Stye treatment
Reading File
Finding Sources
Searching PubMed
hordeolum stye treatment
Reading File
Reading File
Loading Image
Stye (Hordeolum) — Treatment
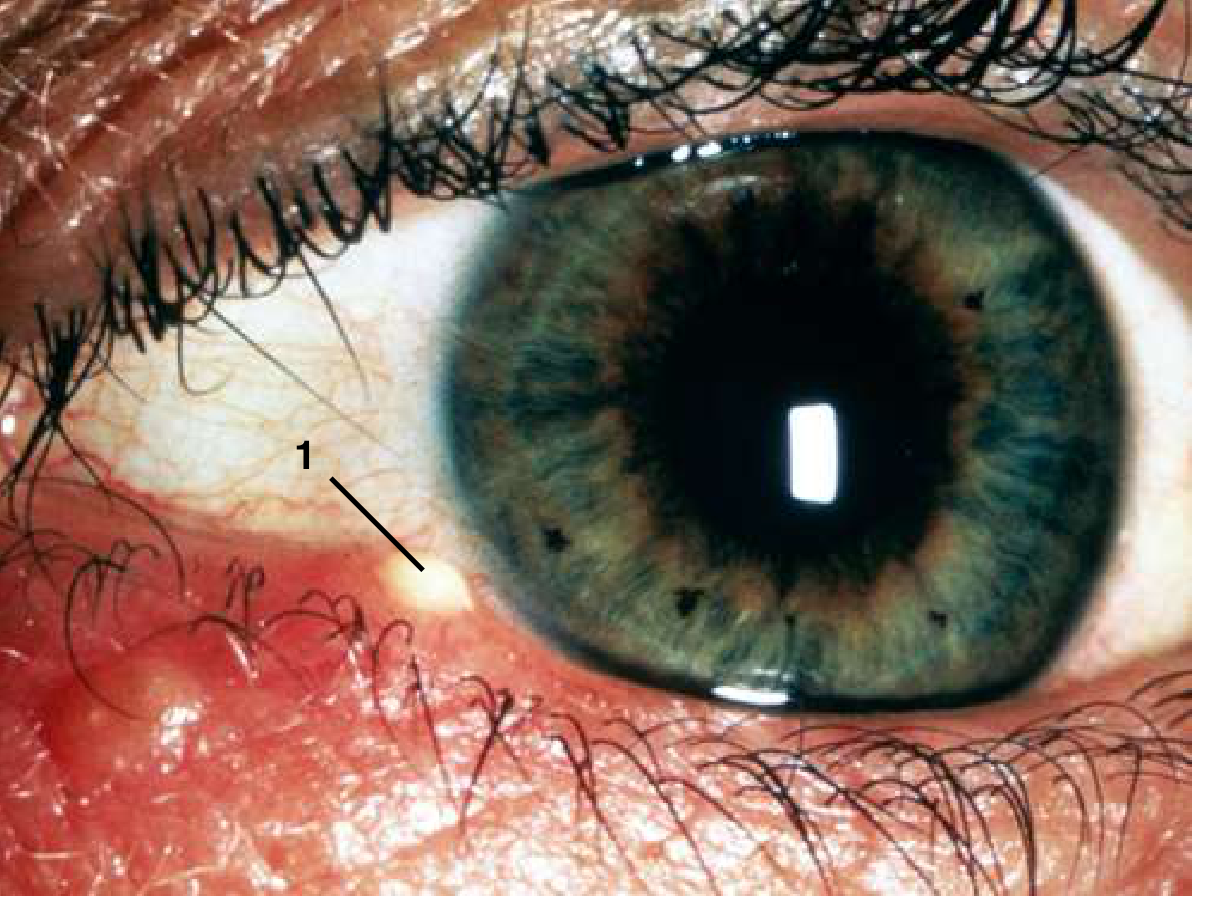
What Is a Stye?
A stye (hordeolum) is an acute bacterial infection — usually Staphylococcus aureus — of:
- External hordeolum: eyelash follicle and adjacent sebaceous (Zeis) or sweat (Moll) glands; presents as a pustule at the eyelid margin.
- Internal hordeolum: meibomian glands on the inner tarsal surface; similar symptoms but the pustule is on the inner eyelid.
Symptoms: pain, localized swelling, erythema, and edema of the eyelid.
Treatment
1. Warm Compresses (First-Line)
Apply a warm, moist cloth to the closed eyelid for 10–15 minutes, 4× daily. This promotes drainage and is the cornerstone of treatment. Most styes are self-limited and resolve with this alone.
2. Topical Antibiotics
Used alongside warm compresses:
- Erythromycin ophthalmic ointment — applied twice daily for 7–10 days (most commonly recommended)
- Bacitracin ointment — alternative topical option
- Fluoroquinolone drops (moxifloxacin or gatifloxacin) — alternative for external hordeolum
3. Eyelash Removal
Removing the offending eyelash can facilitate drainage and resolution, particularly for external hordeolum.
4. Systemic Antibiotics
Reserved for cases with significant surrounding cellulitis (preseptal/periorbital cellulitis). Not routinely required.
5. Incision and Drainage (I&D)
- Indicated when symptoms do not improve within 48 hours of conservative treatment.
- Should be performed by or referred to an ophthalmologist.
When to Refer to Ophthalmology
- No improvement after 48 hours of warm compresses + topical antibiotics
- Signs of orbital/preseptal cellulitis
- Recurrent lesions in the same location (may indicate underlying carcinoma)
- Internal hordeolum requiring I&D
Stye vs. Chalazion
| Feature | Stye (Hordeolum) | Chalazion |
|---|---|---|
| Cause | Bacterial infection | Lipogranulomatous inflammation (blocked meibomian gland) |
| Pain | Painful | Painless or mildly tender |
| Location | Lash margin (external) or tarsal plate (internal) | Within the eyelid (not at lash line) |
| Mobility | Fixed/inflamed | Non-mobile nodule |
| Treatment | Warm compresses + topical antibiotics | Warm compresses; surgical debridement if persistent |
Sources: Goldman-Cecil Medicine, p. 307; Tintinalli's Emergency Medicine, p. 1581
Ciplox eye drop
Finding Sources
Searching the Web
Ciplox eye drops ciprofloxacin ophthalmic uses dosage
Finding Sources
Reading Web Page
Ciplox ciprofloxacin eye drops dosage indications side effects
Reading Web Page
ciprofloxacin ophthalmic corneal ulcer dosage schedule
Ciplox Eye Drops (Ciprofloxacin 0.3% Ophthalmic Solution)
Ciplox is the brand name for ciprofloxacin 0.3% ophthalmic solution, a fluoroquinolone antibiotic used to treat bacterial eye infections.
Drug Class & Mechanism
- Class: Fluoroquinolone antibiotic
- Mechanism: Inhibits bacterial DNA gyrase (topoisomerase II) and topoisomerase IV → prevents DNA replication and repair → bactericidal action
- Spectrum: Broad-spectrum; covers Gram-positive and Gram-negative organisms
Indications
| Condition | Organisms Covered |
|---|---|
| Bacterial conjunctivitis | S. aureus, S. epidermidis, S. pneumoniae, H. influenzae |
| Corneal ulcers (keratitis) | P. aeruginosa, S. aureus, S. epidermidis, S. pneumoniae, Serratia marcescens |
| Stye / hordeolum (off-label supportive) | Staphylococcus spp. |
Dosage
Bacterial Conjunctivitis (Solution)
| Days | Dose |
|---|---|
| Days 1–2 | 1–2 drops into affected eye(s) every 2 hours while awake |
| Days 3–7 | 1–2 drops into affected eye(s) every 4 hours while awake |
Corneal Ulcer (Solution — more intensive)
| Time | Dose |
|---|---|
| Day 1, first 6 hours | 2 drops every 15 minutes |
| Day 1, remainder | 2 drops every 30 minutes |
| Day 2 | 2 drops every 1 hour |
| Days 3–14 | 2 drops every 4 hours |
May continue beyond 14 days if corneal re-epithelialization is incomplete.
Pediatric use: Same dosage for children ≥1 year (solution) and ≥2 years (ointment).
How to Instill
- Wash hands thoroughly.
- Tilt head back, pull down lower eyelid to form a pocket.
- Instill drop(s) into the conjunctival sac — do not touch the dropper tip to the eye or any surface.
- Close eye gently; press on the inner corner (nasolacrimal duct) for 1–2 minutes to reduce systemic absorption.
- Do not wear contact lenses during treatment for bacterial conjunctivitis.
Side Effects
Common (local):
- Burning or stinging on instillation
- Eye redness, itching, irritation
- Foreign body sensation
- Transient blurred vision (especially with ointment)
- White crystalline precipitate (in corneal ulcer treatment — benign, resolves)
Serious (seek medical attention):
- Skin rash, hives — possible hypersensitivity; stop immediately
- Facial/throat swelling, difficulty breathing — anaphylaxis
- Worsening eye pain or no improvement after a few days
Contraindications & Precautions
- Hypersensitivity to ciprofloxacin or any fluoroquinolone
- Do not use for viral (e.g., herpes simplex) or fungal eye infections
- Not for intraocular injection
- Prolonged use may cause superinfection or resistance
- Pregnancy/breastfeeding: Use only if clearly needed; systemic absorption from eye drops is minimal
Key Points
- Complete the full course even if symptoms improve early — stopping too soon can lead to antibiotic resistance.
- If no improvement in 48–72 hours, reassess the diagnosis (consider viral or fungal etiology).
- Available as 0.3% solution (Ciplox) and 0.3% ointment (Ciplox Eye Ointment).
Sources: MedlinePlus (ciprofloxacin ophthalmic); Drugs.com dosage guide (updated May 2025); Tintinalli's Emergency Medicine
This is a shared conversation. Sign in to Orris to start your own chat.