Malnutrition
Reading File
Asking for Preferences
Finding Sources
Searching PubMed
"malnutrition"[MeSH Terms] AND ("diagnosis" OR "management")
Searching the Web
malnutrition types causes clinical features diagnosis treatment 2024
Reading File
Reading File
Finding Sources
Reading File
Reading File
Finding Sources
Reading File
Reading File
Searching Images
kwashiorkor marasmus protein energy malnutrition children
Reading File
I now have sufficient comprehensive content. Here is a complete, textbook-grounded overview of malnutrition:
Malnutrition
Definition & Classification
Malnutrition is an imbalance between nutrient intake and the body's requirements, resulting in deficits that impair physiological function.
- Primary malnutrition: Dietary intake itself is insufficient (poverty, famine, food insecurity).
- Secondary (conditional) malnutrition: Dietary intake is adequate, but malnutrition results from malabsorption, impaired use/storage, excess losses, or increased requirements. Categories include:
- Gastrointestinal diseases (celiac, IBD, short-gut syndrome, pancreatitis)
- Chronic wasting diseases (cancer cachexia, tuberculosis, AIDS)
- Acute critical illness (burns, sepsis, major surgery)
Causes
| Category | Examples |
|---|---|
| Poverty & food insecurity | Refugees, war, drought, crop failure |
| Ignorance | Unrecognized needs of infants, elderly, pregnant women |
| Chronic excess alcohol use | Poor diet + impaired absorption of thiamine, folate, B6, vitamin A |
| Acute/chronic illness | Burns (BMR may double), advanced cancer, disseminated TB, AIDS |
| Self-imposed restriction | Anorexia nervosa, bulimia, restrictive diets |
| GI/malabsorption | IBD, celiac, short-gut, protein-losing enteropathy, nephrotic syndrome |
| Hospitalization | Fasting for procedures, catabolic hormones, drugs (corticosteroids, chemotherapy) |
Severe Acute Malnutrition (SAM)
The WHO defines SAM as weight-for-height ≥3 SD below the median, visible wasting, or nutritional edema. ~50 million children worldwide are affected; ~45% of deaths in children under 5 in low-resource countries are attributable to undernutrition.
SAM has two protein compartments affected differently:
- Somatic compartment (skeletal muscle) — more depleted in marasmus
- Visceral compartment (liver proteins, albumin) — more depleted in kwashiorkor
Marasmus vs. Kwashiorkor
| Feature | Marasmus | Kwashiorkor |
|---|---|---|
| Primary deficit | Severe calorie (and protein) deprivation | Protein deprivation relatively greater than calorie reduction |
| Weight for age | <60% of expected | 60–80% of expected |
| Edema | Absent | Present (bilateral pitting; ascites) |
| Muscle/fat wasting | Marked (emaciation, "old man" facies, "baggy pants" sign) | Relatively spared (masked by edema) |
| Serum albumin | Normal or near-normal | Markedly low (hypoalbuminemia drives edema) |
| Liver | Normal | Enlarged and fatty (impaired lipoprotein synthesis) |
| Skin/hair | Less affected | "Flaky paint" dermatosis; depigmented hair; bands of pale/dark color |
| Behavior | Alert but weak | Apathy, listlessness, loss of appetite |
| Mechanism | Adaptive: cortisol + low leptin → lipolysis; somatic muscle catabolized for gluconeogenesis; visceral protein preserved | Non-adapted: insulin (from carb intake) suppresses lipolysis/proteolysis → visceral protein depleted; fatty liver |
Marasmic-kwashiorkor is a mixed form with features of both.
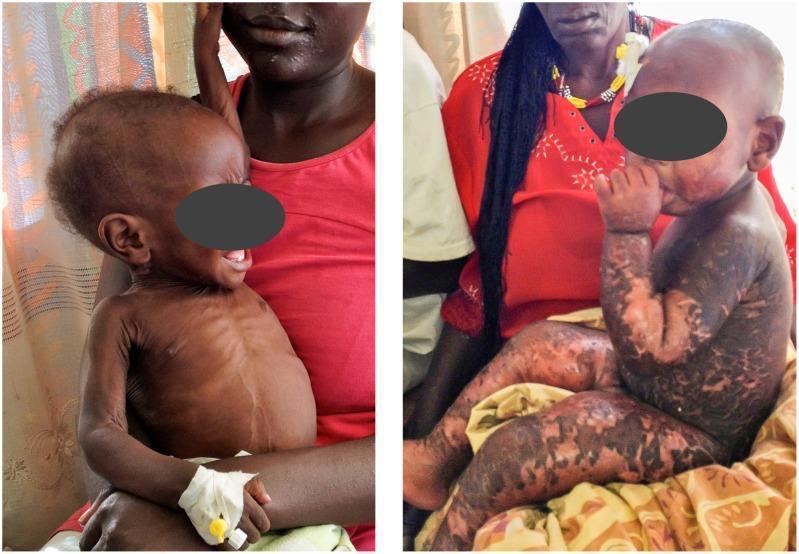
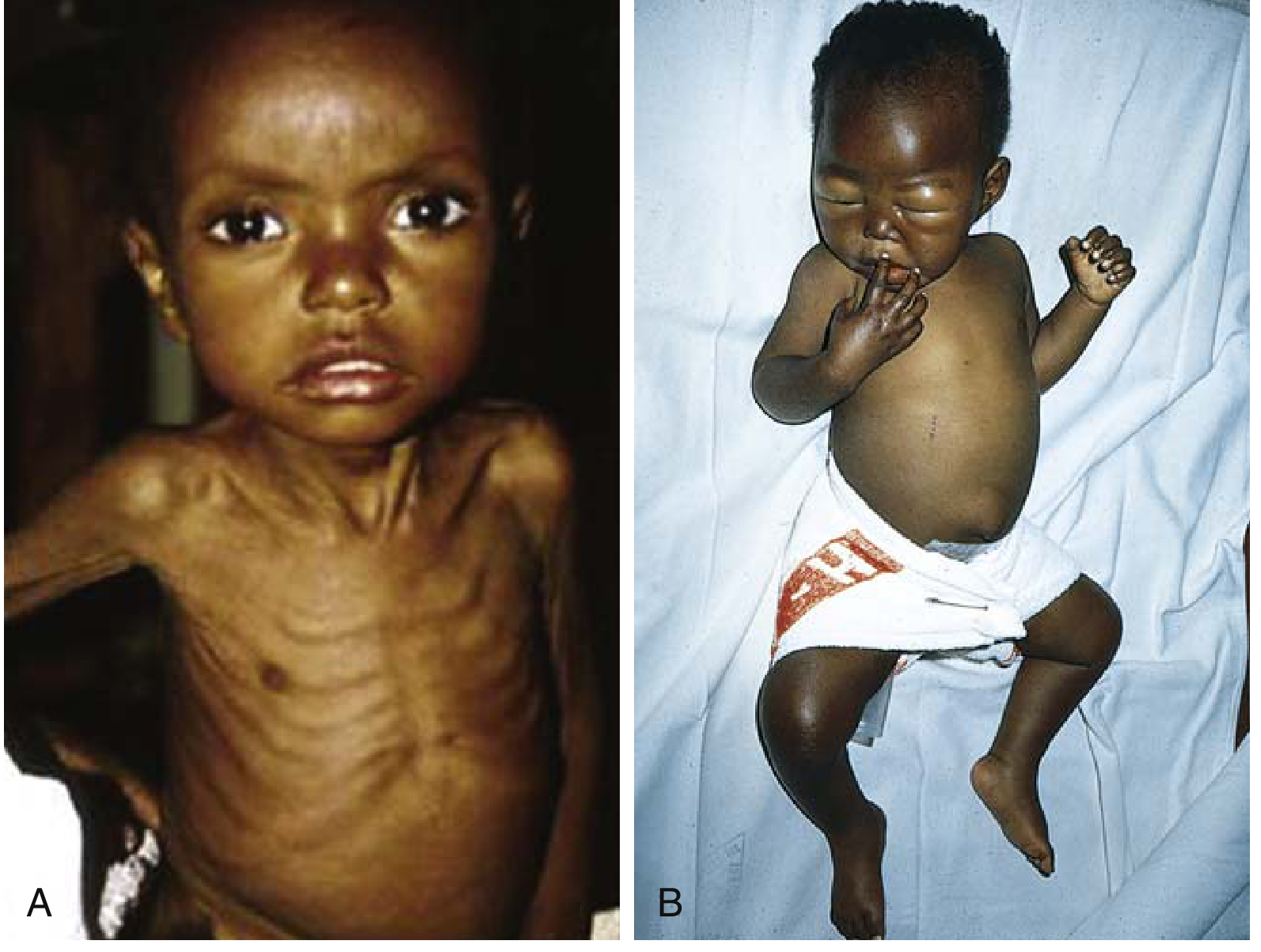
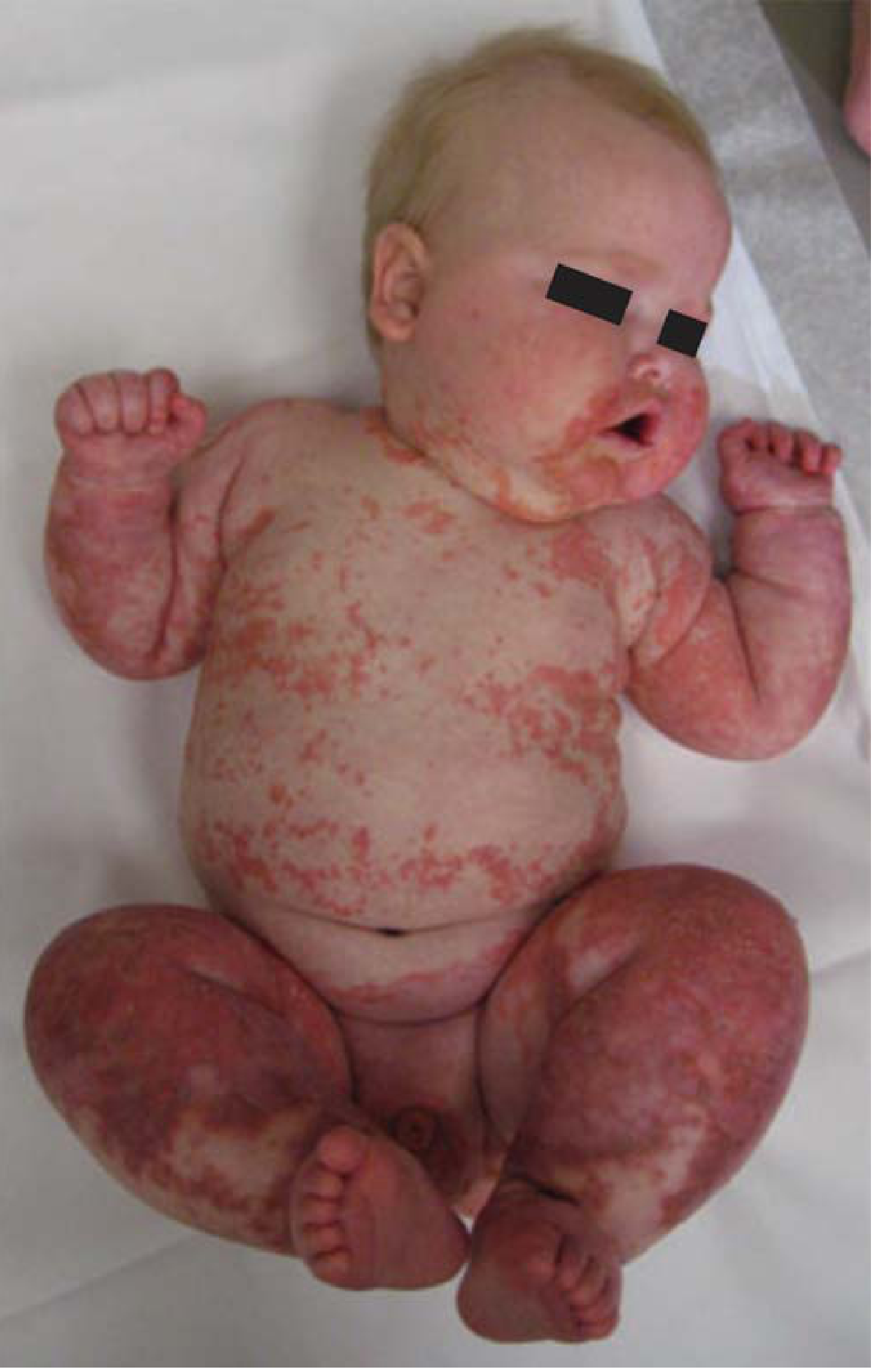
Pathological Changes (Morphology)
- Growth failure in both forms
- Peripheral edema in kwashiorkor; absent in marasmus
- Fatty liver in kwashiorkor (reduced apolipoprotein synthesis → impaired VLDL export → hepatic triglyceride accumulation)
- Small bowel atrophy: decreased crypt mitoses, villous atrophy, disaccharidase deficiency → lactose intolerance (reversible with treatment)
- Bone marrow hypoplasia: predominantly decreased red cell precursors → microcytic anemia (iron deficiency) ± macrocytic component (folate deficiency)
- Cerebral atrophy in infants: reduced neurons, impaired myelination (most critical in first 1–2 years of life)
- Thymic and lymphoid atrophy → impaired T cell–mediated immunity → susceptibility to secondary infections (helminths, TB, etc.)
- Secondary malnutrition signs: subcutaneous fat depletion (arms, chest, shoulders), quadriceps/deltoid wasting, ankle/sacral edema
Gut Microbiome
Recent evidence shows the gut microbiome is substantially altered in SAM — these changes appear to be not merely a consequence but may play a causative role in the pathogenesis of SAM. — Robbins & Kumar Basic Pathology
Secondary Malnutrition (Hospital & Chronic Illness)
More prevalent in high-income countries — >50% of US nursing home residents may be malnourished. Weight loss >5% due to malnutrition increases mortality risk ~5-fold.
Mechanisms in hospitalized patients (from Goldman-Cecil Medicine):
- Reduced food intake (anorexia, GI symptoms, procedure fasting)
- Increased catabolism: cortisol, catecholamines, glucagon, pro-inflammatory cytokines (IL-1, IL-6, TNF-α)
- Peripheral resistance to insulin and IGF-1
- Drug effects: corticosteroids, chemotherapy, diuretics
- Bedrest and immobility → muscle wasting
Screening & Diagnosis
Screening tools:
| Tool | Setting |
|---|---|
| NRS-2002 (Nutritional Risk Screening 2002) | Hospitalized adults — most widely used; predicts postoperative complications |
| MNA-SF (Mini Nutritional Assessment–Short Form) | Elderly / outpatient |
| SNAQ (Short Nutritional Assessment Questionnaire) | Predicts future involuntary weight loss |
| MUST (Malnutrition Universal Screening Tool) | Community settings |
| SGA (Subjective Global Assessment) | General, but limited in critically ill |
GLIM diagnostic criteria (Global Leadership Initiative on Malnutrition — current standard):
- Phenotypic criteria (≥1 required): unintentional weight loss, low BMI, reduced muscle mass
- Etiologic criteria (≥1 required): reduced food intake/assimilation, or high disease burden (inflammation)
- Severity: moderate or severe
Objective parameters:
- Skinfold thickness (fat stores)
- Mid-arm circumference (somatic protein/muscle mass)
- Serum albumin, transferrin (visceral protein compartment)
- Weight-for-height vs. standard tables
Management
1. Nutritional Rehabilitation
- Oral feeding is preferred; high-calorie, high-protein diet with vitamin and mineral supplementation
- Refeeding caution: Severely malnourished patients are at risk of refeeding syndrome — rapid carbohydrate administration drives phosphate into cells → severe hypophosphatemia; also hypokalemia and hypomagnesemia. Monitor and correct electrolytes before and during refeeding
- Kwashiorkor and lactose intolerance: Initial feeding should avoid full-strength milk-based diets due to disaccharidase deficiency; mucosal changes reverse with treatment
2. Enteral Nutrition
- Preferred over parenteral when GI tract is functional (tube feeding)
3. Parenteral Nutrition
- Reserved for patients with non-functional GI tracts; requires vitamin (especially thiamine) and mineral supplementation
4. Micronutrient Correction
- Vitamin C: 10–2000 mg/day reverses impaired wound healing
- Vitamin A: Corrects immune suppression; reverses steroid-impaired wound healing
- Zinc: Critical for RNA/DNA polymerase; supplement in burns, polytrauma, cirrhosis
- Iron: Correct iron-deficiency anemia
- Thiamine: Must be given before glucose in alcoholic malnourished patients to prevent irreversible Wernicke-Korsakoff syndrome
- Folate, B6: Especially in chronic alcohol use
5. Treat Underlying Cause
- Address GI disease, malignancy, infection, eating disorders, or psychosocial determinants
Special Scenarios
Anorexia & Bulimia Nervosa
Self-induced; clinical picture similar to SAM. Key features unique to anorexia: amenorrhea (low GnRH → low LH/FSH), bradycardia, cold intolerance (low T3), lanugo hair, decreased bone density, and risk of sudden cardiac death from hypokalemia (arrhythmia).
Cancer Cachexia
Driven by TNF-α, IL-1, IL-6 — distinct metabolic syndrome with anorexia, muscle wasting, and inflammation; not fully reversible with nutrition alone.
Wound Healing
Hypoalbuminemia (<2.0 g/dL) delays healing and promotes wound dehiscence. Protein supplements, vitamins A and C, and zinc are essential for wound repair.
Global Burden
- ~45% of under-5 deaths in low-resource countries linked to undernutrition
- ~50 million children affected by SAM worldwide
- Malnutrition increases susceptibility to infections (impaired cell-mediated immunity) and creates a vicious cycle: infection → catabolism → worse malnutrition
Sources: Robbins & Kumar Basic Pathology; Goldman-Cecil Medicine; Lippincott Illustrated Reviews Biochemistry; Sabiston Textbook of Surgery; Sleisenger & Fordtran's GI & Liver Disease
This is a shared conversation. Sign in to Orris to start your own chat.