Explain Difference between Tinea curies, incognito and vesicolor with images. Also prepare a poster with images with handwritten font.
Reading File
Finding Sources
Finding Sources
Finding Sources
Searching Images
Tinea cruris groin ringworm clinical appearance
Reading File
Reading File
Searching Images
Tinea incognito steroid modified ringworm skin lesion
Searching Images
Tinea versicolor pityriasis versicolor hypopigmented patches skin
Reading File
Reading File
Reading File
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Running Command
Running Command
Writing File
Running Command
Running Command
The poster is ready! Here's the full explanation followed by your download link.
Tinea Cruris vs Tinea Incognito vs Tinea Versicolor
1. 🔴 Tinea Cruris ("Jock Itch")
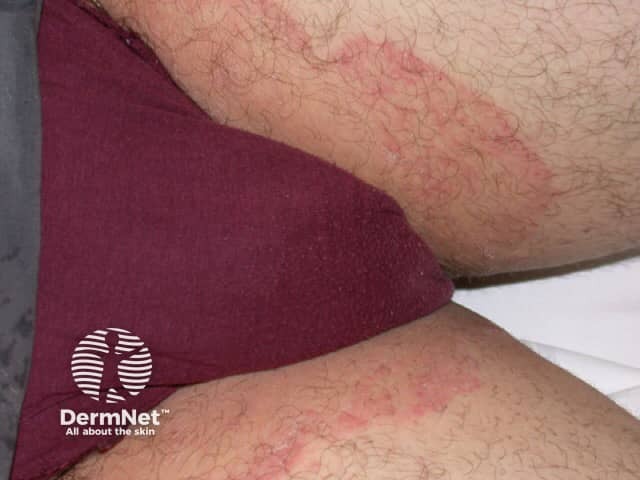
Organism: Dermatophyte fungi — Trichophyton rubrum (most common), T. mentagrophytes, Epidermophyton floccosum
Site: Groin, proximal medial thighs, extending to buttocks and lower abdomen. Scrotum is classically spared — important differential point.
Classic Appearance:
- Well-defined, annular (ring-shaped) erythematous plaque
- Raised scaly advancing border with central clearing
- Active pustules may appear within the border
- Symptoms: burning and pruritus
Why it happens: High ambient heat & humidity, tight/wet clothing, obesity, occlusion. Frequently co-exists with tinea pedis (check the feet as a source). More common in males.
Diagnosis & Treatment:
- KOH prep: branching hyphae
- First line: topical allylamines (terbinafine, naftifine) or topical azoles
- If spread beyond groin: oral fluconazole 150 mg weekly × 2–4 weeks
Source: Textbook of Family Medicine 9e; Fitzpatrick's Dermatology; Red Book 2021
2. 🟡 Tinea Incognito ("Steroid-Masked Tinea")
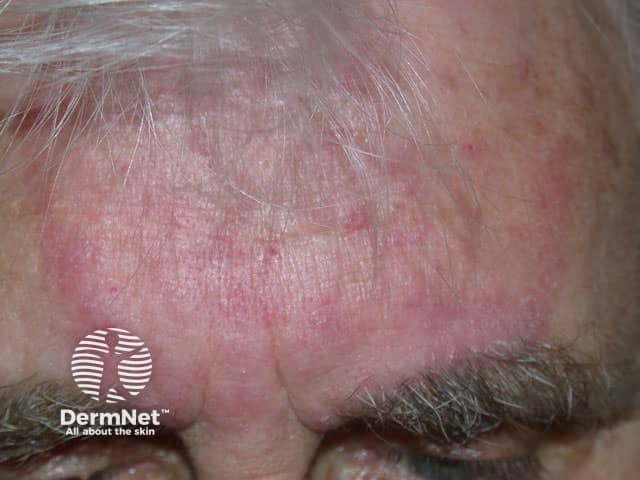
Tinea incognito is NOT a separate species. It is any tinea (usually tinea corporis/cruris) whose classic appearance has been obliterated by the incorrect application of topical corticosteroids.
Organism: Same as underlying tinea — most commonly T. rubrum
How It Happens: Topical steroids suppress the host inflammatory response → erythema fades, scaling border disappears → the classic "ringworm" ring is lost. The clinician is fooled into thinking the "dermatitis" is improving while the fungus actually proliferates.
Modified Appearance:
- Ill-defined, diffuse erythematous patch — no clear annular border
- Diminished scaling
- T. rubrum may produce concentric vesicular rings
- KOH still shows numerous hyphae despite the atypical look
Complication — Majocchi Granuloma: If fungi invade the hair shaft and dermis, a granulomatous dermal reaction forms, extending into subcutaneous fat. Requires systemic (not topical) antifungals.
Treatment:
- STOP topical corticosteroids immediately
- Topical or oral antifungals depending on extent
- Oral therapy mandatory for Majocchi granuloma
Source: Dermatology 5e (Elsevier); Fitzpatrick's Dermatology; Red Book 2021
3. 🔵 Tinea Versicolor ("Pityriasis Versicolor")
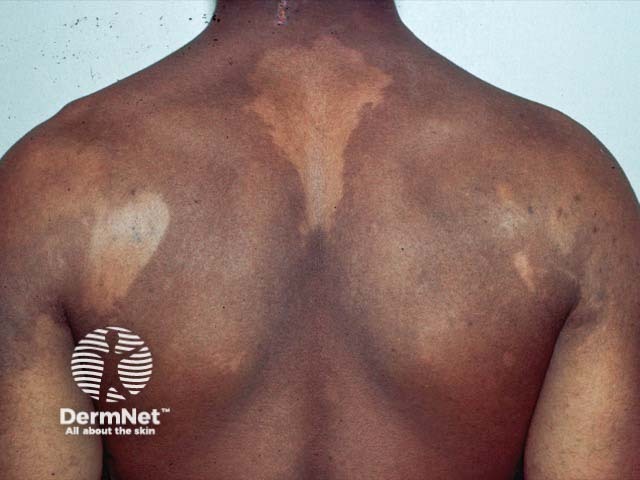
Critical distinction: Tinea versicolor is caused by a YEAST (Malassezia furfur), NOT a dermatophyte. The "tinea" name is a misnomer — it is more accurately called pityriasis versicolor.
Organism: Malassezia furfur (= Pityrosporum ovale) — a lipophilic dimorphic yeast that is normal cutaneous flora. It thrives on sebum.
Site: Sebaceous areas — chest, back, upper arms, abdomen in a characteristic "cape-like" distribution. Rarely face and proximal limbs.
Why the Colour Change? Malassezia produces azelaic acid which inhibits tyrosinase → blocks melanin synthesis → hypopigmentation. In lighter skin or inflamed states, lesions may appear hyperpigmented or pink-brown.
Clinical Appearance:
- Hypo- or hyperpigmented macules and patches
- "Versicolor" = varied colors (pink, tan, white, brown)
- Fine bran-like (pityriasiform) scale — "pityriasis" comes from Greek for "bran"
- Usually asymptomatic; mild pruritus in some
Diagnosis:
- KOH prep: classic "spaghetti and meatballs" pattern — short hyphae ("spaghetti") + clustered round yeast cells ("meatballs")
- Wood's lamp: yellow-green fluorescence
Treatment:
- Selenium sulfide 2.5% lotion/shampoo daily × 1 week
- Ketoconazole 2% shampoo daily × 3 days
- Single oral dose of fluconazole or ketoconazole 400 mg
- Prophylaxis: oral itraconazole 200 mg BID × 1 day/month
Source: Textbook of Family Medicine 9e; Rosen's Emergency Medicine; Henry's Clinical Pathology
Quick Comparison Table
| Feature | Tinea Cruris | Tinea Incognito | Tinea Versicolor |
|---|---|---|---|
| Organism | Dermatophyte (T. rubrum) | Dermatophyte (T. rubrum) | Yeast (Malassezia furfur) |
| Site | Groin (scrotum spared) | Any tinea site | Chest/back/arms ("cape") |
| Morphology | Annular, scaly, well-defined | Ill-defined, no ring | Hypo/hyperpigmented macules |
| Atypical cause | — | Topical steroid misuse | Normal yeast overgrowth |
| KOH | Hyphae | Numerous hyphae | "Spaghetti & meatballs" |
| Wood's Lamp | Negative | Negative | Yellow-green fluorescence |
| Treatment | Topical azole/allylamine | Stop steroid + antifungal | Selenium sulfide / azoles |
📥 Download Your Poster
The 5-slide poster (title + 3 detailed condition slides + comparison table), styled with Segoe Print handwritten font, dark navy background, clinical images, and color-coded panels:
Tinea Comparison Poster
Presentation · PPTX
This is a shared conversation. Sign in to Orris to start your own chat.