Cranial nerve 1 to 12 examination in detail
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Finding Sources
Searching Images
cranial nerve examination clinical
Reading File
Reading File
Loading Image
Loading Image
Here is a detailed, structured examination guide for all 12 cranial nerves, compiled from Harrison's Principles of Internal Medicine 22E, Textbook of Family Medicine 9e, and Goldman-Cecil Medicine.
Cranial Nerve Examination: CN I–XII
Minimum screen: Check fundi, visual fields, pupil size and reactivity, extraocular movements, and facial movements. For a full exam, test all CNs in numerical order (grouping III, IV, VI together).
CN I — Olfactory Nerve
Function: Smell
When to test: Often omitted in routine exams. Indicated when there is suspected inferior frontal lobe disease (e.g., meningioma, head trauma, Parkinson's disease, Alzheimer's disease).
Technique:
- Ask the patient to close their eyes
- Occlude one nostril at a time
- Present a mild, non-irritating odorant — toothpaste, coffee, vanilla, or cloves
- Ask the patient to identify the smell (identification) and confirm they can detect it (detection)
Abnormal findings:
- Anosmia — absent smell; unilateral anosmia suggests a focal lesion (frontal meningioma, trauma); bilateral anosmia suggests neurodegenerative disease or post-viral etiology
- Note: Ammonia tests CN V (trigeminal), not CN I — do not use it
CN II — Optic Nerve
Function: Vision (afferent limb of pupillary light reflex)
Components to test:
1. Visual Acuity
- Test each eye separately with best correction (glasses/contacts)
- Use a Snellen chart at 6 m (20 ft) or a near card at 35 cm
- Record as fraction (20/20, 20/200, etc.)
2. Visual Fields by Confrontation
- Sit ~0.6–1.0 m (2–3 ft) from the patient
- Patient fixes gaze on your nose
- Hold hands at the periphery of your visual field, equidistant between you and the patient
- Wiggle a finger in each quadrant (inferior then superior) — monocularly and simultaneously
- Binocular simultaneous testing screens for visual neglect; individual eye testing detects monocular defects
- Formal perimetry (Humphrey/Goldmann) if an abnormality is found
3. Fundoscopy
Examine with an ophthalmoscope. Note:
- Optic disc: color (pale = atrophy), margins (blurred = papilledema), cup-to-disc ratio
- Retinal vessels: arteriovenous nicking, caliber changes, hemorrhages, exudates
- Retina: pigmentary changes, emboli, macular appearance
4. Pupillary Light Reflex (afferent limb = CN II)
- Shine a bright light in each eye; assess for briskness of constriction
- Relative Afferent Pupillary Defect (RAPD / Marcus Gunn pupil): in the swinging flashlight test, the affected eye dilates when light swings to it, indicating optic nerve dysfunction on that side
CN III, IV, VI — Oculomotor, Trochlear, Abducens
Functions:
| Nerve | Muscle(s) | Action |
|---|---|---|
| CN III | Medial, superior, inferior rectus; inferior oblique; levator palpebrae; pupillary constrictor | Elevation, depression, adduction; eyelid elevation; pupil constriction |
| CN IV | Superior oblique | Intorsion, depression in adduction |
| CN VI | Lateral rectus | Abduction |
Pupils
- Describe size, shape, symmetry (document in mm if possible)
- Direct reflex: light → same eye constricts (efferent = CN III)
- Consensual reflex: light → opposite eye constricts
- Accommodation reflex: ask patient to follow your finger as it moves toward their nose → convergence + miosis + lens thickening
- Anisocoria: if >1 mm difference and one pupil is larger with ptosis → CN III palsy (parasympathetic compression — compressive lesions affect outer fibers first); if smaller pupil with ptosis and anhidrosis → Horner syndrome
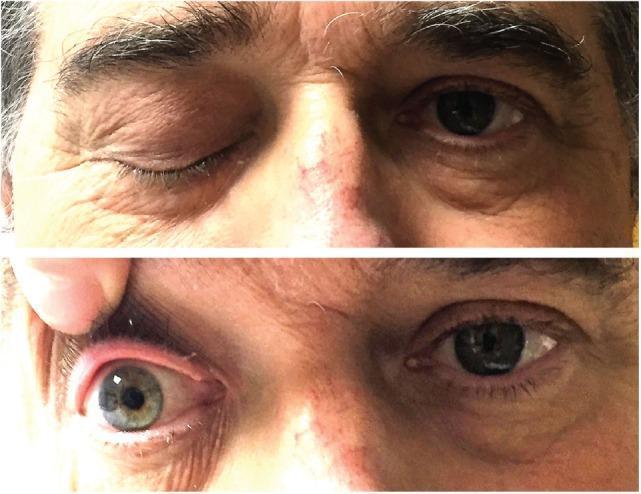
Extraocular Movements (EOM)
- Ask patient to keep head still and track your finger tip
- Move target in an H-pattern (horizontal, then diagonals)
- Test each direction: lateral (CN VI), medial (CN III), up-and-out (CN III superior rectus), down-and-out (CN III inferior rectus), up-and-in (CN III inferior oblique), down-and-in (CN IV superior oblique)
- Observe for: paresis (limitation), nystagmus, saccadic pursuit, diplopia (ask patient)
- True diplopia resolves on covering one eye
- Test for horizontal nystagmus at 45° lateral gaze (not extreme gaze); hold position for several seconds
CN V — Trigeminal Nerve
Function: Facial sensation (3 divisions) + motor to muscles of mastication + afferent limb of corneal reflex
Sensory Testing
Test all three divisions on each side of the face:
| Division | Territory |
|---|---|
| V1 (Ophthalmic) | Forehead, scalp, upper eyelid, cornea |
| V2 (Maxillary) | Cheek, lower eyelid, upper lip, upper teeth |
| V3 (Mandibular) | Lower jaw, lower lip, lower teeth, anterior tongue |
- Test light touch (cotton wisp) and pinprick or temperature (cold tuning fork)
- Compare left vs. right and between divisions
Corneal Reflex
- Touch cornea (not conjunctiva) with a fine wisp of cotton or sterile saline
- Normal: bilateral brisk eye closure
- Afferent limb = CN V1; efferent limb = CN VII
- Absent reflex on stimulus side → CN V lesion; absent closure only on stimulus side → CN VII lesion
Motor
- Ask patient to clench jaw → palpate masseter and temporalis muscles for bulk and symmetry
- Ask patient to open mouth against resistance
- With a unilateral lesion, jaw deviates toward the weak (ipsilateral) side on opening
CN VII — Facial Nerve
Function: Muscles of facial expression; taste anterior 2/3 of tongue; innervates lacrimal, sublingual, and submaxillary glands
Motor Testing (Upper and Lower Face)
- Forehead wrinkling — raise eyebrows
- Eye closure — close eyes tightly (Bell's phenomenon: upward eye deviation is normal)
- Cheek puff — puff out both cheeks; press to check for air escape
- Smile / show teeth — assess symmetry
- Platysma — grimace, pull mouth corners downward
Key distinction:
| Pattern | Lesion |
|---|---|
| Weakness of lower 2/3 face, forehead spared | Upper motor neuron (UMN) — contralateral cortex/corticobulbar tract |
| Weakness of entire ipsilateral face (forehead + lower) | Lower motor neuron (LMN) — CN VII nucleus or nerve itself (Bell's palsy) |
Taste
- Test anterior 2/3 of tongue on each side separately
- Apply sweet (sugar) or bitter (quinine) solution with cotton applicator
- Patient identifies while tongue is extended (to avoid spreading solution)

CN VIII — Vestibulocochlear Nerve
Function: Hearing (cochlear division) + balance (vestibular division)
Hearing (Cochlear Division)
- Screening: Rub fingers next to each ear, or whisper a number at 60 cm; test one ear at a time while the other is masked
- Rinne Test (512 Hz tuning fork):
- Place vibrating fork on mastoid process (bone conduction) → when no longer heard, place beside the ear canal (air conduction)
- Normal (Rinne positive): air conduction > bone conduction
- Conductive hearing loss (Rinne negative): bone conduction > air conduction
- Sensorineural loss: both diminished but air > bone maintained
- Weber Test:
- Place vibrating fork on forehead midline
- Normal: equal sound in both ears
- Sound lateralizes to the worse ear → conductive loss on that side
- Sound lateralizes to the better ear → sensorineural loss on the opposite side
- Formal audiometry if any abnormality detected
Vestibular Division
- Not routinely tested in standard exams
- In dizziness or coma: ice-water caloric stimulation (oculocephalic reflex), Dix-Hallpike maneuver
CN IX — Glossopharyngeal Nerve
Function: Sensation to pharynx and tonsillar fossa; taste to posterior 1/3 of tongue; afferent limb of gag reflex
Testing:
- Elicit the gag reflex by touching the posterior pharyngeal wall on each side separately with a tongue depressor or blunt probe
- Observe for symmetric response; may be absent in some normal individuals
- Taste on posterior 1/3 of tongue is rarely formally tested clinically
CN X — Vagus Nerve
Function: Motor to pharynx, soft palate, larynx; parasympathetic to thoracic and abdominal viscera; efferent limb of gag reflex
Testing:
- Ask patient to say "aah" — observe soft palate and uvula
- Normal: both sides of palate elevate symmetrically; uvula remains midline
- Unilateral vagus lesion: palate drops on the affected side; uvula deviates away from the lesion (toward the normal side)
- Hoarseness or dysphonia → suggests recurrent laryngeal nerve damage (branch of CN X)
- Gag reflex efferent arc — brisk bilateral contraction of pharyngeal muscles
CN XI — Spinal Accessory Nerve
Function: Motor to sternocleidomastoid (SCM) and upper trapezius
Testing:
- Trapezius (shoulder shrug): Ask patient to shrug both shoulders against downward resistance from your hands; compare sides for strength and bulk
- Sternocleidomastoid (head rotation): Ask patient to turn head to each side against your resisting hand placed on the cheek; the active muscle is contralateral to the direction of rotation (turning left = left SCM contracts on the side you resist)
- Inspect for muscle atrophy or asymmetry
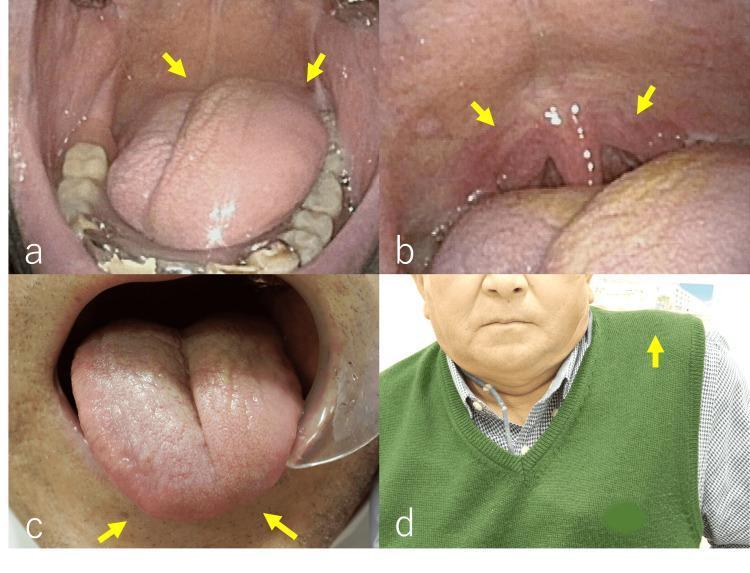
CN XII — Hypoglossal Nerve
Function: Motor to all intrinsic and most extrinsic tongue muscles
Testing:
- Inspect tongue at rest in the floor of the mouth: look for atrophy (hemiatrophy) and fasciculations (LMN lesion)
- Ask patient to protrude the tongue: midline is normal
- Tongue deviates toward the side of the lesion (LMN — the weak side cannot push)
- UMN lesion: tongue deviates away from the lesion (contralateral), no atrophy or fasciculations
- Test tongue strength: ask patient to press tongue against each inner cheek while you press from outside
Summary Table
| CN | Name | Key Functions | Test Method | Abnormal Finding |
|---|---|---|---|---|
| I | Olfactory | Smell | Identify odorant (eyes closed) | Anosmia |
| II | Optic | Vision, afferent pupillary | Acuity, fields, fundoscopy, RAPD | Decreased acuity, field defects, RAPD |
| III | Oculomotor | EOM (except SO, LR), ptosis, pupil constriction | Pupil light reflex, accommodation, H-pattern | Ptosis, mydriasis, "down and out" eye |
| IV | Trochlear | Superior oblique (down + in) | H-pattern, head tilt | Vertical diplopia, worse going down stairs |
| V | Trigeminal | Facial sensation, mastication | Touch/pin/temp in 3 divisions, jaw clench, corneal reflex | Hemisensory loss, absent corneal reflex, jaw deviation |
| VI | Abducens | Lateral rectus (abduction) | H-pattern (lateral gaze) | Esotropia, failure to abduct |
| VII | Facial | Facial expression, taste ant. 2/3 tongue | Wrinkle forehead, close eyes, smile, puff cheeks; taste | LMN: entire face weak; UMN: forehead spared |
| VIII | Vestibulocochlear | Hearing, balance | Whisper test, Rinne, Weber | Conductive vs. sensorineural loss |
| IX | Glossopharyngeal | Pharyngeal sensation, taste post. 1/3 tongue | Gag reflex (afferent) | Loss of gag (afferent) |
| X | Vagus | Palate/larynx motor, gag efferent | "Aah," uvula, gag reflex (efferent) | Uvula deviation, hoarseness, absent gag (efferent) |
| XI | Spinal Accessory | SCM, trapezius | Shoulder shrug, head turn against resistance | Weakness, atrophy of SCM/trapezius |
| XII | Hypoglossal | Tongue movement | Protrude tongue, press against cheeks | Deviation toward lesion, atrophy, fasciculations |
Sources:
- Harrison's Principles of Internal Medicine 22E (McGraw Hill, 2025) — CN Examination chapter
- Textbook of Family Medicine 9e — Cranial Nerve Examination
- Goldman-Cecil Medicine International Edition — Cranial Nerve & Coma Examination
Create a study guide PDF for cranial nerve testing I can print or share
Reading File
Running Command
Running Command
Writing File
Running Command
Running Command
Your credits are exhausted. Your daily credits reset tomorrow, or you can purchase a top-up for more.
This is a shared conversation. Sign in to Orris to start your own chat.