Explain different body fluid compartment and it’s regulation
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Finding Sources
Reading File
Finding Sources
Finding Sources
Reading File
Finding Sources
Reading File
Finding Sources
Finding Sources
Loading Image
Finding Sources
Finding Sources
Loading Image
Now I have comprehensive content from Guyton & Hall and Costanzo to compose a thorough answer.
Body Fluid Compartments and Their Regulation
1. Overview: Total Body Water
Total body water (TBW) accounts for 60% of body weight in an average 70-kg adult male (~42 L). This percentage varies with:
| Factor | Effect |
|---|---|
| High muscle mass | ↑ TBW (muscle is ~75% water) |
| High body fat | ↓ TBW (fat is ~10% water) |
| Female sex | ~50% (more adipose tissue) |
| Neonates/premature | 70–75% of body weight |
| Advancing age | Gradually decreases |
2. The Major Compartments
TBW is divided into two main compartments, separated by the cell membrane:
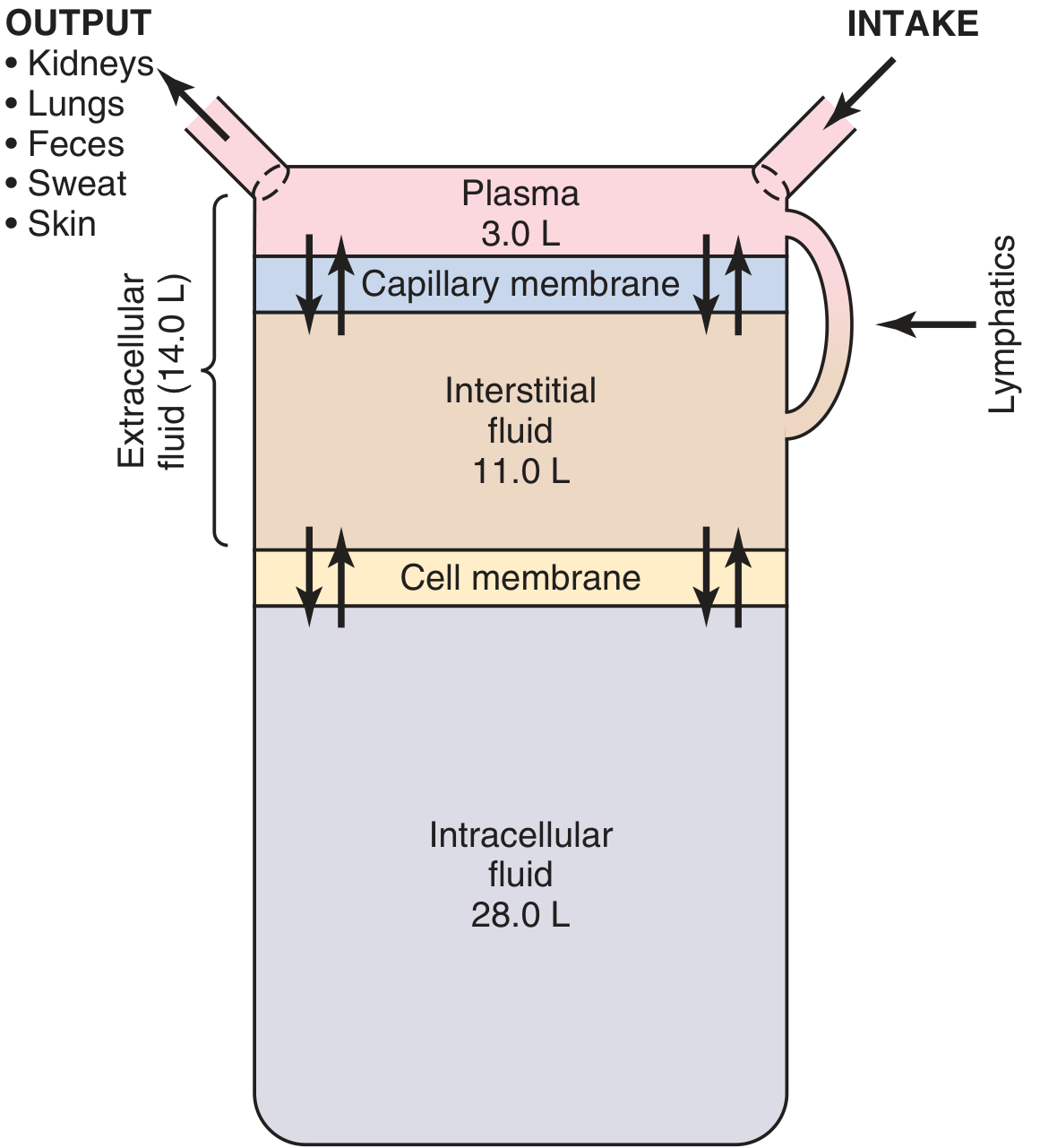
Figure: Summary of body fluid compartments in a 70-kg man (Guyton & Hall)
A. Intracellular Fluid (ICF)
- Volume: ~28 L (⅔ of TBW; 40% of body weight)
- Contains the fluid of all body cells collectively
- Remarkably similar composition across different cell types and species
- Major cation: K⁺ (~150 mEq/L)
- Major anions: PO₄³⁻ and organic anions, protein
B. Extracellular Fluid (ECF)
- Volume: ~14 L (⅓ of TBW; 20% of body weight)
- Divided into two main subcompartments separated by the capillary wall:
i. Plasma
- Volume: ~3 L (~¼ of ECF)
- Circulates within blood vessels
- Contains large plasma proteins (albumin, globulins) that do not cross capillary walls
- Major cation: Na⁺ (~142 mEq/L)
- Major anions: Cl⁻, HCO₃⁻
ii. Interstitial Fluid
- Volume: ~11 L (~¾ of ECF)
- Directly bathes the cells; an ultrafiltrate of plasma
- Virtually protein-free (capillary wall is impermeable to proteins)
- Ionic composition otherwise almost identical to plasma
iii. Transcellular Fluid (a specialized ECF)
- Volume: ~1–2 L
- Includes: CSF, synovial fluid, peritoneal fluid, pericardial fluid, intraocular fluid, pleural fluid
- May differ markedly in composition from plasma/interstitial fluid in some locations
C. Blood Volume
- ~5 L (~7% of body weight)
- Composed of plasma (~60%) + red blood cells (~40%)
- Normal hematocrit: ~0.42 in men, ~0.38 in women
- Considered a distinct functional compartment due to its circulatory role
3. Composition of Compartments
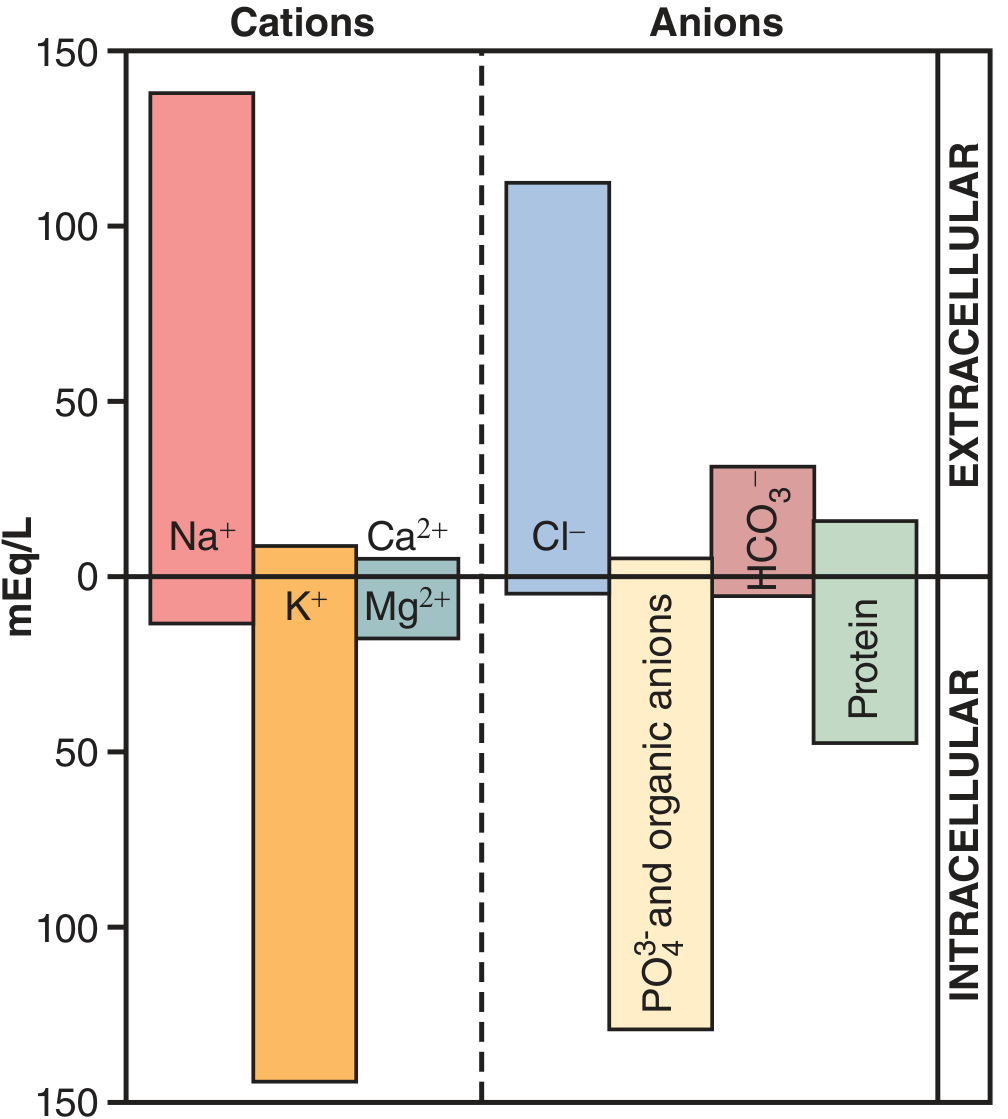
Figure: Major cations and anions in ICF vs ECF (Guyton & Hall)
| Ion | ECF (mEq/L) | ICF (mEq/L) |
|---|---|---|
| Na⁺ | 142 | 10–14 |
| K⁺ | 4–5 | 140–150 |
| Ca²⁺ | 5 (total) | <1 (ionized) |
| Mg²⁺ | 3 | 26 |
| Cl⁻ | 108 | 3–4 |
| HCO₃⁻ | 28 | 10 |
| PO₄³⁻ | 4 | ~75 |
| Protein | 16 | ~54 |
The electroneutrality principle holds in all compartments: the total cation charge equals the total anion charge.
4. Regulation of Fluid Compartments
A. Osmolarity — The Governing Principle
Normal ECF osmolarity is 290–300 mOsm/L. Because water moves freely across cell membranes, ICF osmolarity always equals ECF osmolarity in steady state.
Plasma osmolarity can be estimated by:
Posm = 2 × [Na⁺] + Glucose/18 + BUN/2.8
(Na⁺ in mEq/L, glucose and BUN in mg/dL)
Na⁺ (with its accompanying Cl⁻ and HCO₃⁻) determines ECF volume; osmolarity determines water distribution between ICF and ECF.
B. Regulation of ECF Volume (Na⁺ Balance)
ECF volume is primarily regulated by Na⁺ balance via the kidneys:
1. Renin–Angiotensin–Aldosterone System (RAAS)
- ↓ BP / ↓ ECF volume → renin released from juxtaglomerular cells
- Renin cleaves angiotensinogen → Angiotensin I → (ACE) → Angiotensin II
- Angiotensin II effects:
- Stimulates aldosterone secretion from adrenal cortex
- Aldosterone → ↑ Na⁺ (and water) reabsorption in collecting duct
- Direct vasoconstriction → ↑ BP
- Stimulates thirst and ADH release
2. Atrial Natriuretic Peptide (ANP)
- Released from atria when ECF volume/BP rises
- Causes natriuresis (Na⁺ excretion) and vasodilation → ↓ ECF volume
3. Sympathetic Nervous System
- ↓ volume → baroreceptor activation of sympathetics → ↑ renal Na⁺ retention
C. Regulation of Osmolarity (Water Balance)
1. ADH (Antidiuretic Hormone / Vasopressin)
- Synthesized in hypothalamus; released from posterior pituitary
- Stimuli: ↑ plasma osmolarity (detected by hypothalamic osmoreceptors), ↓ blood volume/pressure
- Action: Inserts aquaporin-2 channels in collecting duct → ↑ water reabsorption → dilute urine
- Net effect: ↓ plasma osmolarity, ↑ ECF volume
2. Thirst Mechanism
- Osmoreceptors in hypothalamus detect ↑ osmolarity → stimulate thirst
- Drinking water → ↓ osmolarity → restores fluid balance
- This is the primary long-term defense against hyperosmolarity
D. Water Shifts Between Compartments
The volume of each compartment depends on its solute content:
| Disturbance | ECF Osmolarity | Water Shift | Example |
|---|---|---|---|
| Pure water loss | ↑ (hyperosmotic) | ECF → ICF (cell shrinks) | Diabetes insipidus |
| Water gain (SIADH) | ↓ (hyposmotic) | ICF → ECF → cells swell | SIADH |
| Isotonic NaCl infusion | Normal | No shift | IV saline administration |
| NaCl gain (excess) | ↑ | Water drawn from ICF | Hypernatremia |
| Diarrhea/dehydration | ↑ | ICF water lost to ECF | Severe gastroenteritis |
Key principles:
- ECF volume is set by total NaCl content
- ICF volume is set by osmolarity (water follows osmoles)
- In steady state, ICF osmolarity = ECF osmolarity
- NaCl and mannitol stay in ECF; urea equilibrates across membranes (ineffective osmole)
E. Starling Forces (Plasma ↔ Interstitial Fluid Exchange)
Movement between plasma and interstitial fluid across the capillary wall is governed by Starling forces:
Net filtration = Kf [(Pc − Pi) − σ(πc − πi)]
| Force | Effect |
|---|---|
| Capillary hydrostatic pressure (Pc) | Pushes fluid OUT of capillary |
| Interstitial hydrostatic pressure (Pi) | Pushes fluid INTO capillary |
| Plasma oncotic pressure (πc) | Draws fluid INTO capillary |
| Interstitial oncotic pressure (πi) | Draws fluid OUT of capillary |
- Normally, a small net filtration at the arterial end is returned via lymphatics
- Loss of plasma proteins → ↓ πc → edema (e.g., nephrotic syndrome, liver failure)
5. Measuring Fluid Compartment Volumes
| Compartment | Indicator Used |
|---|---|
| TBW | ³H₂O, ²H₂O (deuterium), antipyrine |
| ECF | ²²Na, inulin, thiosulfate, ¹²⁵I-iothalamate |
| ICF | Calculated: TBW − ECF |
| Plasma | ¹²⁵I-albumin, Evans blue dye |
| Interstitial | Calculated: ECF − Plasma volume |
The dilution principle underlies all measurements: Volume = (Amount injected) / (Final concentration).
Summary
| Compartment | Volume (70-kg man) | % TBW | Key Solutes | Barrier |
|---|---|---|---|---|
| ICF | 28 L | 67% | K⁺, PO₄³⁻, protein | Cell membrane |
| ECF — Interstitial | 11 L | 26% | Na⁺, Cl⁻, HCO₃⁻ | Capillary wall |
| ECF — Plasma | 3 L | 7% | Na⁺, Cl⁻, protein | Capillary wall |
| Transcellular | 1–2 L | ~2% | Variable | Epithelial cells |
Fluid homeostasis is maintained by the kidneys (primary effector), RAAS, ADH/thirst axis, ANP, and the sympathetic nervous system working in an integrated feedback loop to keep both volume and osmolarity within narrow physiological limits.
Sources: Guyton and Hall Textbook of Medical Physiology; Costanzo Physiology 7th Edition
Fast
Asking for Preferences
You've run out of free credits. Sign up for a free account to continue using Orris.
This is a shared conversation. Sign in to Orris to start your own chat.