urtucarea
Reading File
Finding Sources
Searching PubMed
"urticaria"[MeSH Terms] AND "diagnosis OR management"
Searching the Web
urticaria clinical overview pathophysiology treatment 2025
Reading File
Reading File
Searching Images
urticaria hives skin wheal
Reading File
Reading File
Urticaria (Hives)
Urticaria — popularly known as hives — is one of the most common cutaneous reaction patterns, affecting 15–20% of the population at some point during their lifetime.
Definition & Classification
Urticaria presents as edematous wheals with pale centers and red borders, often intensely pruritic, with individual lesions typically transient (< 24 hours). It exists on a spectrum ranging from simple wheals to angioedema (deeper tissue swelling, present in ~40% of chronic cases).
| Type | Duration |
|---|---|
| Acute | < 6 weeks |
| Chronic | ≥ 6 weeks (often idiopathic) |
Chronic urticaria peaks in women in the 3rd–4th decade; acute urticaria is common in children with atopic dermatitis.
Clinical Image
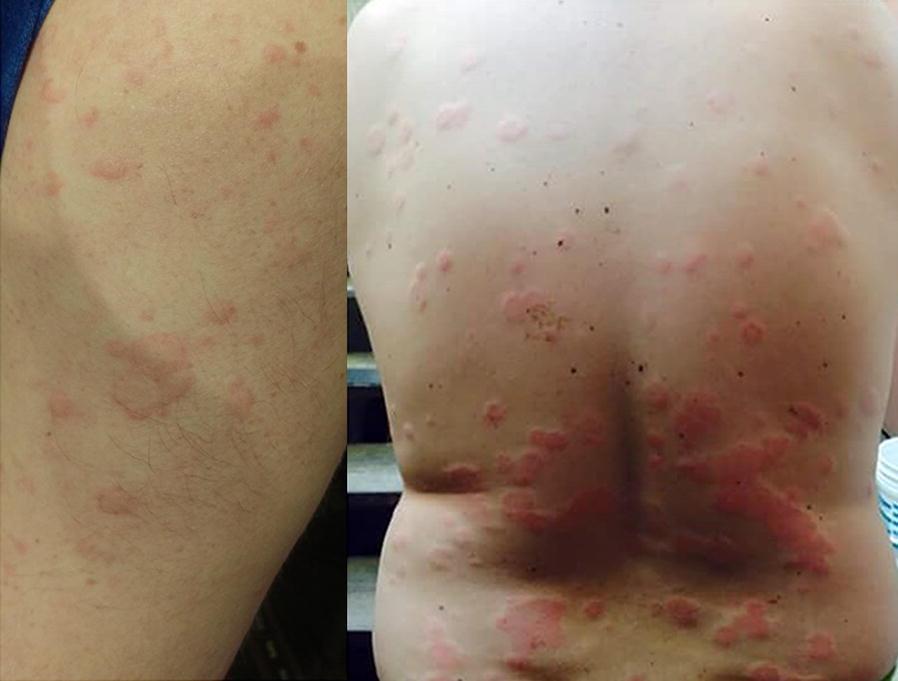
Classic urticaria: raised, edematous wheals with erythematous borders demonstrating the Lewis triple response.
Pathophysiology
Local mast cell degranulation releases histamine and other mediators (bradykinin, kallikrein, slow-reacting substance of anaphylaxis), causing localized dermal edema from transvascular fluid extravasation.
Mechanisms:
- Immunologic: IgE-dependent (classic allergy), immune complex-mediated, complement/kinin-dependent, autoimmune (functional IgE autoantibodies)
- Nonimmunologic: Direct mast cell degranulation by drugs or foods (aspirin, NSAIDs, opioids, strawberries, lobster)
Common Triggers
| Category | Examples |
|---|---|
| Drugs | Penicillin (most common), aspirin, NSAIDs, opioids |
| Foods | Seafood, tree nuts, eggs, shellfish |
| Infections | Rhinovirus, hepatitis, mononucleosis, coxsackievirus, Candida, parasites |
| Contact | Animal dander/saliva, latex, cosmetics, plants |
| Physical stimuli | Cold, heat, pressure, sunlight, exercise |
Special Physical Subtypes
- Cold urticaria – triggered by cold exposure; may be associated with cryoglobulinemia, syphilis, or connective tissue disease. Treat with antihistamines 30–60 min before cold exposure.
- Cholinergic urticaria – triggered by exercise, heat, emotional stress. Lesions are tiny (1–3 mm) with extensive erythematous flare. May cause nausea, abdominal pain, or headache.
- Solar urticaria – confined to sun-exposed skin; clears rapidly when light stimulus removed.
Differential Diagnosis
- Drug eruption / exanthems
- Erythema multiforme
- Erythema marginatum
- Urticarial vasculitis (lesions persist > 24 h, associated with systemic symptoms, hypocomplementemia)
- Juvenile rheumatoid arthritis
Treatment
Step-wise approach (EAACI/JAACI guidelines):
- Remove the trigger (when identifiable)
- Non-sedating H1 antihistamines (first-line): cetirizine, fexofenadine, loratadine
- Dose can be up-titrated up to 4× in chronic urticaria
- Add H2 blocker (e.g., ranitidine/famotidine) if H1 alone insufficient
- Short course corticosteroids (prednisone/dexamethasone) for moderate–severe or recurrent episodes (14–21 days with taper; chronic use not recommended)
- Refractory chronic urticaria:
- Omalizumab (anti-IgE monoclonal antibody) — approved since 2014 for CSU ≥12 years
- Cyclosporine — effective for severe refractory cases
- Dupilumab — FDA-approved April 2025 for CSU ≥12 years unresponsive to antihistamines (promising especially in patients with comorbid atopic disease)
Recent Evidence
A 2025 network meta-analysis (PMID 40663028) compared biologics and systemic immunomodulatory agents for chronic urticaria, providing updated ranking of treatment options. A 2024 systematic review (PMID 38420865) reviewed acute urticaria treatment specifically.
Sources: Rosen's Emergency Medicine, Goldman-Cecil Medicine (9780323757898; 9780323930345)
This is a shared conversation. Sign in to Orris to start your own chat.