Malnutrition
Reading File
Asking for Preferences
Finding Sources
Searching PubMed
"malnutrition"[MeSH Terms] AND "diagnosis"[MeSH Terms]
Searching the Web
malnutrition types causes clinical features management 2024 overview
Reading File
Reading File
Finding Sources
Searching Images
kwashiorkor marasmus malnutrition clinical features children
Reading File
Reading File
Reading File
Reading File
Reading File
I now have all the information needed for a comprehensive answer. Let me compile it.
Malnutrition
Definition
Malnutrition describes a deficiency, excess, or imbalance of energy and/or nutrients resulting in measurable adverse effects on body composition, function, and clinical outcomes. It encompasses both undernutrition and overnutrition (including obesity and diet-related non-communicable diseases).
Classification
1. Primary vs Secondary
| Type | Mechanism |
|---|---|
| Primary | One or more dietary components are absent from the diet |
| Secondary (conditional) | Dietary intake is adequate but malnutrition results from malabsorption, impaired storage, excess losses, or increased requirements (e.g., GI disease, cachexia, critical illness) |
2. WHO Categories of Malnutrition
- Wasting — low weight-for-height (acute undernutrition)
- Stunting — low height-for-age (chronic undernutrition)
- Underweight — low weight-for-age
- Micronutrient deficiency — inadequate vitamins/minerals
- Overweight/obesity — excess caloric intake
- Diet-related NCDs — cardiovascular disease, diabetes, cancers
Severe Acute Malnutrition (SAM)
Previously called protein-energy malnutrition (PEM). The WHO defines SAM as weight-to-height ratio ≥3 SD below the median, visible wasting, or nutritional edema.
~50 million children worldwide are affected; 45% of deaths in children under 5 in low-resource countries are attributable to undernutrition.
SAM exists on a spectrum between two poles:
Marasmus (Calorie Deficiency)
- Severe deficiency of both calories and protein
- The somatic protein compartment (skeletal muscle) is depleted; the visceral compartment is relatively spared
- Serum albumin is normal or near-normal
- Body adapts by catabolizing muscle → amino acids used as fuel
- Subcutaneous fat is also mobilized
- Clinical features: severe emaciation, "skin and bones" appearance, "old man face," large head relative to body, "baggy pants" skin on limbs, concurrent vitamin deficiencies, immune deficiency (especially T-cell), anemia
Kwashiorkor (Protein Deficiency)
- Protein deprivation is relatively greater than caloric deficit
- Classically seen in children weaned early onto a carbohydrate-only diet
- The visceral protein compartment is severely depleted → hypoalbuminemia → edema
- Clinical features:
- Bilateral peripheral edema (starts in dependent areas, ascends)
- "Flaky paint" skin depigmentation with areas of breakdown
- Pale, reddish-yellow ("flag sign") hair
- Enlarged, fatty liver (impaired lipoprotein synthesis)
- Apathy, listlessness, anorexia
- Distended abdomen
- NO ascites typically (unlike hepatic disease)
Marasmic-Kwashiorkor
Mixed features of both; the most severe form.
Key Distinguishing Features:
| Feature | Marasmus | Kwashiorkor |
|---|---|---|
| Protein compartment depleted | Somatic (muscle) | Visceral (liver) |
| Edema | Absent | Present (bilateral) |
| Serum albumin | Normal/near-normal | Low |
| Liver | Normal | Enlarged, fatty |
| Body fat | Severely depleted | Less depleted |
| Skin changes | Minimal | "Flaky paint" dermatosis |
Clinical Images
Marasmus vs. Kwashiorkor comparison:
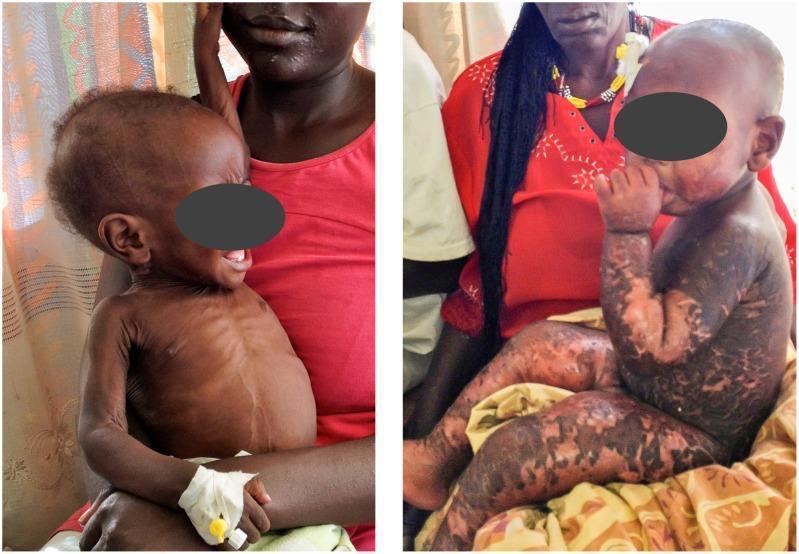
Kwashiorkor skin changes (flaky paint dermatosis) and edema:
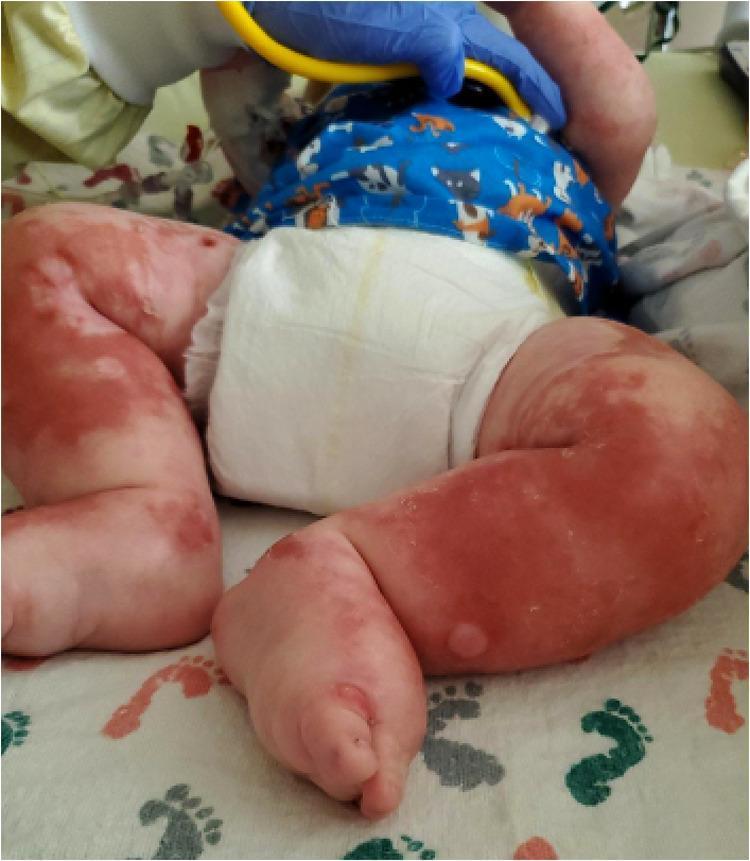
Pathophysiology of Starvation
Within days of starvation:
- Fat replaces glucose as the primary fuel; ketosis develops rapidly
- BMR declines → hypothermia and fatigue
- Cortisol ↑, insulin ↓, thyroid hormone ↓
- Prolonged starvation → near-complete fat depletion, muscle mass cut by ~half
- Hypokalemia → rapid muscle fatigue, cardiac arrhythmia (major cause of death in anorexia nervosa)
- Cardiac: bradycardia, ↓ stroke volume, hypotension
- Pulmonary: decreased respiratory muscle mass, electrolyte disturbances
- GI: villous atrophy, blunted microvilli, disaccharidase deficiency (esp. lactase), impaired pancreatic/biliary secretion → complicates refeeding
- Immune: lymphoid atrophy, impaired cell-mediated immunity → opportunistic infections
- Bone marrow: hypoplasia → anemia (microcytic if Fe-deficient; mixed if folate co-deficient)
- Brain: cerebral atrophy in infants; delayed cognitive development with lifelong consequences
Common Causes
| Category | Examples |
|---|---|
| Poverty | Famine, war, displacement, crop failure |
| Ignorance | Unrecognized increased needs (infants, pregnancy, elderly) |
| Chronic alcohol use | Deficiencies in thiamine, pyridoxine, folate, vitamin A |
| Acute/chronic illness | Burns (BMR doubles), AIDS, TB, cancer cachexia |
| Eating disorders | Anorexia nervosa, bulimia nervosa |
| GI disease | Malabsorption syndromes, IBD, short bowel syndrome |
| Medications | Chemotherapy, glucocorticoids, certain antibiotics |
Diagnosis
Anthropometric Measurements
- Mid-upper arm circumference (MUAC): most practical field tool for children 6–59 months and pregnant women
- Weight-for-height Z-score (WHZ): wasting if ≥2 SD below median; SAM if ≥3 SD
- Height-for-age Z-score (HAZ): stunting if ≥2 SD below median
- BMI: <18.5 kg/m² = moderate secondary malnutrition; <15 kg/m² = severe
Laboratory
- Serum albumin and prealbumin — useful for visceral protein compartment assessment but are acute-phase reactants and non-specific
- Transferrin levels
- Skinfold thickness (subcutaneous fat stores)
- Mid-arm circumference (somatic muscle mass)
- Note: No single reliable lab test; grip strength is the best single clinical measure in secondary malnutrition
Differential Diagnosis of Edema in Kwashiorkor
Cardiac disease, nephrotic syndrome, hepatic cirrhosis, severe anemia, TB — but in endemic, impoverished settings, kwashiorkor remains the leading diagnosis.
Treatment
Uncomplicated SAM (Outpatient)
- Ready-to-use therapeutic food (RUTF): fortified peanut paste (~30 g under directly observed therapy)
- Empiric oral antibiotics (1 week) — shown to decrease mortality, improve nutritional recovery, reduce hospitalization
- Community-based programs have superior outcomes to inpatient care; this is now the international standard of care
Complicated SAM (Inpatient)
Indicated when: anorexia, severe infection, hypoglycemia, hypothermia, severe dehydration, or RUTF unavailable
WHO 10-Step approach:
- Treat/prevent hypoglycemia
- Treat/prevent hypothermia
- Treat/prevent dehydration
- Correct electrolyte imbalances
- Treat/prevent infection
- Correct micronutrient deficiencies
- Cautious initial feeding (F-75 formula — 75 kcal/100 mL)
- Transition to catch-up growth (F-100 formula — 100 kcal/100 mL)
- Sensory stimulation and emotional support
- Prepare for follow-up
Caution — Refeeding syndrome: Rapid reintroduction of carbohydrates can precipitate severe hypophosphatemia, hypokalemia, and hypomagnesemia → cardiac arrhythmia and death. Start feeds slowly.
Lactose intolerance in kwashiorkor: Intestinal mucosal atrophy causes disaccharidase (lactase) deficiency; avoid full-strength milk-based formulas initially — these changes are reversible with treatment.
Stunting
- Limited reversibility once established (first 1000 days are critical)
- Improved dietary quality/diversity (complete protein), immunizations, vitamin A supplementation, deworming, HIV testing, improved sanitation
Secondary Malnutrition
- Treat underlying disease
- Nutritional rehabilitation in parallel with treatment of primary illness
- Wound healing is impaired with albumin <2.0 g/dL; protein supplements can reverse this
Consequences
- Increased susceptibility to infection (immunodeficiency)
- Impaired wound healing and surgical risk
- Cardiac arrhythmia and sudden death (hypokalemia)
- Cerebral atrophy, cognitive impairment
- Growth failure — physical and mental
- Metabolic syndrome and obesity paradox in adult survivors of childhood malnutrition
- Increased healthcare costs and readmission rates
Key Numbers (WHO, 2022)
- 149 million children under 5 are stunted
- 45 million are wasted
- 37 million are overweight/obese
- 2.5 billion adults are overweight; 890 million are obese
- 390 million adults are underweight
Sources: Robbins & Kumar Basic Pathology (10th ed.), Goldman-Cecil Medicine (International Edition), Robbins, Cotran & Kumar Pathologic Basis of Disease; WHO Malnutrition Fact Sheet; ASPEN oncology malnutrition screening systematic review (PMID 39412097, 2024)
This is a shared conversation. Sign in to Orris to start your own chat.