Hip tb full details for md exam answer 15 marks
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Running Command
Running Command
Running Command
Running Command
Running Command
Running Command
Searching Images
hip tuberculosis X-ray radiograph stages arthritis
I now have everything needed for a comprehensive, exam-ready 15-mark answer. Here it is:
Tuberculosis of the Hip Joint — Complete MD Exam Answer (15 Marks)
1. Introduction & Epidemiology
Tuberculosis (TB) of the hip joint is the second most common site of osteoarticular TB after spinal TB. It accounts for 15–20% of all osteoarticular TB cases. It predominantly affects children, but is also seen in young adults. Constitutional symptoms (evening fever, weight loss, night sweats, malaise) typically precede joint symptoms. Evidence of concurrent or prior pulmonary TB is found in approximately 50% of patients.
2. Pathology
Site of Initial Focus
TB of the hip almost always starts in bone. The initial focus may be in the:
- Acetabular roof (most common)
- Femoral epiphysis
- Proximal femoral metaphysis
- Greater trochanter (may involve the trochanteric bursa)
- Rarely, initial focus is in the synovial membrane
Since the head and neck of femur are intracapsular, a bony lesion here invades the joint early and later spreads to involve the acetabulum as well. When the disease starts in the acetabulum, symptoms of joint involvement appear late. Extensive destruction may result in pathological dislocation.
Pathological Process
- Infection begins in subchondral bone → granulation tissue forms → caseation necrosis
- Spreads to synovium, cartilage, capsule, and joint space
- A cold abscess forms in the joint → may perforate the capsule and extend anywhere around the hip
- May perforate the thinned acetabular floor → intrapelvic abscess
- Secondary pyogenic infection can occur through sinus tracts
3. Clinical Features — Three Clinico-pathological Stages
Stage I: Stage of Synovitis
- Earliest manifestation; intra-synovial effusion and exudate distend the capsule
- Hip assumes position of flexion, abduction and external rotation (position of maximum joint capacity)
- Apparent lengthening of limb (no true lengthening)
- Night cries — relaxation of muscle spasm during sleep allows painful unguarded movements
- Often misdiagnosed at this stage (DDx: traumatic synovitis, transient synovitis, rheumatic disease, low-grade pyogenic infection, Perthes' disease, iliopsoas abscess spasm)
- All movements painful and limited to variable degree
Stage II: Stage of Early Arthritis
- Capsule thickens by fibrosis and contracts; articular surface damage progresses
- Hip assumes position of flexion, adduction and internal rotation
- Apparent shortening (limb appears short); true shortening ≤1 cm
- All movements remain painful and limited
Stage III: Stage of Advanced Arthritis
- Capsule further destroyed → true shortening of limb
- Severe flexion–adduction–internal rotation deformity
- With destruction of acetabulum, femoral head, capsule and ligaments → pathological dislocation
- Femoral head migrates proximally and posteriorly → wandering/migrating acetabulum
- Alternatively, protrusio acetabuli develops with medial wall destruction
Symptoms (All Stages)
- Pain: around hip, along thigh, or referred to inner aspect of knee (first symptom)
- Limp and avoidance of weight bearing
- Muscle spasm (severe in acute stage)
- Night cries (early feature)
- Muscle atrophy (develops as acute stage subsides)
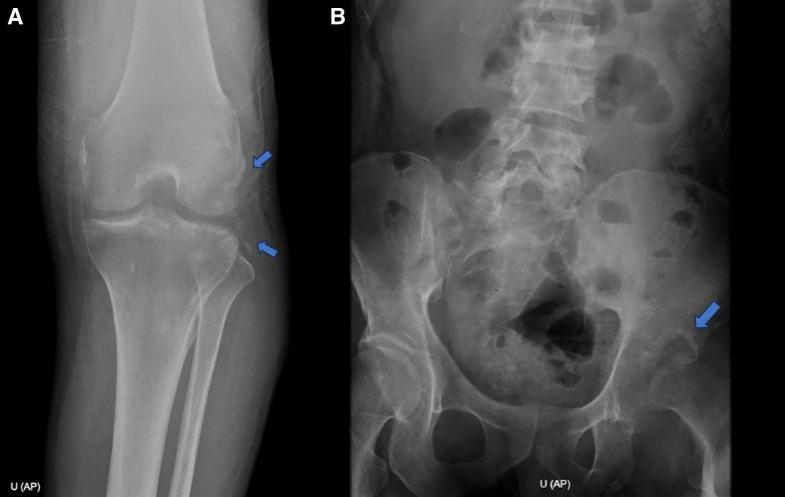
4. Radiographic Features
Early Stage
- Diffuse decalcification of upper end of femur
- Osteolytic bony focus in acetabulum or femoral head
- Soft tissue swelling (ultrasonography useful at this stage)
Seven Radiological Types (Advanced Stage — Bhan & Nag classification)
| Type | Features |
|---|---|
| Normal | Mainly synovial; cysts in femoral neck/head/acetabulum; joint space normal; no gross subchondral bone destruction |
| Perthes' Type | Mainly <5 years; whole femoral head sclerotic; no metaphyseal changes (differentiates from true Perthes') |
| Dislocating Type | Subluxation/dislocation of femoral head; due to capsular laxity and synovial hypertrophy (not pus accumulation) |
| Wandering Acetabulum | Erosion of subchondral bone; results are poor; duration of symptoms 10–14 months |
| Protrusio Acetabuli | Medial acetabular wall destruction; poor surgical results |
| Mortar and Pestle Type | Erosion of subchondral bone; similar poor prognosis |
| Atrophic Type | Irregular femoral head; narrow joint space; seen in adults; almost always progresses to fibrous ankylosis; very poor results |
In Normal, Perthes', and Dislocating types — mean symptom duration: 4–7 months. In Wandering acetabulum, Protrusio, Mortar-and-Pestle types — mean duration: 10–14 months.
Late Stage
- Increasing destruction of acetabulum
- Subluxation or dislocation
- Small atrophic femoral head
5. Investigations
| Investigation | Findings |
|---|---|
| X-ray hip | As above; early: soft tissue swelling + osteopenia; late: joint destruction |
| Ultrasonography | Confirms soft tissue swelling and joint effusion in early stage |
| CT scan | Detects extent of bony destruction, cold abscess, early lesions |
| MRI | Most sensitive; identifies early soft tissue and bony lesions; 100% sensitivity, 88% specificity for osteoarticular TB |
| Synovial fluid | Thick appearance, high protein, variable (usually lymphocytic) cell count; AFB smear usually negative; culture positive in high % |
| Synovial biopsy | Shows caseating granulomas with Langhans giant cells; most definitive |
| CBNAAT (Xpert MTB/RIF) | Pooled sensitivity 94.6% and specificity 85.3% in bone/joint tissue; increasingly used |
| ESR, CRP | Elevated; non-specific |
| Mantoux/TST | Positive in most; not diagnostic |
6. Differential Diagnosis
| Condition | Distinguishing Features |
|---|---|
| Perthes' disease | Children <10 yrs; metaphyseal changes present; no constitutional symptoms |
| Septic arthritis (pyogenic) | Acute onset; high fever; rapid destruction; organisms on culture |
| Rheumatoid arthritis | Polyarticular; bilateral; RF positive; systemic features |
| Transient synovitis | Self-limiting; younger children; no systemic features |
| Congenital dislocation of hip | From birth; no constitutional symptoms; no bone destruction |
| Osteoarthritis | Elderly; no constitutional symptoms; different X-ray pattern |
7. Management
Prognosis Depends on Stage at Diagnosis
- Anti-TB treatment started at Stage I or II → near-normal hip joint possible
- Neglected cases → markedly deformed hip, short limb (due to bony destruction + growth arrest at proximal femoral epiphysis)
A. Anti-TB Treatment
- Standard 2HRZE / 10HRE regimen (or as per INDEX-TB guidelines):
- Intensive phase: 2 months — Isoniazid (H) + Rifampicin (R) + Pyrazinamide (Z) + Ethambutol (E)
- Continuation phase: 10–16 months — H + R + E (extended for skeletal TB, total 12–18 months)
- Many orthopaedicians favour 18–24 months for hip TB
- DOTS to ensure compliance
B. General Supportive Measures
- Improve nutritional status
- Treat associated conditions
C. Skin Traction
- Required initially in all cases
- Corrects deformity, relieves muscle spasm and pain
- Maintains joint space, minimises migrating acetabulum, prevents dislocation
- In abduction deformity: apply traction to both limbs to stabilise pelvis
- Stages I & II: prolonged traction (up to 12 weeks)
- Continue until disease activity well-controlled, movements improve and are pain-free
D. Weight Bearing Protocol
- 12 weeks traction → 12 weeks non-weight bearing with crutches → 12 weeks partial weight bearing → then unprotected weight bearing
E. Surgical Treatment
Stage II (Early Arthritis):
- Partial synovectomy and curettage of large/enlarging osteolytic lesions in acetabulum and femoral head
- Large lesions may be filled with cancellous bone grafts
- Hip joint should not be dislocated during surgery to avoid spread
Stage III (Advanced Arthritis):
- Aim: achieve fibrous ankylosis in functional position
- Partial synovectomy + curettage of extra-articular lesions + joint debridement
- After deformity correction → plaster spica for 6–9 months
- Then partial weight bearing for another 6 months
- Unprotected weight bearing usually possible after 12–18 months from start
Corrective Osteotomy:
- Proximal femoral osteotomy (above lesser trochanter) for ankylosis in unacceptable position
- Converts painful fibrous ankylosis → painless bony ankylosis
Arthrodesis:
- Bony ankylosis, done after 20 years of age (no more growth potential)
- Intra-articular fusion between raw surfaces of femoral head and acetabulum
- Methods: Iliofemoral (Hibb's) arthrodesis; Ischiofemoral (Britain's) arthrodesis (historical)
Excision Arthroplasty (Girdlestone):
- Excision of head and neck of femur + debridement
- Post-op: 10–12 weeks traction → gradual weight bearing
- Limb becomes 2 cm shorter + joint unstable; advantage: preserves range of motion (patient can squat and sit cross-legged)
Total Hip Arthroplasty (THA):
- In selected patients; disease must be clinically healed for >5 years
- Currently also performed in active TB (controversial) with anti-TB treatment cover
F. Drainage of Cold Abscess
- Done without undue delay to prevent sinus formation
8. Complications
- Pathological dislocation of hip
- Wandering/migrating acetabulum
- Fibrous ankylosis in deformity
- Limb shortening (bony destruction + growth arrest)
- Cold abscess and sinus formation
- Secondary pyogenic infection through sinuses
- Premature epiphyseal fusion
9. Summary Box — Key Points for Exam
| Feature | Detail |
|---|---|
| Incidence | 15–20% of osteoarticular TB |
| Common age | Children (also young adults) |
| Initial site | Acetabular roof most common |
| Stage I deformity | Flexion + Abduction + External rotation |
| Stage II deformity | Flexion + Adduction + Internal rotation |
| X-ray classification | 7 types (Normal, Perthes, Dislocating, Wandering acetabulum, Protrusio, Mortar & Pestle, Atrophic) |
| Best diagnostic tool | MRI (100% sensitivity) |
| Gold standard | Synovial biopsy + culture |
| CBNAAT | Xpert MTB/RIF: 94.6% sensitivity in bone/joint tissue |
| Treatment duration | 12–18 months (some 18–24 months) |
| Key surgical procedure | Girdlestone (excision arthroplasty) / Arthrodesis |
| THA prerequisite | Disease healed >5 years |
Sources:
- Textbook of Tuberculosis and Nontuberculous Mycobacterial Diseases, 3rd Ed. — Sharma & Mohan, Chapter 19: Skeletal Tuberculosis (S Bhan, HL Nag), pp. 267–293
- Harrison's Principles of Internal Medicine, 22nd Ed. — Skeletal TB, p. 1432
- Murray & Nadel's Textbook of Respiratory Medicine — Bone and Joint TB, p. 1199
- Rosen's Emergency Medicine — Bone and Joint Infection
Give crisp and consise structured answer
TB Hip — MD Exam Answer (15 Marks)
Definition & Incidence
- 2nd most common site of osteoarticular TB after spine
- 15–20% of all osteoarticular TB cases
- Predominantly affects children; concurrent/prior pulmonary TB in ~50%
Pathology
Site of initial focus (in order):
- Acetabular roof (most common)
- Femoral epiphysis
- Proximal femoral metaphysis
- Greater trochanter
- Rarely — synovial membrane
Sequence: Bone focus → granulation tissue → caseation → spreads to cartilage, synovium, capsule → cold abscess → perforation of capsule → sinus/intrapelvic abscess
Head and neck of femur are intracapsular → bony lesion here invades joint early; acetabular lesion invades joint late
Clinical Features — Three Stages
| Stage I: Synovitis | Stage II: Early Arthritis | Stage III: Advanced Arthritis | |
|---|---|---|---|
| Deformity | Flexion + Abduction + External rotation | Flexion + Adduction + Internal rotation | Flexion + Adduction + IR (severe) |
| Limb length | Apparent lengthening | Apparent shortening (true ≤1 cm) | True shortening |
| Capsule | Distended by effusion | Fibrotic, contracting | Destroyed |
| Joint | Max capacity position | Damaged articular surface | Pathological dislocation |
Common symptoms (all stages):
- Pain in hip/thigh or referred to medial knee
- Limp, avoidance of weight bearing
- Night cries (muscle spasm relaxes during sleep)
- Muscle atrophy, restricted movements
Radiological Classification (7 Types — Bhan & Nag)
| Type | Feature | Prognosis |
|---|---|---|
| Normal | Mainly synovial; joint space preserved | Good |
| Perthes' | Sclerotic femoral head; children <5 yrs | Good |
| Dislocating | Subluxation/dislocation; due to capsular laxity | Good (open relocation) |
| Wandering acetabulum | Subchondral bone erosion | Poor |
| Protrusio acetabuli | Medial acetabular wall destroyed | Poor |
| Mortar & Pestle | Erosion of subchondral bone | Poor |
| Atrophic | Irregular femoral head; narrow joint space; adults only | Very poor → fibrous ankylosis |
Normal/Perthes'/Dislocating → symptom duration 4–7 months Wandering/Protrusio/Mortar & Pestle → duration 10–14 months
Investigations
| Test | Finding |
|---|---|
| X-ray | Osteopenia → osteolytic focus → joint destruction |
| USG | Early soft tissue swelling, effusion |
| MRI | Best early imaging; 100% sensitivity, 88% specificity |
| Synovial fluid | Thick; high protein; lymphocytic; culture positive in most |
| Synovial biopsy | Caseating granuloma + Langhans giant cells — gold standard |
| CBNAAT (Xpert MTB/RIF) | Sensitivity 94.6%, specificity 85.3% in bone/joint tissue |
Differential Diagnosis
Perthes' disease · Septic arthritis · Transient synovitis · Rheumatoid arthritis · CDH · Osteoarthritis
Management
1. Anti-TB Treatment
- 2HRZE / 10–16HRE (total 12–18 months; many orthopaedicians prefer 18–24 months)
- DOTS compliance mandatory
2. Skin Traction (all stages initially)
- Corrects deformity, relieves spasm, maintains joint space, prevents dislocation
- Abduction deformity → traction to both limbs
- Stages I & II: up to 12 weeks traction
3. Weight-Bearing Protocol
12 weeks traction → 12 weeks NWB with crutches → 12 weeks partial WB → unprotected WB
4. Surgery
| Stage | Procedure |
|---|---|
| Stage II | Partial synovectomy + curettage of osteolytic lesions ± cancellous bone graft |
| Stage III | Synovectomy + debridement → plaster spica 6–9 months → aim: fibrous ankylosis in functional position |
| Ankylosis in bad position | Corrective femoral osteotomy (above lesser trochanter) |
| After age 20, ankylosis needed | Arthrodesis — Hibb's (iliofemoral) or Britain's (ischiofemoral) |
| Painful hip, preserve ROM | Excision arthroplasty (Girdlestone) — excise head & neck; limb 2 cm short but patient can squat |
| Healed >5 years / selected active cases | Total Hip Arthroplasty (THA) |
5. Cold Abscess
Drain promptly to prevent sinus formation
Complications
- Pathological dislocation · Wandering acetabulum · Cold abscess & sinuses
- Limb shortening (bone destruction + growth arrest) · Secondary pyogenic infection · Fibrous ankylosis in deformity
Rapid Recall
Stage I = FAb+ER (like resting position) → apparent long Stage II = FAd+IR (like antalgic guard) → apparent short Stage III = same + true shortening + dislocation MRI = best early; biopsy = gold standard; CBNAAT = rapid molecular
— Sharma & Mohan, Textbook of TB, 3rd Ed., Chapter 19 (Bhan & Nag); Harrison's 22e
This is a shared conversation. Sign in to Orris to start your own chat.