Conjunctivitis children
Reading File
Finding Sources
Searching PubMed
conjunctivitis children management
Reading File
Reading File
Reading File
Finding Sources
Reading File
Reading File
Loading Image
I now have comprehensive information to provide a detailed, well-structured answer on conjunctivitis in children.
Conjunctivitis in Children
Conjunctivitis is inflammation of the conjunctiva and is one of the most common causes of the "red eye" in pediatric patients. The primary task clinically is to distinguish the common, self-limited forms from cases that risk vision loss.
Types and Clinical Features
1. Bacterial Conjunctivitis
Presentation: Painless, uni- or bilateral mucopurulent discharge causing eyelid adherence on waking. Conjunctiva is injected; cornea is clear; no preauricular lymphadenopathy (except in gonococcal infection).
Common pathogens in children:
- Staphylococcus and Streptococcus spp. (most common)
- Non-typeable Haemophilus influenzae (very common in school-age children)
- Pseudomonas (in contact lens wearers)
Management:
- Usually self-limited; antibiotics shorten the course
- First line: Trimethoprim-polymyxin B drops (avoids sulfa/neomycin allergy)
- Contact lens wearers: Fluoroquinolone (moxifloxacin, gatifloxacin, ofloxacin) or tobramycin to cover Pseudomonas
- Always perform fluorescein staining of the cornea in infants to exclude corneal abrasion, ulcer, or herpetic dendrite
- Culture discharge in severe cases
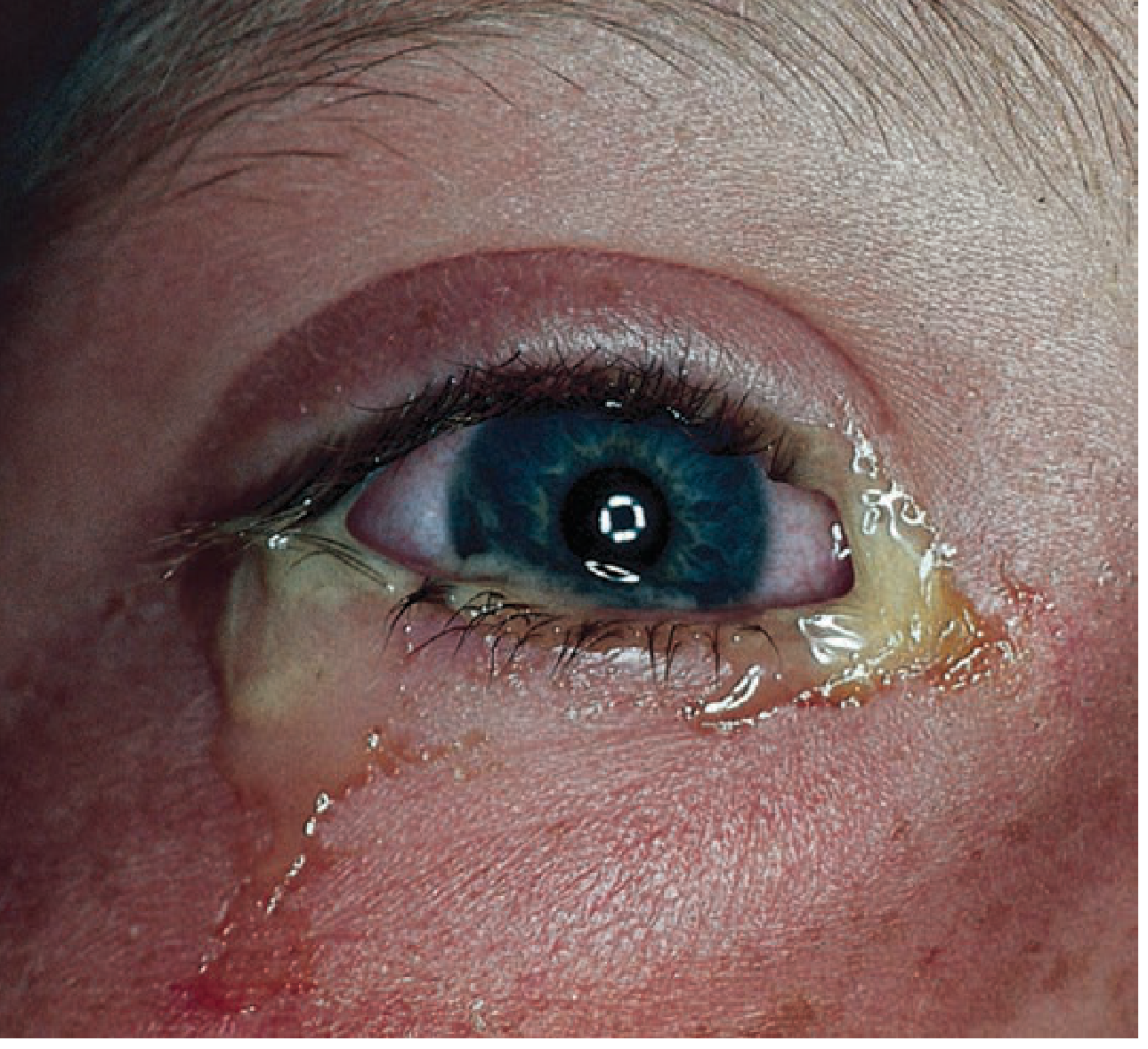
2. Viral Conjunctivitis
Most common cause: Adenovirus. Epidemic keratoconjunctivitis (EKC) is a severe, highly contagious adenoviral form.
Presentation:
- Watery discharge, no eye pain (unless keratitis)
- Starts unilateral → spreads to other eye within days
- Preauricular lymphadenopathy (distinguishes from bacterial)
- Follicles on inferior palpebral conjunctiva on slit-lamp exam
- URI may precede it; EKC may include fever, malaise, myalgias
Management (supportive):
- Cool compresses
- Ocular decongestants (e.g., Naphcon-A, 1 drop TID as needed)
- Artificial tears 5–6×/day
- Duration: 1–3 weeks; highly contagious — hand hygiene, separate towels
- If viral vs. bacterial distinction is unclear, prescribe empiric topical antibiotics pending ophthalmology review
- Disinfect exam equipment after contact
3. Allergic Conjunctivitis
Presentation: Bilateral, itching, watery discharge, erythematous swollen eyelids, papillae on inferior conjunctival fornix (irregular mounds with central vascular tuft — contrasts with viral follicles).
Management (stepwise):
- Identify and eliminate allergen
- Cool compresses QID
- Mild: Artificial tears alone
- Moderate: Topical antihistamine/decongestant, mast cell stabilizers (e.g., ketotifen, olopatadine), or NSAIDs
- Severe: Topical steroids — use only after ophthalmology consultation (occult herpetic infection must be excluded first)
Neonatal Conjunctivitis (Ophthalmia Neonatorum)
Defined as conjunctivitis in neonates ≤30 days old. Always obtain a Gram stain of discharge — it guides management.
| Type | Cause | Age of Onset | Key Findings | Treatment |
|---|---|---|---|---|
| Chemical | Erythromycin prophylaxis | First 24 h | Bilateral, watery, negative Gram stain | Watchful waiting; resolves ≤48 h |
| Gonococcal | N. gonorrhoeae | Days 2–7 | Intense chemosis, copious purulent discharge, gram-negative diplococci | Admit; single-dose IV ceftriaxone 50 mg/kg (max 125 mg); eye irrigation; evaluate for disseminated disease |
| Chlamydial | C. trachomatis | Days 7–14 | Intense erythema, purulent discharge | Admit; oral + topical antibiotics (oral erythromycin/azithromycin) |
| Other bacterial | S. aureus, NTHi, E. coli, Pseudomonas | Days 7–14 | Identified on Gram stain | Topical antibiotics per organism |
| Viral (HSV-2) | HSV-2 (rarely HSV-1) | Days 14–28 | Dendrites on fluorescein exam | Admit; IV + topical antivirals |
Key actions for gonococcal disease:
- Admit, ophthalmology consult
- Test blood, urine, CSF for disseminated disease
- If hyperbilirubinemia or disseminated infection suspected, use cefotaxime (50 mg/kg IV q8h) instead of ceftriaxone
When to Refer / Red Flags
- Any neonatal conjunctivitis (except suspected chemical)
- Suspected gonococcal or HSV infection at any age
- Reduced or altered visual acuity
- Corneal involvement (fluorescein-positive, herpetic dendrite)
- Failure to improve with standard therapy
- Contact lens wearers with purulent discharge
Prophylaxis at Birth
- AAP: Recommends routine erythromycin ointment for all newborns (to prevent gonococcal ophthalmia)
- Canadian Paediatric Society: Advises against routine prophylaxis
- Practice varies by institution and jurisdiction
Sources: Tintinalli's Emergency Medicine — A Comprehensive Study Guide; The Harriet Lane Handbook, 23rd ed. (The Johns Hopkins Hospital)
This is a shared conversation. Sign in to Orris to start your own chat.