Evaluate this case
Reading File
Finding Sources
Finding Sources
Finding Sources
Searching the Web
fever chills dark urine lower back pain irregular periods dysuria differential diagnosis young female
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
I now have sufficient information for a comprehensive case evaluation. Let me synthesize this fully.
Case Evaluation — 30/04/26, 3:30 PM
Extracted Clinical Information
Vitals:
| Parameter | Value | Interpretation |
|---|---|---|
| Temperature | 100°F (37.8°C) | Low-grade fever |
| SpO₂ | 96% | Borderline low (normal ≥98%) |
| Pulse Rate | 125/min | Tachycardia |
| Blood Pressure | 90/70 mmHg | Hypotension (borderline/early shock) |
Complaints (×2 days):
- Fever and chills (worse at night)
- Abdominal pain (lower)
- Lower back pain — stated as the 1st/initial symptom
- Dark urine
- Irregular periods
- No nausea/vomiting, no dysuria, no loose stools, no cold/cough at presentation
On Examination:
- Conscious and oriented
- RS → Clear, AEBE (Air Entry Bilateral Equal)
- CVS → S1S2+ (normal heart sounds)
- P/A → Soft, Non-tender
- CNS → NFND (No Focal Neurological Deficit)
Investigations ordered: CBC, ESR, URE (Urine Routine Examination)
Clinical Analysis
Key Pattern Recognition
This presentation in a female patient of likely reproductive age features:
- Fever + chills (night spikes) → cyclical or infectious
- Lower back pain as the first symptom → renal/retroperitoneal origin
- Dark urine → hemoglobinuria, hematuria, myoglobinuria, or bilirubinuria
- Irregular periods → hormonal disruption, systemic illness, or pelvic pathology
- HR 125 + BP 90/70 → early sepsis / SIRS criteria met (fever + tachycardia + hypotension)
- Non-tender abdomen despite abdominal pain → possible visceral/referred pain
Differential Diagnoses (in order of probability)
1. 🔴 Acute Pyelonephritis (Most Likely)
The clinical triad — fever, chills, flank/loin pain + dark urine — strongly points here. Classic presentation per Campbell-Walsh Urology: "chills, fever, and flank pain accompanied by bacteriuria and pyuria." Rosen's Emergency Medicine confirms: "fever, chills, flank pain, costovertebral angle tenderness, and nausea or vomiting."
- Lower back pain as the first symptom = renal origin before full infection establishes
- Dark urine = hematuria or pyuria-related turbidity
- Tachycardia + hypotension = early urosepsis — a well-recognized complication; pyelonephritis is a leading cause of septic shock in women
- Irregular periods = systemic febrile illness disrupting menstrual cycle, or concurrent UTI-related pelvic inflammation
- SpO₂ 96% warrants monitoring (ARDS is a known complication if sepsis progresses)
2. 🟡 Pelvic Inflammatory Disease (PID)
Supports: lower abdominal pain, irregular periods, young female. Against: lower back pain as initial symptom, dark urine, and non-tender abdomen (PID typically causes significant pelvic tenderness). Could coexist.
3. 🟡 Malaria (if endemic area/travel history — South Asian context likely)
Fever + chills at night, dark urine (hemoglobinuria in falciparum = "blackwater fever"), and constitutional symptoms fit. The date (30/4/26) and clinical setting suggest India/South Asia where falciparum/vivax malaria is endemic. Must be excluded.
4. 🟠 Typhoid Fever / Enteric Fever
Fever worsening progressively, abdominal pain, relative bradycardia is classic — but this patient has tachycardia, making uncomplicated typhoid less likely. Possible co-infection.
5. 🟢 Hemolytic Anemia (e.g., G6PD crisis)
Dark urine (hemoglobinuria), fever, chills, abdominal pain. Tintinalli's notes: "attacks of high fever, chills, headache, abdominal cramps... dark urine or hemoglobinuria." Less likely without precipitant, but CBC is essential.
Vital Sign Alarm 🚨
| Finding | Significance |
|---|---|
| HR 125 + Temp 100°F | SIRS criteria (2/4 met) |
| BP 90/70 | Borderline septic hypotension |
| SpO₂ 96% | Early respiratory compromise possible |
This patient meets criteria for early sepsis — the combination of a presumed infection source (likely urinary) + tachycardia + hypotension demands urgent management, not just investigations.
Immediate Management Plan
Urgent (do NOW):
- IV access — two large-bore cannulae
- IV fluid resuscitation — 500 mL crystalloid bolus (0.9% NS or Ringer's Lactate), reassess BP and HR
- Blood cultures × 2 (before antibiotics)
- Urine culture + sensitivity (midstream clean catch before antibiotics)
- Empirical IV antibiotics — Ceftriaxone 1g IV or Piperacillin-Tazobactam (for urosepsis/pyelonephritis)
- Monitor urine output (catheterise if needed)
Investigations (already ordered + additions):
| Test | Purpose |
|---|---|
| CBC | Leukocytosis (infection), anaemia (haemolysis/malaria) |
| ESR | Inflammatory marker |
| Urine Routine + Microscopy | Pyuria, casts, hematuria |
| Urine C&S | Identify organism + sensitivity |
| Blood cultures × 2 | Rule out bacteraemia |
| Peripheral blood smear | Malaria (given dark urine + cyclical chills) |
| RFT (Renal function tests) | Baseline creatinine — monitor for AKI |
| LFT | Malaria, hepatitis |
| Serum electrolytes | Electrolyte imbalance from fever/poor intake |
| Pregnancy test (urine β-hCG) | Essential in reproductive-age female before any imaging/antibiotics |
| Pelvic ultrasound | If PID suspected; also assess kidneys |
Summary
Working Diagnosis: Acute Pyelonephritis with early urosepsis in a young woman, presenting with classic loin pain → fever → dark urine triad, now with haemodynamic compromise (HR 125, BP 90/70). Malaria must be urgently excluded given night chills and dark urine.
The non-tender abdomen despite abdominal pain is a key clue — it suggests visceral/referred pain (kidney capsule distension) rather than peritoneal irritation, consistent with a retroperitoneal source.
The ordered investigations (CBC, ESR, URE) are appropriate but insufficient — urine culture, blood cultures, renal function tests, and a malaria smear should be added. IV fluid resuscitation and empirical antibiotics should not be delayed pending results given the haemodynamic instability.
— Rosen's Emergency Medicine, p.1390 | Creasy & Resnik's Maternal-Fetal Medicine, p. (Pyelonephritis section) | Comprehensive Clinical Nephrology, 7th Ed.
SIRS
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Loading Image
SIRS — Systemic Inflammatory Response Syndrome
Definition
SIRS is a non-specific exaggerated systemic inflammatory response to a stressor (infectious or non-infectious), defined clinically by meeting ≥2 of 4 criteria from the original 1992 consensus definition.
"SIRS is the result of proinflammatory cytokines related to tissue malperfusion or injury. The dominant cytokines implicated include IL-1, IL-6, and TNF." — Schwartz's Principles of Surgery, 11e
The 4 Classic SIRS Criteria (1992 Bone Criteria)
| # | Parameter | Criterion |
|---|---|---|
| 1 | Temperature | >38°C (>100.4°F) or <36°C |
| 2 | Heart Rate | >90 bpm |
| 3 | Respiratory Rate | >20 breaths/min or PaCO₂ <32 mmHg |
| 4 | WBC | >12,000/μL or <4,000/μL or >10% band forms |
Diagnosis requires ≥2 of these 4 criteria.
Applying to the Case (30/04/26)
| SIRS Criterion | Patient's Value | Met? |
|---|---|---|
| Temp >38°C | 100°F = 37.8°C | ❌ Borderline (just below threshold) |
| HR >90 bpm | 125 bpm | ✅ YES |
| RR >20 or PaCO₂ <32 | Not documented | ⚠️ Unknown |
| WBC >12,000 or <4,000 | Pending (CBC ordered) | ⚠️ Pending |
Confirmed SIRS criteria met: at minimum 1 (HR). Likely ≥2 once CBC returns.
Additionally, the patient has:
- SBP 90 mmHg → meets hypotension criterion from the extended Sepsis-2 criteria
- SpO₂ 96% → possible early respiratory compromise
SIRS → Sepsis → Severe Sepsis → Septic Shock Continuum
SIRS (≥2 criteria)
↓ + confirmed/suspected infection
SEPSIS
↓ + organ hypoperfusion or dysfunction
SEVERE SEPSIS
↓ + hypotension despite adequate fluid resuscitation
SEPTIC SHOCK
Per Schwartz's:
- Sepsis = SIRS + infection
- Severe Sepsis = Sepsis + signs of cellular hypoperfusion or end-organ dysfunction
- Septic shock = Sepsis + hypotension after adequate fluid resuscitation
In this patient: suspected urinary infection + tachycardia + borderline hypotension (BP 90/70) = Sepsis with features of early septic shock — pending adequate fluid challenge response.
Mortality by SIRS Criteria Count
| SIRS Criteria Met | Mortality |
|---|---|
| 2 criteria | ~5% |
| 3 criteria | ~10% |
| 4 criteria | 15–20% |
— Schwartz's Principles of Surgery, 11e
Sepsis-3 (2016) — The Modern Update
Sepsis-3 abandoned SIRS criteria as the primary definition because SIRS is non-specific (also occurs in trauma, burns, pancreatitis — see diagram below) and can be SIRS-negative in true sepsis.
Sepsis-3 defines sepsis as:
"Life-threatening organ dysfunction caused by a dysregulated host response to infection" Operationalized by a SOFA score increase of ≥2
qSOFA (bedside screen — no labs needed):
Score 1 point each for:
- Altered mental status
- SBP ≤100 mmHg
- RR ≥22 breaths/min
qSOFA ≥2 = suspected sepsis with poor outcome risk
This patient: SBP 90 mmHg (≤100) = 1 qSOFA point already. If RR ≥22, qSOFA = 2 → sepsis flag.
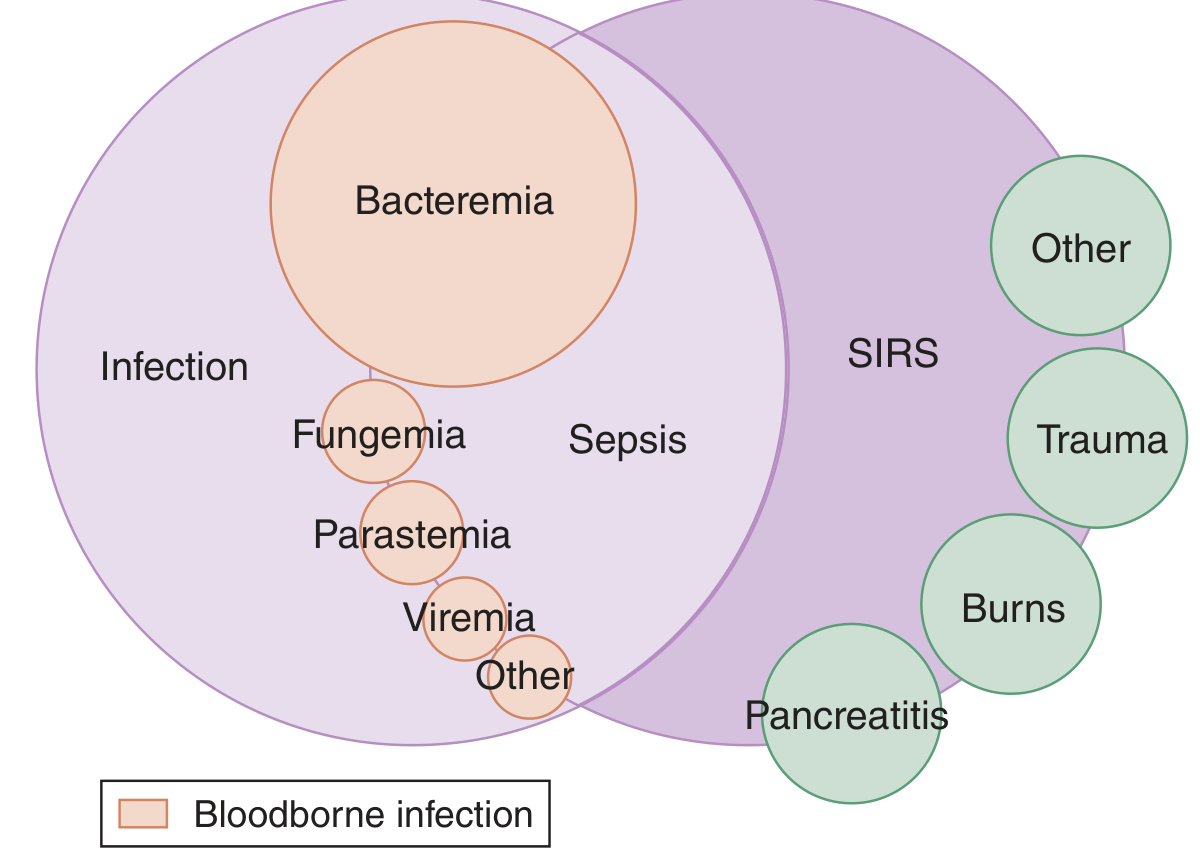
Interrelationship between SIRS, infection, and sepsis — Tintinalli's Emergency Medicine
Key Points
- SIRS ≠ Sepsis — SIRS is a response; sepsis requires a confirmed/suspected infectious source
- SIRS ≠ a diagnosis — it is a physiological stratification tool signalling systemic stress
- This patient has a presumed infectious source (pyelonephritis/urosepsis) + SIRS physiology = Sepsis
- The urinary tract is the #1 source of sepsis (48.9% of community-onset sepsis cases per Harrison's 22e)
- Serum lactate should be ordered — levels 2–4 mmol/L carry ~15% 28-day mortality even without hypotension
- Don't wait for labs — if SIRS + suspected infection + hypotension → start IV fluids + empirical antibiotics now
— Harrison's Principles of Internal Medicine 22e | Schwartz's Principles of Surgery 11e | Tintinalli's Emergency Medicine
Can you make a document about it
Reading File
Running Command
Running Command
Writing File
Running Command
Running Command
Your credits are exhausted. Your daily credits reset tomorrow, or you can purchase a top-up for more.
Hi
Your credits are exhausted. Your daily credits reset tomorrow, or you can purchase a top-up for more.
This is a shared conversation. Sign in to Orris to start your own chat.