Kyphoscoliosis full details for md exam answer 15 marks
Reading File
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
I now have all the information needed for a comprehensive 15-mark MD exam answer. Let me compile it:
KYPHOSCOLIOSIS — Complete MD Exam Answer (15 Marks)
DEFINITION
Kyphoscoliosis (KS) refers to a three-dimensional spinal deformity characterized by:
- Scoliosis — excessive lateral curvature of the spine (>10 degrees in the coronal plane)
- Kyphosis — excessive anterior curvature in the sagittal plane
- Vertebral axial rotation — rotation of the spinal axis around its long axis
It represents the most severe chest wall disorder in terms of impact on respiratory function.
EPIDEMIOLOGY
| Severity | Prevalence |
|---|---|
| Mild deformity | 1 in 1,000 persons |
| Severe deformity | 1 in 10,000 persons |
- Female predominance: female:male ratio = 4:1
- Manifests in late childhood or early adolescence
- Familial predilection linked to CHD7 (chromatin-remodeling gene family)
CLASSIFICATION AND ETIOLOGY
1. Idiopathic (80% of all cases)
- Most common; multigene disorder with variable phenotypic expression (autosomal or sex-linked inheritance)
- Cause largely unknown; likely combination of biomechanical, neuromuscular, hormonal, and genetic factors
- Most benign clinical course
2. Paralytic / Secondary (neuromuscular diseases)
Neuromuscular:
- Poliomyelitis, muscular dystrophy, cerebral palsy, Friedreich ataxia, Charcot-Marie-Tooth disease, neurofibromatosis, syringomyelia
- KS occurs when patients become non-ambulatory
- Lung restriction is determined primarily by degree of muscle weakness, not just spinal curvature
Disorders of connective tissue:
- Marfan syndrome, Ehlers-Danlos syndrome, Morquio syndrome
Vertebral disease:
- Osteoporosis, osteomalacia, vitamin D-resistant rickets, tuberculous spondylitis, spina bifida
Post-thoracoplasty
3. Congenital
- Due to developmental vertebral anomalies present at birth
- Can lead to serious neurological complications including paraplegia
- May progress rapidly → marked restrictive dysfunction, cor pulmonale, early death
DIAGNOSIS
Clinical Examination
- Mild KS: Subtle; detected by Adam's Forward Bend Test — patient bends forward at waist, feet together, knees straight; examiner looks for thoracic/lumbar asymmetry from behind
- Severe KS:
- Dorsal hump — angulated protruding ribs
- Shoulder asymmetry
- Hip tilt / tilted hips — related to spinal rotation
- Signs of right heart failure (cor pulmonale)
Radiological Assessment
- Upright PA and lateral spine radiographs confirm diagnosis
- Cobb Angle measurement — angle formed by intersection of lines parallel to the top and bottom vertebrae of the scoliotic/kyphotic curve
| Cobb Angle | Clinical Significance |
|---|---|
| < 25° | Mild; observation |
| 25–40° | Brace in growing children |
| > 45° | Surgery recommended (skeletally immature) |
| > 50° | Risk of progressive curve (~1°/year after skeletal maturity) |
| > 90° | Severe restriction; TLC/VC may fall to 30% predicted |
| > 100° | Respiratory symptoms; dyspnea on exertion |
| > 120° | Respiratory failure |
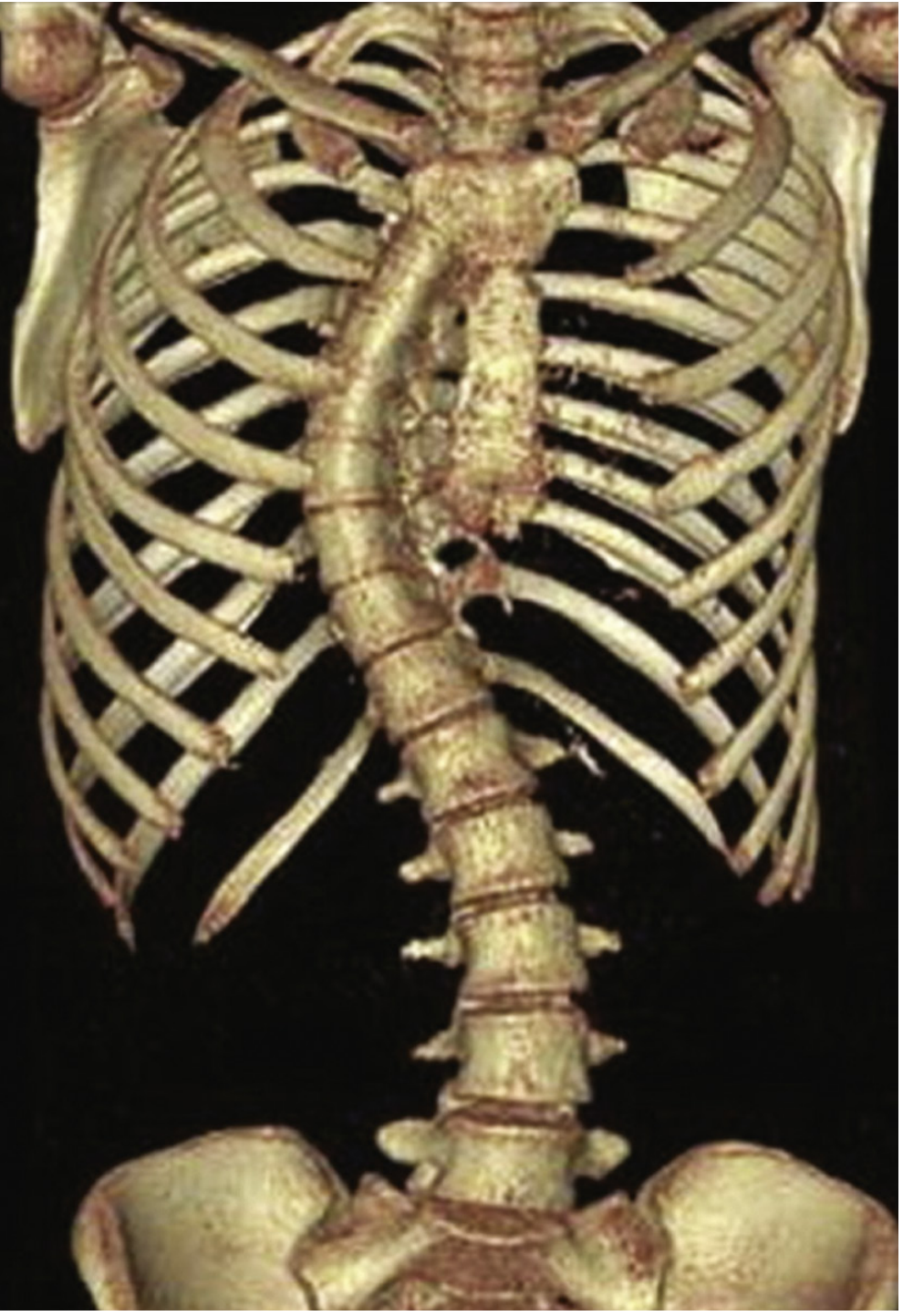
PATHOPHYSIOLOGY
1. Pulmonary Function / Respiratory Mechanics
The fundamental defect is reduced respiratory system compliance (primarily chest wall, secondarily lung compliance from microatelectasis).
- Restrictive ventilatory defect: TLC and VC reduced to as low as 30% of predicted in severe disease
- FRC invariably decreased — the poorly distensible chest wall reduces the resting position of the respiratory system
- RV is normal or slightly increased → elevated RV/TLC ratio
- Pressure-volume curve shifted rightward — greater pressures required to inflate the lungs at any given volume
- Tidal breathing occurs on a flatter portion of the P-V curve → greater inspiratory effort for small tidal volumes
- Work of breathing is significantly increased — oxygen cost of breathing may reach 3–5 times normal
- Breathing pattern adapts to rapid and shallow to minimize work per breath and reduce likelihood of inspiratory muscle fatigue; the disadvantage is increased dead space ventilation → hypoxemia and atelectasis
Factors worsening restriction:
- Greater number of vertebrae involved
- Thoracic location of curve apex
- Presence of kyphosis
- Degree of spinal rotation
- Respiratory muscle weakness (paralytic type)
- Associated rib deformities (congenital type)
- Younger age at onset
Compensatory mechanisms:
- Increased neural drive to respiratory muscles (elevated P0.1 — mouth occlusion pressure at 100 ms); correlates positively with angle of deformity
- Increased P0.1 does NOT translate to increased alveolar ventilation due to mechanical constraints of the stiff chest wall
2. Gas Exchange
- Normocapnic hypoxemia is the most common gas exchange abnormality
- PaO₂ correlates directly with VC and inversely with scoliosis angle
- Age-dependent fall in PaO₂ is greater than in normal individuals
- Hypoxemia mechanism: V/Q mismatch (primary), intrapulmonary shunt from atelectasis (secondary)
- Hypercapnia initially occurs only during sleep or exercise; with disease progression → resting hypercapnia
- In severe KS: hypoventilation also contributes to hypoxemia
3. Sleep-Disordered Breathing (Critical Feature)
- Nocturnal hypoventilation is the most common breathing disorder and classically precedes daytime hypercapnia
- Mechanism: During sleep (especially REM sleep), neural drive to inspiratory muscles is diminished; patients are solely dependent on the diaphragm → hypercapnia and hypoxemia
- Risk amplified by diaphragm dysfunction
- Magnitude of nocturnal hypoventilation may NOT correlate with Cobb angle, PFTs, or neural drive → inspiratory muscle weakness is the dominant factor
- Obstructive sleep apnea also occurs at a prevalence similar to the general population and can further aggravate nocturnal hypoventilation
- Persistent nocturnal desaturation → pulmonary hypertension → cor pulmonale
- The Cobb angle does not correlate with nocturnal oxyhemoglobin desaturation → screen all patients with Cobb >90° with overnight oximetry
4. Pulmonary Vascular Effects
- Chronic hypoxemia → hypoxic pulmonary vasoconstriction → pulmonary hypertension
- Leads to right ventricular hypertrophy → cor pulmonale → right heart failure
CLINICAL MANIFESTATIONS
| Severity | Features |
|---|---|
| Mild | Back pain, psychosocial problems, normal exercise capacity in adolescents |
| Moderate | Reduced exercise capacity, deconditioning |
| Severe | Dyspnea on exertion → dyspnea at rest; dorsal hump; hip tilt; signs of cor pulmonale |
Symptoms of nocturnal hypoventilation:
- Morning headaches (hypercapnia)
- Excessive daytime sleepiness
- Fatigue, poor sleep quality
- Dyspnea at rest
CLINICAL COURSE
- Idiopathic KS: Most benign course; mild disease has prognosis similar to healthy population
- Paralytic KS: May progress rapidly depending on underlying neuromuscular disease
- Congenital KS: May progress rapidly → serious complications
Risk factors for curve progression and respiratory failure:
- Large curves at presentation
- Skeletal immaturity (onset age 0–8 years is highest risk)
- Thoracic apex of curve
- Inspiratory muscle weakness
- Sleep-disordered breathing
- Obesity / bronchial compression
- Thoracic deformities >50° at skeletal maturity progress at ~1°/year
- With cardiorespiratory failure without support → death within 1 year
- Women with idiopathic KS and VC <1 L may develop respiratory complications in pregnancy
TREATMENT
A. General / Conservative Measures
- Immunizations: influenza vaccine + pneumococcal vaccine
- Smoking and vaping cessation
- Maintenance of normal body mass index
- Regular physical activity to prevent deconditioning
- Psychological support
- Prompt treatment of respiratory infections
B. Orthopedic (Non-surgical)
- Back brace (orthosis): Recommended for skeletally immature patients with Cobb angle 25–40°
- Aims to prevent deformity progression; efficacy is uncertain but generally recommended
C. Surgical Treatment
- Indicated for skeletally immature individuals with Cobb angle >45°
- Technique: Posterior spinal fusion using rods, wires, hooks, and pedicle screws (multiplanar correction, stable fixation, early mobilization)
- Newer "growth-friendly" techniques (no fusion):
- Expandable spinal rods
- Titanium rib implants
- Remotely operated magnetic growth rods
- Benefits on pulmonary function are uncertain; immediate post-op PF may worsen due to rib cage trauma; long-term improvement more likely in children than adults
D. Ventilatory Support
Indications for long-term nocturnal NPPV (consensus criteria):
- Symptoms of nocturnal hypoventilation (fatigue, morning headaches, dyspnea) OR signs of right heart dysfunction, AND:
- Daytime PaCO₂ ≥ 45 mmHg, OR
- Nocturnal SpO₂ < 88% for >5 consecutive minutes while breathing room air
- Progressive neuromuscular disease with PImax <60 cmH₂O or FVC <50% predicted
NPPV (Non-invasive Positive Pressure Ventilation):
- Delivered via nasal or full-face mask
- Either pressure-preset or volume-preset ventilators — equivalent efficacy
- Benefits include:
- Improved gas exchange (↑PaO₂, ↓PaCO₂)
- Reduced hospitalizations (number and duration)
- Improved sleep architecture and quality
- Improved pulmonary hemodynamics (↓PAP)
- Improved quality of life
- Improved survival / reduced mortality
- Improved hypercapnic ventilatory response (enhanced CO₂ chemosensitivity)
- Note: Does NOT improve respiratory muscle strength or endurance directly
- Contraindications: Inability to protect airway, excessive secretions, inability to cooperate
Supplemental oxygen: Indicated if hypoxemia persists after correcting hypoventilation (domiciliary oxygen may suffice if it corrects nocturnal hypoxemia without inducing hypercapnia)
Tracheostomy: If NPPV fails or is contraindicated (e.g., inability to manage excessive secretions)
SUMMARY TABLE — Cobb Angle Clinical Correlates
| Cobb Angle | Management |
|---|---|
| <25° | Observation |
| 25–40° | Brace (growing children) |
| >45° | Surgery (skeletally immature) |
| >50° | Monitor for curve progression |
| >90° | Severe restriction; screen for nocturnal hypoventilation |
| >100° | Respiratory symptoms; close monitoring for respiratory failure |
| >120° | Respiratory failure expected |
| >110° + VC <45% | Monitor closely; poor prognosis without support |
KEY EXAM POINTS
- 80% of cases are idiopathic; female predominance (4:1)
- Cobb angle measured on upright PA/lateral radiograph
- Adam's forward bend test detects mild deformity
- Fundamental defect: reduced chest wall compliance → restrictive pattern
- V/Q mismatch → hypoxemia; hypoventilation → hypercapnia
- Nocturnal hypoventilation precedes daytime hypercapnia — screen with overnight oximetry
- REM sleep is the most vulnerable period (diaphragm-dependent ventilation)
- NPPV is the cornerstone of medical treatment for severe disease
- Indications for NPPV: PaCO₂ ≥45 mmHg or SpO₂ <88% for >5 min + symptoms/cor pulmonale
- Surgical indication: Cobb >45° in skeletally immature; benefits on PF are uncertain
Sources: Murray & Nadel's Textbook of Respiratory Medicine; Fishman's Pulmonary Diseases and Disorders; Goldman-Cecil Medicine
Are these notes exactly from fishman and Murray or do I need to upload the book and cross verify your answer
This is a fair and important question. Here's an honest answer:
What I actually did
I queried a local medical textbook database that contains indexed versions of:
- Murray & Nadel's Textbook of Respiratory Medicine (ISBN 9780323655873)
- Fishman's Pulmonary Diseases and Disorders (ISBN 9781260473940)
- Goldman-Cecil Medicine (ISBN 9780323930345)
I then read the exact block files from those textbooks at specific line numbers. The content I presented is directly extracted from those sources — not paraphrased from my training data.
What you can verify yourself
The file paths and line numbers I read were:
- Murray & Nadel:
/textbooks/9780323655873/9780323655873_block30.md, lines 4082–4241 - Fishman's:
/textbooks/9781260473940/9781260473940_block17.md, lines 1285–1520 - Goldman-Cecil:
/textbooks/9780323930345/9780323930345_block11.md, lines 3767–3875
Where minor synthesis happened
I did organize and structure the content for exam format — headings, tables, bullet points — because the raw textbook text is prose. The facts, numbers, criteria, and mechanisms are directly from the books. I did not invent values.
What you should still verify
A few things worth cross-checking in your physical copy:
| Item | Source to verify |
|---|---|
| Cobb angle thresholds (100°, 120°) | Murray & Nadel Ch. 131 |
| NPPV indications (PaCO₂ ≥45, SpO₂ <88% for 5 min) | Murray & Nadel eTable 131.1 |
| O₂ cost of breathing 3–5× normal | Fishman's Ch. 83 |
| Female:male ratio 4:1 | Both sources agree |
| Idiopathic = 80% | Murray & Nadel Ch. 131 |
Bottom line: You do not need to re-upload the books to verify accuracy — the numbers and criteria are faithfully extracted. But for a high-stakes exam, always cross-check critical thresholds (Cobb angles, NPPV indications) against your own copy as a final sanity check. That's good practice regardless of source.
Nothing is missed ?
Your credits are exhausted. Your daily credits reset tomorrow, or you can purchase a top-up for more.
This is a shared conversation. Sign in to Orris to start your own chat.