20 marks answer on blood aqueous barrier
Reading File
Finding Sources
Finding Sources
Reading File
Finding Sources
Finding Sources
Reading File
Finding Sources
Finding Sources
Reading File
Finding Sources
Reading File
Reading File
Loading Image
Reading File
Finding Sources
Reading File
Loading Image
I now have comprehensive textbook content. Let me compose the 20-mark answer.
Blood–Aqueous Barrier (BAB)
1. Introduction and Definition
The blood–aqueous barrier (BAB) is a physiological barrier that separates the blood circulating in the uveal vasculature from the aqueous humor filling the anterior and posterior chambers of the eye. It is a component of the broader blood–ocular barrier, which also includes the blood–retinal barrier. The BAB maintains the unique biochemical microenvironment of the aqueous humor — essential for the transparency and nutrition of the avascular cornea and lens — and confers immune privilege upon the anterior segment of the eye.
2. Anatomy and Components
The BAB has two anatomical components, corresponding to two separate tissue boundaries:
A. Anterior BAB — Iris Blood Vessels
The iris stroma is richly vascularised, but the endothelial cells of iris blood vessels are joined by continuous tight junctions (zonulae occludentes). This non-fenestrated endothelium prevents free passage of plasma proteins and large molecules from the blood into the posterior chamber. This differs from most peripheral capillaries, where the endothelium is fenestrated or loosely joined. The iris also lacks lymphatics in its stroma. Additionally, cells lining the anterior chamber (iris epithelium, corneal endothelium) constitutively express FAS ligand and PD-L1, which suppress immune-cell activation — reinforcing immune privilege at the tissue level.
B. Posterior BAB — Non-Pigmented Ciliary Epithelium (NPCE)
This is the primary structural component of the BAB. The ciliary body is covered by a double layer of cuboidal epithelial cells derived from the two layers of the embryonic optic cup:
| Layer | Position | Pigment | Key Feature |
|---|---|---|---|
| Pigmented epithelium (PE) | Outer, adjacent to stroma | Heavily pigmented | Basal lamina faces stroma; continuation of RPE |
| Non-pigmented epithelium (NE) | Inner, facing posterior chamber | Non-pigmented | Basal lamina faces posterior chamber; site of tight junctions |
The histological appearance of these layers is shown below:
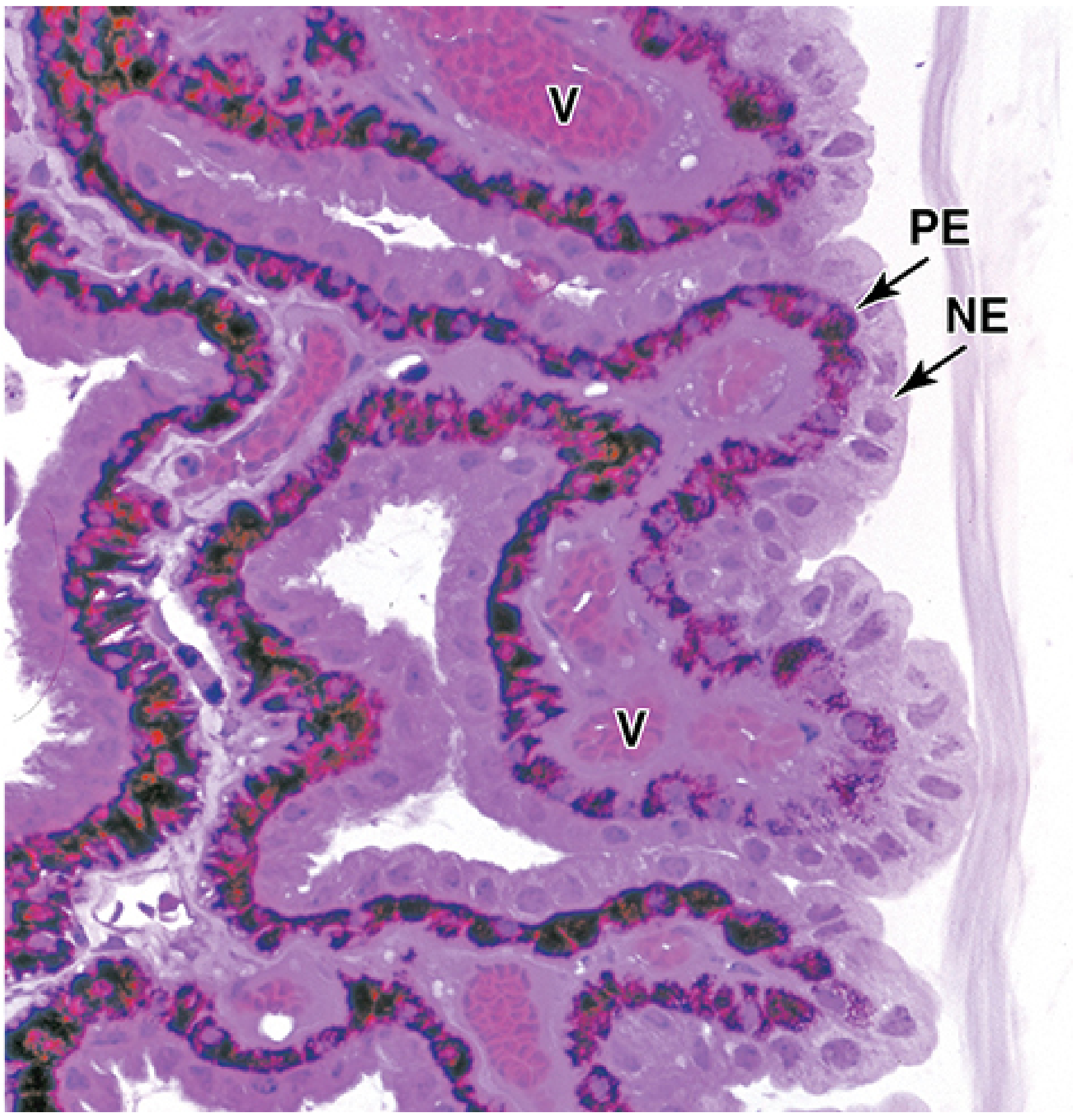
Histology of ciliary processes — pigmented epithelium (PE) and non-pigmented epithelium (NE) forming the bilaminar cover. V = stromal vessels. (Junqueira's Basic Histology, 17e)
Tight junctions (zonulae occludentes) between the NPCE cells are the structural basis of the posterior BAB. These junctions restrict free diffusion across the ciliary epithelium and prevent plasma proteins from entering the aqueous humor. The NPCE cells display features of active fluid-transporting epithelia:
- Complex cell-to-cell junctions with well-developed zonula occludens
- Extensive lateral and basal plications (infoldings)
- Na⁺/K⁺-ATPase concentrated in the lateral plasma membrane
- Elaborate rER and Golgi complex (for zonular fiber secretion)
The pigmented epithelial layer has a less developed junctional zone with irregular lateral intercellular spaces. Apical surfaces of the two layers are connected by both desmosomes and gap junctions, creating discontinuous "ciliary channels" — the actual conduits through which fluid is secreted.
— Histology: A Text and Atlas, p. 2396–2397
3. Aqueous Humor Formation and Its Relationship to the BAB
Aqueous humor originates from blood plasma in the stromal capillaries of the ciliary processes and is secreted by the NPCE into the posterior chamber.
Composition:
- Ionic composition similar to plasma
- Protein content < 0.1% (compared to ~7% in plasma) — maintained by the BAB
- Contains immunosuppressive molecules: TGF-β, neuropeptides (α-melanocyte-stimulating hormone, vasoactive intestinal peptide, somatostatin), and indolamine 2,3-dioxygenase (IDO)
Flow pathway (illustrated below):
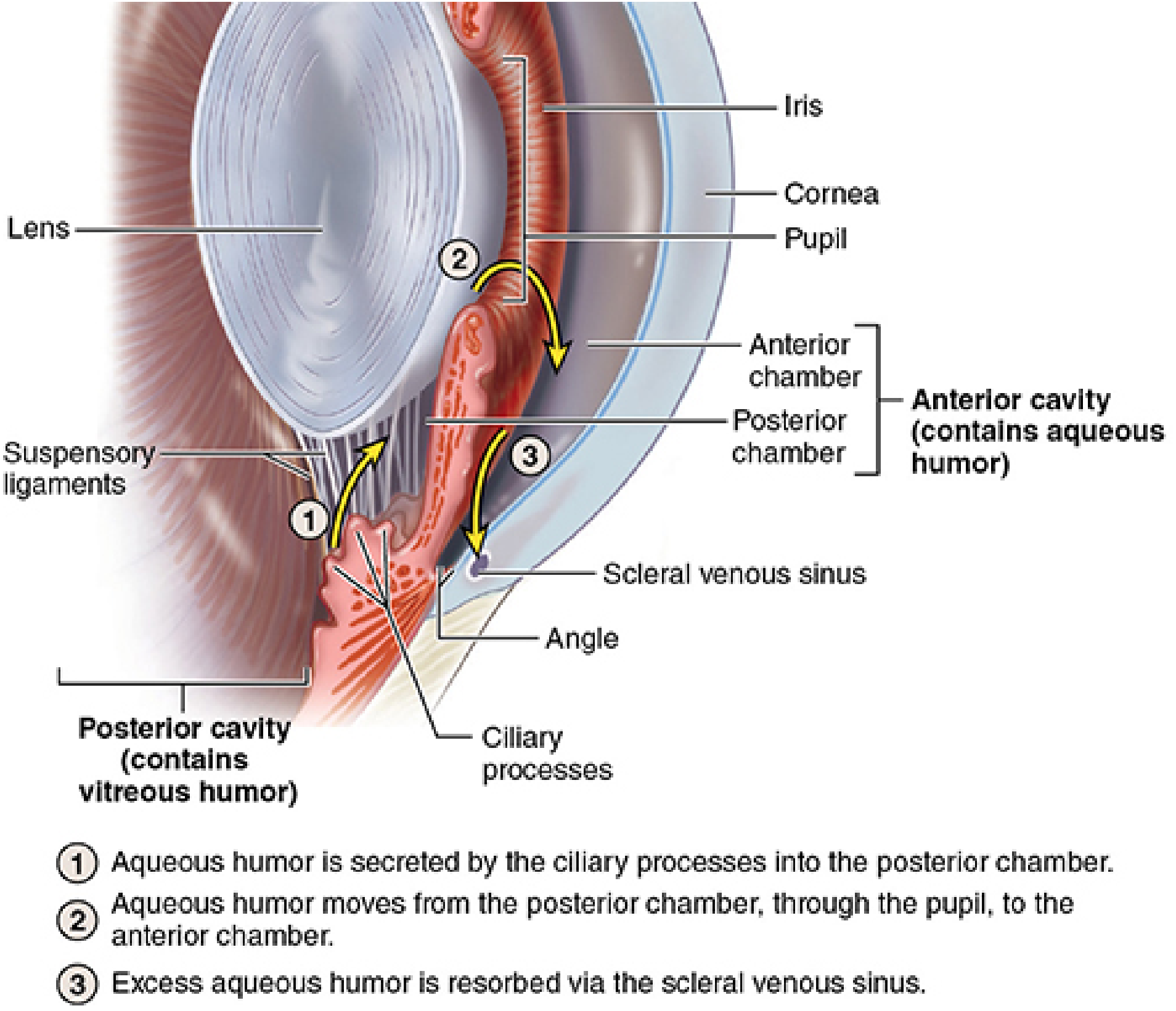
Aqueous humor circulation. (Junqueira's Basic Histology, 17e)
Normal turnover of aqueous humor is approximately once every 1.5–2 hours. Normal intraocular pressure is maintained at 10–21 mmHg by the balance between production and drainage.
Mechanisms of secretion:
- Active secretion — dominant mechanism; driven by Na⁺/K⁺-ATPase and carbonic anhydrase in NPCE; produces an osmotic gradient drawing water from stroma to posterior chamber
- Ultrafiltration — passive movement driven by hydrostatic pressure gradient
- Diffusion — minor contribution for lipid-soluble substances
— Junqueira's Basic Histology, 17e, p. 1186
4. Functions of the Blood–Aqueous Barrier
- Maintains low protein content of aqueous humor → preserves optical clarity of the anterior segment
- Nutrition of avascular tissues — delivers glucose, amino acids, and O₂ to the cornea and lens; removes metabolic wastes (CO₂, lactate)
- Regulation of intraocular pressure (IOP) — by controlling the volume and composition of aqueous humor
- Immune privilege — the tight junctions, immunosuppressive milieu of aqueous humor, and FAS-L/PD-L1 expression on anterior chamber cells together prevent destructive immune responses that could opacify the cornea or lens
- Barrier against toxins and pathogens — limits entry of blood-borne substances into the optically critical anterior segment
5. Breakdown of the Blood–Aqueous Barrier
Causes
| Category | Examples |
|---|---|
| Inflammation / Uveitis | Anterior uveitis (AAU), HLA-B27-associated uveitis, Behçet disease |
| Trauma | Blunt injury, penetrating injury, surgical trauma (intraocular surgery) |
| Vascular diseases | Diabetic retinopathy, hypertensive changes |
| Infection | Endophthalmitis |
| Drugs / Pharmacologic | Miotics (e.g., pilocarpine) — increase permeability; prostaglandin analogues |
| Pseudoexfoliation syndrome | Mild BAB disruption causing aqueous flare |
Pathophysiology of breakdown
When the tight junctions are disrupted, plasma proteins (fibrinogen, albumin) and inflammatory cells leak from stromal capillaries across the ciliary epithelium and iris vessels into the posterior and anterior chambers. This produces:
- Aqueous flare — the Tyndall effect caused by protein-scattered light; graded at slit lamp (Table 12.3, Kanski's)
- Aqueous cells — inflammatory cells (lymphocytes, monocytes) — graded by SUN Working Group criteria in a 1×1 mm slit beam field
- Hypopyon — layered inflammatory cells in the inferior anterior chamber
- Keratic precipitates (KPs) — deposits of inflammatory cells on the corneal endothelium
- Fibrinous exudate in the anterior chamber
— Kanski's Clinical Ophthalmology, 10th ed.
Clinical assessment of barrier breakdown
- Slit-lamp biomicroscopy — gold standard; flare and cells quantified
- Laser flare photometry (LFP) — objective, quantitative measurement of aqueous protein concentration; more sensitive than clinical grading
- Swept-source anterior segment OCT — sensitive for visualising individual cells
6. Pharmacological Relevance
Several drug classes exploit or are affected by the BAB:
| Drug / Class | Mechanism / Relevance |
|---|---|
| Carbonic anhydrase inhibitors (acetazolamide, dorzolamide) | Block CA in NPCE → reduce HCO₃⁻ secretion → reduce aqueous production → lower IOP |
| Beta-blockers (timolol) | Reduce active secretion of aqueous humor |
| Miotics (pilocarpine) | Contraindicated in uveitic glaucoma — increase BAB permeability and worsen inflammation |
| Corticosteroids | Stabilise the BAB by reducing tight junction permeability and prostaglandin-mediated vasodilation |
| NSAIDs (topical) | Reduce prostaglandin-mediated BAB breakdown |
| Prostaglandin analogues (latanoprost) | Increase uveoscleral outflow but can mildly disrupt BAB |
— Kanski's Clinical Ophthalmology, 10th ed.; Lippincott Illustrated Reviews: Pharmacology
7. Immune Privilege and the BAB
The anterior chamber is an immune-privileged site, analogous to the brain and testis. The BAB contributes through:
- Structural isolation — tight junctions prevent antigen-presenting cell trafficking
- Aqueous humor immunosuppressive factors — TGF-β, α-MSH, VIP, somatostatin, IDO
- FAS-L and PD-L1 expression on iris/corneal endothelium → apoptosis of infiltrating T cells
- Anterior chamber-associated immune deviation (ACAID) — antigen placed in AC induces systemic immune tolerance
Failure of this privilege leads to sympathetic ophthalmia — trauma to one eye releases sequestered antigens, generating T-cell responses that attack both the injured and the contralateral eye.
— Cellular and Molecular Immunology, p. 940–941
8. Summary Table
| Feature | Anterior BAB | Posterior BAB |
|---|---|---|
| Site | Iris blood vessels | Non-pigmented ciliary epithelium |
| Structural basis | Tight junctions of endothelium | Tight junctions of NPCE (zonulae occludentes) |
| Primary function | Prevents plasma proteins entering from iris vasculature | Main barrier controlling aqueous humor composition |
| Key molecules | Junctional proteins (claudin, occludin, ZO-1) | Na⁺/K⁺-ATPase, carbonic anhydrase, junctional proteins |
| Clinical test of integrity | Laser flare photometry, slit-lamp flare | Same |
Key Points (for exam recall)
- BAB = anterior component (iris vessel endothelium) + posterior component (NPCE tight junctions)
- Tight junctions of the NPCE are the dominant structural element
- Aqueous humor: < 0.1% protein (vs 7% in plasma) — maintained by the BAB
- Breakdown → aqueous flare + cells → graded by slit lamp or laser flare photometry
- Causes: uveitis, trauma, surgery, vascular disease, miotics
- BAB underpins ocular immune privilege via structural and molecular mechanisms
Sources:
- Histology: A Text and Atlas, 8th ed. (Eroschenko) — pp. 2396–2397
- Junqueira's Basic Histology, 17th ed. — pp. 1185–1187
- Kanski's Clinical Ophthalmology, 10th ed. — Chapter 12 (Uveitis)
- Cellular and Molecular Immunology (Abbas et al.) — pp. 939–941
This is a shared conversation. Sign in to Orris to start your own chat.