Please make diagnosis
Reading File
Finding Sources
Finding Sources
Finding Sources
Searching Images
CT brain intracerebral hemorrhage basal ganglia hyperdense
Reading File
Loading Image
Based on careful review of the CT head series, here is my radiological analysis:
CT Head — Radiological Report & Diagnosis
Patient: Darshan Singh, SAY M | Age: ~52 years | Non-contrast CT Brain
Key Findings
Row 2 (basal ganglia level) — most critical finding:
There is a focal hyperdense (bright white) lesion in the right basal ganglia / putaminal region, seen clearly in the right-sided image of row 2. This acute hyperdensity is characteristic of fresh blood clot on non-contrast CT (blood has a Hounsfield unit value of ~50–80 HU, making it brighter than normal brain parenchyma).
Ventricular system: The lateral ventricles appear mildly prominent. There is early effacement of the right lateral ventricle, consistent with mild mass effect from the hemorrhage.
Midline: Mild midline shift toward the left is suggested.
Cortical sulci: Preserved at the vertex, arguing against significant diffuse cerebral edema.
Posterior fossa / cerebellum: No obvious cerebellar hemorrhage or herniation.
Bone windows (rows 6–7): No obvious skull fracture or bony defect.
Primary Diagnosis
Right Basal Ganglia (Putaminal) Intracerebral Hemorrhage (ICH)
This is the classic location and CT appearance of hypertensive hemorrhagic stroke — the putamen / basal ganglia is the most common site (~35% of all spontaneous ICH), supplied by the lenticulostriate arteries, which are highly susceptible to hypertensive changes.
Reference Image for Comparison
Below is a textbook CT showing the identical pattern — acute hyperdense lesion in the right putamen with surrounding hypodense edema:
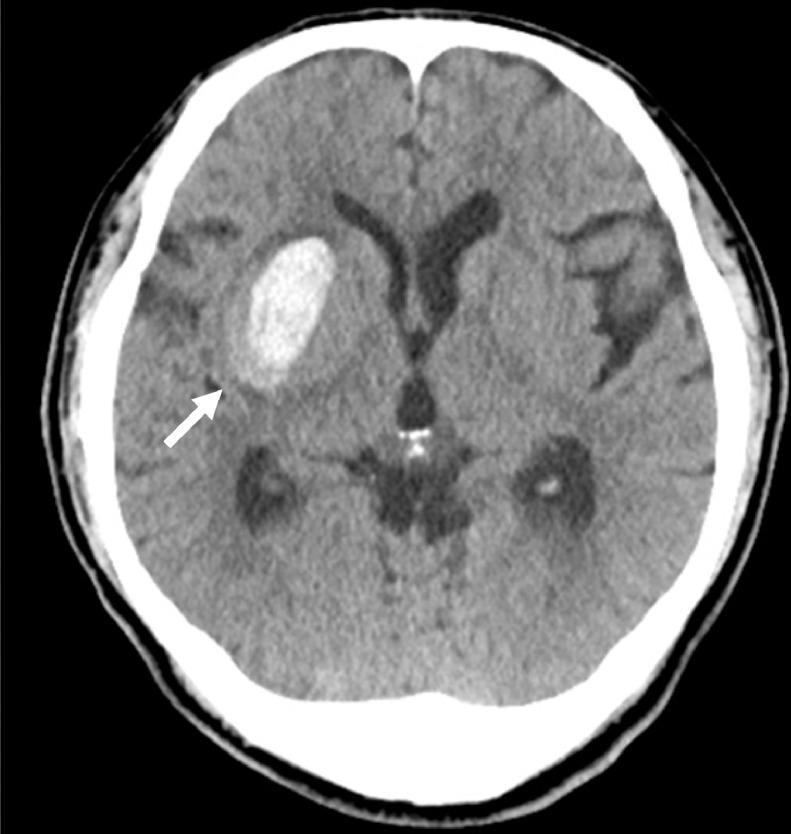
Differential Diagnosis
| Diagnosis | Likelihood | Comment |
|---|---|---|
| Hypertensive putaminal ICH | Most likely | Classic location + age + hyperdense lesion |
| Hemorrhagic transformation of ischemic stroke | Less likely | Would expect wedge-shaped hypodensity first |
| AVM rupture | Possible | Younger patients; MRI/angiography needed |
| Cavernous malformation bleed | Possible | Usually smaller; "popcorn" appearance on MRI |
| Hemorrhagic tumor | Less likely | Would expect ring enhancement + surrounding edema |
Clinical Correlation
Typical presentation:
- Sudden-onset contralateral hemiplegia (left-sided weakness given right putaminal bleed)
- Hemisensory loss
- Possible dysarthria
- Headache, nausea/vomiting
Urgent management steps:
- Neurosurgical consultation
- Blood pressure control (target SBP <140 mmHg per AHA guidelines)
- Reverse any anticoagulation if applicable
- Serial neurological assessment and repeat CT if deterioration
- Consider surgical evacuation if hematoma volume >30 mL with deterioration
⚠️ Important: This analysis is for educational/support purposes. Formal radiological diagnosis must be made by a licensed radiologist in conjunction with the treating clinician and full clinical history.
This is a shared conversation. Sign in to Orris to start your own chat.