1 Clinical anatomy of the organ of vision. Membranes of the organ of vision. Chambers of the eye. Accessory apparatus of the eye (eyelids, lacrimal organs).
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Finding Sources
Finding Sources
Reading File
Finding Sources
Reading File
Reading File
Reading File
Reading File
Finding Sources
Searching Images
anatomy of the eyeball layers membranes cross section
Reading File
Searching Images
eyelid anatomy layers tarsus conjunctiva orbicularis
I now have comprehensive information from the textbooks. Let me compile the complete answer.
Clinical Anatomy of the Organ of Vision
1. The Eyeball — Overview
The globe-shaped eyeball occupies the anterior part of the orbit. Its rounded shape is disrupted anteriorly, where it bulges outward — this projection represents about one-sixth of the total eyeball surface and corresponds to the transparent cornea.
From front to back, the internal contents are arranged:
- Anterior chamber → iris/pupil → posterior chamber → lens → vitreous (postremal) chamber → retina
The eyeball is surrounded by the fascial sheath of the eyeball (bulbar fascia/Tenon's capsule), which encloses the scleral surface from the optic nerve entrance posteriorly to the corneoscleral junction anteriorly. As extraocular muscles pass through it, their investing fascia blends with this sheath.
(Gray's Anatomy for Students)
2. Membranes (Walls/Tunics) of the Eyeball
The eyeball wall has three concentric layers:
Outer Fibrous Layer
| Component | Location | Features |
|---|---|---|
| Sclera | Posterior 5/6 | Opaque dense connective tissue; the "white of the eye"; pierced by vessels, nerves, and optic nerve posteriorly; attachment for extraocular muscles |
| Cornea | Anterior 1/6 | Transparent; allows light entry; continuous with sclera at the limbus (corneoscleral junction) |
Middle Vascular Layer (Uvea)
Three continuous parts from posterior to anterior:
| Component | Location | Features |
|---|---|---|
| Choroid | Posterior ~2/3 | Thin, highly vascular, pigmented; smaller vessels adjoin the retina, larger vessels lie peripherally; firmly attached to retina internally, loosely to sclera externally |
| Ciliary body | Between choroid and iris | Triangular ring; contains ciliary muscle (longitudinal, circular, radial smooth muscle fibers; parasympathetic via CN III) and ciliary processes (ridges projecting inward, attached to lens via zonular fibers / suspensory ligament). Contraction of ciliary muscle relaxes tension on the zonule → lens rounds up → accommodation for near vision. Ciliary processes also secrete aqueous humor |
| Iris | Anterior | Colored disc with central pupil; contains sphincter pupillae (circular fibers, parasympathetic → pupil constriction) and dilator pupillae (radial myoepithelial cells, sympathetic → pupil dilation) |
Inner Layer (Retina)
| Component | Location | Features |
|---|---|---|
| Optic (neural) retina | Posterior | Light-sensitive; two sub-layers: outer pigmented layer (attached to choroid) and inner neural layer (detaches in retinal detachment) |
| Non-visual retina | Anterior | Covers internal surface of ciliary body and iris; continues anteriorly as a non-functional epithelium |
| Ora serrata | Junction | Irregular line between optic and non-visual retina |
Key landmarks on the posterior retina:
- Optic disc — where optic nerve exits; no photoreceptors → physiological blind spot; central retinal artery branches here
- Macula lutea — lateral to disc; yellowish area with highest visual acuity
- Fovea centralis — central depression of the macula; thinnest area; dominated by cones (color, bright light); fewest rods
(Gray's Anatomy for Students)
3. Chambers of the Eye
Anterior Chamber
- Between cornea (anteriorly) and iris (posteriorly)
- Contains aqueous humor
Posterior Chamber
- Between iris (anteriorly) and lens (posteriorly)
- Smaller than the anterior chamber
- Also contains aqueous humor
Communication & Aqueous Humor Flow
The anterior and posterior chambers communicate through the pupillary opening. Aqueous humor is:
- Secreted by ciliary processes into the posterior chamber
- Flows anteriorly through the pupil into the anterior chamber
- Drained into the scleral venous sinus (Canal of Schlemm) — a circular venous channel at the iridocorneal angle (cornea–iris junction)
Functions of aqueous humor: supplies nutrients to the avascular cornea and lens; maintains intraocular pressure (IOP).
Glaucoma results when this cycle is disturbed and IOP rises, threatening visual function.
Vitreous (Postremal) Chamber
- Occupies the posterior 4/5 of the eyeball, between lens and retina
- Filled with the vitreous body — a transparent, gelatinous substance
- Unlike aqueous humor, the vitreous cannot be replaced once lost
(Gray's Anatomy for Students)
4. Accessory Apparatus of the Eye
4a. Eyelids (Palpebrae)
The eyelids are the protective coverings of the eye. They consist of anterior and posterior lamellae:
Palpebral fissure dimensions (normal): horizontal 28–30 mm; vertical 9–10 mm. Upper lid margin sits midway between the superior limbus and pupil; lower lid margin abuts the inferior limbus.
Anterior Lamella
| Structure | Details |
|---|---|
| Skin | Thinnest skin of the body; highly vascular; minimal reticular dermis; heals rapidly with minimal scar |
| Orbicularis oculi | Subcutaneous sphincter of the eyelid; innervated by temporal and zygomatic branches of CN VII (facial nerve); three segments: pretarsal (involuntary blinking), preseptal (forced closure), orbital (tight/voluntary closure). Also drives the lacrimal pump — pumps tears into the puncta during blinking. Failure (e.g., facial nerve palsy) → epiphora |
Orbital Septum
- A fibrous sheet forming the anterior boundary of the orbit; extension of orbital periosteum from the arcus marginalis
- Acts as a barrier to spread of infection between preseptal and orbital spaces
Posterior Lamella
| Structure | Details |
|---|---|
| Tarsus (tarsal plates) | Dense fibrous plates that give rigidity to the eyelids; contain Meibomian (tarsal) glands (modified sebaceous glands) |
| Conjunctiva | Thin, transparent mucous membrane; palpebral conjunctiva lines the inner eyelid; reflects at the fornix to become bulbar conjunctiva over the sclera |
Upper Eyelid Retractors
- Levator palpebrae superioris — main upper lid elevator; originates from lesser wing of sphenoid at orbital apex; innervated by CN III (oculomotor)
- Müller's muscle (superior tarsal muscle) — sympathetic innervation; contributes ~2 mm of lid elevation
- Lid crease — formed by insertion of levator aponeurosis into orbicularis/skin; 10–12 mm above lid margin in women, 7–8 mm in men
Lower Eyelid Retractors
- Capsulopalpebral fascia — analogue of the levator aponeurosis; inserts into the inferior tarsus and anterior surface of the lower lid retractors
- Inferior tarsal muscle — sympathetic supply; analogous to Müller's muscle
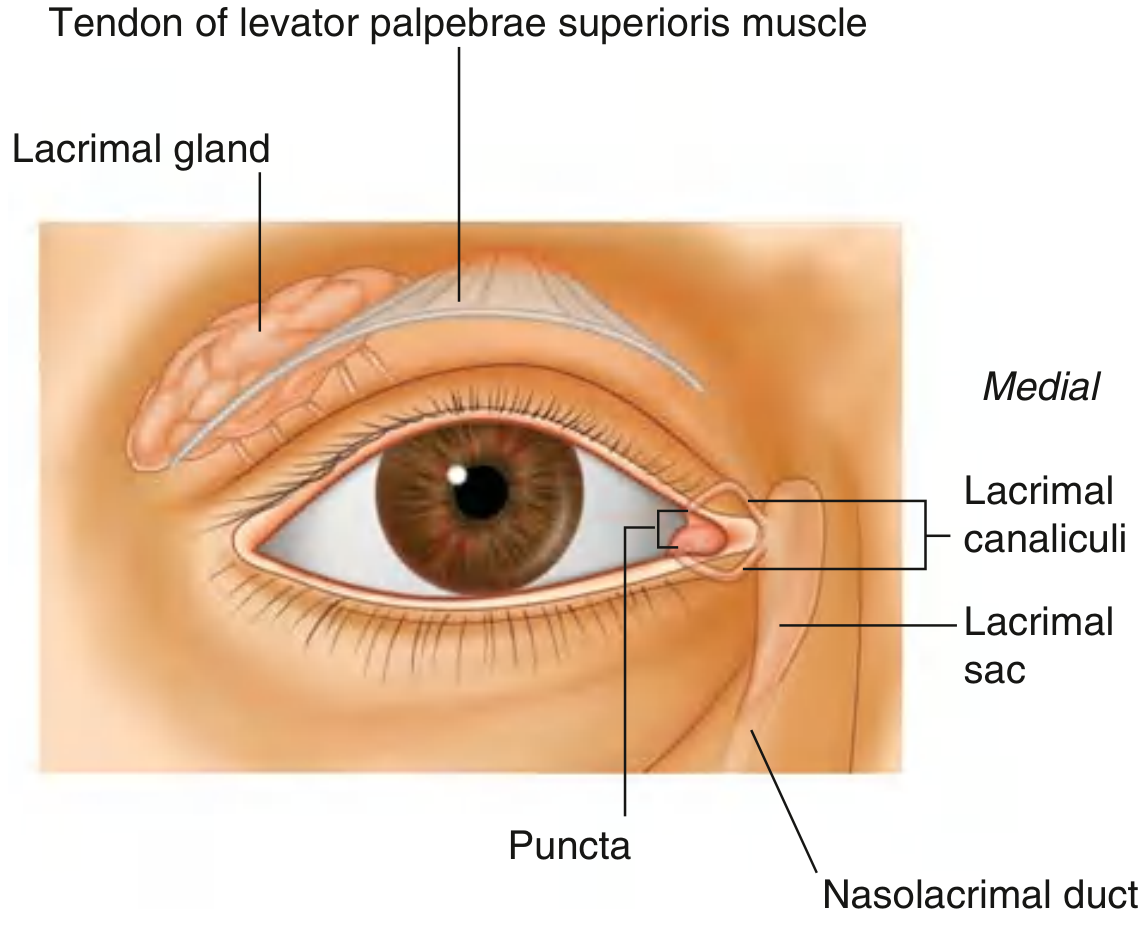
4b. Lacrimal Apparatus
The lacrimal apparatus produces, moves, and drains fluid from the ocular surface. It consists of:
| Component | Location/Structure |
|---|---|
| Lacrimal gland | Superolateral orbit; divided by levator palpebrae superioris into orbital part (larger, in lacrimal fossa of frontal bone) and palpebral part (smaller, in superolateral eyelid); secretions drain via numerous ducts into the lateral superior conjunctival fornix |
| Lacrimal canaliculi | One per eyelid; fluid enters through the lacrimal punctum at the medial edge of each lid; canaliculi pass medially to join the lacrimal sac |
| Lacrimal sac | Lies in the lacrimal fossa between anterior and posterior lacrimal crests, posterior to the medial palpebral ligament; when orbicularis oculi contracts during blinking, the lacrimal portion dilates the sac → draws tears in through canaliculi |
| Nasolacrimal duct | Drains from lacrimal sac inferiorly to open into the inferior meatus of the nasal cavity (under the inferior nasal concha) |
Tear flow direction: Lacrimal gland → lateral fornix → across eye surface (lateral → medial via blinking) → lacrimal lake → lacrimal puncta → canaliculi → lacrimal sac → nasolacrimal duct → inferior nasal meatus
Innervation of the Lacrimal Gland
| Type | Pathway |
|---|---|
| Sensory | Lacrimal branch of ophthalmic nerve (V1) |
| Secretomotor (parasympathetic) | Preganglionic from superior salivatory nucleus → via CN VII (greater petrosal nerve) → pterygopalatine ganglion → postganglionic fibers travel with zygomatic nerve (V2) then via communicating branch to the lacrimal nerve (V1) |
| Sympathetic | From superior cervical ganglion via the internal carotid plexus; reduces secretion |
(Gray's Anatomy for Students)
Summary Table: Eyeball Tunics
| Layer | Components | Function |
|---|---|---|
| Outer fibrous (tunica fibrosa) | Sclera, Cornea | Protection, shape maintenance, light refraction |
| Middle vascular (tunica vasculosa / uvea) | Choroid, Ciliary body, Iris | Nutrition, accommodation, pupil control |
| Inner nervous (tunica interna) | Retina (optic + non-visual) | Light transduction, image formation |
This is a shared conversation. Sign in to Orris to start your own chat.