Physiology of hearing from scott brown 8 th edition
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Finding Sources
Reading File
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Loading Image
Loading Image
I now have all the content needed. Let me compile a comprehensive answer from Cummings Otolaryngology (which covers the same content as Scott Brown's on hearing physiology).
Physiology of Hearing
Source: Cummings Otolaryngology Head and Neck Surgery, Chapter 128 — Physiology of the Auditory System (Wade W. Chien, Daniel J. Lee)
Note: Scott Brown's Otolaryngology (8th edition) is not in the library collection. The content below is drawn from Cummings Otolaryngology Head and Neck Surgery (Chapter 128), which covers identical physiological principles and is the standard ENT reference for auditory physiology.
1. Sound and Its Measurement
Sound is produced by a disturbance in particle density in a medium, triggered by a sound source. When this disturbance travels through an elastic medium, it is perceived as sound. The intensity of sound is measured in decibels (dB):
dB = 20 × log₁₀ (P / Pᵣ)
where P = sound pressure of interest and Pᵣ = reference sound pressure. The most common reference is 20 μPa (sound pressure level, SPL). A 10× increase in pressure = 20 dB; a 100× increase = 40 dB.
2. Impedance
Acoustic impedance is the ratio of acoustic pressure to volume velocity. It has three components:
| Component | Effect at Low Frequency | Effect at High Frequency |
|---|---|---|
| Stiffness | Dominant (varies inversely with frequency) | Minimal |
| Mass | Minimal | Dominant (increases with frequency) |
| Resistance (damping) | Causes energy loss | Causes energy loss |
At resonance, stiffness and mass components cancel each other, and impedance is at its lowest.
3. External Ear
The external ear (pinna + external auditory canal) funnels sound into the ear.
- Concha resonant frequency: ~5300 Hz
- External auditory canal resonant frequency: ~3000 Hz
Sound Localization
Achieved by two mechanisms:
- Interaural time difference (ITD): The farther ear receives the sound later — important for low-frequency localization
- Interaural amplitude difference (IAD): Amplified by the head shadow effect (head attenuates sound to the contralateral ear) — important for high-frequency localization
4. Middle Ear Mechanics
The middle ear consists of the tympanic membrane (TM), ossicular chain (malleus → incus → stapes), and two muscles (stapedius + tensor tympani).
Ossicular Transmission (Air Conduction)
Sound vibrates the TM → malleus → incus → stapes footplate → oval window → inner ear fluids.
Impedance Matching
The middle ear solves the fundamental problem of impedance mismatch between air (low impedance) and cochlear fluid (high impedance). Without the middle ear, ~99.9% of sound energy would be reflected (a 30 dB loss). The middle ear achieves impedance matching by two mechanisms:
- Area ratio: TM area (~60 mm²) >> stapes footplate area (~3.2 mm²) → ~18:1 pressure amplification
- Lever ratio of the ossicles (malleus:incus): ~1.3:1 mechanical advantage
Third Window Concept
Normally, cochlear sound energy is directed through the oval window and dissipated at the round window. A pathological "third window" (e.g., superior canal dehiscence, large vestibular aqueduct) bypasses this path, reducing cochlear impedance and causing conductive hearing loss (air–bone gap) and/or vestibular symptoms.
5. Inner Ear — Cochlear Mechanics
Anatomy
The cochlea has 2¾ turns and contains three fluid-filled chambers:
- Scala vestibuli (perilymph) — communicates with the oval window
- Scala tympani (perilymph) — communicates with the round window
- Scala media / cochlear duct (endolymph, high K⁺) — contains the organ of Corti
The helicotrema connects the scala vestibuli and scala tympani at the apex.
Travelling Wave (von Békésy)
Sound entering the oval window sets up a travelling wave on the basilar membrane that propagates from base to apex. The basilar membrane is:
- Narrow and stiff at the base → responds best to high frequencies
- Wide and compliant at the apex → responds best to low frequencies
This creates tonotopic organization — the basilar membrane acts as a series of frequency filters.
Active Amplification — The Cochlear Amplifier
Passive travelling waves alone cannot account for the exquisite sensitivity and frequency selectivity of human hearing. The outer hair cells (OHCs) provide active amplification:
- OHCs contract with depolarization and elongate with hyperpolarization via the motor protein prestin in their lateral wall
- This electromotility sharpens the tuning curve and amplifies basilar membrane motion by up to 40–60 dB at low sound levels
6. Hair Cell Transduction
Structure
The organ of Corti sits on the basilar membrane and contains:
- Inner hair cells (IHCs): ~3,500; single row; primary sensory cells
- Outer hair cells (OHCs): ~12,000; three rows; amplifier cells
Both have stereocilia arranged in a staircase pattern, connected by tip links.
Mechanoelectrical Transduction
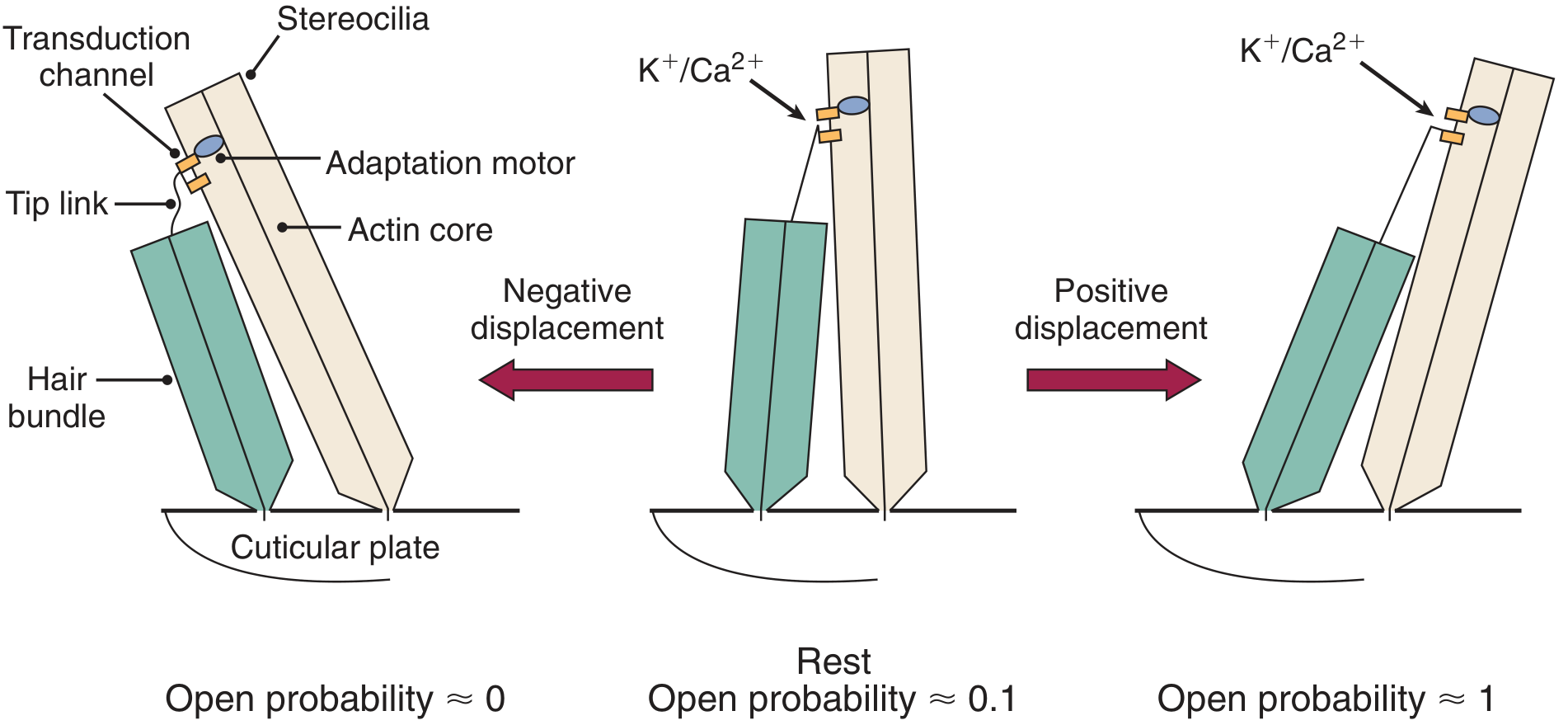
Fig. 128.8 — Role of tip links in hair cell signal transduction (Cummings Otolaryngology)
The endolymph in the scala media has a uniquely high K⁺ concentration and a +80 mV endocochlear potential (maintained by the stria vascularis). The hair cell interior is at ~−45 mV, creating a large driving force of ~125 mV.
Mechanism:
- Basilar membrane displacement → stereocilia deflect toward the tallest row → tip links stretch → mechanically-gated cation channels open
- K⁺ and Ca²⁺ flood into the hair cell → depolarization
- Depolarization triggers Ca²⁺-dependent exocytosis of glutamate at the IHC ribbon synapse → activates type I auditory nerve fibres
- Deflection away from tallest row → tip links relax → channels close → hyperpolarization
IHC vs OHC Function
| Feature | Inner Hair Cells | Outer Hair Cells |
|---|---|---|
| Number | ~3,500 | ~12,000 |
| Innervation | 90–95% of afferent fibres (type I) | Mostly efferent (type II afferents) |
| Role | Sensory transduction | Active amplification (electromotility via prestin) |
| Response | AC + DC receptor potential | Primarily AC |
7. Auditory Nerve and Spiral Ganglion
- Spiral ganglion cells are bipolar first-order neurons — they send peripheral processes to IHCs and central processes to the cochlear nucleus
- Each auditory nerve fibre has a characteristic frequency (CF) — the frequency to which it is most sensitive
- Firing rate increases with sound intensity up to a saturation point
- The auditory nerve carries information about: (a) which fibres fire (place coding), (b) rate of firing, and (c) temporal/phase-locking patterns
8. Central Auditory Pathway
Cochlear Nucleus (Pons)
- First relay station for all ascending auditory information
- Receives input from spiral ganglion via the auditory nerve (CN VIII)
- Three divisions: anteroventral (AVCN), posteroventral (PVCN), dorsal (DCN)
- Sends three fibre tracts: dorsal, intermediate, and ventral acoustic stria → form the lateral lemniscus
- Tonotopic organization preserved
Superior Olivary Complex (SOC)
- Located medial to cochlear nucleus, in caudal pons
- First brainstem nucleus receiving bilateral input
- Key nuclei:
- MSO (Medial Superior Olive): sensitive to interaural time differences (ITD) — low-frequency localization
- LSO (Lateral Superior Olive): sensitive to interaural amplitude differences (IAD) — high-frequency localization; integrates excitatory ipsilateral + inhibitory contralateral inputs
Binaural hearing benefits:
| Mechanism | Description |
|---|---|
| Head shadow effect | Ipsilateral ear closer to signal; contralateral ear in noise |
| Binaural squelch | SOC increases SNR via signal processing |
| Summation | Signal received by both ears is 3 dB louder than monaural |
Lateral Lemniscus
Major ascending fibre tract from cochlear nucleus → inferior colliculus, with branches to SOC and lemniscal nuclei.
Inferior Colliculus (Midbrain)
- Processes frequency information along isofrequency laminae
- Integrates auditory, somatosensory, visual, and vestibular inputs
- Projects to medial geniculate body (~250,000 fibres — ~10× more than auditory nerve, reflecting extensive processing)
Medial Geniculate Body (Thalamus)
- Thalamic relay station
- Three divisions:
- Ventral → primary auditory cortex
- Dorsal → auditory association cortex
- Medial → limbic structures
Auditory Cortex (Temporal Lobe)
- Primary auditory cortex (A1): Heschl's gyrus; Brodmann area 41; tonotopically organized (high frequencies medially, low frequencies laterally); processes complex auditory signals and language
- Auditory association cortex (A2): Brodmann areas 22 and 42; Wernicke's area — critical for speech perception; consonant perception deficits occur with direct electrical interference
- Additional projections to the amygdala (limbic system) explain emotional responses to music
9. Efferent Auditory System
The auditory system has descending feedback pathways that modulate peripheral function:
Middle Ear Muscle Reflex (Stapedius Reflex)
- Loud sounds activate the stapedius muscle (via facial nerve) → stiffens the ossicular chain → reduces low-frequency transmission
- Bilateral reflex (loud sound in one ear causes bilateral stapedius contraction)
- Protects the cochlea from sustained loud sounds (but too slow to protect from sudden noise)
Medial Olivocochlear (MOC) Reflex
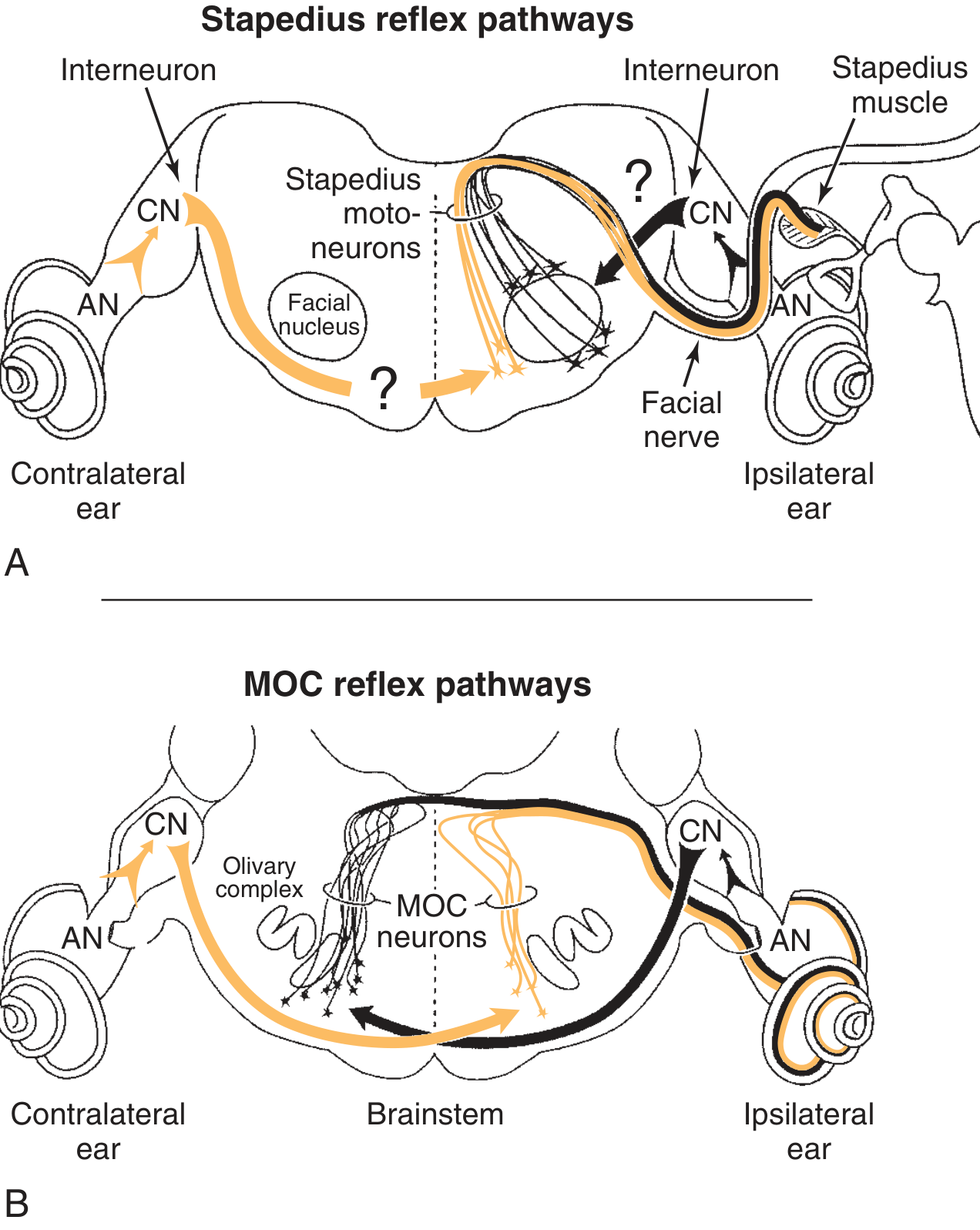
Fig. 128.14 — Auditory efferent pathways showing stapedius and MOC reflex circuits (Cummings Otolaryngology)
- MOC neurons in the SOC send efferent fibres via the vestibular nerve to synapse on OHC lateral walls
- Activation suppresses OHC electromotility → reduces cochlear amplification
- Functions: improves SNR in background noise, protects against noise-induced damage
- Pathway: sound → IHCs → cochlear nucleus (multipolar cells in PVCN) → MOC neurons in contralateral SOC → OHCs of ipsilateral cochlea
Summary: Sound Processing Flow
Sound waves
↓
External ear (pinna + EAC) → directs sound, enables localization
↓
Tympanic membrane vibrates
↓
Ossicular chain (malleus → incus → stapes) → impedance matching (~×30 pressure gain)
↓
Oval window → stapes footplate
↓
Cochlear fluids → travelling wave on basilar membrane (tonotopic)
↓
Organ of Corti → IHC stereocilia deflect → tip links → mechanically-gated channels open
↓
K⁺ influx → hair cell depolarization → glutamate release at ribbon synapse
↓
Auditory nerve (spiral ganglion type I fibres) → action potentials
↓
Cochlear nucleus → Superior olive → Lateral lemniscus → Inferior colliculus
↓
Medial geniculate body (thalamus)
↓
Primary auditory cortex (Heschl's gyrus) → Wernicke's area
Source: Cummings Otolaryngology Head and Neck Surgery, Chapter 128 — Physiology of the Auditory System (Wade W. Chien, Daniel J. Lee)
This is a shared conversation. Sign in to Orris to start your own chat.