Placental development. The role of the chorion in the formation of the placenta. The structure and role of the hematoplacental barrier
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Loading Image
Loading Image
Loading Image
I now have comprehensive information from multiple authoritative textbooks. Let me compile a thorough answer.
Placental Development, the Role of the Chorion, and the Hematoplacental Barrier
1. Overview: The Placenta as a Fetomaternal Organ
The placenta is a fetomaternal organ with two components:
- Fetal part — derived from the villous chorion (chorion frondosum)
- Maternal part — derived from the decidua basalis (endometrium)
It serves as the primary transport system between mother and fetus, performing respiration, nutrition, excretion, protection, and hormone production. — The Developing Human: Clinically Oriented Embryology
2. The Decidua
The decidua is the endometrium of the pregnant uterus — the functional layer that separates after parturition. It has three regions named by their relation to the implantation site:
| Region | Location | Role |
|---|---|---|
| Decidua basalis | Deep to the conceptus | Forms the maternal part of the placenta |
| Decidua capsularis | Superficial layer overlying the conceptus | Compresses and eventually fuses with decidua parietalis |
| Decidua parietalis | Remaining endometrium | Lines the remainder of the uterine cavity |
In response to rising progesterone, connective tissue cells enlarge into decidual cells, accumulating glycogen and lipid. These cells nourish the early embryo, may protect against uncontrolled trophoblast invasion, and contribute to hormone production (decidual reaction). — The Developing Human
3. Development of the Placenta
3.1 Trophoblast Differentiation and Early Uteroplacental Circulation
After implantation (~day 9), the trophoblast differentiates into two populations:
- Syncytiotrophoblast: multinucleated, invasive, actively erodes the decidua; forms trophoblastic lacunae filled with maternal blood
- Cytotrophoblast (Langhans cells): mitotically active inner layer that supplies new cells to the syncytiotrophoblast
Maternal sinusoids anastomose with the trophoblastic lacunae by ~day 9, establishing a primitive uteroplacental circulation driven by the pressure differential between spiral arteries and veins. — Histology: A Text and Atlas
3.2 Formation of Chorionic Villi
Villi develop through three successive stages:
Primary villi (days 11–13): Rapidly proliferating cytotrophoblast sends solid cords into the blood-filled lacunae of the syncytiotrophoblast.
Secondary villi: Extraembryonic mesenchyme (chorionic mesoderm) grows into the cytotrophoblastic cores; the villus now has a mesenchymal stroma surrounded by cytotrophoblast.
Tertiary villi: Blood vessels differentiate within the mesenchymal core; this is when the barrier between fetal and maternal blood is properly established.
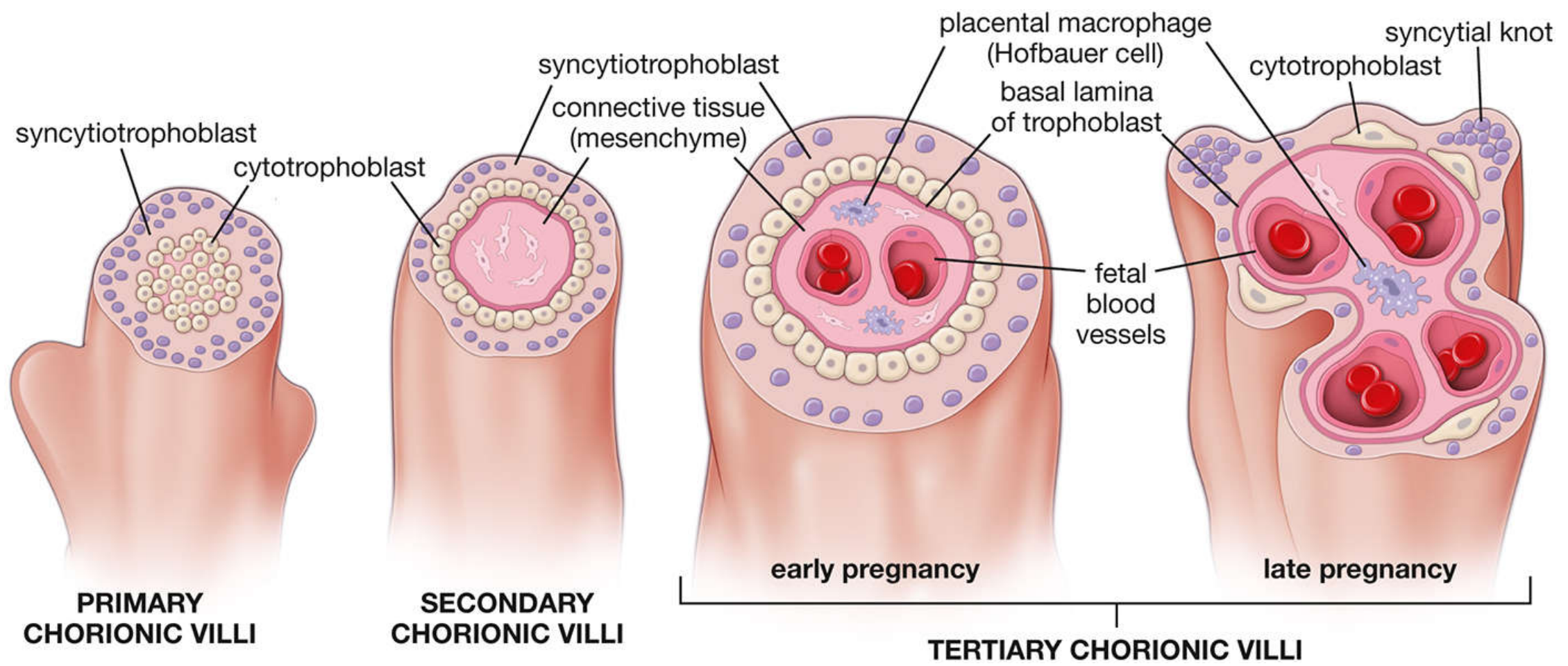
Developmental stages of chorionic villi — Histology: A Text and Atlas
In early pregnancy, villi are large, edematous, with few vessels and a thick continuous syncytiotrophoblast + cytotrophoblast covering. In late pregnancy, the cytotrophoblast layer becomes thin and discontinuous; syncytial knots form. — Histology: A Text and Atlas
4. The Role of the Chorion in Placental Formation
4.1 Smooth Chorion vs. Villous Chorion
Until the 8th week, chorionic villi cover the entire chorionic sac. As the sac grows, two zones differentiate:
- Chorion laeve (smooth chorion): Villi on the side of the decidua capsularis are compressed and their blood supply reduced → they degenerate → a relatively avascular, smooth surface results
- Chorion frondosum (villous chorion): Villi on the side of the decidua basalis proliferate vigorously, branch profusely, and enlarge → this forms the fetal part of the placenta
The shape of the placenta (typically discoid) is determined by the persistent area of the chorion frondosum. — The Developing Human
4.2 Cytotrophoblastic Shell and Attachment
The fetal part attaches to the maternal decidua through the cytotrophoblastic shell — an external layer of trophoblastic cells on the maternal surface of the placenta that anchors the chorionic sac to the decidua basalis. Endometrial arteries and veins pass through gaps in this shell to supply the intervillous space.
4.3 Cotyledons and Placental Septa
As chorionic villi invade the decidua basalis, wedge-shaped projections of decidual tissue — placental septa — extend toward the chorionic plate, dividing the fetal portion into 15–30 irregular convex areas called cotyledons. Each cotyledon consists of two or more stem villi and many branch villi. By the end of the 4th month, the decidua basalis is almost entirely replaced by fetal cotyledons.
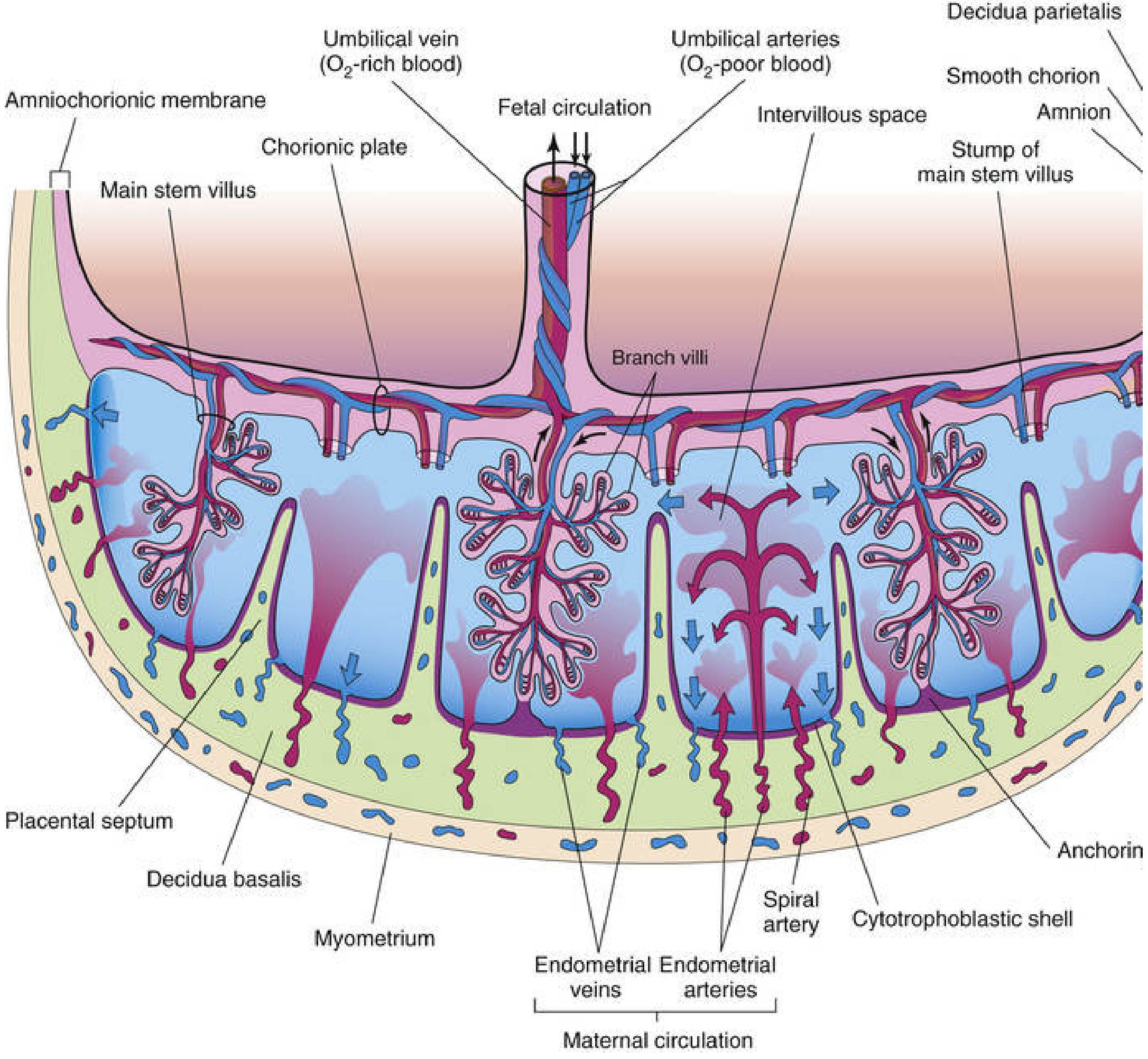
Cross-section of full-term placenta — The Developing Human: Clinically Oriented Embryology
4.4 Maternal Blood Supply
80–100 spiral endometrial arteries penetrate the basal plate, injecting maternal blood into the base of the intervillous spaces at each pulse. The intervillous space contains approximately 150 mL of maternal blood exchanged 3–4 times per minute. Blood flows up toward the chorionic plate, bathes the villi (where exchange occurs), and drains via endometrial veins. — Histology: A Text and Atlas
5. Structure of the Hematoplacental Barrier
The hematoplacental barrier (placental membrane) is the composite structure of fetal tissue layers separating maternal blood in the intervillous space from fetal blood in the villous capillaries. Fetal and maternal blood do not normally mix.
5.1 Layers of the Barrier
Early pregnancy (before ~20 weeks) — 4 layers:
- Syncytiotrophoblast — outer multinucleated layer with dense microvilli; the critical barrier layer
- Cytotrophoblast — inner continuous layer of mononuclear cells (Langhans cells)
- Connective tissue (mesenchyme) of the villus
- Endothelium of fetal capillaries
Late pregnancy (after ~20 weeks) — thinned to 3 (or fewer) layers:
The cytotrophoblast becomes attenuated and then discontinuous over large areas. In many villi the effective barrier is:
- Syncytiotrophoblast
- Basal lamina of the trophoblast
- Connective tissue of the villus
- Basal lamina of the endothelium
- Endothelium of fetal capillary
At its thinnest (vasosyncytial membrane), the syncytiotrophoblast comes into direct contact with the endothelium of the fetal capillaries, maximizing exchange. — The Developing Human; Histology: A Text and Atlas
Color Atlas of Human Anatomy summarises the early barrier as 6 layers: syncytiotrophoblast → cytotrophoblast → basal plate → connective tissue of fetal villi → basal lamina of fetal capillaries → endothelium.
5.2 Electron-Microscopic Appearance
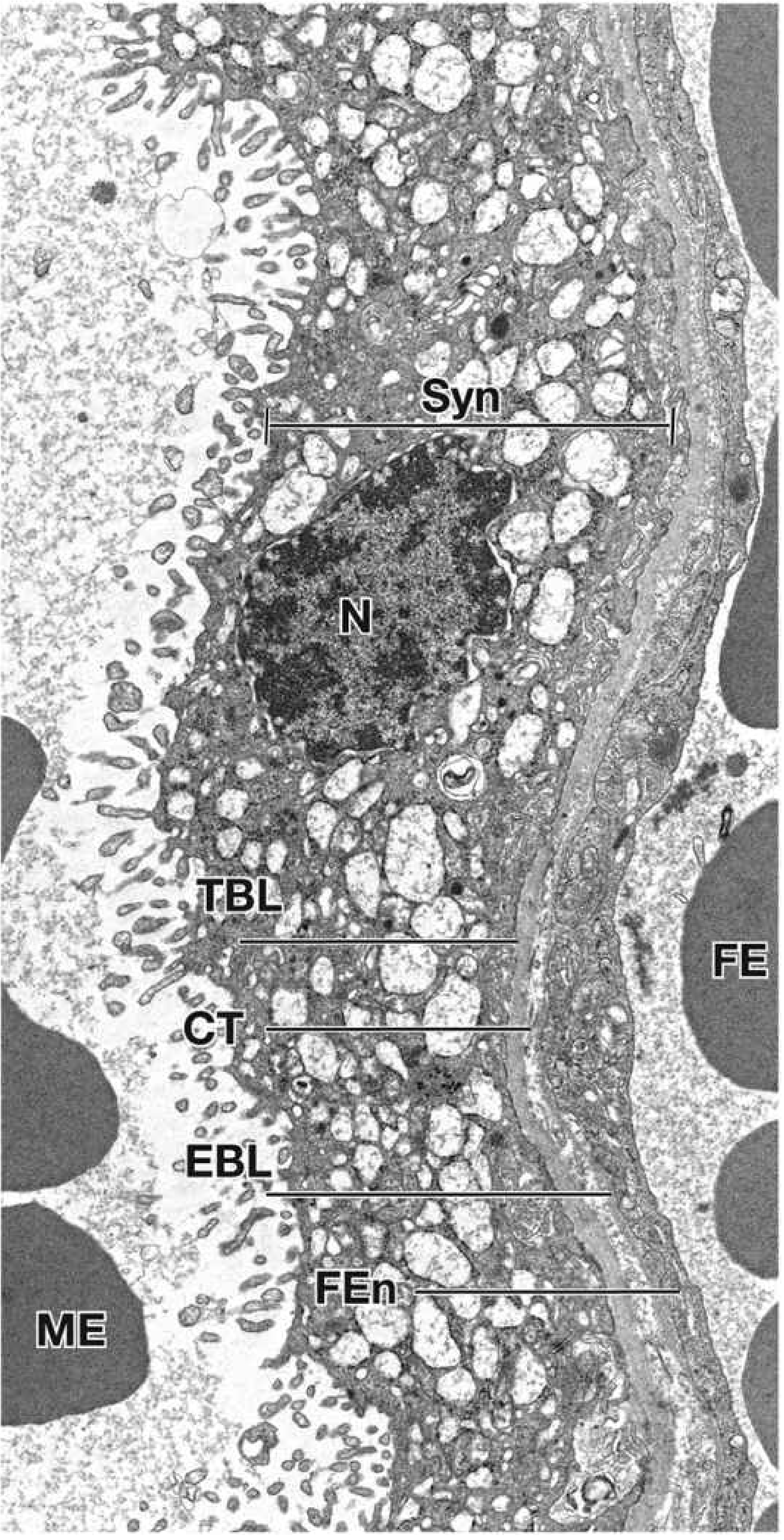
Electron micrograph of the third-trimester placental barrier (×11,000) — Histology: A Text and Atlas
Key ultrastructural features of the syncytiotrophoblast:
- Dense microvilli on the apical surface (increases surface area for exchange)
- Abundant transport vesicles, rER, sER, mitochondria
- No lateral intercellular gaps (tight barrier function)
5.3 Changes Through Pregnancy
| Feature | Early pregnancy | Late pregnancy |
|---|---|---|
| Cytotrophoblast layer | Continuous, thick | Thin or discontinuous |
| Syncytiotrophoblast | Thick, few nuclei | Thinner; forms syncytial knots |
| Fetal vessels | Sparse in stroma | Numerous, close to surface |
| Barrier thickness | Thick (4+ layers) | Markedly attenuated |
| Fibrinoid material | Absent | Accumulates on villus surfaces |
Syncytial knots — multinucleated protrusions of syncytiotrophoblast that regularly break off into the maternal circulation and are destroyed in the pulmonary capillaries.
6. Functions of the Hematoplacental Barrier
6.1 Substances Transferred from Mother → Fetus
| Substance | Mechanism |
|---|---|
| O₂ | Simple diffusion |
| Glucose | Facilitated diffusion (GLUT-1) |
| Amino acids | Active transport (against gradient) |
| Water | Simple diffusion |
| Vitamins | Diffusion (water-soluble > fat-soluble) |
| IgG antibodies | Pinocytosis → passive immunity |
| Electrolytes, hormones | Various |
6.2 Substances Transferred from Fetus → Mother
CO₂, metabolic waste products, water, some hormones — by simple diffusion.
6.3 Barrier Limitations
The term "placental barrier" is considered a misnomer because very few substances are genuinely excluded. The barrier is effective only when a molecule is of a specific size, configuration, or charge (e.g., heparin). Most drugs, alcohol, nicotine, viruses, exogenous hormones, and heavy metals cross freely. — The Developing Human
Large proteins are transferred very slowly by pinocytosis. Protein hormones (e.g., insulin) do not cross in significant amounts; steroid hormones cross readily.
6.4 Endocrine Function
The placenta is a major endocrine organ producing:
- Steroid hormones: chiefly progesterone (maintains pregnancy, inhibits uterine contractions)
- Protein hormones: hCG (maintains corpus luteum), human chorionic somatomammotropin (hCS), relaxin, leptin
Summary Diagram of Placental Organisation
The mature placenta:
- Fetal side (chorionic plate): umbilical arteries divide radially → stem villi → branch villi with capillary networks
- Intervillous space: filled with ~150 mL maternal blood renewed 3–4×/min
- Maternal side (basal plate): decidua basalis + cytotrophoblastic shell; 80–100 spiral arteries pierce it
- Cotyledons: 15–30 units separated by placental septa, each with 2+ stem villi
Sources:
- The Developing Human: Clinically Oriented Embryology (Moore, Persaud & Torchia)
- Histology: A Text and Atlas with Correlated Cell and Molecular Biology (Ross & Pawlina)
- Color Atlas of Human Anatomy, Vol. 2: Internal Organs (Schünke et al.)
Make ppt of on this topic in about 10-15 slides
Reading File
Reading File
Reading File
Running Command
Running Command
Running Command
!
Your input exceeds the context window of this model. Please adjust your input and try again.
We encountered an error while processing your request. Please try again or reach out to us for help.
Placental development. The role of the chorion in the formation of the placenta. The structure and role of the hematoplacental barrier ,for histology
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Your credits are exhausted. Your daily credits reset tomorrow, or you can purchase a top-up for more.
This is a shared conversation. Sign in to Orris to start your own chat.