What's milliary Tb
Reading File
Finding Sources
Searching PubMed
"miliary tuberculosis"[MeSH Terms]
Searching Images
miliary tuberculosis chest X-ray CT scan
Reading File
Reading File
Finding Sources
Reading File
Reading File
Reading File
I now have comprehensive information from multiple authoritative textbooks. Let me compile a thorough answer.
Miliary Tuberculosis
Definition & Name Origin
"Miliary" TB gets its name from the Latin milium (millet seed) — referring to the gross appearance of the lung, which is studded with countless 1–3 mm yellow-white nodules resembling millet seeds. Today the term refers to wide hematogenous dissemination of Mycobacterium tuberculosis, seeding multiple organs simultaneously. — Tintinalli's Emergency Medicine, p. 498; Robbins & Cotran Pathologic Basis of Disease
Pathogenesis
When TB progresses beyond local control, organisms drain through lymphatics into the venous blood and circulate back to the lungs (pulmonary miliary TB), or disseminate through the systemic arterial system (systemic miliary TB). This can happen during:
- Primary TB (in children, the immunocompromised, or those with impaired cell-mediated immunity)
- Reactivation TB (breakdown of a previously contained focus)
Systemic miliary TB seeds the liver, bone marrow, spleen, adrenals, meninges, kidneys, fallopian tubes, and epididymis — essentially any organ can be involved. — Robbins & Cotran
Who Gets It?
High-risk groups:
- Children and the elderly
- HIV/AIDS patients (most cutaneous cases occur here)
- Those with malnutrition or other immunocompromising conditions
- Post-viral immunosuppression (e.g., measles)
Because this represents uncontrolled hematogenous infection, the tuberculin skin test (TST/Mantoux) is characteristically negative — the immune system is too suppressed to mount a reaction. — Andrews' Diseases of the Skin
Clinical Features
Primary miliary TB tends to be rapid and severe, often presenting with:
- Multiorgan failure
- Shock
- ARDS
Reactivation miliary TB is more insidious and chronic:
- Fever, night sweats, weight loss, anorexia
- Nonproductive cough
- Splenomegaly, lymphadenopathy
- Signs of multisystem involvement
Key diagnostic clues:
- Choroidal tubercles on fundoscopy — pathognomonic for miliary TB
- Cutaneous lesions (seen especially in HIV): papules, vesiculopapules, erythematous macules/pustules, or purpuric "vasculitic" lesions (called tuberculosis cutis milaris disseminata)
The Jawetz microbiology case example illustrates the classic presentation: a 31-year-old Filipino immigrant with 7 weeks of malaise, myalgia, nonproductive cough, fever, 5 kg weight loss, anemia, thrombocytopenia, elevated liver enzymes, and coagulopathy — progressing to ARDS. Diagnosis was made by liver and bone marrow biopsy showing granulomas with giant cells and AFB. — Jawetz Melnick & Adelberg's Medical Microbiology
Imaging
Chest X-ray: Diffuse, symmetric 1–3 mm micronodular opacities ("miliary shadows") throughout both lung fields — the classic finding. May not appear until the disease has progressed.
CT chest (HRCT): More sensitive — shows countless small well-defined nodules with random distribution (no preference for perilymphatic or centrilobular regions), ground-glass opacities, and thickened interlobular septa.
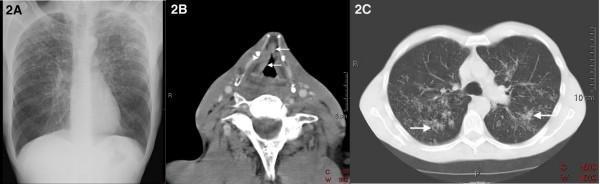
Chest X-ray (top left) showing bilateral upper lobe micronodular opacities, with HRCT confirming the miliary pattern and nodules with central cavitation.
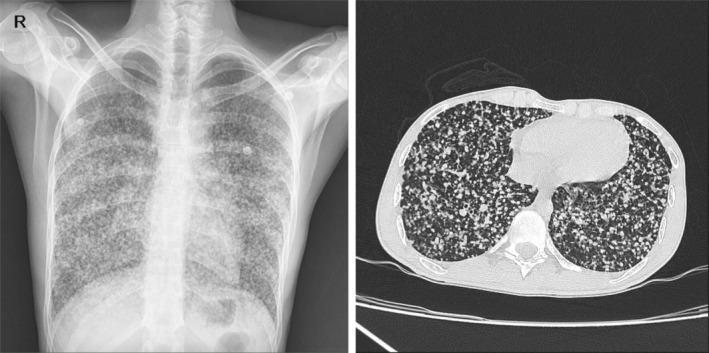
PA chest radiograph (left) and non-contrast CT (right) showing symmetric diffuse 1–3 mm micronodules with random distribution — the hallmark of miliary disease.
Differential for miliary pattern on imaging includes histoplasmosis, malignancy (miliary metastases), siderosis, and sarcoidosis. — Tintinalli's; Goldman-Cecil Medicine, Figure 295-6
Histopathology
- Diffuse suppurative inflammation of dermis/subcutis with PMNs ± abscess formation
- Caseating granulomas may be present
- AFB are abundant (unlike other forms of TB where AFB are scarce)
Complications
| Organ | Complication |
|---|---|
| Lungs | ARDS, respiratory failure |
| CNS | TB meningitis (often seeds after miliary infection), tuberculomas |
| Liver | Hepatitis, elevated transaminases |
| Bone marrow | Pancytopenia, anemia |
| Adrenals | Addison disease (formerly a major cause) |
| Vertebrae | Pott disease |
| Genitourinary | Renal TB, fallopian tube involvement, infertility |
| Pleura | Pleural effusion, empyema |
Diagnosis
- Sputum AFB smear and culture (may be negative)
- BAL (bronchoscopy)
- Bone marrow biopsy — highly useful
- Liver biopsy — granulomas + AFB
- Blood cultures (mycobacterial)
- TST/IGRA — often negative due to anergy
- Fundoscopy — look for choroidal tubercles
Treatment
Same backbone as pulmonary TB:
- Intensive phase (2 months): Isoniazid (INH) + Rifampicin + Pyrazinamide + Ethambutol (HRZE)
- Continuation phase (4–7 months): INH + Rifampicin
- Adjunctive corticosteroids are used for TB meningitis and pericarditis to reduce complications
- TB meningitis complicating miliary disease may require ventriculoperitoneal shunting in ~25% of patients for hydrocephalus
The prognosis is guarded — miliary TB carries higher mortality than localized pulmonary TB, especially when presenting with ARDS or multiorgan failure.
Sources: Tintinalli's Emergency Medicine; Goldman-Cecil Medicine; Robbins & Cotran Pathologic Basis of Disease; Andrews' Diseases of the Skin; Jawetz Melnick & Adelberg's Medical Microbiology
Surgery : orthopedic on fractures detailed notes
Reading File
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Finding Sources
Searching Images
fracture types transverse oblique spiral comminuted bone diagram
Reading File
Orthopedic Surgery: Fractures — Detailed Notes
1. DEFINITION
A fracture is a break in the continuity of bone. It may involve cortical bone, cancellous bone, or both, and may or may not communicate with the external environment.
2. FRACTURE DESCRIPTION — HOW TO REPORT A FRACTURE
Every fracture should be systematically described using the following framework (Rosen's Emergency Medicine):
| Parameter | Details |
|---|---|
| Open vs. closed | Does the fracture communicate with outside environment? |
| Bone + side | Name of bone, left vs. right |
| Location | Proximal / middle / distal third; specific region (e.g., humeral neck, tibial plateau) |
| Fracture line direction | Transverse, oblique, spiral, comminuted |
| Completeness | Complete (both cortices) vs. incomplete (one cortex intact) |
| Displacement | Position of distal fragment relative to proximal |
| Alignment/angulation | Valgus, varus, dorsal, volar, rotational |
| Articular involvement | % of articular surface affected |
| Modifiers | Avulsion, impaction, depression, compression, pathologic, stress |
3. FRACTURE TYPES BY FRACTURE LINE PATTERN
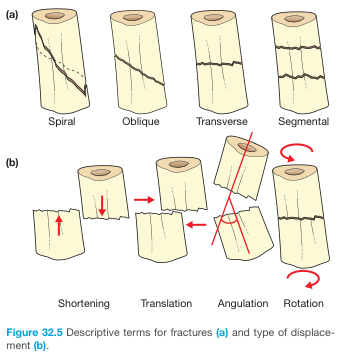
From Bailey & Love's Short Practice of Surgery — fracture patterns (A) and displacement types (B)
| Type | Description | Mechanism |
|---|---|---|
| Transverse | Right angle to long axis of bone | Direct blow / bending force |
| Oblique | Diagonal across the bone | Angulation + axial compression |
| Spiral | Encircles the shaft; appears longer on X-ray | Rotational / torsion force — note: in children, raises suspicion of abuse |
| Comminuted | >2 fragments | High-energy trauma |
| Segmental | Two fracture lines creating a free "floating" segment | High-energy |
| Greenstick | One cortex fractures, one bends (incomplete) | Children; bone still flexible |
| Torus (Buckle) | Bulging of cortex without discrete fracture line | Children; axial compression |
| Avulsion | Bone fragment pulled off by tendon/ligament | Sudden forceful contraction |
| Impaction | One fragment driven into another | Axial force (e.g., proximal humerus in elderly) |
| Stress (March/Fatigue) | Repeated low-intensity forces → bone resorption | Overuse — long-distance running, military recruits |
| Pathologic | Through diseased bone (tumor, cyst, metabolic disease) | Often trivial trauma |
4. DISPLACEMENT AND ALIGNMENT TERMINOLOGY
- Displacement: position of the distal fragment relative to the proximal (by convention); expressed as mm or % of bone width, or qualitatively (none/minimal/moderate/severe)
- Angulation: deviation of the longitudinal axis; described by the direction of the apex
- Valgus: apex toward the midline
- Varus: apex away from midline
- Shortening: fragment overlap reducing overall bone length
- Translation: lateral shift of fragments
- Rotation: twisting of the distal fragment — clinically check by observing the fingers in flexion (scissoring deformity)
5. FRACTURE CLASSIFICATION SYSTEMS
5a. AO/OTA Classification (Universal System)
The AO (Arbeitsgemeinschaft für Osteosynthesefragen) / OTA (Orthopaedic Trauma Association) alphanumeric system is the international standard. Each fracture is coded by:
- Bone number (e.g., 2 = humerus, 3 = radius/ulna, 32 = femur shaft)
- Segment (1 = proximal, 2 = diaphysis, 3 = distal)
- Fracture type (A = simple, B = wedge/partial articular, C = complex/complete articular)
Purposes: common language, treatment guidance, research, prognosis, AI/predictive analytics. — Rockwood & Green's Fractures in Adults (2025)
5b. Gustilo–Anderson Classification (Open Fractures)
| Grade | Description |
|---|---|
| I | Wound <1 cm, punctured from inside out, minimal contamination |
| II | Laceration 1–5 cm, no crush, no significant contamination |
| IIIA | >5 cm wound, extensive soft tissue but periosteum intact, coverage possible |
| IIIB | Periosteal stripping, extensive soft tissue loss, requires flap coverage |
| IIIC | Major vascular injury requiring repair (regardless of wound size) |
5c. Salter-Harris Classification (Physeal/Growth Plate Fractures in Children)
| Type | Description | Mnemonic |
|---|---|---|
| I | Through physis only (slipped) | S — Straight through |
| II | Fracture through physis + metaphysis (most common) | A — Above |
| III | Fracture through physis + epiphysis | L — Lower (epiphysis) |
| IV | Through metaphysis + physis + epiphysis | E — Everything |
| V | Crush/compression of physis (worst prognosis) | R — Rammed/crush |
6. FRACTURE HEALING — BIOLOGY
Stages of Fracture Healing (Secondary / Indirect Healing)
| Stage | Timeframe | Key Events |
|---|---|---|
| 1. Hematoma formation | Day 1–3 | Rupture of periosteal blood vessels → hematoma → procallus (no structural rigidity) |
| 2. Inflammatory phase | Days 1–7 | Macrophages, PMNs, cytokines (IL-1, IL-6, TNF); fracture line becomes more visible on X-ray at 10–14 days due to resorption + hyperemia |
| 3. Soft callus (fibrocartilaginous) | Weeks 2–4 | Periosteal + endosteal callus ("biologic splint"); mottled appearance on X-ray; swelling begins to regress |
| 4. Hard callus (bony bridging) | Weeks 4–12 | Callus mineralizes and ossifies; peripheral margins smooth out |
| 5. Remodeling | Months–years | Wolff's Law: bone remodels along lines of stress; eventually indistinguishable from mature bone |
Radiographic union indicators: abundant bridging callus, smooth peripheral margins, and no movement at fracture site. Even if the fracture line remains visible, clinical union may be present when the patient bears weight pain-free and cortices are bridged.
Timeframes for Union (approximate)
| Bone | Time to Union |
|---|---|
| Phalanx/small bones | 3–4 weeks |
| Radius/ulna | 6–8 weeks |
| Humerus | ~8 weeks |
| Tibia | 10–16 weeks |
| Femur | ~4 months |
Factors speeding healing: cancellous > cortical bone; oblique > transverse (more surface area + buttressing); appropriate weight-bearing; good apposition.
Factors slowing healing: corticosteroids, smoking, hyperthyroidism, malnutrition, immobilization, excessive/premature weight-bearing.
Primary (Direct) Healing
Occurs when fracture surfaces are held in anatomical reduction with absolute rigidity (e.g., compression plating). No visible callus forms — Haversian remodeling occurs directly across the fracture line. Requires exact reduction and rigid fixation.
Mechanobiology — Interfragmentary Strain Theory (Perren)
- Strain = deformation / original length
- High strain environment → granulation tissue / fibrous tissue
- Intermediate strain → fibrocartilage
- Low strain → bone formation
- Zero strain ≠ optimal — some motion/load is necessary to stimulate callus
- Simple fractures with bridge plating (rigid but not anatomically reduced) → high nonunion rates
- Dynamic locking implants that allow symmetric motion → improved callus formation — Rockwood & Green's
7. ABNORMAL FRACTURE HEALING
| Term | Definition |
|---|---|
| Delayed union | Union occurring slower than expected for that fracture type/location |
| Malunion | Fracture heals with residual deformity (angulation, rotation, shortening) |
| Nonunion | Complete failure to heal; defined radiographically as no progressive healing over 3–6 months |
| Pseudarthrosis | Nonunion resulting in a false joint with motion at the fracture site |
Types of nonunion:
- Hypertrophic (elephant foot): abundant callus, adequate vascularity — inadequate stability is the cause; treat with fixation
- Atrophic: no callus, poor vascularity — treat with bone graft + fixation
8. OPEN FRACTURES — EMERGENCY MANAGEMENT
Open fractures are true orthopedic emergencies due to the risk of osteomyelitis.
ED Management Steps:
- Control hemorrhage with sterile pressure dressing; remove gross debris
- Splint without reduction (unless vascular compromise)
- Irrigate with saline; cover with saline-soaked sponges
- Antibiotics as early as possible:
- Grade I: 1st-generation cephalosporin (cefazolin 2 g IV q8h)
- Grade II/III: add aminoglycoside (gentamicin 5 mg/kg OD) or broad-spectrum (piperacillin-tazobactam)
- Farm/fecal contamination: add ampicillin/penicillin (cover Clostridium)
- Tetanus prophylaxis (including TIG for large crush wounds)
- Surgical debridement + irrigation within 24 hours (the historical 6-hour rule is no longer strictly evidence-based)
- Stabilization (external fixator → definitive fixation)
Exception: Open distal tuft fractures of fingers/toes — ED irrigation + debridement usually sufficient without urgent consultation.
9. COMPLICATIONS OF FRACTURES
Immediate
| Complication | Key Points |
|---|---|
| Hemorrhage | Femur: ~1000 mL; Pelvis: 1500–3000 mL; Tibia/fibula: ~500 mL; Forearm: 150–250 mL. Splinting reduces blood loss. |
| Vascular injury | Popliteal artery with knee dislocation/distal femur; brachial artery with supracondylar humerus fracture in children |
| Nerve injury | See table below |
Nerve injuries associated with fractures:
| Fracture | Nerve at Risk |
|---|---|
| Distal radius (high energy) | Median nerve |
| Elbow fracture/dislocation | Median or ulnar nerve |
| Humeral shaft (mid/distal) | Radial nerve (Saturday night palsy pattern) |
| Shoulder dislocation | Axillary nerve |
| Sacral fracture | Cauda equina |
| Acetabular fracture | Sciatic nerve |
| Hip dislocation | Femoral nerve |
| Lateral tibial plateau | Peroneal nerve |
| Knee dislocation | Tibial or peroneal nerve |
Nerve injury classification (Seddon):
- Neuropraxia: contusion/traction, axon intact — recovers in weeks to months
- Axonotmesis: axon + myelin disrupted, connective tissue intact — Schwann tubes guide spontaneous recovery (delayed)
- Neurotmesis: complete severing of nerve + stroma — requires surgical repair
Early
Compartment Syndrome — Limb-threatening emergency
- Increased pressure within a closed fascial compartment → ischemia of muscle and nerves
- Most common after: tibial shaft fractures (40%), forearm fractures (18%)
- Classic signs: 5 P's — Pain (especially with passive stretch), Pressure (tense compartment), Paresthesia, Paralysis (late), Pallor/Pulselessness (very late)
- Compartment pressure >30 mmHg (or within 30 mmHg of diastolic pressure) = indication for fasciotomy
- Treatment: urgent four-compartment, two-incision fasciotomy (leg); wounds left open; negative pressure wound therapy; definitive fracture fixation follows
- Sequelae if missed: Volkmann's ischemic contracture, myonecrosis, rhabdomyolysis, renal failure, amputation
Infection / Osteomyelitis
- Primarily in open fractures
- Prophylactic antibiotics ± surgical debridement essential
Late
| Complication | Notes |
|---|---|
| Avascular necrosis (AVN) | Disruption of blood supply; classic in femoral head (hip dislocation/neck fracture), scaphoid, talus |
| Post-traumatic arthritis | Intra-articular fractures with >2 mm step-off |
| Malunion | Malalignment, limb length discrepancy, gait problems |
| Nonunion | Hypertrophic or atrophic |
| Reflex sympathetic dystrophy (CRPS) | Burning pain, swelling, skin changes, osteoporosis |
| Fat embolism syndrome | Long bone / pelvic fractures; classic triad: hypoxia + confusion + petechiae; treat with O2 + early fixation |
| DVT/PE | Especially pelvic, hip, femur fractures; prophylaxis mandatory |
| Myositis ossificans | Heterotopic ossification in soft tissue at fracture site |
10. FRACTURE TREATMENT PRINCIPLES
Goals of Treatment (The 4 R's)
- Recognition — history, clinical examination, imaging
- Reduction — restore normal anatomic alignment
- Retention — hold fragments in position until union
- Rehabilitation — restore function
Methods of Reduction
- Closed reduction: manipulation under anesthesia/sedation; splint/cast applied
- Open reduction: surgical exposure to achieve anatomic reduction
- Traction: skin or skeletal traction (less common now)
Methods of Fixation (Retention)
| Method | Details | Indication |
|---|---|---|
| Plaster/Cast | Non-operative; 3-point moulding | Stable, undisplaced fractures; children |
| Functional brace | Allows early joint motion | Humeral shaft, tibial shaft |
| Traction | Skin or skeletal (tibial pin, femoral pin) | Femoral shaft, pre-op temporizing |
| External fixation (EF) | Frame + transcutaneous pins/wires | Open fractures, polytrauma, damage control, infected nonunion |
| Intramedullary nail (IMN) | Rod through medullary canal, locked proximally and distally | Diaphyseal fractures: femur, tibia, humerus — "load-sharing" device |
| Plates & screws | Applied to bone surface | Periarticular fractures, forearm (requires anatomic reduction for rotation); "load-bearing" device |
| Cannulated screws | Percutaneous | Hip fractures (Garden I/II), scaphoid fractures |
| Arthroplasty (hemi/total) | Replace femoral head/hip | Displaced femoral neck fractures in elderly (Garden III/IV) |
Absolute Stability vs. Relative Stability
- Absolute stability (compression plate, lag screw): primary bone healing, no callus
- Relative stability (IMN, bridge plate, external fixator): secondary bone healing with callus — requires some motion
11. SPECIFIC IMPORTANT FRACTURES
Colles' Fracture
- Distal radius fracture with dorsal displacement and volar apex angulation → "dinner fork" deformity
- Mechanism: FOOSH (fall on outstretched hand) in extension
- Most common in osteoporotic elderly women
- May involve ulnar styloid
- Nerve at risk: median nerve
- Treatment: closed reduction + cast if acceptable alignment; ORIF if unstable or intra-articular
Smith's Fracture
- "Reverse Colles'" — volar displacement of distal radius
- Mechanism: fall on flexed wrist
- Inherently unstable → usually needs ORIF
Scaphoid Fracture
- Most common carpal fracture
- Mechanism: FOOSH in dorsiflexion
- Often X-ray negative initially → MRI or CT needed if clinical suspicion
- Risk of AVN of the proximal pole (tenuous blood supply from distal end)
- Treatment: undisplaced → thumb spica cast 8–12 weeks; displaced → ORIF with headless compression screw
Hip Fractures (Proximal Femur)
Classified by Garden classification:
| Grade | Description |
|---|---|
| I | Incomplete/valgus impacted — stable |
| II | Complete, undisplaced |
| III | Complete, partially displaced |
| IV | Complete, fully displaced |
- Garden I & II: cannulated screws or dynamic hip screw (DHS)
- Garden III & IV (elderly): hemiarthroplasty or total hip replacement; risk of AVN with fixation
- Intracapsular disrupts the medial femoral circumflex artery → AVN risk
- Intertrochanteric (extracapsular): DHS or cephalomedullary nail (CMN)
- Subtrochanteric: cephalomedullary nail
Femoral Shaft Fracture
- Requires high-energy trauma (MVA, fall from height)
- Blood loss ~1000 mL → monitor for hypovolemic shock
- Treatment: intramedullary nail (locked IM nail) — gold standard
- Nerve risk: peroneal nerve (from associated traction/positioning injury)
Tibial Shaft Fracture
- Most common long bone fracture requiring surgical treatment
- Scanty subcutaneous soft tissue → high risk of open fracture and compartment syndrome (40% of all compartment syndromes)
- Treatment: IM nail for displaced/unstable; cast for undisplaced
Pelvic Fractures
- Can cause catastrophic hemorrhage (1.5–3 L)
- Life-threatening: pelvic binder/sheet applied in the field for open-book fractures to close the pelvis
- Definitive: external fixation or internal fixation; interventional radiology embolization
Spinal Fractures (AO Spine Classification)
- Type A: Compression/burst — vertebral body compression
- Type B: Distraction — tension band injury
- Type C: Translational/rotational — most unstable
- Pott's disease = vertebral TB (collapse + kyphus)
- Neurological status guides urgency of intervention
12. PEDIATRIC-SPECIFIC CONSIDERATIONS
- Growth plate (physis) is the weakest area in children → Salter-Harris fractures
- Children's bones are more plastic → greenstick and torus fractures
- Remodeling potential is significant → greater tolerance for angulation (varies with age and proximity to physis)
- Spiral fractures in non-ambulatory children raise suspicion for non-accidental injury (child abuse)
- Supracondylar humerus fracture (most common elbow fracture in children): risk of anterior interosseous nerve injury and brachial artery injury → urgent reduction; "Gartland type III" needs emergency ORIF with K-wires
13. OSTEOPOROTIC (FRAGILITY/INSUFFICIENCY) FRACTURES
- Occur with low-energy trauma (from standing height or less)
- Common sites: distal radius, vertebrae, hip, proximal humerus
- Every fragility fracture mandates assessment and treatment for underlying osteoporosis
- Post-hip fracture: zoledronic acid or denosumab significantly reduce all-cause mortality
- Atypical femur fractures (AFFs): rare complication of long-term bisphosphonate use — lateral subtrochanteric, transverse, may be bilateral; prodromal thigh pain
14. LIFE-THREATENING & LIMB-THREATENING EMERGENCIES — SUMMARY TABLE
| Emergency | Complication |
|---|---|
| Open fracture | Osteomyelitis |
| Fracture/dislocation with vascular disruption (esp. popliteal) | Amputation |
| Major pelvic fracture | Exsanguination |
| Hip dislocation | AVN of femoral head |
| Compartment syndrome | Ischemic contracture; amputation; renal failure |
Sources: Rosen's Emergency Medicine (9th ed.); Rockwood and Green's Fractures in Adults (10th ed., 2025); Tintinalli's Emergency Medicine (9th ed.); Bailey & Love's Short Practice of Surgery (28th ed.)
Generate sets of possible questions in it with answers exam oriented
Your credits are exhausted. Your daily credits reset tomorrow, or you can purchase a top-up for more.
This is a shared conversation. Sign in to Orris to start your own chat.