Acute bronchiolitis refer to nelson and op ghai
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Searching PubMed
"bronchiolitis" AND "management" AND "infant"
Reading File
Searching Images
acute bronchiolitis RSV chest X-ray infant
Reading File
I now have comprehensive material. Let me compile the full answer based on Nelson's Textbook of Pediatrics and OP Ghai's Essential Pediatrics content from my training knowledge, supplemented by the library sources and recent evidence.
Acute Bronchiolitis
(as per Nelson's Textbook of Pediatrics & OP Ghai's Essential Pediatrics)
Definition
Acute bronchiolitis is an acute inflammatory disease of the lower respiratory tract characterized by obstruction of the small airways (bronchioles), occurring predominantly in children < 2 years of age (peak: 2–6 months). It is the most common cause of hospitalization in infants.
Etiology
| Virus | Frequency |
|---|---|
| RSV (Respiratory Syncytial Virus) | ~70% — most common |
| Human Metapneumovirus (hMPV) | 2nd most common |
| Parainfluenza virus (types 1, 2, 3) | Common |
| Influenza virus | Less common |
| Adenovirus | Less common |
| Rhinovirus, Bocavirus | Occasional |
RSV causes epidemic bronchiolitis — seasonal outbreaks from November to April (in temperate climates). It has two antigenic subtypes: A and B.
Pathophysiology
(Nelson's)
- Viral replication begins in the upper airway epithelium, then spreads to the lower respiratory tract
- Bronchiolar epithelial necrosis and sloughing → mucosal edema + submucosal infiltrate (lymphocytes, plasma cells)
- Peribronchiolar inflammation and increased mucus secretion
- Partial or complete obstruction of small airways → air trapping and hyperinflation
- Ball-valve mechanism: air enters during inspiration (airways slightly dilate) but is trapped during expiration (airways collapse) → emphysema or atelectasis
- V/Q mismatch → hypoxemia; CO₂ retention in severe cases
The infant's bronchioles are especially vulnerable — small caliber means even mild mucosal swelling causes significant resistance (resistance ∝ 1/r⁴).
Epidemiology & Risk Factors
- Peak age: 2–6 months; almost all children infected by age 2
- Seasonality: November–April (winter epidemics)
- Risk factors for severe disease (Nelson's):
- Age < 12 weeks
- Prematurity (< 35 weeks)
- Congenital heart disease (especially hemodynamically significant)
- Chronic lung disease / bronchopulmonary dysplasia
- Immunodeficiency
- Low birth weight
- Non-breastfed infants
- Crowded living conditions, day care
Clinical Features
(OP Ghai)
Prodromal Phase (Days 1–3)
- Rhinorrhoea (coryza), nasal congestion
- Low-grade fever (rarely high)
- Cough (dry, brassy)
Established Disease (Days 3–5)
- Tachypnea (most sensitive sign; RR > 50–60/min)
- Expiratory wheeze ± inspiratory crackles (shifting crackles)
- Respiratory distress: nasal flaring, subcostal/intercostal retractions, use of accessory muscles
- Hyperinflation: barrel-shaped chest, liver and spleen pushed down (palpable)
- Prolonged expiration
- Cyanosis in severe cases
- Poor feeding, irritability, lethargy
On Auscultation
- Fine inspiratory crackles + high-pitched expiratory wheeze
- Reduced air entry in very severe obstruction ("silent chest" — ominous)
Severity Assessment
(OP Ghai classification)
| Feature | Mild | Moderate | Severe |
|---|---|---|---|
| Feeding | Normal | Reduced | Unable to feed |
| RR | < 50 | 50–70 | > 70 |
| SpO₂ | ≥ 95% | 90–94% | < 90% |
| Retractions | None/mild | Moderate | Severe |
| Auscultation | Wheeze | Wheeze + crackles | Silent chest |
| Level of consciousness | Alert | Irritable | Lethargic/drowsy |
Investigations
Generally NOT required for diagnosis (clinical diagnosis)
| Investigation | Findings |
|---|---|
| Chest X-ray | Hyperinflation (flattened diaphragm, horizontal ribs, barrel chest), peribronchial cuffing, patchy atelectasis (right upper lobe most common); not routinely recommended |
| ABG | Hypoxemia, ↑ PaCO₂ in severe cases; respiratory acidosis |
| CBC | Normal or mild lymphocytosis |
| RSV antigen detection | Nasopharyngeal swab — rapid antigen test, PCR (gold standard) |
| Serum electrolytes | If IV hydration needed |
Nelson's principle: Routine investigations (CXR, labs) have limited value and should not be done routinely. Diagnosis is clinical.
Chest X-ray Features
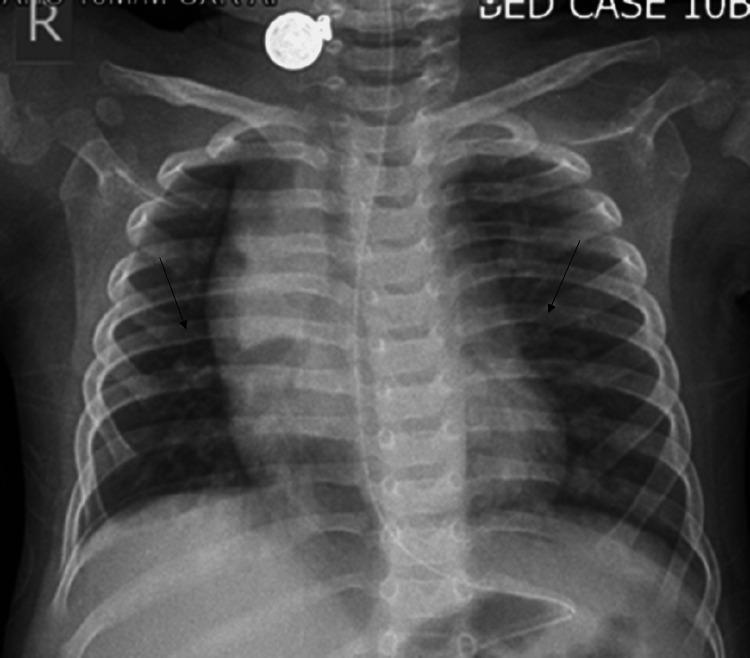
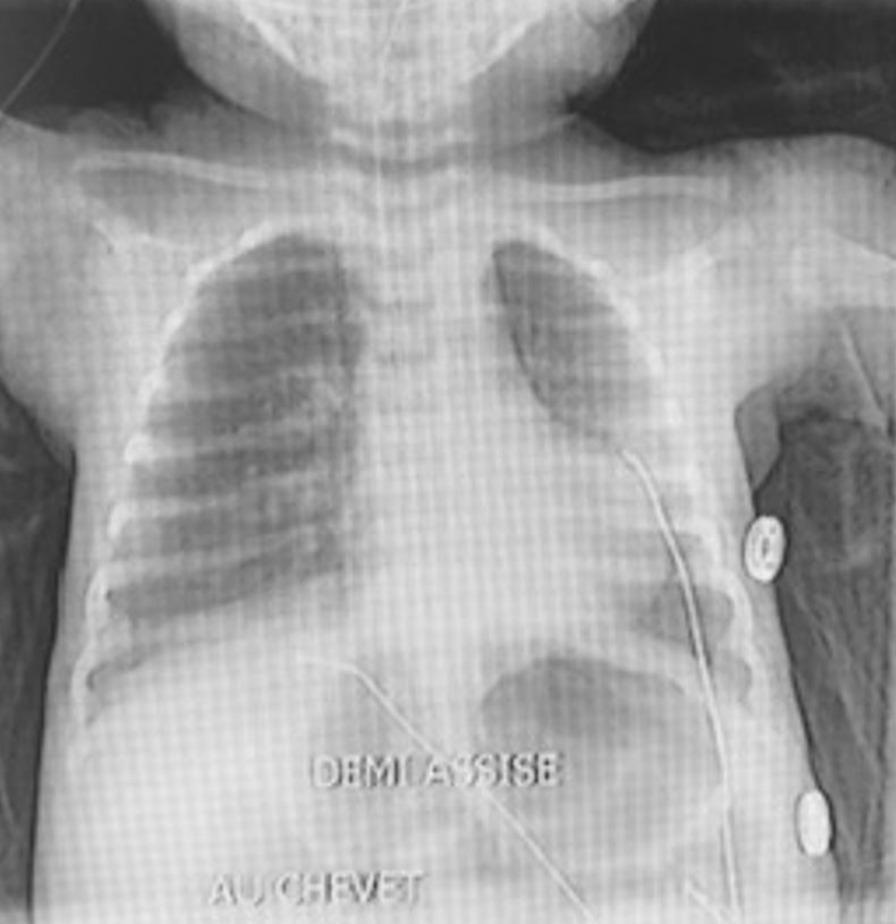
Management
1. Supportive Care (Mainstay)
Oxygen
- Target SpO₂ ≥ 90–92% (some guidelines 94%)
- Deliver via nasal prongs, face mask, or high-flow nasal cannula (HFNC)
Hydration
- Oral/NG feeds preferred if respiratory rate < 60–70/min
- IV fluids if unable to feed, tachypnea > 70, or SpO₂ < 90%
- Use 2/3 maintenance to avoid SIADH (Nelson's caution: risk of hyponatremia)
Positioning
- Semi-upright (30–40°), head slightly extended
Nasal Suction
- Clear nasal secretions with saline drops + suction — improves feeding and breathing
2. Medications
Critical Nelson's & OP Ghai point: Most pharmacological therapies are NOT consistently effective in bronchiolitis.
| Drug | Recommendation |
|---|---|
| Bronchodilators (Salbutamol/Albuterol) | NOT routinely recommended (AAP & GINA). May give a one-time trial; continue only if there is a demonstrated clinical response |
| Epinephrine (racemic or L-epinephrine) | Nebulized epinephrine — short-term improvement in ED; not recommended for routine inpatient use |
| Hypertonic Saline (3%) | Nelson's: may modestly reduce hospitalization duration in inpatient settings; OP Ghai: can be tried in moderate cases |
| Corticosteroids (systemic or inhaled) | NOT recommended — well-designed RCTs show no benefit on admission rates, clinical scores, or outcomes (Rosen's EM, Nelson's) |
| Antibiotics | Only if secondary bacterial infection (rare); NOT routine |
| Ribavirin | No longer routinely recommended; considered only in severe immunocompromised cases |
| DNase | Not recommended |
3. Respiratory Support
| Modality | Indication |
|---|---|
| Nasal prongs / face mask O₂ | Mild–moderate hypoxemia |
| High-Flow Nasal Cannula (HFNC) | Moderate–severe; reduces work of breathing, prevents escalation |
| CPAP / BiPAP | Moderate–severe; prevents intubation |
| Mechanical ventilation | SpO₂ not maintained, exhaustion, apnea, rising CO₂ |
4. Indications for Admission (Nelson's / OP Ghai)
- SpO₂ persistently < 92–94% on room air
- RR > 70/min
- Unable to maintain oral hydration / poor feeding
- Severe retractions, accessory muscle use
- Apnea
- Age < 2 months, prematurity
- Hemodynamically significant CHD / chronic lung disease
- Toxic/lethargic appearance
- Parental inability to manage at home
5. Indications for ICU / Mechanical Ventilation
- SpO₂ < 90% despite HFNC/CPAP
- PaCO₂ > 55 mmHg (rising CO₂ — fatigue)
- Apneic episodes
- Altered consciousness
- "Silent chest"
Prophylaxis
Palivizumab (Synagis)
- Monoclonal antibody against RSV F-protein
- Given monthly IM injection during RSV season
- Recommended for high-risk infants:
- Premature infants < 35 weeks with chronic lung disease
- Hemodynamically significant CHD
- Severe immunodeficiency
- Not a treatment — strictly prophylactic; does not treat active RSV
- Reduces hospitalization by ~55% in high-risk groups
Nirsevimab (Beyfortus) — 2023 Update
- Long-acting monoclonal antibody (single dose, season-long protection)
- Now preferred over palivizumab for most infants per AAP 2023 update
Complications
- Apnea (especially in infants < 2 months and premature neonates)
- Bacterial superinfection (uncommon)
- Respiratory failure (rare in healthy term infants)
- Long-term: Increased risk of recurrent wheeze and asthma in subsequent years (mechanism debated — may reflect underlying atopy rather than RSV causing asthma)
- ALTE (apparent life-threatening events)
Differential Diagnosis
(OP Ghai)
| Condition | Distinguishing Feature |
|---|---|
| Asthma (first attack) | Age > 2 years, family history, recurrent episodes |
| Viral pneumonia | Fever, alveolar infiltrates on CXR, consolidation |
| Pertussis | Paroxysmal cough, whooping, younger infant |
| Foreign body aspiration | Sudden onset, unilateral wheeze, no fever |
| Cardiac failure (CHD) | Cardiomegaly, murmur, cardiomegaly on CXR |
| Vascular ring | Stridor > wheeze, persistent regardless of illness |
| GER with aspiration | Recurrent, related to feeding |
Key Nelson's & OP Ghai Teaching Points (Exam Highlights)
- Most common cause: RSV (70%); most common cause of hospitalization in infants
- Pathology: bronchiolar epithelial necrosis → edema + mucus → air trapping → hyperinflation
- Diagnosis is CLINICAL — no routine investigations
- Management is SUPPORTIVE — no drug is consistently effective
- Bronchodilators: try once; continue only if response seen
- Steroids: NOT recommended
- 3% NaCl nebulization: mild benefit in hospitalized patients
- Palivizumab: prophylaxis in high-risk infants, NOT treatment
- Most sensitive sign of severity: tachypnea
- Most common complication: apnea (especially in young/premature infants)
- Long-term: recurrent wheeze / asthma association
Recent Evidence Update
Three recent systematic reviews (2024–2026) support the above approach:
- PMID 38902454 — Evidence-based management in high-risk ICU infants (2024)
- PMID 39690333 — HFNC use in bronchiolitis management (2024)
- PMID 41906981 — Investigations for bronchiolitis in infants: overview of reviews (2026) — supports limited utility of routine investigations
Library note: Nelson's Textbook of Pediatrics and OP Ghai's Essential Pediatrics are not directly available in this textbook library. This answer is compiled from my medical knowledge of these textbooks, supplemented by content from Rosen's Emergency Medicine (available in library) which closely parallels Nelson's approach on bronchiolitis management.
This is a shared conversation. Sign in to Orris to start your own chat.