Pulmonary involvement in systemic disease
Reading File
Finding Sources
Finding Sources
Searching PubMed
"pulmonary manifestations" AND "systemic disease"
Finding Sources
Finding Sources
Reading File
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Loading Image
Finding Sources
Finding Sources
Reading File
Reading File
I now have comprehensive content from multiple authoritative sources. Let me compile a detailed, well-organized response.
Pulmonary Involvement in Systemic Disease
The lung is a frequent target organ in systemic diseases — particularly connective tissue diseases (CTDs), vasculitides, and granulomatous disorders. Virtually every compartment of the lung can be affected: parenchyma, pleura, vasculature, and airways.
1. Rheumatoid Arthritis (RA)
Pleuropulmonary complications occur in 30–60% of RA patients and are a major source of morbidity and mortality. ILD abnormalities may be present in >60% on imaging, though many are initially asymptomatic. Clinically apparent ILD occurs in ~10% and carries increased mortality.
Risk factors for pleuropulmonary disease in RA:
- High rheumatoid factor titers
- Anti-CCP antibodies (independent of tobacco use)
- Subcutaneous nodules
- Male sex (ILD is 3:1 male, even though RA is 2–4:1 female)
- MUC5B promoter variant rs35705950
- Elevated serum KL-6
Forms of lung involvement:
| Manifestation | Details |
|---|---|
| ILD / Interstitial pneumonitis | UIP or NSIP pattern; early lymphocytic infiltrate with germinal follicles, later replaced by fibrosis |
| Pleural disease | Found in 40% at autopsy; clinically apparent in ~5%; more common in men; effusion may precede arthritis |
| Pulmonary nodules | Necrobiotic nodules; must be aggressively investigated to exclude malignancy |
| Follicular bronchiolitis | Lymphoid hyperplasia along airways |
| Pulmonary hypertension | Least common; associated with Raynaud phenomenon |
| Caplan syndrome | Progressive upper lobe nodular fibrosis in RA + pneumoconiosis (coal workers) |
| Diffuse alveolar hemorrhage | Via pulmonary capillaritis (rare) |
Prognosis: UIP pattern on HRCT confers worse prognosis than NSIP. DLCO correlates with mortality; chronic fibrosis increases risk of bronchogenic carcinoma (adenocarcinoma/BAC).
Treatment: Corticosteroids first-line; methotrexate generally avoided (can cause ILD itself); nintedanib (150 mg BID) attenuates progressive lung function decline; rituximab used as second-line.
— Goldman-Cecil Medicine, p. 947; Fishman's Pulmonary Diseases, p. 1025
2. Systemic Sclerosis (Scleroderma)
ILD is the most common pulmonary complication of systemic sclerosis, occurring in 30–100% of cases (HRCT shows abnormality in >90%). Pulmonary disease is a leading cause of death.
Manifestations:
- ILD: Predominantly NSIP pattern (cellular > fibrotic early on, then honeycombing); UIP pattern also seen. Ground-glass attenuation on HRCT reflects the inflammatory/cellular phase, which predates fibrosis.
- Pulmonary arterial hypertension (PAH): More common in limited cutaneous SSc (lcSSc / CREST). Anticentromere antibodies predict PAH; anti-Scl-70 antibodies predict fibrosis. A disproportionate reduction in DLCO relative to lung volumes is a key clue to PAH.
- Pleural disease: Fibrous adhesions in 40% at autopsy; clinically apparent pleural effusion uncommon (usually secondary to cardiomyopathy or cor pulmonale).
- Scleroderma sine scleroderma: ILD and PAH can precede skin involvement; greater tendency toward PAH.
- Scar carcinoma: Scleroderma was the first ILD associated with scar carcinoma (adenocarcinoma or alveolar cell carcinoma).
Symptoms: Dyspnea on exertion → rest, cough; bibasilar crackles; clubbing is unusual (capillary destruction in nail beds).
Physiology: Restrictive pattern, preserved flow rates, reduced DLCO. Hypoxemia at rest and with exercise may be the only early finding.
Treatment:
- Mycophenolate mofetil (1500 mg BID) — first-line for SSc-ILD; similar efficacy to cyclophosphamide with fewer side effects
- Nintedanib (150 mg BID) — attenuates lung function loss, alone or with mycophenolate
- Tocilizumab (IL-6 receptor blocker, 162 mg weekly SC) — mitigates decline in patients with elevated inflammatory markers and short disease duration
- Rituximab — alternate immunosuppressive regimen
— Goldman-Cecil Medicine, p. 947; Fishman's Pulmonary Diseases, p. 1030
3. Systemic Lupus Erythematosus (SLE)
SLE has a predominantly vasculitic mechanism of lung injury, unlike the fibro-inflammatory pattern of RA and SSc.
Manifestations:
| Manifestation | Details |
|---|---|
| Pleuritis / pleural effusion | Most common lung manifestation; exudative |
| Acute lupus pneumonitis | Mimics acute interstitial pneumonia; widespread ground-glass + consolidation |
| Diffuse alveolar hemorrhage | Via pulmonary capillaritis; can be life-threatening |
| Thromboembolic disease | Antiphospholipid antibodies → pulmonary embolism |
| Chronic ILD | Less common; NSIP or LIP patterns |
| "Shrinking lung" syndrome | Restrictive defect from diaphragmatic weakness/dysfunction; resistant to corticosteroids |
| Pulmonary hypertension | Via vasculitis or recurrent emboli |
CT in SLE-associated Sjögren overlap (LIP pattern) shows characteristic cysts interspersed within ground-glass attenuation in the lower lobes:
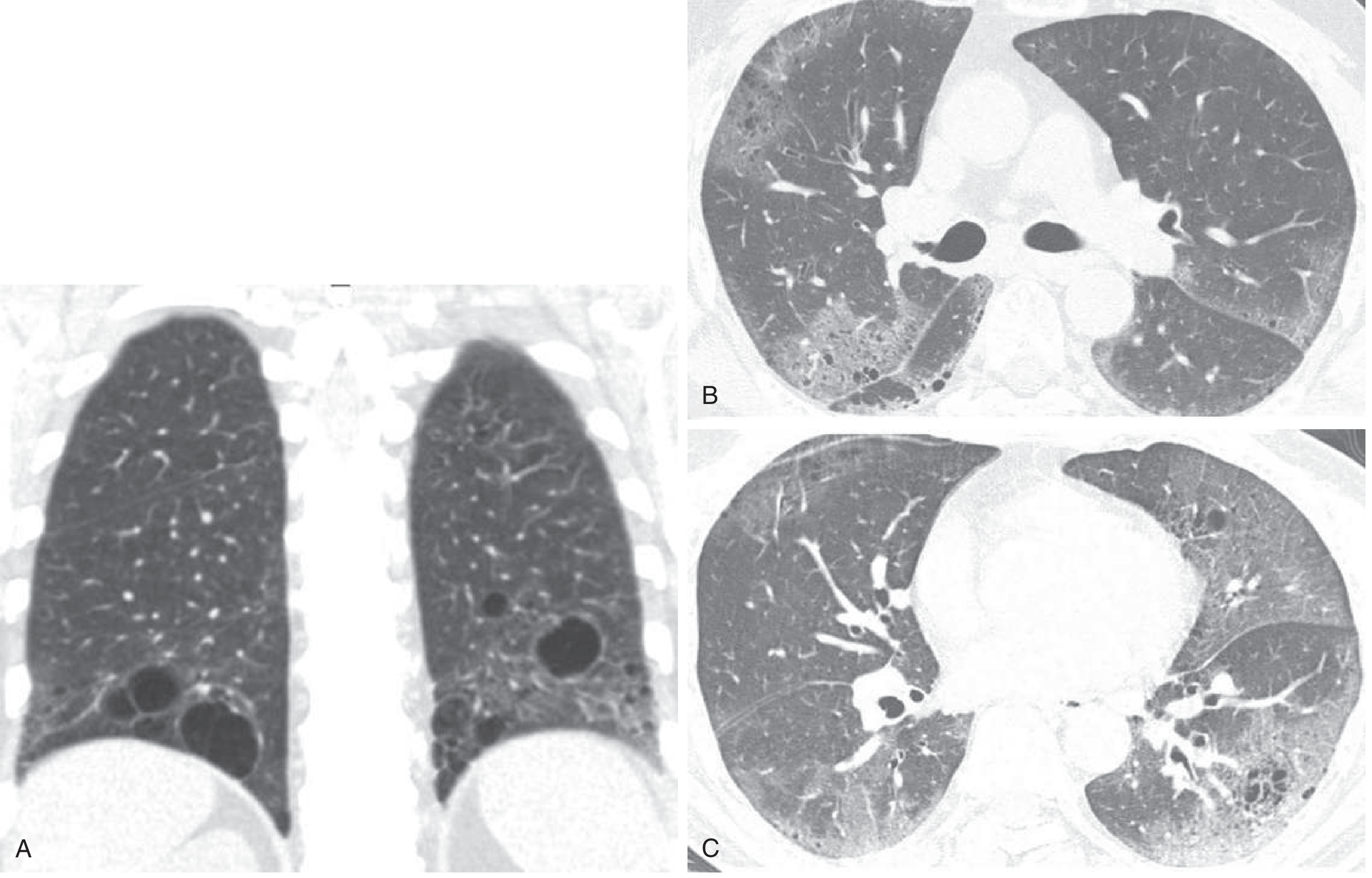
Treatment: Underlying SLE treatment (hydroxychloroquine, corticosteroids, immunosuppressives); infection must always be excluded in immunosuppressed acutely ill patients.
— Goldman-Cecil Medicine, p. 947–948; Textbook of Family Medicine 9e, p. 339
4. Dermatomyositis / Polymyositis (DM/PM)
ILD in DM/PM is more heterogeneous than other CTDs, with UIP, NSIP, organizing pneumonia (OP), and DAD patterns all reported.
Key features:
- Anti-Jo-1 antibody (or anti-PL-7) — the antisynthetase syndrome; associated with ILD, "mechanic's hands," and Raynaud
- ILD may precede muscular manifestations by months to years
- Severity of muscle disease does not correlate with ILD severity
- Acute presentation (DAD pattern): High mortality despite aggressive immunosuppression; resembles diffuse infectious pneumonia
- OP pattern: Responds well to corticosteroids
- Diffuse alveolar hemorrhage via pulmonary capillaritis — coincides with muscle disease onset; treat with corticosteroids + cyclophosphamide
Treatment: Corticosteroids; for refractory cases: cyclophosphamide, cyclosporine, tacrolimus, mycophenolate, IVIG, rituximab.
— Goldman-Cecil Medicine, p. 472; Fishman's Pulmonary Diseases, p. 1032
5. Sjögren Syndrome
- LIP (Lymphoid Interstitial Pneumonia): The most frequent subtype; also cryptogenic organizing pneumonia
- Bronchiectasis and recurrent respiratory infections are common in advanced disease (inspissated mucus)
- Response to corticosteroids/immunosuppressives is usually good
6. Mixed Connective Tissue Disease (MCTD)
- Overlap of SSc, SLE, RA, and PM/DM features; anti-RNP antibody
- Pleuropulmonary complications in 20–80%, most often subclinical
- Pulmonary hypertension is a major complication (5-year survival drops from 96% to 73% when PAH is present)
- Medium-vessel pulmonary artery vasculitis with IgG/C3 deposition
- Antiphospholipid syndrome may coexist → thromboembolic pulmonary hypertension
7. Ankylosing Spondylitis
- Upper lobe bilateral reticulonodular infiltrates with cyst formation due to parenchymal destruction (apical fibrobullous disease)
- No known effective therapy for this apical fibrosis
8. Sarcoidosis
A systemic granulomatous disease with lung involvement in >90% of cases.
Pulmonary staging (chest X-ray):
| Stage | Finding |
|---|---|
| 0 | Normal |
| I | Bilateral hilar lymphadenopathy only |
| II | Hilar adenopathy + parenchymal infiltrates |
| III | Parenchymal infiltrates without adenopathy |
| IV | Pulmonary fibrosis / honeycombing |
Key features:
- Non-caseating granulomas with ACE-secreting epithelioid cells → elevated serum ACE reflects granuloma burden
- Airway obstruction in bronchial sarcoidosis
- Pulmonary hypertension — vasocentric growth of granulomas; treated with bosentan (BoSAPAH trial)
- Even asymptomatic cutaneous sarcoidosis patients should be screened with CXR and PFTs annually
- Cavitary pulmonary sarcoidosis → risk of aspergilloma
9. ANCA-Associated Vasculitides
Granulomatosis with Polyangiitis (GPA, formerly Wegener's)
- Triad: upper respiratory tract (sinusitis, saddle-nose), pulmonary (nodules, cavities, DAH), and renal (crescentic GN)
- PR3-ANCA (c-ANCA) positive
- Upper and lower airway involvement; subglottic stenosis
Eosinophilic Granulomatosis with Polyangiitis (EGPA, formerly Churg-Strauss)
- Allergic rhinitis + asthma + peripheral eosinophilia + pulmonary infiltrates + systemic vasculitis
- MPO-ANCA (p-ANCA) positive
- Skin: palpable purpura, indurated nodules over extensor surfaces
- Histology: necrotizing granulomas + tissue eosinophilia
Summary Table
| Disease | Dominant ILD Pattern | Pleural | PAH | Other Key Features |
|---|---|---|---|---|
| RA | UIP, NSIP | Common (exudate, low glucose) | Uncommon | Nodules, Caplan syndrome |
| SSc | NSIP > UIP | Uncommon | Major (especially lcSSc) | Anticentromere → PAH; anti-Scl-70 → fibrosis |
| SLE | LIP, NSIP | Common (pleuritis) | Via emboli/vasculitis | Shrinking lung, DAH, APS |
| DM/PM | NSIP, UIP, OP, DAD | Uncommon | Rare | Anti-Jo-1; DAD = high mortality |
| Sjögren | LIP, OP | Rare | Rare | Bronchiectasis |
| MCTD | NSIP | Pleuritis (40%) | Significant | Anti-RNP |
| AS | Apical fibrobullous | No | No | Upper lobe bullae |
| Sarcoidosis | Granulomatous | Rare | Vasocentric form | ACE elevated; staged I–IV |
| GPA | Nodules/cavities/DAH | Rare | Rare | PR3-ANCA, saddle-nose |
| EGPA | Eosinophilic infiltrates | Rare | Rare | Asthma, MPO-ANCA |
Sources: Robbins & Cotran Pathologic Basis of Disease (p. 646); Goldman-Cecil Medicine (pp. 947–948); Fishman's Pulmonary Diseases and Disorders (pp. 1025–1032); Textbook of Family Medicine 9e (p. 339)
Include recent guidelines, add pictures, references and make me a proper presentation
Reading File
Searching PubMed
"interstitial lung disease" AND "connective tissue disease" AND guidelines
Searching PubMed
"systemic sclerosis" AND "interstitial lung disease" AND treatment
Searching Images
pulmonary interstitial lung disease CT HRCT connective tissue
Reading File
Reading Article
Reading Article
Reading Article
Searching Images
sarcoidosis chest X-ray bilateral hilar lymphadenopathy
Searching Images
rheumatoid arthritis pulmonary nodules pleural effusion chest CT
Searching Images
scleroderma systemic sclerosis NSIP interstitial fibrosis HRCT honeycomb
Reading Article
Reading Article
Running Command
Running Command
Running Command
Writing File
Running Command
Running Command
Editing File
Running Command
Running Command
Running Command
Running Command
Running Command
Running Command
Your presentation is ready — 2.7 MB, 18 slides:
Pulmonary Involvement Systemic Disease
Presentation · PPTX
What's inside (18 slides)
| # | Slide |
|---|---|
| 1 | Title slide — dark navy design with topic and guideline sources |
| 2 | Outline — all 10 topic sections with color-coded navigation |
| 3 | Introduction — compartment overview (CTDs, vasculitides, granulomatous) |
| 4 | RA — Manifestations — 7 forms of pleuropulmonary disease + risk factors + HRCT image |
| 5 | RA — Treatment — ACR/CHEST 2023 recommendations; methotrexate warning; nintedanib |
| 6 | Systemic Sclerosis — ILD vs PAH side-by-side; antibody associations |
| 7 | SSc Imaging — 3 HRCT panels: GGO, traction bronchiectasis, dilated PA, dilated esophagus |
| 8 | SSc Treatment — Drug table: MMF (STRONG first-line), nintedanib, tocilizumab, rituximab; glucocorticoids STRONG AGAINST |
| 9 | SLE — 7 manifestations + CT image of LIP (cysts/GGO) |
| 10 | DM/PM + Sjögren + MCTD — 3-column with MCTD HRCT image |
| 11 | Ankylosing Spondylitis & Drug-Induced ILD |
| 12 | Sarcoidosis — Stage 0–IV table + Key features + Stage I CXR image |
| 13 | ANCA Vasculitides — GPA, EGPA, Goodpasture 3-column |
| 14 | 2023 ACR/CHEST Screening Guidelines — all 15 recommendations structured by strength |
| 15 | Summary Table — 9 diseases × 5 columns |
| 16 | Recent Guidelines 2023–2026 — 5 guidelines with PMIDs (ACR/CHEST, ATS, EULAR, ERS/EULAR) |
| 17 | Imaging Gallery — 4-panel HRCT/CXR on dark background |
| 18 | References — 9 citations with PMIDs |
make the ppt simple and elegant
Reading File
Running Command
Writing File
Running Command
Running Command
Done. Here's your clean, elegant rebuild:
Pulmonary Systemic Disease Elegant
Presentation · PPTX
What changed in the redesign:
| Before | After |
|---|---|
| Heavy colored bars everywhere | Warm off-white (#F8F7F5) background, single 6px top accent line |
| Multiple competing colors per slide | Deep navy + mid blue as the only two accents |
| Busy header boxes on every slide | Subtle small-caps category label + clean title |
| Cluttered boxes with thick borders | Minimal white cards with a 1pt light border |
| Color-saturated footers | Simple slide counter in muted grey, bottom right |
| Dark "imaging" slides with neon labels | Clean dark slide with restrained caption text |
Slides (16 total):
- Title — navy left / white right split layout
- Overview — three disease-category cards
- Rheumatoid Arthritis — manifestations + HRCT image
- Systemic Sclerosis — ILD vs PAH + two HRCT images
- SSc Treatment — drug cards (MMF, nintedanib, tocilizumab, rituximab, CYC, steroid-avoid)
- SLE — manifestations + LIP CT image
- DM/PM · Sjögren · MCTD — three-column cards
- Ankylosing Spondylitis & Drug-Induced ILD
- Sarcoidosis — staging + CXR image + management
- ANCA Vasculitides (GPA, EGPA, Goodpasture)
- ACR/CHEST 2023 Screening Guidelines
- ACR/CHEST 2023 Treatment Guidelines
- ERS/EULAR 2026 + ATS 2024 + EULAR 2023 Guidelines
- Summary Table (9 diseases × 5 columns)
- Imaging Gallery (dark, 4-panel)
- References (9 citations with PMIDs)
YOU SKIPPED SOME SLIDES, S
Running Command
Writing File
Running Command
Your credits are exhausted. Your daily credits reset tomorrow, or you can purchase a top-up for more.
This is a shared conversation. Sign in to Orris to start your own chat.