Cummings Otolaryngology Head and Neck Surgery
1. The Orbit
The orbits are bilateral pyramidal bony cavities in the upper half of the face. They contain the eyeball, optic nerve, extra-ocular muscles, lacrimal apparatus, adipose tissue, fascia, and neurovascular structures.
Seven bones form the orbital framework:
- Maxilla, Zygomatic, Frontal, Ethmoid, Lacrimal, Sphenoid, Palatine
The orbit has the shape of a pyramid, with its wide base opening anteriorly and its apex directed posteromedially at the optic foramen (optic canal). The four walls are:
| Wall | Main Bone(s) |
|---|---|
| Roof (superior) | Orbital part of frontal bone + lesser wing of sphenoid |
| Medial | Ethmoid (largest contributor), lacrimal, maxilla, sphenoid |
| Floor | Maxilla, zygomatic, palatine |
| Lateral | Zygomatic + greater wing of sphenoid (strongest wall) |
The periorbita is the periosteum lining the orbit. Posteriorly, it thickens to form the common tendinous ring — the origin of the four rectus muscles.
2. The Eyeball
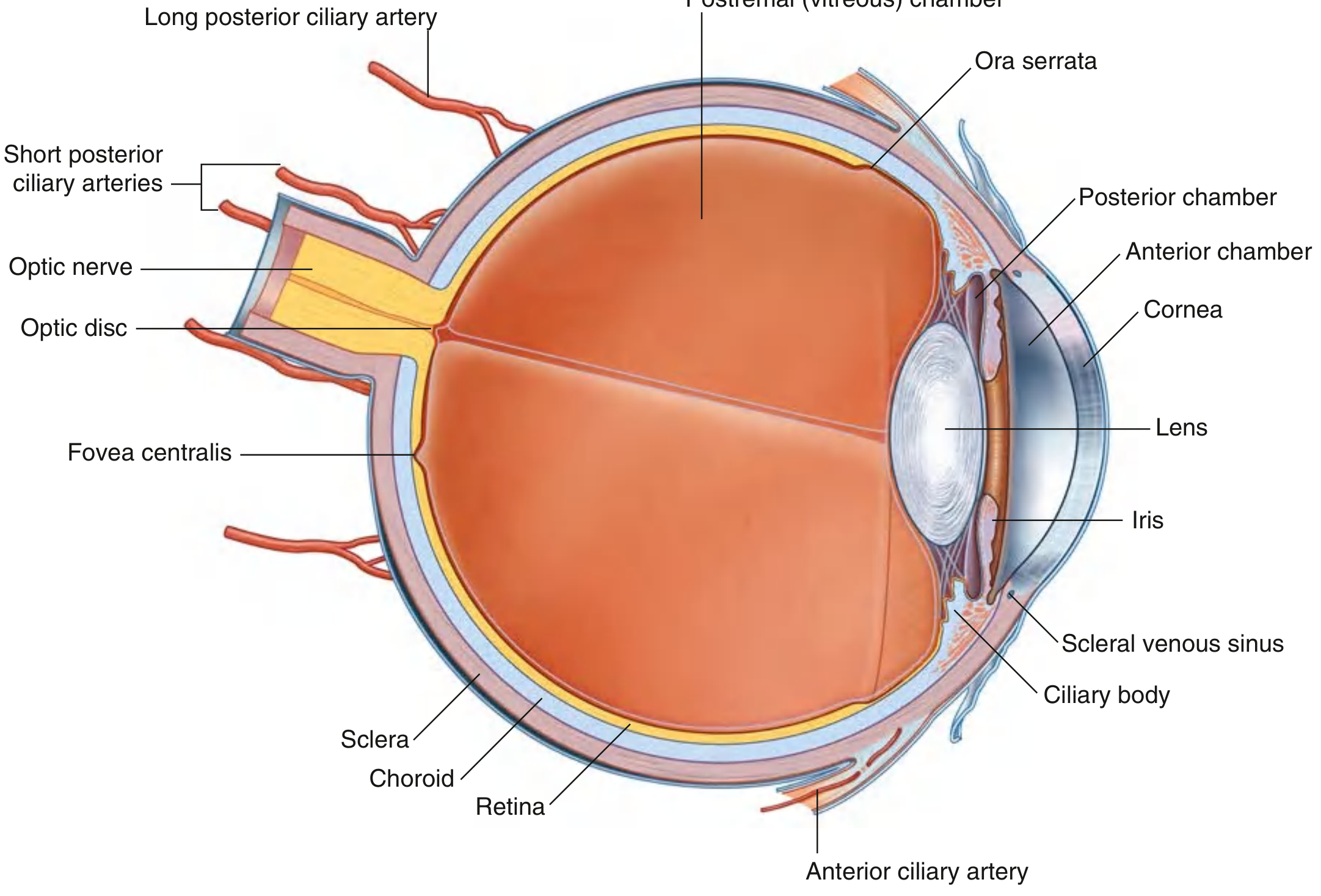
Fig. 8.111 — Cross-section of the Eyeball (Gray's Anatomy for Students)
The globe-shaped eyeball occupies the anterior orbit. Its anterior one-sixth bulges outward as the transparent cornea. From front to back the internal structures are: anterior chamber → iris/pupil → posterior chamber → lens → postremal (vitreous) chamber → retina.
3. Membranes (Walls/Tunics) of the Eyeball
The eyeball wall has three concentric layers:
A. Outer Fibrous Layer
- Sclera — covers the posterior and lateral 5/6 of the eyeball; opaque dense connective tissue (the "white of the eye"); pierced by the optic nerve posteriorly; provides muscle attachment points. The fascial sheath of the eyeball (bulbar sheath / Tenon's capsule) covers the external scleral surface between the optic nerve entrance and the corneoscleral junction.
- Cornea — covers the anterior 1/6; transparent, avascular; continuous with the sclera at the limbus; allows light entry.
B. Middle Vascular Layer (Uvea)
Three continuous parts from posterior to anterior:
- Choroid — posterior 2/3 of the vascular layer; thin, highly vascular and pigmented; supplies the outer retina; firmly adherent to retina internally, loosely to sclera externally.
- Ciliary body — extends from the anterior border of the choroid; triangular ring containing:
- Ciliary muscle — smooth muscle fibers (longitudinal, circular, radial); parasympathetic innervation via CN III; contraction loosens the suspensory ligament → lens rounds up → accommodation for near vision.
- Ciliary processes — longitudinal ridges projecting inward; give rise to zonular fibers (suspensory ligament of the lens) and secrete aqueous humor.
- Iris — the colored diaphragm anterior to the lens; contains:
- Sphincter pupillae — parasympathetic (CN III via ciliary ganglion); constricts pupil (miosis)
- Dilator pupillae — sympathetic (superior cervical ganglion via long ciliary nerves); dilates pupil (mydriasis)
C. Inner Layer (Retina)
- Optic (visual) retina — posterior portion; contains photoreceptors (rods for dim light/peripheral vision; cones for color/central vision)
- Optic disc (blind spot) — where the optic nerve exits; no photoreceptors
- Fovea centralis — highest cone density; sharpest central vision
- Nonvisual retina — covers the inner surface of the ciliary body and iris anteriorly (ora serrata marks the transition)
4. Chambers of the Eye
Anterior Chamber
- Located posterior to the cornea, anterior to the iris
- Filled with aqueous humor
Posterior Chamber
- Located posterior to the iris, anterior to the lens
- Aqueous humor is secreted here by ciliary processes → flows through the pupil → anterior chamber → drains into the scleral venous sinus (Canal of Schlemm) at the iridocorneal angle
- Aqueous humor supplies nutrients to the avascular cornea and lens and maintains intraocular pressure
- Disruption → glaucoma (elevated intraocular pressure)
Postremal (Vitreous) Chamber
- The posterior 4/5 of the eyeball, from lens to retina
- Filled with the vitreous body — transparent, gelatinous; unlike aqueous humor, it cannot be replaced
Lens
- Separates anterior 1/5 from posterior 4/5 of the eyeball
- Transparent, biconvex, elastic; attached by zonular fibers to the ciliary body
- Opacity of the lens = cataract
5. Accessory Apparatus
A. Eyelids (Palpebrae)
The eyelids are the protective coverings of the eye. Each consists of anterior and posterior lamellae:
Anterior lamella:
- Skin — thinnest skin in the body; highly vascular; heals rapidly with minimal scarring
- Orbicularis oculi muscle — subcutaneous sphincter of the eyelid; innervated by temporal and zygomatic branches of CN VII (facial nerve); divided into pretarsal, preseptal, and orbital segments; also drives the lacrimal pump — contraction during blinking dilates the lacrimal sac and draws tears through the canaliculi
Posterior lamella:
- Tarsal plates — dense connective tissue plates giving rigidity to the eyelids; contain tarsal (Meibomian) glands — modified sebaceous glands secreting an oily substance that reduces tear evaporation; blockage = chalazion
- Conjunctiva — thin transparent membrane lining the posterior eyelid surface, then reflecting onto the anterior sclera to the limbus; forms the conjunctival sac (superior and inferior fornices)
Muscles specific to upper lid:
- Levator palpebrae superioris — raises the upper eyelid; inserts into superior tarsus and eyelid skin; innervated by CN III (oculomotor)
- Superior tarsal muscle (Müller's muscle) — smooth muscle from the inferior surface of the levator to the upper edge of the superior tarsus; innervated by postganglionic sympathetic fibers from the superior cervical ganglion. Loss of either muscle → ptosis
Surface anatomy:
- Normal horizontal palpebral fissure: 28–30 mm; vertical: 9–10 mm
- Upper lid margin sits at the midpoint between superior corneal limbus and pupil
- Lower lid margin abuts the inferior corneal limbus
- Upper lid crease: 10–12 mm above lid margin in women, 7–8 mm in men
Glands of the eyelid margin:
- Tarsal (Meibomian) glands — sebaceous, open onto lid margin; blockage → chalazion (inner surface)
- Sebaceous and sweat glands of the eyelash follicles — blockage → sty/hordeolum (lid edge)
B. Lacrimal Apparatus
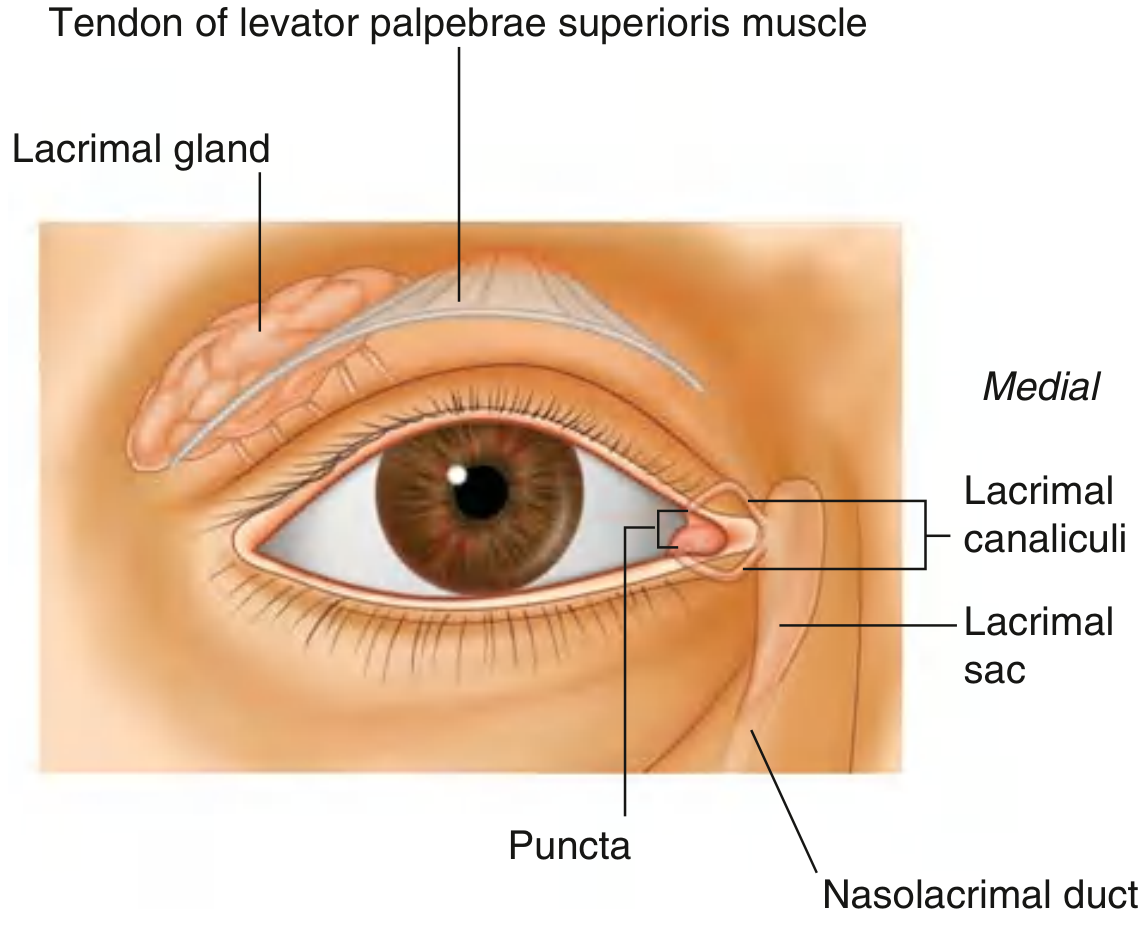
Fig. 8.86 — Lacrimal Apparatus, Anterior View (Gray's Anatomy for Students)
The lacrimal apparatus produces, distributes, and drains tears. It comprises:
1. Lacrimal Gland
- Located in the superolateral orbit, in the lacrimal fossa of the frontal bone
- Divided into two parts by the levator palpebrae superioris:
- Orbital part (larger) — in the lacrimal fossa
- Palpebral part (smaller) — inferior to the levator, in the superolateral eyelid
- Numerous ducts empty into the lateral superior conjunctival fornix
- Innervation:
- Sensory — lacrimal branch of the ophthalmic nerve (V1)
- Secretomotor (parasympathetic) — preganglionic from CN VII (greater petrosal nerve) → pterygopalatine ganglion → postganglionic fibers travel with the zygomatic nerve then lacrimal nerve → gland
- Sympathetic — from superior cervical ganglion
2. Tear Flow Path
- Secreted laterally → spread medially by blinking
- Accumulate in the medial lacrimal lake
- Enter through the lacrimal puncta (one per eyelid, on the medial lid margin)
- Travel through the lacrimal canaliculi (superior and inferior) medially
- Enter the lacrimal sac — situated in the lacrimal fossa between the anterior and posterior lacrimal crests (posterior to the medial palpebral ligament)
- Drain inferiorly via the nasolacrimal duct → opens into the inferior nasal meatus beneath the inferior nasal concha
Clinical note: Blinking contracts the orbicularis oculi (lacrimal part), dilating the lacrimal sac and actively drawing tears into it. Facial nerve paralysis disrupts this pump → epiphora (overflow of tears).
Summary Table
| Structure | Key Feature | Clinical Relevance |
|---|---|---|
| Cornea | Transparent, avascular | Nourished by aqueous humor |
| Sclera | Opaque, "white of eye" | Muscle attachment |
| Choroid | Highly vascular, pigmented | Supplies outer retina |
| Ciliary body | Aqueous production + accommodation | Glaucoma, accommodation disorders |
| Iris | Sphincter + dilator pupillae | Miosis/mydriasis, pupillary reflexes |
| Retina | Photoreceptors, fovea, optic disc | Retinal detachment, macular disease |
| Canal of Schlemm | Aqueous drainage at limbus | Blocked → glaucoma |
| Lens | Biconvex, transparent | Opacity → cataract |
| Vitreous | Irreplaceable gelatinous filling | Floaters, retinal detachment |
| Tarsal (Meibomian) glands | Reduce tear evaporation | Chalazion if blocked |
| Lacrimal puncta | Tear entry to drainage | Obstruction → epiphora |
| Nasolacrimal duct | Drains to inferior meatus | Dacryocystitis |
— Gray's Anatomy for Students, pp. 1067–1093; Cummings Otolaryngology, Chapter 26
This is a shared conversation. Sign in to Orris to start your own chat.