Give in detail about 9 quadrat ana patho pom surgery medicine
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Finding Sources
Searching Images
nine abdominal regions quadrants diagram anatomy
Loading Image
Loading Image
Finding Sources
Finding Sources
I now have everything I need for a comprehensive, well-illustrated answer. Let me compile the full detailed response covering all 9 abdominal regions across anatomy, pathology, pharmacology (POM), surgery, and medicine.
The 9 Abdominal Regions (Quadrants) — Anatomy, Pathology, Pharmacology, Surgery & Medicine
Anatomical Basis of the Nine-Region Division
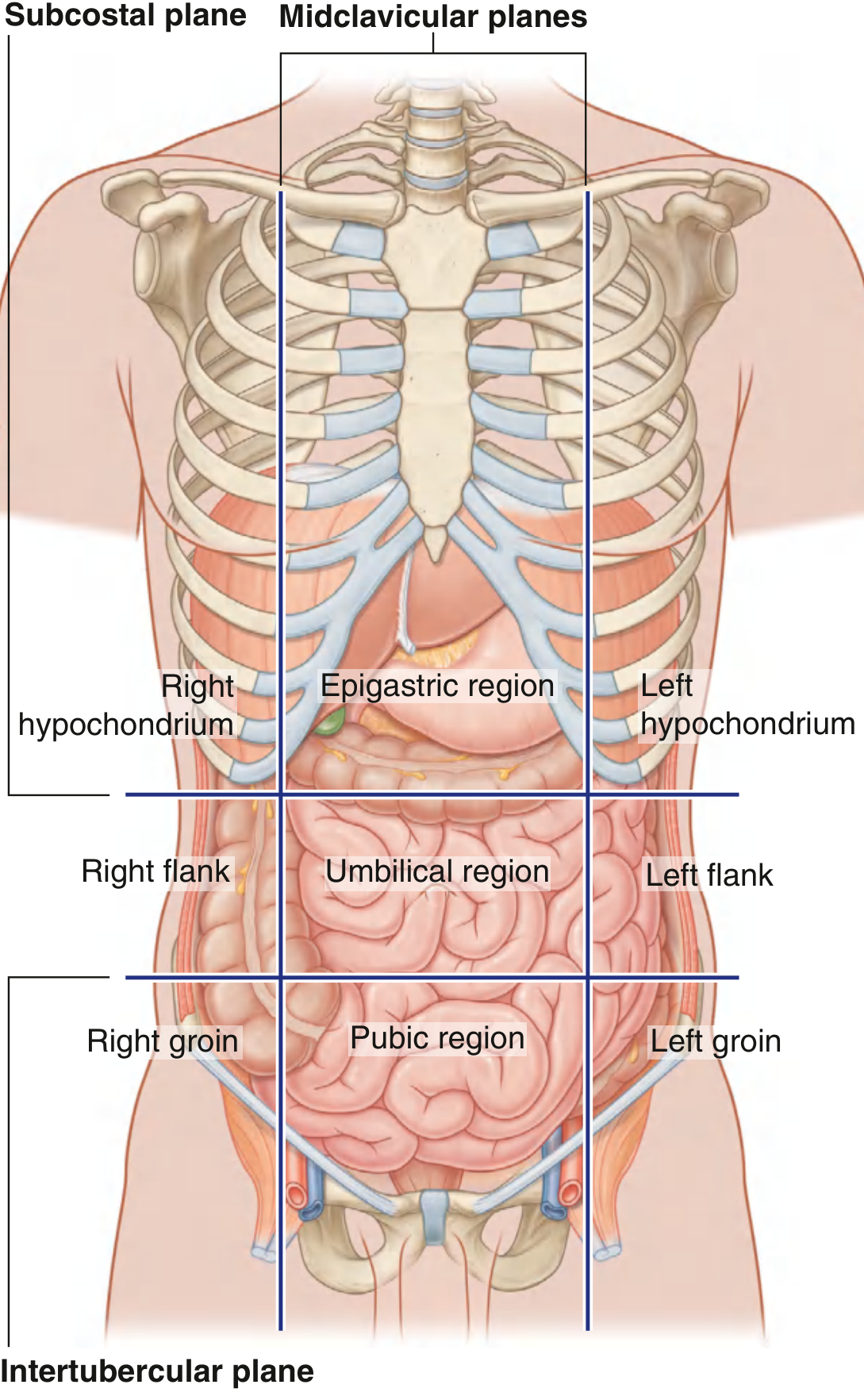
The abdomen is divided into 9 regions by 4 planes:
- Two horizontal planes: Subcostal plane (below costal margins, at lower border of costal cartilage of rib X / vertebra LIII) and Intertubercular plane (connecting iliac crest tubercles / vertebra LV)
- Two vertical (midclavicular) planes: Running from midpoint of clavicles to midpoint between ASIS and pubic symphysis
(Gray's Anatomy for Students)
Region 1: Right Hypochondrium (Right Subcostal)
Anatomy
- Liver (right lobe — primary location), gallbladder, hepatic flexure of colon, right kidney (upper pole), right adrenal gland, part of duodenum
Pathology
- Hepatitis (viral, alcoholic, autoimmune) — tender hepatomegaly
- Cholecystitis (acute/chronic) — Murphy's sign positive
- Cholelithiasis — biliary colic
- Liver abscess, hepatocellular carcinoma
- Subphrenic abscess
Pharmacology (POM)
- Ursodeoxycholic acid — dissolution of cholesterol gallstones; also used in primary biliary cholangitis
- Antivirals (tenofovir, entecavir for HBV; sofosbuvir/ledipasvir for HCV)
- Analgesics: Antispasmodics (hyoscine butylbromide) for biliary colic
- Avoid hepatotoxic drugs (paracetamol overdose, statins, isoniazid) — monitor LFTs
Surgery
- Laparoscopic cholecystectomy — gold standard for symptomatic gallstones (4-port technique; camera at umbilicus, working ports at epigastrium and right upper quadrant)
- Open cholecystectomy (Kocher's incision — right subcostal) for complicated cases
- ERCP + sphincterotomy for choledocholithiasis
- Liver resection (hepatectomy) for HCC/metastases
Medicine
- Murphy's sign (right subcostal tenderness on inspiration) — pathognomonic of cholecystitis
- RUQ pain + jaundice + fever = Charcot's triad (cholangitis)
- Courvoisier's law: palpable gallbladder + jaundice = likely malignancy (not gallstones)
- US abdomen is first-line imaging; MRCP for bile duct evaluation
Region 2: Epigastric Region
Anatomy
- Stomach, duodenum (D1, D2), liver (left lobe), pancreas (head and body), lesser omentum, abdominal aorta, inferior vena cava, coeliac axis
Pathology
- Peptic ulcer disease (gastric/duodenal) — burning epigastric pain, worse/better with food
- Acute pancreatitis — severe epigastric pain radiating to back
- Gastritis, GORD
- Aortic aneurysm (AAA) — pulsatile epigastric mass
- Gastric cancer
Pharmacology (POM)
- PPIs (omeprazole, lansoprazole) — first-line for GORD, peptic ulcer, H. pylori eradication
- H2-blockers (ranitidine, famotidine) — second-line
- H. pylori triple therapy: PPI + clarithromycin + amoxicillin (7–14 days)
- Antacids (magnesium hydroxide, aluminium hydroxide) — symptomatic relief
- Octreotide — reduces pancreatic secretions in acute pancreatitis
- IV morphine or pethidine for severe pancreatitis pain
- Prokinetics (metoclopramide, domperidone) for gastroparesis/GORD
Surgery
- Truncal vagotomy + pyloroplasty (historical) for peptic ulcer
- Billroth I/II gastrectomy or Roux-en-Y reconstruction for gastric cancer
- Whipple's procedure (pancreaticoduodenectomy) for pancreatic head/periampullary cancer
- Endoscopic hemostasis for bleeding peptic ulcer (adrenaline injection, clips)
- AAA repair — open (midline laparotomy) or EVAR (endovascular)
Medicine
- Ranson's criteria / APACHE II / Glasgow score for pancreatitis severity
- Cullen's sign (periumbilical bruising) + Grey Turner's sign (flank bruising) = severe pancreatitis with retroperitoneal hemorrhage
- H. pylori testing: urea breath test, stool antigen, biopsy (CLO test)
- Epigastric pain + ECG changes → rule out inferior MI (referred pain via phrenic nerve)
Region 3: Left Hypochondrium (Left Subcostal)
Anatomy
- Spleen, tail of pancreas, stomach (fundus), left kidney (upper pole), left adrenal gland, splenic flexure of colon
Pathology
- Splenomegaly (malaria, CML, portal hypertension, EBV, lymphoma)
- Splenic injury/rupture — trauma; Kehr's sign (left shoulder tip pain)
- Splenic infarct — sickle cell disease, emboli
- Gastric volvulus
- Subphrenic abscess (left)
Pharmacology (POM)
- Hydroxycarbamide (hydroxyurea) — reduces sickling crises; prevents splenic infarction in sickle cell disease
- Anti-malarials (artemisinin-based, chloroquine, quinine)
- Penicillin V prophylaxis — lifelong post-splenectomy to prevent overwhelming post-splenectomy infection (OPSI)
- Vaccines post-splenectomy: pneumococcal (PCV13/PPSV23), meningococcal (ACWY + B), Hib, annual influenza
Surgery
- Splenectomy (laparoscopic preferred) — for trauma, ITP refractory to treatment, hereditary spherocytosis, hypersplenism
- Splenic artery embolization (non-operative management of splenic laceration grade I–III)
- Distal pancreatectomy ± splenectomy for pancreatic tail tumours
Medicine
- Massive splenomegaly causes: CML, myelofibrosis, visceral leishmaniasis (kala-azar), tropical splenomegaly
- Traube's space dullness on percussion indicates splenomegaly
- OPSI — potentially fatal; highest risk in first 2 years post-splenectomy; caused by encapsulated organisms (S. pneumoniae, N. meningitidis, H. influenzae)
Region 4: Right Flank (Right Lumbar / Right Lateral)
Anatomy
- Ascending colon, right kidney (main body), right ureter, small intestinal loops, right psoas muscle, right quadratus lumborum
Pathology
- Renal colic (ureteric stones) — severe colicky loin-to-groin pain, hematuria
- Pyelonephritis — loin pain, fever, dysuria; positive renal angle tenderness (CVAT)
- Renal cell carcinoma — classic triad: hematuria, loin pain, palpable mass
- Crohn's disease (right-sided involvement)
- Retroperitoneal fibrosis
Pharmacology (POM)
- Alpha-blockers (tamsulosin) — facilitate ureteric stone passage (medical expulsive therapy)
- NSAIDs (diclofenac IV/IM) — first-line analgesia for renal colic (reduces ureteral spasm + prostaglandin-mediated inflammation)
- Opioids (morphine, pethidine) — adjunct for severe renal colic
- Antibiotics for pyelonephritis: ciprofloxacin or co-amoxiclav (7–14 days); IV gentamicin + amoxicillin if severe
- Sunitinib, pazopanib, nivolumab — targeted/immunotherapy for metastatic RCC
Surgery
- Ureteroscopy + laser lithotripsy for ureteric calculi
- ESWL (extracorporeal shock wave lithotripsy) for renal/proximal ureteric stones
- Percutaneous nephrolithotomy (PCNL) for large staghorn calculi
- Radical nephrectomy for RCC
- Right hemicolectomy for Crohn's stricture / ascending colon cancer
Medicine
- Renal angle tenderness (costovertebral angle) — pyelonephritis vs. musculoskeletal vs. renal colic
- Urinalysis + urine culture mandatory; CT KUB (non-contrast) is gold standard for renal/ureteric calculi
- ACE inhibitors/ARBs for renoprotection in diabetic nephropathy
Region 5: Umbilical Region (Periumbilical)
Anatomy
- Small intestine (jejunum, ileum), transverse colon, abdominal aorta, inferior mesenteric artery origin, lymph nodes, umbilicus, mesentery
Pathology
- Small bowel obstruction — colicky periumbilical pain, distension, vomiting, absolute constipation
- Aortic aneurysm (AAA) — pulsatile mass at/above umbilicus; pain may radiate to back
- Mesenteric ischemia — "pain out of proportion to signs"; postprandial angina
- Umbilical hernia
- Early appendicitis — visceral pain starts periumbilical before migrating to RIF (McBurney's point)
Pharmacology (POM)
- IV fluids (crystalloids) + nasogastric decompression for bowel obstruction
- Anticoagulants (heparin, warfarin) — prevent/treat mesenteric venous thrombosis
- Thrombolytics / papaverine — intra-arterial for acute mesenteric ischemia (non-occlusive)
- Antifibrinolytics are avoided
- Beta-blockers — reduce AAA expansion rate (evidence for propranolol; currently used perioperatively)
- Statins — slow aneurysm growth and reduce cardiovascular events
Surgery
- Emergency laparotomy — for ruptured AAA (massive mortality); EVAR if available
- Elective AAA repair — when >5.5 cm (men), >5 cm (women), or rapid expansion
- Adhesiolysis — for adhesion-related SBO (laparoscopic or open)
- Bowel resection — for mesenteric ischemia with necrosis (second-look laparotomy at 24–48 h)
- Umbilical hernia repair — mesh or primary suture
Medicine
- Cullen's sign (periumbilical bruising) = hemorrhagic pancreatitis or ruptured ectopic pregnancy
- Sister Mary Joseph nodule = periumbilical lymph node metastasis from intra-abdominal malignancy
- Aortic bruit on auscultation → investigate with US abdomen for AAA
- Small bowel obstruction: "ladder pattern" (dilated loops with valvulae conniventes) on plain AXR
Region 6: Left Flank (Left Lumbar / Left Lateral)
Anatomy
- Descending colon, left kidney, left ureter, small bowel loops, left psoas muscle, left quadratus lumborum
Pathology
- Renal colic (left ureteric stones)
- Pyelonephritis (left)
- Polycystic kidney disease (bilateral flank masses)
- Descending colon cancer — iron deficiency anemia, change in bowel habit
- Retroperitoneal hematoma
Pharmacology (POM)
- Same as right flank (NSAIDs, alpha-blockers for stones; antibiotics for UTI/pyelonephritis)
- FOLFOX / FOLFIRI (fluorouracil + oxaliplatin or irinotecan) — chemotherapy for colon cancer
- Bevacizumab (anti-VEGF) — add-on for metastatic colorectal cancer
- Tolvaptan — vasopressin receptor antagonist for ADPKD (slows cyst growth)
Surgery
- Same urological procedures as right flank
- Left hemicolectomy for descending colon cancer
- Bilateral laparoscopic nephrectomy in ADPKD (prior to transplantation if massive enlargement)
Medicine
- PKD: bilateral flank masses + hypertension + hematuria; associated with berry aneurysms (screen MRA)
- Descending colon cancer often presents with obstruction (narrower lumen than right colon); less likely to cause anemia than right-sided cancers
Region 7: Right Iliac Fossa (Right Groin / Right Inguinal Region)
Anatomy
- Appendix (most common position: retrocaecal, 65%), caecum, terminal ileum, right ovary + right fallopian tube (females), right ureter (lower), psoas muscle, inguinal ligament, femoral/inguinal canal structures
Pathology
- Acute appendicitis — most common surgical emergency worldwide
- Ectopic pregnancy (right) — acute pain; positive bhCG; US shows no intrauterine pregnancy
- Ovarian cyst / Mittelschmerz / Ovarian torsion
- Mesenteric adenitis (children — mimics appendicitis)
- Inguinal hernia (indirect most common, especially in males)
- Crohn's disease (terminal ileitis)
- Caecal carcinoma
- Psoas abscess
Pharmacology (POM)
- IV antibiotics pre-/post-appendicectomy: cefuroxime + metronidazole (covers aerobes + anaerobes)
- Piperacillin-tazobactam or meropenem for complicated (perforated) appendicitis
- Analgesia: IV opioids (morphine) — does NOT mask peritonism in studies; safe to give
- Methotrexate — medical management of ectopic pregnancy (if unruptured, β-hCG <3000, no cardiac activity)
- Mesalazine / azathioprine / biologics (infliximab, adalimumab) — Crohn's disease management
Surgery
- Laparoscopic appendicectomy — standard of care; McBurney's point incision used in open (grid-iron incision)
- Antibiotic-only management of uncomplicated appendicitis (Appendicitis Acuta trial) — controversial but gaining acceptance
- Appendicectomy + right hemicolectomy for caecal carcinoma found incidentally
- Inguinal hernia repair: open (Lichtenstein mesh) or laparoscopic (TEP/TAPP)
- Salpingectomy / salpingostomy for ectopic pregnancy
Medicine
- McBurney's point: 1/3 of the way from ASIS to umbilicus
- Rovsing's sign (palpation LIF causes RIF pain), Psoas sign, Obturator sign
- Alvarado score (MANTRELS) for appendicitis diagnosis
- In women of childbearing age: always check β-hCG before attributing RIF pain to appendicitis
Region 8: Pubic/Hypogastric Region (Suprapubic)
Anatomy
- Urinary bladder, uterus (body and cervix), fallopian tubes (bilateral), rectum/sigmoid colon junction, prostate (males), ureters (terminal portions), seminal vesicles
Pathology
- Pelvic inflammatory disease (PID) — bilateral lower abdominal pain, vaginal discharge, cervical excitation
- Ovarian cysts (bilateral)
- Cystitis / UTI — suprapubic pain, dysuria, frequency
- Bladder cancer — painless hematuria
- Fibroids (uterine leiomyomas) — menorrhagia, pressure symptoms
- Pelvic peritonitis / Pouch of Douglas abscess (pelvic abscess)
- BPH / prostate cancer (males)
Pharmacology (POM)
- Antibiotics for PID: doxycycline + metronidazole ± ceftriaxone (covers C. trachomatis, N. gonorrhoeae, anaerobes)
- Antibiotics for UTI: trimethoprim, nitrofurantoin (uncomplicated); ciprofloxacin (complicated)
- Antispasmodics / anticholinergics (oxybutynin, solifenacin) for overactive bladder
- 5-alpha reductase inhibitors (finasteride) + alpha-blockers (tamsulosin) for BPH
- GnRH agonists (leuprolide) for fibroids (induces medical menopause preoperatively)
- NSAIDs / mefenamic acid for dysmenorrhea and fibroid-related pain
- Combined oral contraceptive — suppresses endometriosis, reduces PID recurrence
Surgery
- Laparoscopic drainage of pelvic abscess (Pouch of Douglas)
- TURP / laser prostatectomy for BPH
- Radical cystectomy + neobladder for muscle-invasive bladder cancer
- Total abdominal hysterectomy ± bilateral salpingo-oophorectomy (TAH-BSO) for fibroids/cancer
- Anterior/posterior repair (colporrhaphy) for pelvic organ prolapse
- Pelvic lymph node dissection — staging for cervical/endometrial/bladder malignancy
Medicine
- Fitz-Hugh-Curtis syndrome: right upper quadrant pain (perihepatic adhesions) secondary to ascending PID — mimics cholecystitis
- Cervical motion tenderness (chandelier sign) = PID
- PSA + TRUS-guided biopsy for prostate cancer; Gleason score for grading
- Bimanual examination essential for pelvic pathology; transvaginal US for ovarian/uterine lesions
Region 9: Left Iliac Fossa (Left Groin / Left Inguinal Region)
Anatomy
- Sigmoid colon, descending colon (lower), left ovary + left fallopian tube (females), left ureter (lower), inguinal structures (left), psoas muscle (left lower)
Pathology
- Diverticulitis — "left-sided appendicitis"; older patients; LIF pain, fever, altered bowel habit
- Diverticular abscess / perforation — peritonitis, pneumoperitoneum
- Sigmoid colon cancer — change in bowel habit, bleeding PR, obstruction
- Ectopic pregnancy (left)
- Ovarian pathology (left) — same as right
- Inguinal hernia (left)
- Constipation (very common cause of LIF pain, especially elderly)
Pharmacology (POM)
- Antibiotics for uncomplicated diverticulitis: metronidazole + ciprofloxacin (outpatient); IV co-amoxiclav or piperacillin-tazobactam (inpatient)
- Recent evidence (DIABOLO trial, AVOD trial): antibiotics may not be needed for uncomplicated acute diverticulitis — conservative management (bowel rest, analgesia) gaining acceptance
- Mesalazine — reduces recurrence of diverticulitis (limited evidence)
- High-fibre diet — prevents diverticular disease progression
- FOLFOX/FOLFIRI + bevacizumab — for metastatic sigmoid colon cancer
- Osmotic laxatives (lactulose, macrogol) and stimulant laxatives (senna, bisacodyl) for constipation
Surgery
- Hartmann's procedure — emergency sigmoid resection + end colostomy (for perforated diverticulitis with Hinchey III/IV peritonitis)
- Laparoscopic sigmoid colectomy — elective, after resolution of recurrent/complicated diverticulitis (usually ≥2 attacks or single complicated episode)
- Emergency Hartmann's reversal — reconnection of Hartmann's stoma (colostomy takedown)
- Anterior resection — for sigmoid colon / upper rectal cancer (with or without defunctioning ileostomy)
- Abdominoperineal resection (APR) — for low rectal cancer where sphincter cannot be preserved
Medicine
- Hinchey classification for perforated diverticulitis (I: pericolic abscess → IV: fecal peritonitis)
- CT abdomen/pelvis with IV contrast is the investigation of choice
- Colonoscopy contraindicated in acute diverticulitis (risk of perforation) — perform 6–8 weeks after resolution
- Diverticular disease vs. diverticulitis: former is asymptomatic; latter implies infection/inflammation
Summary Table
| Region | Key Organs | Key Pathology | Key Surgery | Key Drugs |
|---|---|---|---|---|
| R. Hypochondrium | Liver, Gallbladder | Cholecystitis, Hepatitis | Laparoscopic cholecystectomy | Ursodeoxycholic acid, PPIs, antivirals |
| Epigastric | Stomach, Duodenum, Pancreas | PUD, Pancreatitis, AAA | Whipple's, gastrectomy, EVAR | PPIs, H. pylori triple therapy, octreotide |
| L. Hypochondrium | Spleen, Stomach fundus | Splenomegaly, Splenic rupture | Splenectomy | Penicillin V (post-splenectomy), hydroxyurea |
| R. Flank | R. Kidney, Ascending colon | Renal colic, Pyelonephritis, RCC | Nephrectomy, ureteroscopy, PCNL | NSAIDs, tamsulosin, ciprofloxacin |
| Umbilical | Small bowel, Aorta | SBO, AAA, Mesenteric ischemia | Laparotomy, EVAR, adhesiolysis | IV fluids, heparin, statins |
| L. Flank | L. Kidney, Descending colon | Renal colic, Colon cancer, PKD | Hemicolectomy, nephrectomy | FOLFOX, tolvaptan, NSAIDs |
| R. Iliac Fossa | Appendix, Caecum, R. Ovary | Appendicitis, Ectopic pregnancy, Crohn's | Appendicectomy, hernia repair | Cefuroxime + metronidazole, methotrexate |
| Pubic/Hypogastric | Bladder, Uterus, Rectum | PID, Cystitis, BPH, Bladder Ca | Cystectomy, TURP, hysterectomy | Doxycycline + metronidazole, tamsulosin |
| L. Iliac Fossa | Sigmoid colon, L. Ovary | Diverticulitis, Sigmoid Ca, Ectopic | Hartmann's, anterior resection | Metronidazole + ciprofloxacin, FOLFOX |
Sources:
- Gray's Anatomy for Students, Nine-region pattern (block2, p. 336)
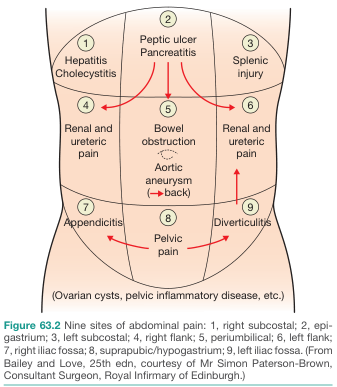
- Bailey and Love's Short Practice of Surgery, 28th Edition, Figure 63.2
- Tintinalli's Emergency Medicine, Rosen's Emergency Medicine, Sleisenger & Fordtran's Gastrointestinal and Liver Disease, Yamada's Textbook of Gastroenterology — clinical correlations throughout
Give pdf
Reading File
Running Command
Running Command
Writing File
Running Command
Your PDF is ready! Download it here:
9 Abdominal Regions
PDF Document · PDF
What's included in the PDF:
- Cover page with both anatomical diagrams (Gray's Anatomy nine-region diagram + Bailey & Love clinical pain sites illustration)
- 9 region sections, each covering:
- Anatomy (key organs)
- Pathology (key diseases)
- Pharmacology/POM (key drugs with mechanisms)
- Surgery (key procedures)
- Medicine (clinical signs, investigations, pearls)
- Full summary table of all 9 regions at the end
- References from Gray's Anatomy, Bailey & Love, Tintinalli's, Rosen's, Sabiston's, and more
This is a shared conversation. Sign in to Orris to start your own chat.