Squint
Reading File
Finding Sources
Searching the Web
squint strabismus overview types causes treatment
Finding Sources
Reading File
Finding Sources
Reading File
Finding Sources
Loading Image
Reading File
Reading File
Reading File
Here is a comprehensive overview of squint (strabismus):
Squint (Strabismus)
Squint, medically termed strabismus, is the misalignment of the eyes — meaning the visual axes of the two eyes do not point at the same object simultaneously.
Types
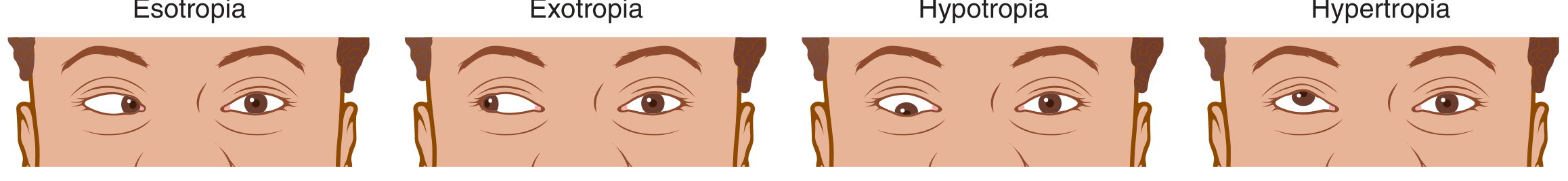
| Type | Direction of deviation |
|---|---|
| Esotropia | Eye turns inward ("crossed eyes") |
| Exotropia | Eye turns outward ("wall-eye") |
| Hypertropia | Eye turns upward |
| Hypotropia | Eye turns downward |
Deviations can also be horizontal, vertical, or rotational (cyclotorsional).
Epidemiology
- Strabismus affects ~4% of the population
- Half of all amblyopia patients have a concurrent strabismus
- Esotropia accounts for ~45–50% of cases; congenital esotropia ~20%
Causes & Pathophysiology
Strabismus results from failure of the six extraocular muscles to coordinate both eyes for single binocular vision. Specific causes include:
- Neuromuscular abnormalities — affecting oculomotor nuclei (CN III, IV, VI), their nerves, or the muscles themselves
- Refractive errors — especially hyperopia leading to accommodative esotropia
- Anatomic anomalies — congenital muscle or orbital abnormalities
- Abnormal fusion development — in early childhood, one eye may fail to fixate correctly, locking in a misalignment pattern
- Acquired causes — diabetes mellitus, stroke, brain tumors, trauma, cranial nerve palsies (e.g., viral URI → CN VI palsy)
- Retinoblastoma — strabismus may be its presenting sign
Pseudostrabismus is a false appearance of crossing due to a flat nasal bridge or epicanthal skin folds — not a true misalignment. Children do not "grow out of" real strabismus.
Consequences
Amblyopia ("lazy eye") is the key complication. When one eye is suppressed by the brain to avoid diplopia, that eye's visual acuity fails to develop, potentially resulting in permanent vision loss (20/400 or worse). It is the most common cause of unilateral vision loss in children under 4 years.
- Reversible if treated before age 7–13 years
- Visual cortex synaptogenesis depends on balanced input from both eyes
Adults with newly acquired strabismus develop diplopia rather than suppression, because the brain's plasticity has closed.
Diagnosis
Four key tests:
- Corneal light reflex (Hirschberg test) — penlight shone at both eyes; a symmetric reflex indicates alignment. Asymmetric = deviation
- Cover test — one eye is covered; movement of the uncovered eye indicates it was deviated. Inward movement → exotropia; outward → esotropia
- Red reflex test — asymmetric or white reflex signals media opacity, high refractive error, or retinoblastoma
- Extraocular movements — tested in the cardinal positions of gaze
Treatment
| Modality | Indication |
|---|---|
| Spectacle correction | Accommodative esotropia, refractive errors |
| Patching / atropine drops | Amblyopia — occlude the better eye to force use of the weaker eye |
| Botulinum toxin injection | Selected cases of strabismus |
| Strabismus surgery | Congenital esotropia (6–12 months of age), large exotropia/hypertropia |
| Prism glasses | Small deviations, diplopia management |
Patching and atropine have equal efficacy for amblyopia if started before age 7. Earlier diagnosis yields better prognosis.
Sources: Guyton & Hall Textbook of Medical Physiology; Goldman-Cecil Medicine; Textbook of Family Medicine 9e
This is a shared conversation. Sign in to Orris to start your own chat.