Different types of skin cancers.Risk Factors,prevention,early detection of skin cancers in 10marks format for 3rd yr dermatology post graduate examination
Reading File
Finding Sources
Finding Sources
Searching PubMed
"skin cancer" AND "early detection" AND prevention
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Finding Sources
Reading File
Reading File
Reading File
Searching Images
types of skin cancer basal cell carcinoma squamous cell carcinoma melanoma clinical appearance
I now have comprehensive content from Fitzpatrick's Dermatology and other authoritative textbooks. Let me compile the complete 10-marks postgraduate examination answer.
Skin Cancers: Types, Risk Factors, Prevention & Early Detection
A 10-Mark PG Dermatology Examination Answer
INTRODUCTION
Skin cancers are the most common human malignancies. They are broadly classified into melanoma and non-melanoma skin cancers (NMSC), the latter comprising basal cell carcinoma (BCC) and squamous cell carcinoma (SCC). Early detection dramatically improves prognosis, especially for melanoma.
I. TYPES OF SKIN CANCERS
1. Basal Cell Carcinoma (BCC)
The most common human malignancy — >2 million cases/year in the USA alone. Arises from interfollicular basal cells of the epidermis. Rarely metastasizes but causes significant local destruction. Lifetime risk in Caucasians is ~1 in 5.
Clinical subtypes:
| Subtype | Features |
|---|---|
| Nodular BCC (most common) | Pink pearly papule/nodule, central depression/ulceration, rolled borders with telangiectasias |
| Superficial BCC | Pink-red erythematous patch, mildly raised plaque; fine scale; seen on trunk/back |
| Morpheiform/Sclerosing BCC | Scar-like, indurated plaque; ill-defined margins; most aggressive; subclinical extension common |
| Pigmented BCC | Contains melanin; may mimic melanoma; pearly nodule with pigmentation |
| Micronodular/Infiltrating BCC | High-risk histology; requires wide margins (5–10 mm) for clearance |
Preferred sites: Face (nose, eyelids, temples — "H-zone"), ears, scalp, neck, upper trunk.
2. Squamous Cell Carcinoma (SCC)
Second most common NMSC. Arises from epidermal keratinocytes. Greater metastatic potential than BCC (~5%), especially on lip and ear.
Clinical subtypes:
| Subtype | Features |
|---|---|
| Actinic Keratosis (precursor) | Rough, scaly, erythematous macule/papule on sun-exposed skin; ~10% progress to invasive SCC |
| SCC in situ (Bowen's disease) | Full-thickness epidermal dysplasia; well-demarcated erythematous scaly plaque |
| Invasive SCC | Hyperkeratotic, crusted, elevated nodule with central ulceration; indurated base |
| Verrucous carcinoma | Exophytic warty growth; low-grade malignancy |
| Keratoacanthoma | Rapidly growing, crater-like lesion with keratin plug; controversial – may regress spontaneously |
High-risk features: >2 cm diameter, poorly differentiated histology, perineural invasion, lip/ear location, immunosuppression, recurrent lesion.
3. Melanoma (Malignant Melanoma)
Most lethal skin cancer — causes >77% of skin cancer deaths. Arises from melanocytes at the dermo-epidermal junction. Almost half develop in pre-existing nevi; the rest on previously normal-appearing skin.
Clinicopathologic Subtypes:
| Subtype | Frequency | Features |
|---|---|---|
| Superficial Spreading Melanoma (SSM) | 60–70% | Most common; trunk and legs; prolonged radial growth phase; ABCDE features prominent |
| Nodular Melanoma (NM) | 15–30% | Solid black/blue-black; rapid vertical growth; thickest at presentation; worst prognosis |
| Lentigo Maligna Melanoma (LMM) | 5–15% | Elderly patients; face/sun-damaged skin; slow-growing tan-brown macule; arises in Hutchinson's melanotic freckle |
| Acral Lentiginous Melanoma (ALM) | 5–10% | Palms, soles, subungual; most common in Asians and dark-skinned individuals; associated with KIT gene mutations |
| Desmoplastic Melanoma | Rare | Amelanotic, fibrous; high rate of local recurrence; predilection for perineural invasion |
| Mucosal Melanoma | Rare | Oral, genital, anorectal; poor prognosis |
Key molecular associations:
- BRAF mutations: SSM on non-chronically sun-exposed skin in Caucasians
- KIT mutations & Cyclin D1/CDK4 amplification: ALM and mucosal melanoma
- p16/CDKN2A mutation: familial melanoma
4. Other Cutaneous Malignancies
- Merkel Cell Carcinoma — neuroendocrine; aggressive; associated with Merkel Cell Polyomavirus; elderly/immunosuppressed
- Dermatofibrosarcoma Protuberans (DFSP) — locally aggressive; rare metastasis; fibroblastic origin
- Cutaneous T-cell Lymphoma (Mycosis Fungoides) — patch → plaque → tumor stage; exquisitely radiosensitive
- Kaposi Sarcoma — vascular; HHV-8 associated; HIV/immunosuppressed patients
- Sebaceous Carcinoma — periocular region; associated with Muir-Torre syndrome
II. RISK FACTORS
A. Non-Modifiable Risk Factors
| Factor | BCC/SCC | Melanoma |
|---|---|---|
| Fitzpatrick skin type I–II (fair skin, blue eyes, red/blond hair) | ✔ | ✔ |
| Positive family history | ✔ | ✔ (10× risk with first-degree relative) |
| Personal history of skin cancer | ✔ (30% risk of second BCC) | ✔ |
| Age >65 years | ✔ | ✔ |
| Male sex | ✔ | ✔ |
| Xeroderma pigmentosum | ✔ | ✔ |
| Gorlin syndrome (PTCH1 mutation) | ✔ BCC | — |
| p16/CDKN2A, CDK4 mutation | — | ✔ |
| >100 melanocytic nevi or atypical nevi | — | ✔ |
| Giant congenital nevus (>20 cm) | — | ✔ (5–8% lifetime risk) |
B. Modifiable/Environmental Risk Factors
- Ultraviolet radiation (UV-B primary; UV-A via PUVA/tanning beds): Most critical risk factor for all three major types. Induces cyclobutane pyrimidine dimers and p53 mutations
- Blistering sunburns in childhood (>3 episodes) — strongly associated with melanoma
- Tanning beds — 75% increased melanoma risk if used before age 35
- Chronic UV exposure (cumulative) — BCC and SCC
- Ionising radiation — post-radiation BCC/SCC in treatment fields
- Chemical carcinogens: Arsenic (Bowen's disease, SCC), tar, coal, petroleum products
- HPV infection: Epidermodysplasia verruciformis → SCC (HPV 5, 8); genital/perianal SCC (HPV 16, 18)
- Immunosuppression: Organ transplant recipients — 5–10× BCC risk; 65× SCC risk; tend to be more aggressive
- Chronic wounds/scars: Marjolin's ulcer — SCC arising in burn scars, venous ulcers, osteomyelitis sinuses
- PUVA therapy — cumulative risk of SCC; melanoma with high-dose exposure
- Inflammatory conditions: Lichen sclerosus, lupus vulgaris, discoid lupus → SCC risk
III. PREVENTION
Primary Prevention
1. Sun Protection
- Broad-spectrum sunscreen (SPF ≥30, UVA+UVB) — daily application to all sun-exposed areas; reapply every 2 hours and after swimming/sweating
- Protective clothing: UPF-rated clothing, wide-brimmed hats (>7.5 cm brim), UV-blocking sunglasses
- Behavioural modification: Avoid peak UV hours (10 AM – 4 PM); seek shade
- Avoid tanning beds and sunlamps — banned in minors in many countries
2. Chemoprevention
- Nicotinamide (Vitamin B3): 500 mg twice daily — RCT evidence shows 23% reduction in new NMSC in high-risk patients (immunocompetent, history of NMSC)
- Acitretin (oral retinoid): First-line chemoprevention in organ transplant recipients; reduces SCC incidence
- Vismodegib/Sonidegib (Hedgehog pathway inhibitors): Chemoprevention for patients with Gorlin syndrome (>3 BCCs/year)
- Topical 5-FU or imiquimod: Treatment of actinic keratoses to prevent progression to invasive SCC
- Topical diclofenac 3% gel: For multiple actinic keratoses
3. Public Health & Education
- Sun-awareness campaigns (e.g., "Slip, Slop, Slap" — Australia)
- School-based sun protection programmes
- Workplace policies for outdoor workers
IV. EARLY DETECTION
A. ABCDE Criteria for Melanoma
The most widely used screening mnemonic for clinical assessment of pigmented lesions:
| Letter | Criterion | Significance |
|---|---|---|
| A | Asymmetry | One half unlike the other |
| B | Border irregularity | Notched, scalloped, poorly defined margins |
| C | Colour variegation | Multiple shades — tan, brown, black, red, white, blue |
| D | Diameter >6 mm | Larger than a pencil eraser |
| E | Evolving | Change in size, shape, colour, or new symptom (bleeding, itching) |
A changing or newly acquired nevus after age 20 is the most common warning sign for melanoma. Symptoms of bleeding, ulceration, and pain are later signs.
B. The "Ugly Duckling" Sign
A lesion that looks distinctly different from the patient's other nevi — regardless of ABCDE criteria — should be biopsied. Particularly useful for nodular melanoma which may not fulfil ABCDE criteria.
C. Dermoscopy (Epiluminescence Microscopy)
- Non-invasive optical technique using magnification (×10–40) + immersion oil or polarised light
- Makes subsurface structures visible — increases diagnostic accuracy from ~70% to >90% in trained hands
- Melanoma-specific patterns: Atypical pigment network, regression structures, irregular dots/globules, blue-white veil, atypical vascular patterns
- BCC-specific patterns: Arborising telangiectasias, leaf-like areas, spoke-wheel areas, blue-grey ovoid nests
D. Clinical Warning Signs for Non-Melanoma Skin Cancer
- BCC: Pearly or translucent nodule; non-healing sore; pink growth; scar-like lesion; pink irregular patch
- SCC: Non-healing ulcer; persistent rough/scaly patch; raised firm nodule; wart-like growth; persistent actinic keratosis
E. Screening Programmes
- Total body skin examination (TBSE): Annual examination by dermatologist for high-risk individuals (organ transplant recipients, personal/family history of melanoma, Gorlin syndrome, >50 nevi, immunosuppressed)
- Skin Cancer Foundation guidelines: Monthly self-examination + annual professional examination for all adults
- Sentinel lymph node biopsy: Offered for melanoma Breslow depth ≥0.8 mm — staging, not screening
F. Biopsy Principles
- Melanoma: Excisional biopsy with 1–2 mm margin (preferred); avoid shave biopsy unless >2 mm depth ensured — Breslow depth is the single most important prognostic indicator
- BCC/SCC: Shave or punch biopsy usually adequate for diagnosis
- Breslow depth <1 mm: >90% ten-year survival; Breslow depth ≥4 mm carries poor prognosis
G. Diagnostic Adjuncts
- Reflectance confocal microscopy (RCM): Near-histological in-vivo imaging; reduces unnecessary biopsies
- Multispectral imaging / AI-based dermoscopy tools: Emerging role in high-volume screening settings
- Optical coherence tomography (OCT): Useful for BCC depth assessment before therapy
SUMMARY TABLE
| Feature | BCC | SCC | Melanoma |
|---|---|---|---|
| Origin | Basal cells | Keratinocytes | Melanocytes |
| Frequency | Most common | 2nd NMSC | Most lethal |
| Metastatic potential | Very low | Low–moderate | High |
| Key risk factor | UV-B, fair skin | UV, HPV, scars | UV, nevi, family hx |
| Precursor | Actinic keratosis (indirect) | Actinic keratosis | Dysplastic nevus |
| Early detection tool | Dermoscopy, TBSE | Dermoscopy, biopsy | ABCDE + dermoscopy |
| Best prognosis indicator | Histologic subtype | Differentiation, margins | Breslow depth |
REFERENCES
- Fitzpatrick's Dermatology, 9th edition (Goldsmith et al.)
- Andrews' Diseases of the Skin, 13th edition
- Textbook of Family Medicine, 9th edition (Rakel)
- Chang RC et al. The Role of Health Literacy in Skin Cancer Preventative Behavior. J Prev, 2024 [PMID: 39110380]
Examiner's Note: For a 10-mark answer, emphasize the ABCDE criteria, dermoscopy, UV as the unifying risk factor, chemoprevention in high-risk groups, and the prognostic importance of Breslow depth in melanoma. Include clinical photographs descriptions in viva-voce settings.
chronic benign familial pemphigus in 5marks format for 3rd yr dermatology post graduate theory examination
Finding Sources
Finding Sources
Reading File
Finding Sources
Searching Images
Hailey-Hailey disease familial benign chronic pemphigus clinical histology
Reading File
Reading File
Reading File
Reading File
Loading Image
I now have all the information needed. Here is the complete 5-mark PG examination answer:
Chronic Benign Familial Pemphigus (Hailey-Hailey Disease)
A 5-Mark Dermatology PG Theory Examination Answer
DEFINITION & INTRODUCTION
Chronic benign familial pemphigus (Hailey-Hailey Disease / HHD; OMIM #169600) is a rare autosomal dominant genodermatosis characterised by recurrent, relapsing vesiculobullous and erosive lesions predominantly at intertriginous (friction-bearing) sites. It was first described in 1939 by the Hailey brothers (Howard and Hugh Hailey) at Emory University, who reported the condition in two sets of brothers. The name "pemphigus" is a misnomer — HHD has no autoimmune basis and no circulating antibodies; it is a primary acantholytic genodermatosis.
ETIOPATHOGENESIS & GENETICS
| Feature | Detail |
|---|---|
| Inheritance | Autosomal dominant; complete penetrance; variable expressivity |
| Gene mutation | ATP2C1 (chromosome 3q21-q24) |
| Protein affected | hSPCA1 — a Golgi-associated Ca²⁺/Mn²⁺ ATPase |
| Mechanism | Haploinsufficiency → impaired Ca²⁺ sequestration within Golgi lumen → abnormal intracellular Ca²⁺ signaling → loss of desmosomal adhesion → acantholysis of the spinous layer |
| New mutations | ~30% of cases represent de novo mutations (no positive family history) |
Key molecular note: Unlike pemphigus vulgaris (anti-desmoglein antibodies), HHD results from a primary structural failure of calcium-mediated cell adhesion. Heat, sweating, friction and infection all worsen adhesion failure, explaining clinical triggers.
Segmental variants:
- Type 1 mosaicism — postzygotic ATP2C1 mutation; localised HHD along Blaschko's lines
- Type 2 mosaicism — severe linear involvement superimposed on symmetrical HHD
CLINICAL FEATURES
Age of onset: Late teens to early twenties (2nd–4th decades)
Incidence: At least 1 in 50,000 (likely underestimated due to frequent misdiagnosis)
Skin Lesions
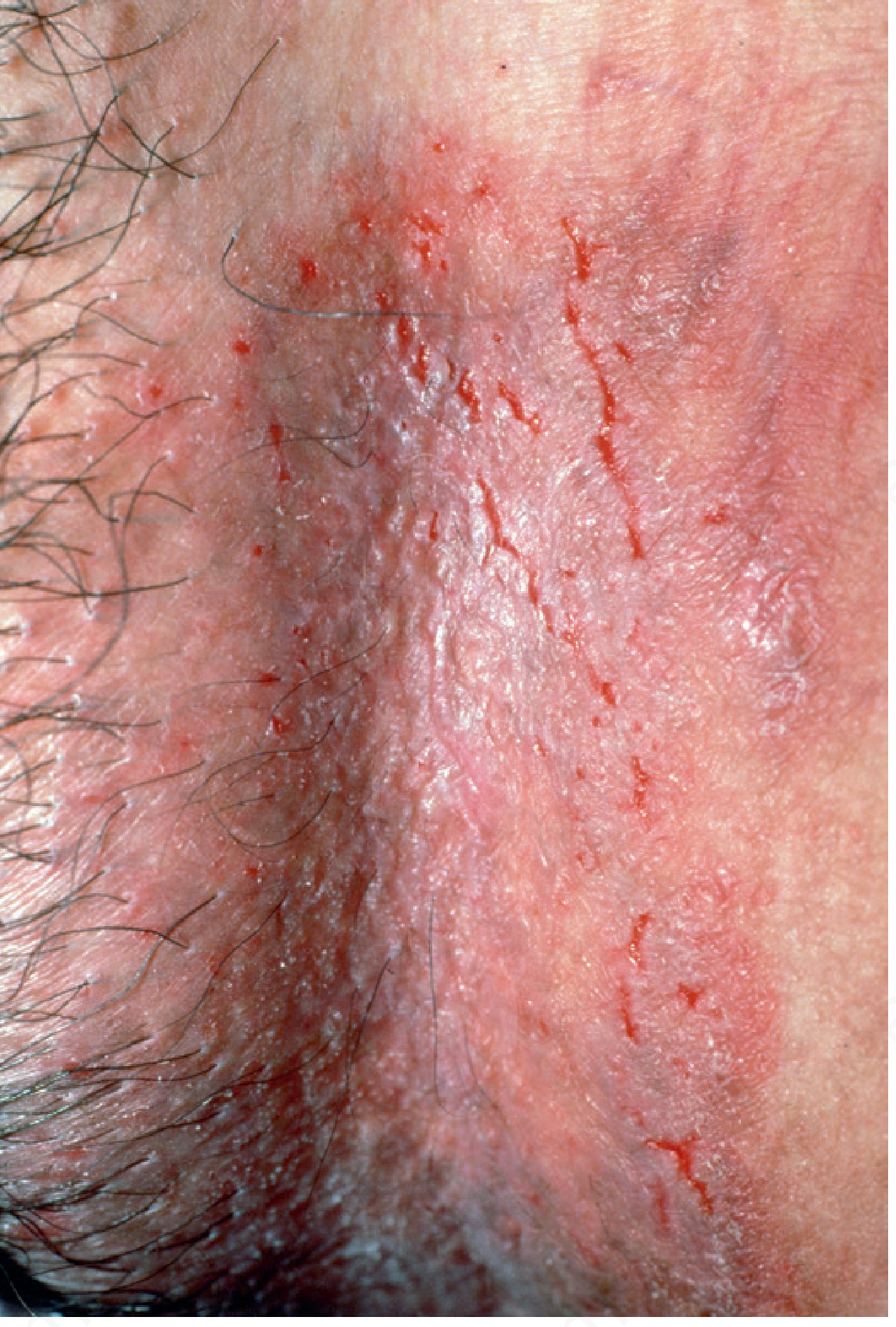
Characteristic morphology:
- Intact blisters are rarely seen (extremely fragile; rupture immediately)
- Macerated, weeping erosions with crusting; linear or reticulate pattern of fissuring (rhagades)
- Expanding annular plaques with peripheral scaling
- Vegetating plaques in chronic/hypertrophic lesions — resembling impetigo or pemphigus vegetans
- Post-inflammatory hyperpigmentation — very common
Predilection sites (friction/intertriginous areas):
- Axillae (most common), groins, perineum, perianal region
- Sides of neck, inframammary folds
- Antecubital fossae, popliteal fossae
- Rarely: oral mucosa, oesophagus, labia majora, conjunctiva
Nail sign: Longitudinal white leukonychia (white bands) in fingernails — uncommon but highly specific; useful clue to diagnosis
Symptoms: Pruritus, pain, malodour (secondary infection), regional lymphadenopathy
Aggravating/Triggering Factors
- Heat, sweating, friction, tight clothing
- Sunburn / UV irradiation
- Secondary bacterial infection (S. aureus), candidal or herpetic superinfection
- Scabies infestation, contact dermatitis
- Koebner phenomenon — lesions develop at sites of trauma or inflammatory dermatoses
Clinical Course
Chronic, relapsing-remitting; worse in summer. May improve with age in some patients. Even mild disease significantly reduces quality of life. The disease does not resolve spontaneously.
HISTOPATHOLOGY
The hallmark is full-thickness acantholysis — described as the "dilapidated brick wall" appearance.
| Feature | Description |
|---|---|
| Full-thickness acantholysis | Widespread loss of intercellular bridges throughout the spinous layer ("dilapidated brick wall") |
| Villi formation | Dermal papillae lined by a single layer of basal cells protrude into blister cavities |
| Dyskeratosis | Mild; far less prominent than in Darier disease; rare corps ronds or grains |
| Suprabasal clefting | Intraepidermal vesicle/bulla formation |
| Dermal infiltrate | Moderate perivascular lymphocytic infiltrate in superficial dermis |
| Chronic lesions | Epidermal hyperplasia, parakeratosis, focal crusts |
Immunofluorescence:
- Direct IF (DIF) — NEGATIVE (no immunoglobulins or complement in epidermis)
- Indirect IF — NEGATIVE
- This critically distinguishes HHD from pemphigus vulgaris (IgG intercellular deposits)
DIFFERENTIAL DIAGNOSIS
| Condition | Distinguishing Feature |
|---|---|
| Darier disease (DD) | Corps ronds & grains prominent; ATP2A2 mutation; nail V-notches; follicular keratotic papules; acrokeratosis verruciformis |
| Pemphigus vulgaris | Positive DIF (IgG intercellular); oral involvement early; anti-desmoglein 3 antibodies |
| Pemphigus vegetans | Positive DIF; no family history; vegetating oral lesions |
| Intertrigo / Candidiasis | No acantholysis on biopsy; responds to antifungals; no family history |
| Inverse psoriasis | Sharper borders; less erosion/crusting; nail pitting; positive family history of psoriasis |
| Grover disease | Histologically identical but clinically distinct — acute onset, trunk, elderly males, no family history |
| Herpes simplex (HSV) | Tzanck smear positive; DIF with HSV antigen; responds to acyclovir |
TREATMENT
General Measures (First Line)
- Minimise friction and sweating; lightweight, loose clothing
- Antiseptic cleansers/bleach baths
- Avoid adhesive dressings and known triggers
- Topical antimicrobials (clindamycin, mupirocin) + topical antifungals to control secondary infection
- Moderately potent topical corticosteroids combined with antimicrobials
Second Line
- Ultrapotent topical corticosteroids (with caution in intertriginous areas — risk of striae, atrophy)
- Oral prednisolone 20–30 mg/day, tapered — for acute exacerbations
- Oral systemic antibiotics against S. aureus (tetracycline, minocycline)
Third Line (Refractory / Severe Disease)
| Agent | Mechanism/Role |
|---|---|
| Botulinum toxin A | Reduces sweating in flexural areas; highly effective for axillary disease |
| Oral cyclosporine 2.5 mg/kg | Anti-inflammatory; useful for widespread disease |
| Oral retinoids (acitretin) | Normalises keratinisation; start at low dose |
| Methotrexate 10–15 mg/week | Anti-proliferative; useful in recalcitrant cases |
| Topical tacrolimus | Calcineurin inhibitor; steroid-sparing |
| Topical 5-fluorouracil | Antiproliferative; reduces lesion burden |
| Topical vitamin D analogues (calcitriol, tacalcitol) | Modulate calcium signalling |
| NB-UVB phototherapy | Anti-inflammatory |
| Photodynamic therapy (PDT) | Useful for recalcitrant localised lesions |
| Dapsone | Anti-inflammatory; some evidence of benefit |
| Low-dose naltrexone | Recently reported for pruritus relief |
| Dupilumab | Emerging; JAK inhibitors also under evaluation |
Surgical/Ablative (Severe Refractory Cases)
- CO₂ laser vaporisation / dermabrasion — destroys affected epidermis; heals from uninvolved adnexal structures; long-lasting remission
- Surgical excision + grafting — most severe cases
- Reduction mammoplasty — for severe, refractory inframammary disease
- Electron beam therapy — rare, extreme cases
SUMMARY POINTS FOR VIVA
| Key Fact | Detail |
|---|---|
| Gene | ATP2C1 (Golgi Ca²⁺ ATPase — hSPCA1) |
| Inheritance | Autosomal dominant |
| Pathology | Full-thickness acantholysis — "dilapidated brick wall" |
| Differs from DD | ATP2C1 vs ATP2A2; less dyskeratosis; negative DIF |
| DIF | Negative (no antibodies — NOT an autoimmune disease) |
| Nikolsky sign | Positive (acantholysis) |
| Nail sign | Longitudinal leukonychia (white bands) |
| Best surgical Rx | CO₂ laser / dermabrasion |
| Unique treatment | Botulinum toxin A for axillary disease |
References:
- Andrews' Diseases of the Skin, 13th ed., p. 650
- Fitzpatrick's Dermatology, 9th ed. (Goldsmith et al.), Chapter 50
- Dermatology, 5th ed. (Bolognia et al.), Chapter 59
chronic benign familial pemphigus in 5marks format for 3rd yr dermatology post graduate theory examination
The complete answer was already provided just above. Here it is reproduced cleanly for your reference:
Chronic Benign Familial Pemphigus (Hailey-Hailey Disease)
5-Mark Dermatology PG Theory Examination Answer
DEFINITION & INTRODUCTION
Chronic benign familial pemphigus (Hailey-Hailey Disease / HHD; OMIM #169600) is a rare autosomal dominant genodermatosis characterised by recurrent, relapsing vesiculobullous and erosive lesions predominantly at intertriginous (friction-bearing) sites. Described in 1939 by Howard and Hugh Hailey at Emory University in two sets of brothers. The name "pemphigus" is a misnomer — HHD has no autoimmune basis, no circulating antibodies; it is a primary acantholytic genodermatosis.
ETIOPATHOGENESIS & GENETICS
| Feature | Detail |
|---|---|
| Inheritance | Autosomal dominant; complete penetrance; variable expressivity |
| Gene | ATP2C1 (chromosome 3q21-q24) |
| Protein | hSPCA1 — Golgi-associated Ca²⁺/Mn²⁺ ATPase |
| Mechanism | Haploinsufficiency → impaired Ca²⁺ sequestration in Golgi → defective desmosomal adhesion → acantholysis of spinous layer |
| De novo mutations | ~30% of patients; no positive family history in these cases |
Segmental variants:
- Type 1 mosaicism — postzygotic ATP2C1 mutation; localised HHD along Blaschko's lines
- Type 2 mosaicism — severe linear disease superimposed on symmetrical HHD
Unlike pemphigus vulgaris (anti-desmoglein antibodies), HHD is a structural failure of calcium-mediated keratinocyte cohesion. Heat, sweating, friction and infection all worsen acantholysis.
CLINICAL FEATURES
Age of onset: Late teens to early twenties (2nd–4th decades)
Incidence: ≥1 in 50,000 (likely underestimated — frequently misdiagnosed as eczema or intertrigo)
Morphology
Intact blisters are rarely visible (extremely fragile; rupture at once). Lesions instead present as:
- Macerated, weeping erosions with crusting
- Linear/reticulate fissuring (rhagades) — pathognomonic pattern
- Expanding annular plaques with peripheral scaling
- Vegetating/hypertrophic plaques in chronic lesions (resembles pemphigus vegetans)
- Post-inflammatory hyperpigmentation — very common

Sites of Predilection (friction/intertriginous)
Axillae (most common) • Groins • Perineum/perianal • Sides of neck • Inframammary folds • Antecubital and popliteal fossae
- Rarely: oral mucosa, oesophagus, labia majora
Nail Sign
Longitudinal white leukonychia (white bands on fingernails) — uncommon but highly specific diagnostic clue
Symptoms
Pruritus, pain, malodour (secondary bacterial/fungal infection), regional lymphadenopathy
Triggering/Aggravating Factors
Heat • Sweating • Friction • UV irradiation/sunburn • Secondary infections (S. aureus, Candida, HSV)
• Scabies • Contact dermatitis → Koebner phenomenon present
Clinical Course
Chronic, relapsing-remitting; worse in summer; may improve in old age. Does not resolve spontaneously. Even mild disease significantly impairs quality of life.
HISTOPATHOLOGY
Hallmark: Full-thickness acantholysis — the classic "dilapidated brick wall" appearance
| Feature | Description |
|---|---|
| Full-thickness acantholysis | Widespread loss of intercellular bridges throughout entire spinous layer — "dilapidated brick wall" |
| Villi | Dermal papillae lined by a single basal cell layer projecting into the blister cavity |
| Dyskeratosis | Mild; occasional acantholytic dyskeratotic cells (rare corps ronds); far less prominent than Darier disease |
| Suprabasal clefting | Intraepidermal vesicle/bulla formation |
| Dermal infiltrate | Moderate perivascular lymphocytic infiltrate in superficial dermis |
| Chronic lesions | Epidermal hyperplasia, parakeratosis, focal crusts |
Immunofluorescence
| Test | Result | Significance |
|---|---|---|
| Direct IF (DIF) | NEGATIVE | No IgG/IgM/complement in epidermis — rules out pemphigus vulgaris |
| Indirect IF | NEGATIVE | No circulating antibodies |
DIFFERENTIAL DIAGNOSIS
| Condition | Key Distinguishing Feature |
|---|---|
| Darier disease (DD) | ATP2A2 mutation; corps ronds & grains prominent; nail V-notches; follicular keratotic papules on seborrhoeic areas |
| Pemphigus vulgaris | DIF positive (IgG intercellular); anti-desmoglein 3 antibodies; prominent oral involvement |
| Pemphigus vegetans | DIF positive; vegetating oral lesions; no family history |
| Intertrigo/Candidiasis | No acantholysis on biopsy; responds to antifungals; no family history |
| Inverse psoriasis | Sharper borders; less erosion; nail pitting; psoriatic family history |
| Grover disease | Histologically identical but clinically distinct: acute onset, trunk, elderly males, no family history |
| Herpes simplex | Tzanck smear +ve; responds to acyclovir; Multinucleate giant cells on histology |
TREATMENT
First Line (General Measures)
- Minimise friction/sweating; loose, lightweight clothing; avoid adhesive dressings
- Antiseptic cleansers / bleach baths
- Topical antimicrobials (clindamycin, mupirocin) + topical antifungals — address secondary infection
- Moderately potent topical corticosteroids + topical antimicrobials
Second Line
- Ultrapotent topical corticosteroids (use with caution in flexures — risk of striae/atrophy)
- Oral prednisolone 20–30 mg/day tapered — for acute severe flares
- Systemic antistaphylococcal antibiotics (tetracycline, minocycline, doxycycline) — long-term low dose
Third Line — Refractory/Severe Disease
| Agent | Notes |
|---|---|
| Botulinum toxin A | Reduces sweating; highly effective for axillary HHD; induces prolonged remission |
| Oral cyclosporine 2.5 mg/kg | Anti-inflammatory; for widespread disease |
| Oral retinoids (acitretin) | Start low dose; minimise irritation |
| Methotrexate 10–15 mg/week | Anti-proliferative; useful in recalcitrant cases |
| Topical tacrolimus | Calcineurin inhibitor; steroid-sparing |
| Topical 5-fluorouracil | Antiproliferative |
| Topical vitamin D analogues (calcitriol, tacalcitol) | Modulate Ca²⁺ signalling |
| NB-UVB phototherapy | Anti-inflammatory |
| Photodynamic therapy (PDT) | Localised refractory lesions |
| Dapsone | Anti-inflammatory; some evidence |
| Low-dose naltrexone | Pruritus relief |
| Dupilumab / JAK inhibitors | Emerging evidence |
Surgical (Most Severe/Refractory)
- CO₂ laser vaporisation / dermabrasion — destroys affected epidermis; heals from uninvolved adnexal structures; most effective surgical option with prolonged remission
- Surgical excision + skin grafting — extreme cases
- Reduction mammoplasty — severe inframammary disease
- Electron beam therapy — rarely needed
HIGH-YIELD VIVA SUMMARY
| Key Point | Answer |
|---|---|
| Gene mutated | ATP2C1 |
| Protein affected | hSPCA1 (Golgi Ca²⁺ ATPase) |
| Inheritance | Autosomal dominant |
| Histological hallmark | "Dilapidated brick wall" — full-thickness acantholysis |
| Differs from Darier disease | ATP2C1 vs ATP2A2; less dyskeratosis; no corps ronds; negative DIF |
| Differs from pemphigus vulgaris | DIF negative; no antibodies; autosomal dominant; not autoimmune |
| Nikolsky sign | Positive (epidermal acantholysis) |
| Specific nail sign | Longitudinal leukonychia (white bands) |
| Best unique treatment | Botulinum toxin A (axillary disease) |
| Best surgical option | CO₂ laser / dermabrasion |
References:
- Andrews' Diseases of the Skin, 13th ed., p. 650
- Fitzpatrick's Dermatology, 9th ed. (Goldsmith et al.), Chapter 50
- Dermatology, 5th ed. (Bolognia, Schaffer & Cerroni), Chapter 59
Blau syndrome in 5marks format for 3rd yr dermatology post graduate theory examination
Finding Sources
Finding Sources
Your credits are exhausted. Your daily credits reset tomorrow, or you can purchase a top-up for more.
This is a shared conversation. Sign in to Orris to start your own chat.