Explain about oral cavity and salivary glands for anatomy of GI tract first year mbbs
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Finding Sources
Reading File
Reading File
Finding Sources
Loading Image
Loading Image
Reading File
Loading Image
Loading Image
I now have comprehensive content from Gray's Anatomy for Students and Junqueira's Basic Histology. Let me compile the complete answer:
Oral Cavity and Salivary Glands — Anatomy of the GI Tract
(Sources: Gray's Anatomy for Students; Junqueira's Basic Histology, 17e)
1. Overview of the Oral Cavity
The oral cavity is the inlet of the digestive system, inferior to the nasal cavities. It opens anteriorly onto the face through the oral fissure and is continuous posteriorly with the pharynx at the oropharyngeal isthmus.
Functions:
- Initial processing of food (mastication + salivary digestion)
- Speech — modulates sounds produced by the larynx
- Breathing — opens into the pharynx, a common air/food pathway
Boundaries
| Wall | Structure |
|---|---|
| Roof | Hard palate (anterior ¾) + Soft palate (posterior ¼) |
| Floor | Muscular diaphragm (mylohyoid) + Tongue |
| Lateral walls | Cheeks (buccinator muscle) |
| Anterior opening | Oral fissure (lips) |
| Posterior opening | Oropharyngeal isthmus |
Two Regions
The upper and lower dental arches divide the oral cavity into:
- Oral vestibule — horseshoe-shaped space between the teeth and the cheeks/lips
- Oral cavity proper — the space enclosed within the dental arches
2. Skeletal Framework
Key bones contributing to the oral cavity:
- Maxillae — palatine processes form the anterior ⅔ of the hard palate; alveolar processes carry the upper teeth
- Palatine bones — horizontal plates form the posterior ⅓ of the hard palate; transmit the greater palatine nerve and vessels via the greater palatine foramen and lesser palatine nerve via the lesser palatine foramen
- Mandible — carries the lower teeth; articulates at the temporomandibular joint
- Sphenoid — pterygoid processes anchor soft palate muscles
- Hyoid bone — provides attachment for tongue muscles
3. The Palate
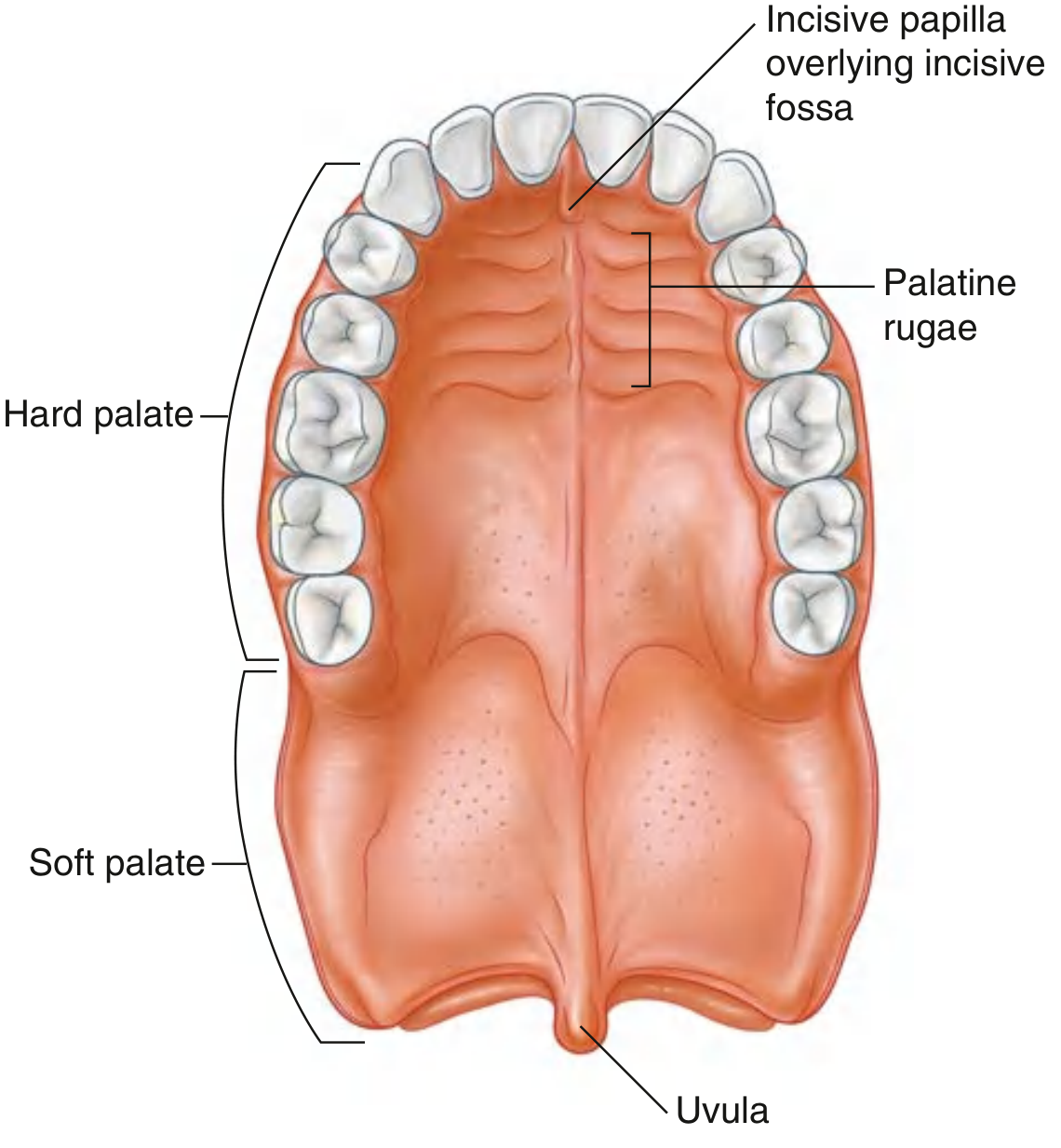
Gray's Anatomy for Students, Fig. 8.272 — Palate
Hard Palate
- Formed anteriorly by the palatine processes of the maxillae (anterior ¾) and posteriorly by the horizontal plates of the palatine bones (posterior ¼)
- Mucosa bears transverse palatine rugae and a median palatine raphe ending in the incisive papilla anteriorly
Soft Palate
- Continues posteriorly from the hard palate as a movable fibromuscular flap
- Elevated → separates nasopharynx from oropharynx (during swallowing)
- Depressed → closes the oropharyngeal isthmus
- Has a pendant projection posteriorly — the uvula
Five Muscles of the Soft Palate
| Muscle | Action | Nerve |
|---|---|---|
| Tensor veli palatini | Tenses palate; opens auditory tube | Mandibular nerve [V3] |
| Levator veli palatini | Elevates soft palate | Vagus [X] |
| Palatoglossus | Depresses palate / elevates tongue | Vagus [X] |
| Palatopharyngeus | Elevates pharynx; closes isthmus | Vagus [X] |
| Musculus uvulae | Shortens/elevates uvula | Vagus [X] |
Key rule: All soft palate muscles are innervated by vagus nerve [X], EXCEPT tensor veli palatini (→ V3).
4. The Tongue
The tongue is a muscular structure forming part of the floor of the oral cavity and the anterior wall of the oropharynx.
Surfaces
- Oral (anterior ⅔) — lies in the horizontal plane; bears papillae
- Pharyngeal (posterior ⅓) — curves inferiorly; bears lymphoid nodules (lingual tonsil)
- Separated by the V-shaped terminal sulcus, at whose apex is the foramen cecum (embryological origin of the thyroid gland)
Papillae (on the dorsal/oral surface)
| Type | Description | Taste buds |
|---|---|---|
| Filiform | Numerous, cone-shaped, no taste buds | ✗ |
| Fungiform | Mushroom-shaped, along lateral margins | ✓ |
| Vallate (Circumvallate) | Largest; ~8–12 in a V-line anterior to terminal sulcus | ✓ |
| Foliate | Linear mucosal folds on sides of tongue | ✓ |
Inferior Surface
- Frenulum of tongue — median mucosal fold; tethers tongue to floor of mouth
- Lingual veins visible on either side
- Fimbriated folds lateral to the veins
Muscles of the Tongue
Intrinsic muscles (entirely within the tongue; change shape):
- Superior/inferior longitudinal, transverse, and vertical
Extrinsic muscles (attach tongue to external structures; change position):
| Muscle | Origin | Action |
|---|---|---|
| Genioglossus | Mandible (mental spine) | Protrudes tongue |
| Hyoglossus | Hyoid bone | Depresses and retracts |
| Styloglossus | Styloid process | Retracts and elevates |
| Palatoglossus | Soft palate | Elevates posterior tongue |
Key rule: All tongue muscles are innervated by hypoglossal nerve [XII], EXCEPT palatoglossus (→ vagus [X]).
Innervation Summary
| Region | Sensation | Taste |
|---|---|---|
| Anterior ⅔ | Lingual nerve (V3) | Chorda tympani (VII) |
| Posterior ⅓ | Glossopharyngeal nerve [IX] | Glossopharyngeal nerve [IX] |
| Epiglottic region | Internal laryngeal branch of vagus [X] | Vagus [X] |
5. Innervation of the Oral Cavity
General sensory innervation is by branches of the trigeminal nerve [V]:
- Upper parts (palate, upper teeth) → Maxillary nerve [V2]
- Lower parts (lower teeth, floor, anterior tongue) → Mandibular nerve [V3]
Taste from the anterior ⅔ of tongue → facial nerve [VII] (via chorda tympani branch)
Parasympathetic (secretomotor) to glands → facial nerve [VII] (distributed via V branches) — except the parotid, which receives parasympathetics via glossopharyngeal nerve [IX]
6. Salivary Glands
Salivary glands open into the oral cavity. There are:
- Numerous small minor glands in the submucosa (lips, palate, tongue, cheeks) — contribute ~10% of total saliva
- Three major paired glands — contribute ~90% of saliva
Together they produce 0.75–1.5 L of saliva per day.
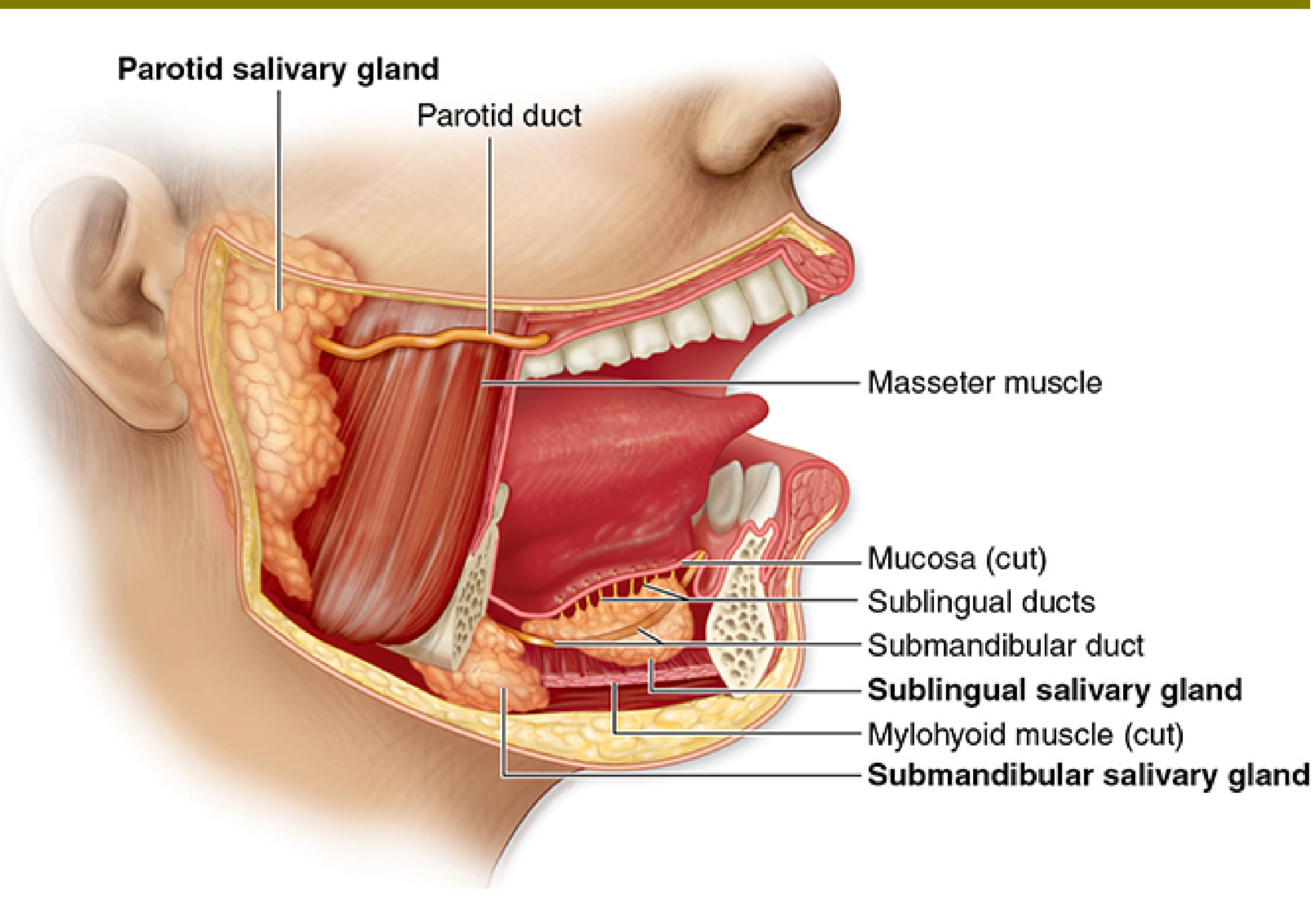
Junqueira's Basic Histology, Fig. 16–1 — Major Salivary Glands
6.1 Parotid Gland
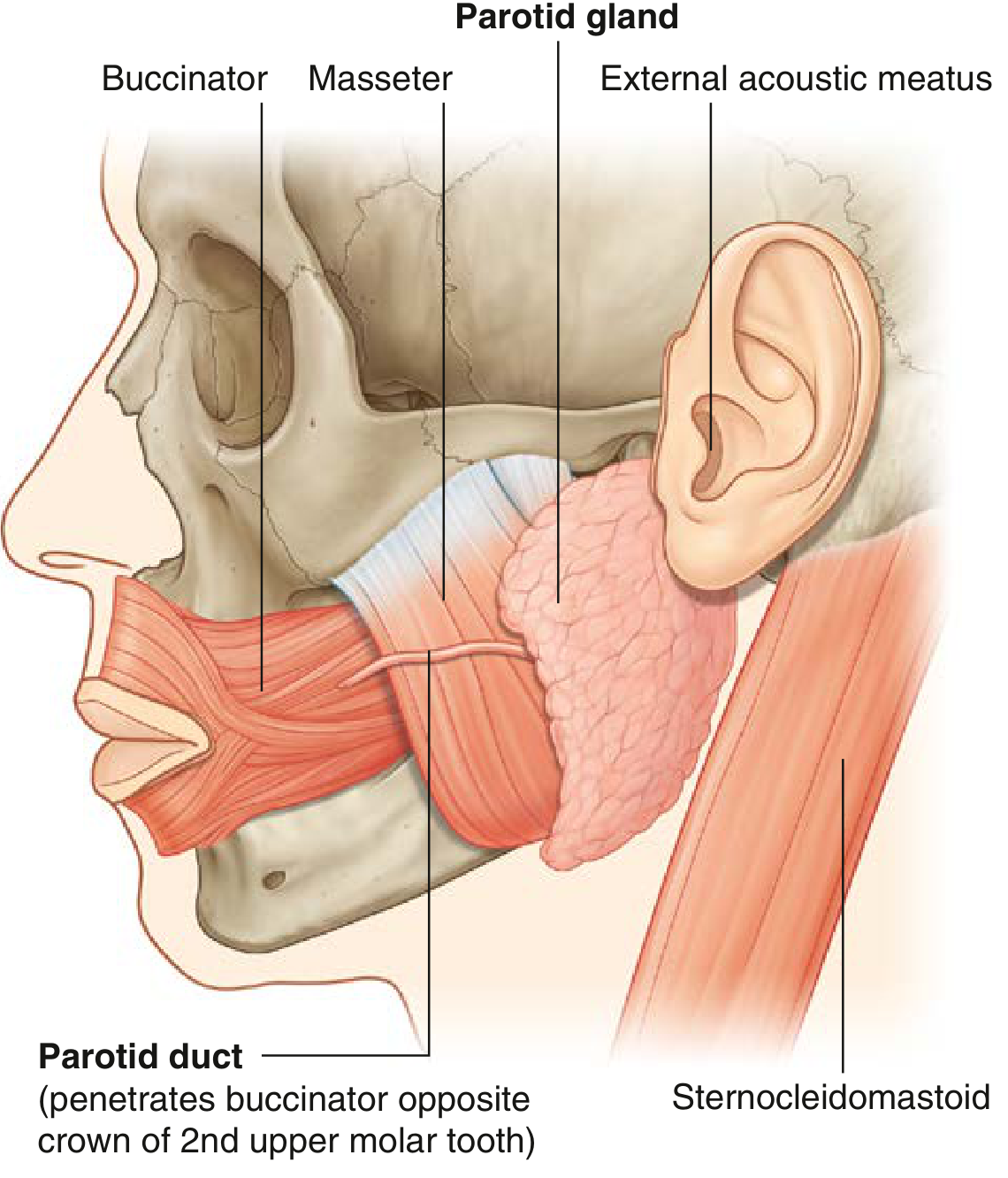
Gray's Anatomy for Students, Fig. 8.267 — Parotid Gland
- Largest of the three major salivary glands
- Lies in a triangular trench bounded by:
- Behind — sternocleidomastoid muscle
- In front — ramus of mandible
- Above — external acoustic meatus + zygomatic arch
- Extends anteriorly over the masseter muscle
- Parotid duct (Stensen's duct) passes anteriorly over masseter, turns medially to penetrate buccinator, and opens into the oral vestibule opposite the crown of the 2nd upper molar tooth
- Encloses: external carotid artery, retromandibular vein, and facial nerve [VII] (important surgical landmark)
- Secretion: Purely serous (watery, enzyme-rich)
- Blood supply: External carotid artery and branches
- Venous drainage: External jugular vein
- Lymphatics: Parotid nodes → superficial and deep cervical nodes
- Parasympathetic innervation: Glossopharyngeal nerve [IX] → lesser petrosal nerve → otic ganglion → auriculotemporal nerve (V3) → parotid gland
6.2 Submandibular Gland
- Hook-shaped (intermediate in size; smaller than parotid, larger than sublingual)
- Superficial (larger) part — lies in the submandibular triangle, against the submandibular fossa of the mandible, inferior to the mylohyoid line and below the mylohyoid muscle
- Deep (smaller) part — loops around the posterior margin of mylohyoid to lie in the floor of the oral cavity, lateral to the root of the tongue on the hyoglossus muscle
- Submandibular duct (Wharton's duct) emerges from the deep part and opens on the sublingual caruncle (papilla) beside the base of the frenulum of the tongue
- The lingual nerve loops under and around the submandibular duct (crosses its lateral then medial side)
- Secretion: Seromucous (mixed serous + mucous)
- Blood supply: Facial and lingual arteries
- Venous drainage: Lingual and facial veins
- Lymphatics: Submandibular nodes → deep cervical nodes (especially jugulo-omohyoid node)
- Parasympathetic innervation: Facial nerve [VII] → chorda tympani → lingual nerve → submandibular ganglion → postganglionic fibers to gland
6.3 Sublingual Gland
- Smallest of the three paired major salivary glands
- Almond-shaped; lies in the floor of the oral cavity, immediately lateral to the submandibular duct and lingual nerve
- Lies against the medial surface of mandible (sublingual fossa, above the anterior ⅓ of mylohyoid line)
- Its superior margin raises the sublingual fold of mucosa, running from the posterolateral floor to the sublingual caruncle anteriorly
- Drainage: Via numerous minor sublingual ducts opening onto the sublingual fold; occasionally a major sublingual duct joins the submandibular duct at the sublingual caruncle
- Secretion: Predominantly mucous
- Blood supply: Facial and lingual arteries
- Venous drainage: Lingual and facial veins
- Lymphatics: Submandibular nodes → deep cervical nodes
- Parasympathetic innervation: Same pathway as submandibular — chorda tympani → submandibular ganglion
Summary Table — Three Major Salivary Glands
| Feature | Parotid | Submandibular | Sublingual |
|---|---|---|---|
| Size | Largest | Intermediate | Smallest |
| Location | Preauricular; outside oral cavity | Submandibular triangle + floor of mouth | Floor of oral cavity |
| Duct | Stensen's duct | Wharton's duct | Multiple minor ducts (± major) |
| Duct opening | Opposite 2nd upper molar | Sublingual caruncle | Sublingual fold |
| Secretion type | Serous | Seromucous | Mucous |
| Parasympathetic | CN IX → otic ganglion → auriculotemporal (V3) | CN VII → chorda tympani → submandibular ganglion | CN VII → chorda tympani → submandibular ganglion |
| Contents enclosed | ECA, retromandibular vein, CN VII | — | — |
7. Parasympathetic Innervation of Salivary Glands (High-Yield)
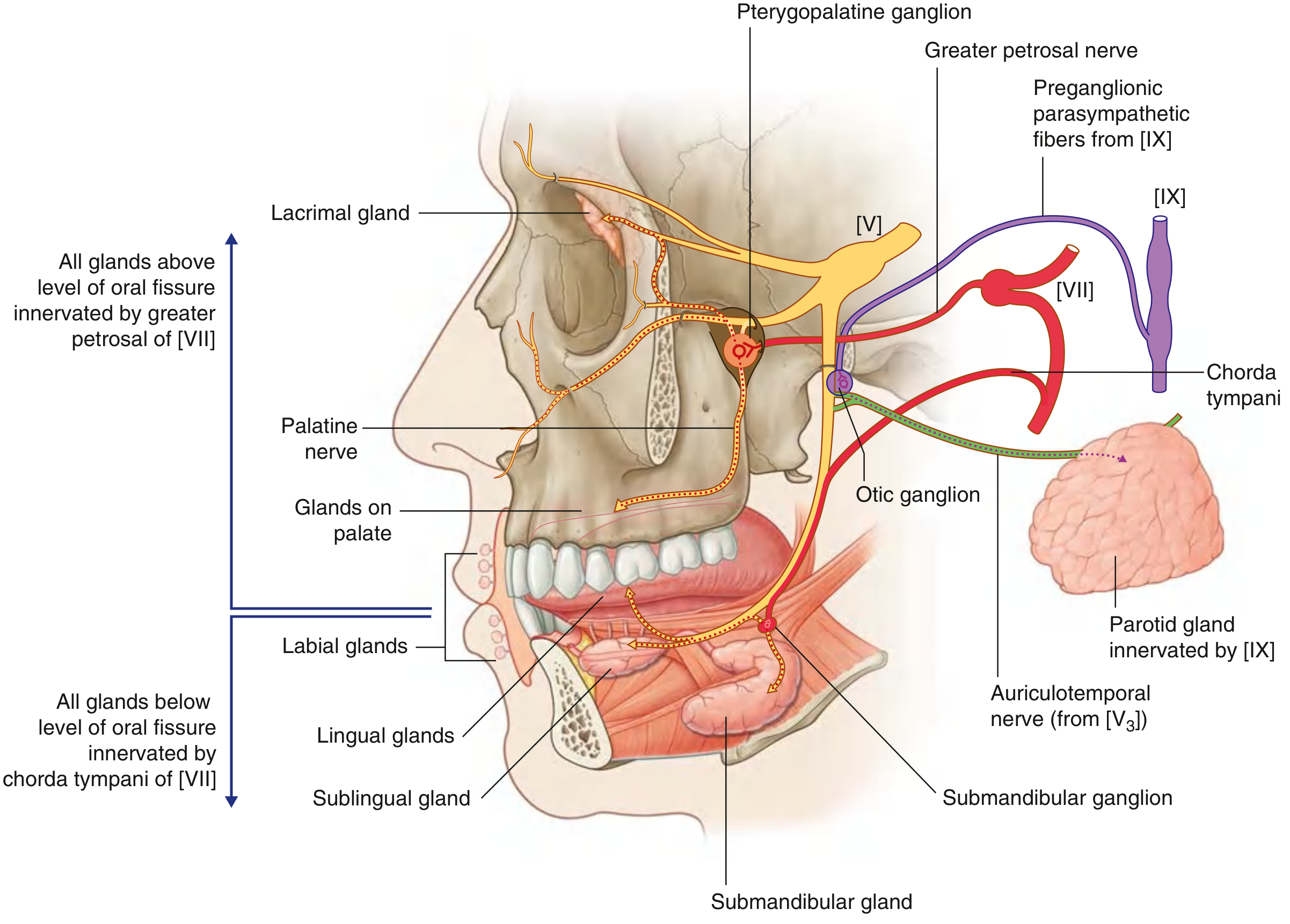
Gray's Anatomy for Students, Fig. 8.269 — Summary of Parasympathetic Innervation of Glands in the Head
Key rule to remember:
- All glands above the level of the oral fissure → innervated by greater petrosal nerve (branch of CN VII) → pterygopalatine ganglion
- All glands below the level of the oral fissure (submandibular, sublingual, lingual minor glands) → innervated by chorda tympani (branch of CN VII) → submandibular ganglion
- Parotid gland (exception) → innervated by CN IX → lesser petrosal nerve → otic ganglion → auriculotemporal nerve
8. Histology of Salivary Glands (Junqueira's)
Three epithelial cell types in secretory units:
- Serous cells — pyramidal; round nuclei; prominent RER; apical secretory granules; form spherical acini with a small central lumen; secrete enzymes (e.g., amylase) and proteins
- Mucous cells — flattened/basal nuclei; condensed chromatin; pale cytoplasm; form tubuloacinar units; produce mucin glycoproteins
- Myoepithelial cells — lie between secretory cells and their basal lamina; contraction expels secretion into ducts
Mixed units: "Serous demilunes" — clusters of serous cells capping mucous tubules
Duct system:
- Intercalated ducts → low cuboidal epithelium
- Striated ducts → columnar cells with basal infoldings and mitochondria (for ion transport, modify saliva electrolytes)
- Excretory ducts → pseudostratified or stratified epithelium
Clinical note: Xerostomia (dry mouth) results from decreased salivary production — causes include mumps (parotitis), radiation therapy to the head and neck, and drugs such as antihistamines and anticholinergics.
Sources: Gray's Anatomy for Students, p. 1227–1246; Junqueira's Basic Histology — Text and Atlas, 17e, p. 809–810
This is a shared conversation. Sign in to Orris to start your own chat.