Create a clinical case with a diagnosis of acute tubulointerstitial nephritis
Reading File
Checking Date & Time
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Loading Image
Searching Images
acute tubulointerstitial nephritis histology interstitial infiltrate eosinophils
Loading Image
I now have comprehensive material to construct a detailed, clinically rich case. Here it is:
Clinical Case: Acute Tubulointerstitial Nephritis
📋 Clinical Presentation
Patient: 54-year-old woman
Setting: Outpatient nephrology referral
Chief Complaint: "I've been running a low-grade fever for two weeks and my kidneys feel sore."
History of Present Illness:
Mrs. R.M. was started on omeprazole 20 mg daily approximately 3 weeks ago for a new diagnosis of gastroesophageal reflux disease. Ten days after starting the medication, she noticed fatigue, a low-grade fever (38.1 °C), and bilateral flank discomfort. She developed nocturia (3–4 times per night), increased thirst, and noted her urine appeared slightly cloudy. She denies dysuria, urinary frequency, rigors, or recent upper respiratory infection. No recent NSAIDs, antibiotics, or contrast dye exposure. No prior kidney disease.
Past Medical History:
- Hypertension (controlled with amlodipine 5 mg)
- GERD (newly diagnosed, 3 weeks ago)
- No diabetes, no autoimmune disease history
Medications:
- Omeprazole 20 mg PO daily (started 3 weeks ago)
- Amlodipine 5 mg PO daily
Allergies: Sulfonamides (rash)
Social History: Non-smoker, occasional wine, teacher, no occupational exposures.
Review of Systems:
- Mild skin rash on the trunk (maculopapular, appeared 1 week ago)
- No joint pain, no eye symptoms, no dry mouth/eyes
🔬 Physical Examination
| Parameter | Finding |
|---|---|
| Temperature | 38.2 °C |
| Blood pressure | 138/84 mmHg |
| Heart rate | 88 bpm |
| SpO₂ | 98% on room air |
| BMI | 26 kg/m² |
- General: Mildly ill-appearing, alert and oriented ×3
- Skin: Diffuse maculopapular erythematous rash on trunk and upper arms
- Abdomen: Soft, mild bilateral costovertebral angle (CVA) tenderness on deep palpation; no guarding or rebound
- Cardiovascular / Pulmonary: Normal
- Eyes: No redness, no photophobia
🧪 Laboratory Results
Complete Blood Count:
| Test | Result | Reference |
|---|---|---|
| WBC | 9.8 × 10³/µL | 4.5–11 |
| Eosinophils | 12% (absolute: 1.18 × 10³/µL) | < 0.5 × 10³/µL ↑ |
| Hemoglobin | 12.1 g/dL | 12–16 |
| Platelets | 228 × 10³/µL | 150–400 |
Comprehensive Metabolic Panel:
| Test | Result | Reference |
|---|---|---|
| Serum creatinine | 3.1 mg/dL | 0.6–1.1 mg/dL ↑ |
| BUN | 38 mg/dL | 7–20 mg/dL ↑ |
| eGFR (CKD-EPI) | 21 mL/min/1.73m² | > 60 |
| Sodium | 138 mEq/L | 136–145 |
| Potassium | 5.4 mEq/L | 3.5–5.0 ↑ |
| Bicarbonate | 16 mEq/L | 22–29 ↓ |
| Chloride | 112 mEq/L | 98–107 ↑ |
| Calcium | 9.1 mg/dL | 8.5–10.5 |
| Glucose | 94 mg/dL | 70–99 |
Interpretation: Hyperchloremic metabolic acidosis (non-anion gap; AG = 138 − 112 − 16 = 10), consistent with type 4 or distal RTA pattern from tubular dysfunction.
Urinalysis:
| Test | Result |
|---|---|
| Color | Pale yellow, slightly cloudy |
| Specific gravity | 1.008 (↓ — impaired concentrating ability) |
| pH | 6.5 |
| Protein | 1+ (trace, non-nephrotic) |
| Blood | 1+ |
| Leukocyte esterase | 3+ |
| Nitrites | Negative |
| Glucose | Negative |
Urine Microscopy (cytocentrifuged, Giemsa-stained):
- WBC casts present ✓
- Eosinophiluria present (Hansel stain) ✓
- RBCs (non-dysmorphic): 5–10/hpf
- No bacteria
24-hour urine protein: 380 mg/day (mild proteinuria — not nephrotic range)
Urine β₂-microglobulin: Elevated (proximal tubular dysfunction marker)
Urine electrolytes / tubular function:
- Fractional excretion of sodium (FeNa): 3.1% (intrinsic renal, not pre-renal)
- Urine anion gap: positive (impaired NH₄⁺ excretion → distal tubular dysfunction)
Serology (to exclude other causes):
- ANA, Anti-dsDNA: Negative
- ANCA (p and c): Negative
- Complement (C3, C4): Normal
- Serum IgE: Elevated (2.4× upper limit of normal)
- Blood cultures: Negative ×2
- Urine culture: No growth
🔍 Imaging
Renal Ultrasound:
- Bilateral kidneys normal in size (right 11.2 cm, left 11.0 cm)
- Increased echogenicity of renal cortex bilaterally — consistent with interstitial edema and inflammation
- No hydronephrosis, no nephrolithiasis, no masses
- Normal resistive indices on Doppler
🧫 Renal Biopsy
Indication: Unexplained AKI with eGFR < 30 mL/min/1.73m², no improvement at 5 days after drug withdrawal.
Light Microscopy (H&E):
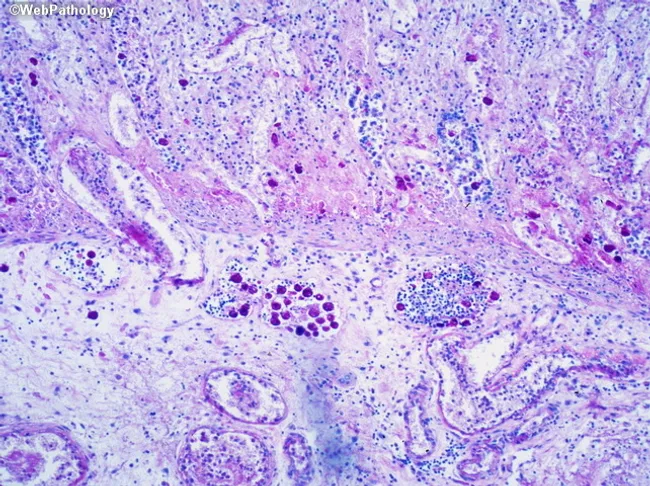
Renal biopsy (H&E): Diffuse interstitial edema with a mixed inflammatory infiltrate — predominantly T lymphocytes and plasma cells with scattered eosinophils. Tubulitis is evident as lymphocytes disrupting tubular epithelium. Glomeruli appear relatively preserved (no proliferative or necrotizing lesions).
Findings:
- Diffuse interstitial edema with mononuclear infiltrate (lymphocytes, macrophages, plasma cells)
- Scattered eosinophils within the interstitium
- Tubulitis: lymphocytes infiltrating tubular epithelium
- Glomeruli: normal (no nephrotic or nephritic pattern)
- No granulomas, no vasculitis, no immune deposits on IF
- Immunofluorescence: Negative for IgG, IgA, IgM, C3, C1q
Conclusion: Acute hypersensitivity tubulointerstitial nephritis — consistent with drug-induced (PPI) etiology.
🩺 Differential Diagnosis
| Diagnosis | Arguments For | Arguments Against |
|---|---|---|
| Acute TIN (drug-induced, PPI) | Temporal relation to omeprazole, eosinophilia, rash, fever, WBC casts, biopsy findings | — |
| Acute pyelonephritis | Pyuria, fever, CVA tenderness | Negative urine/blood culture, no nitrites, biopsy shows no bacteria |
| Acute tubular necrosis (ATN) | AKI, FeNa > 1% | No granular muddy casts, no hemodynamic insult, eosinophiluria, rash |
| ANCA-associated nephritis | AKI, hematuria | ANCA negative, no glomerular lesions on biopsy |
| Lupus nephritis (Class III/IV) | AKI, female patient | ANA/anti-dsDNA negative, no immune deposits on IF |
| Prerenal AKI | Creatinine elevation | FeNa 3.1%, no signs of volume depletion, no response to fluids |
✅ Final Diagnosis
Acute Allergic Tubulointerstitial Nephritis (ATIN) secondary to Omeprazole (proton pump inhibitor)
💊 Management
1. Immediate
- Discontinue omeprazole immediately — withdrawal of the offending agent is the cornerstone of treatment
- Switch GERD management to an H₂-blocker (famotidine) — different class, no cross-reactivity
- IV hydration (NS 0.9%) if volume-depleted; maintain adequate urine output
2. Corticosteroid Therapy
Given biopsy-confirmed ATIN with persistent AKI at 5 days after drug withdrawal:
- Prednisone 1 mg/kg/day (max 60 mg/day) × 4 weeks, then taper over 4 weeks
- Consider methylprednisolone IV pulse if creatinine continues to rise
3. Monitoring
- Daily creatinine and electrolytes during acute phase
- Bicarbonate supplementation for acidosis (target HCO₃⁻ ≥ 20 mEq/L)
- Dietary potassium restriction while hyperkalemia persists
- Monitor blood pressure closely (may worsen transiently with steroids)
- Repeat creatinine at 4, 8, and 12 weeks
4. Outcome Counseling
- Most patients recover with creatinine returning toward baseline over weeks to months
- Older patients and those with delayed diagnosis are at higher risk for incomplete recovery
- Avoid all PPI agents in future; document allergy/adverse drug reaction
📖 Pathophysiology Summary
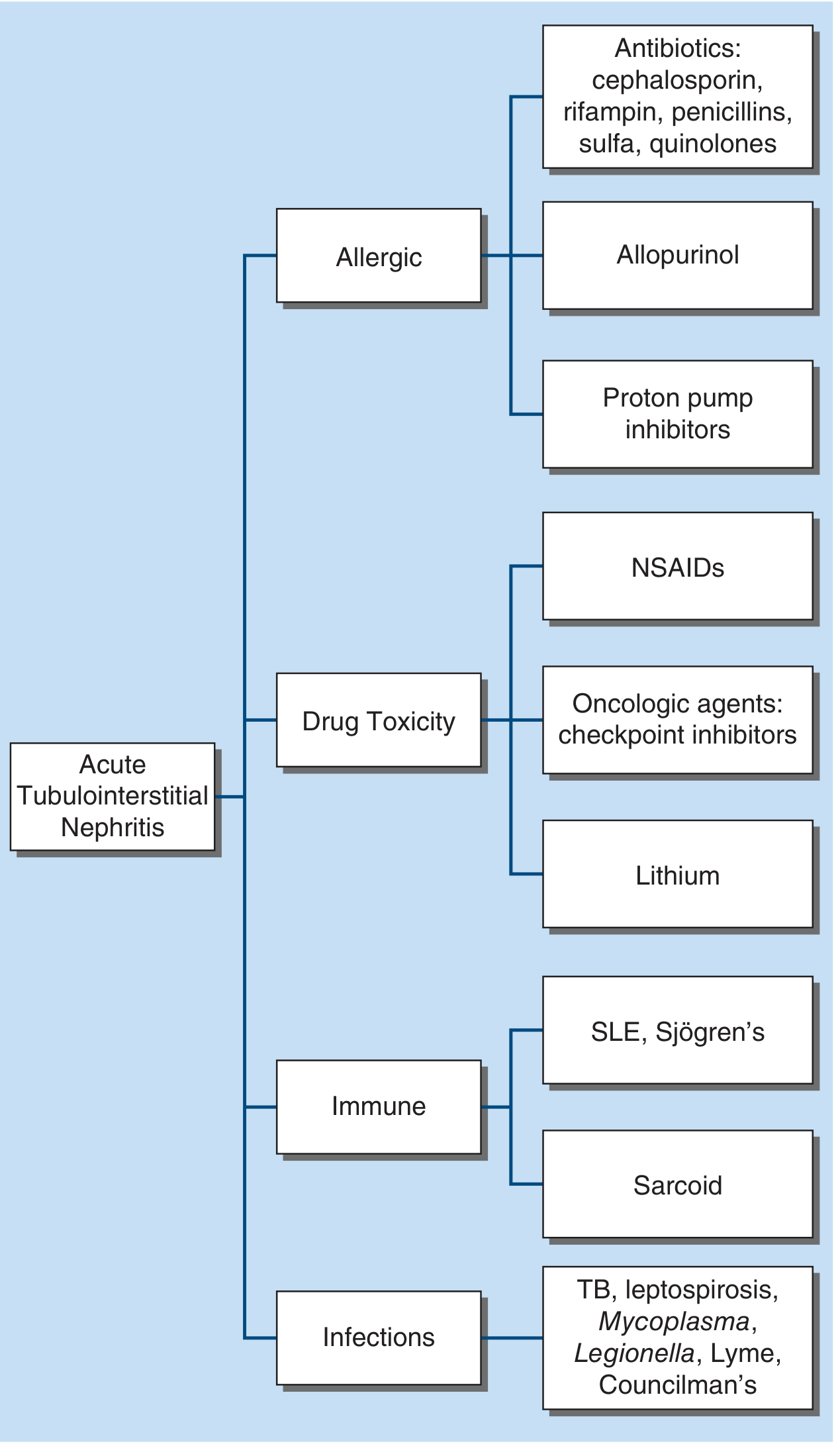
Figure: Etiologic categories of acute tubulointerstitial nephritis (Harrison's Principles of Internal Medicine, 22e).
The mechanism in drug-induced ATIN involves the offending drug being secreted into the tubular lumen, where it covalently binds to tubular cell components, creating immunogenic neoantigens. This triggers both type I (IgE-mediated, explaining eosinophilia and rash) and type IV (T cell-mediated) hypersensitivity reactions. The resultant immune injury causes interstitial edema, inflammatory infiltration, tubular dysfunction, and — if unchecked — tubular atrophy and interstitial fibrosis. — Robbins & Kumar Basic Pathology (Robbins Pathology)
PPIs are now among the most common causes of ATIN, alongside NSAIDs, synthetic penicillins, fluoroquinolones, and cephalosporins. The classic triad of fever + rash + eosinophilia is present in fewer than one-third of cases and is atypical for NSAID- and PPI-induced ATIN specifically — making drug exposure history and biopsy central to diagnosis. — Harrison's Principles of Internal Medicine, 22e
Sources:
- Harrison's Principles of Internal Medicine, 22e (2025), Chapter 319
- Robbins & Kumar Basic Pathology (Robbins Pathology), Chapter 12
- Robbins, Cotran & Kumar Pathologic Basis of Disease, Chapter 20
Create a clinical case with a diagnosis of acute tubulointerstitial nephritis
Checking Date & Time
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Finding Sources
Searching Images
acute tubulointerstitial nephritis kidney biopsy histology lymphocyte infiltrate tubulitis
Reading File
Loading Image
Loading Image
I now have comprehensive source material from multiple authoritative textbooks. Here is the complete clinical case:
Clinical Case: Acute Tubulointerstitial Nephritis (ATIN)
Patient Presentation
Patient: 67-year-old male, retired mechanic
Setting: Emergency Department, referred from primary care
Chief Complaint: Progressive fatigue, decreased urine output, and flank discomfort for 10 days.
History of Present Illness
Mr. J.V. was diagnosed with Helicobacter pylori-associated peptic ulcer disease 4 weeks ago and was started on a triple therapy regimen including omeprazole 40 mg twice daily, amoxicillin, and clarithromycin. He completed the antibiotic course 2 weeks ago but continued on omeprazole. Approximately 12 days ago he noticed progressively worsening fatigue, bilateral flank aching, reduced urine output (no complete anuria), and new-onset nocturia (waking 3–4 times per night). He also reports a low-grade fever at home (~37.9 °C) and a pruritic, blotchy skin rash that appeared on his trunk and arms one week ago.
He denies dysuria, gross hematuria, recent vomiting, diarrhea, or changes in fluid intake. No recent contrast studies or nephrotoxic medications. No prior history of kidney disease.
Past Medical History:
- Hypertension — well controlled on losartan 50 mg/day for 3 years
- Dyslipidemia — rosuvastatin 10 mg/day
- Peptic ulcer disease (new diagnosis, 4 weeks ago)
- No diabetes, no autoimmune disease
Current Medications:
- Losartan 50 mg PO daily
- Rosuvastatin 10 mg PO nightly
- Omeprazole 40 mg PO twice daily (started 4 weeks ago) ← offending agent
- Amoxicillin + clarithromycin (completed 2 weeks ago)
Allergies: Penicillin (rash in childhood — documented)
Social History: Retired, non-smoker, rare alcohol use. No herbal supplements or OTC NSAID use.
Physical Examination
| Parameter | Finding |
|---|---|
| Temperature | 38.3 °C |
| Blood pressure | 148/90 mmHg |
| Heart rate | 94 bpm, regular |
| Respiratory rate | 16/min |
| SpO₂ | 97% on room air |
| Weight | 81 kg |
General: Mildly ill-appearing, fatigued but alert and oriented ×3.
Skin: Diffuse maculopapular, erythematous rash covering the trunk, upper arms, and upper back. Non-vesicular, mildly pruritic.
Abdomen: Soft, non-distended. Bilateral costovertebral angle (CVA) tenderness on firm palpation. No peritoneal signs.
Cardiovascular: Regular rhythm, no murmurs. No signs of volume overload (no peripheral edema, no raised JVP).
Eyes: Clear, no conjunctival injection, no photophobia.
Lymph nodes: No lymphadenopathy.
Diagnostic Workup
Complete Blood Count
| Test | Result | Reference Range |
|---|---|---|
| WBC | 10.2 × 10³/µL | 4.5–11.0 |
| Eosinophils | 14% → 1.43 × 10³/µL | < 0.5 × 10³/µL ↑ |
| Hemoglobin | 11.8 g/dL | 13.5–17.5 ↓ (mild normocytic anemia) |
| MCV | 87 fL | 80–100 |
| Platelets | 214 × 10³/µL | 150–400 |
Comprehensive Metabolic Panel
| Test | Result | Reference Range |
|---|---|---|
| Serum Creatinine | 4.2 mg/dL | 0.7–1.3 mg/dL ↑↑ |
| BUN | 52 mg/dL | 7–20 mg/dL ↑↑ |
| eGFR (CKD-EPI) | 14 mL/min/1.73 m² | >60 |
| BUN/Creatinine ratio | 12.4 | (intrinsic renal pattern, not prerenal) |
| Sodium | 136 mEq/L | 136–145 |
| Potassium | 5.6 mEq/L | 3.5–5.0 ↑ |
| Bicarbonate | 14 mEq/L | 22–29 ↓ |
| Chloride | 110 mEq/L | 98–107 ↑ |
| Anion gap | 136 − 110 − 14 = 12 mEq/L | (normal AG → hyperchloremic metabolic acidosis) |
| Calcium | 9.3 mg/dL | 8.5–10.5 |
| Phosphorus | 5.8 mg/dL | 2.5–4.5 ↑ |
| Albumin | 3.6 g/dL | 3.5–5.0 |
| Total bilirubin | 0.7 mg/dL | Normal |
| AST/ALT | Normal |
Acid-base interpretation: Hyperchloremic, normal anion gap metabolic acidosis — consistent with impaired tubular H⁺ secretion (distal RTA pattern) and/or reduced ammoniagenesis due to tubular dysfunction.
Urinalysis
| Test | Result |
|---|---|
| Color | Pale yellow, cloudy |
| Specific gravity | 1.007 (↓ — impaired urinary concentrating ability) |
| pH | 6.5 |
| Protein | 2+ |
| Blood | 1+ |
| Leukocyte esterase | 3+ |
| Nitrites | Negative |
| Glucose | Negative (no glucosuria despite AKI) |
Urine Microscopy (Giemsa-stained cytocentrifuged preparation)
| Finding | Result |
|---|---|
| WBC casts | Present ✓ |
| Eosinophiluria (Hansel stain) | Present ✓ |
| Non-dysmorphic RBCs | 8–12/hpf |
| Renal tubular epithelial cells | Present |
| Bacteria | Absent |
| Granular (muddy) casts | Absent |
Additional Urine Studies
| Test | Result | Interpretation |
|---|---|---|
| Spot urine protein/creatinine ratio | 0.8 g/g | Moderate proteinuria — subnephrotic |
| Urine β₂-microglobulin | Elevated | Proximal tubular dysfunction |
| FeNa | 2.8% | Intrinsic renal injury (not prerenal) |
| Urine anion gap | Positive (+12 mEq/L) | Impaired NH₄⁺ excretion — distal tubular dysfunction |
| Urine culture | No growth |
Serologic Workup (to exclude secondary causes)
| Test | Result |
|---|---|
| ANA | Negative |
| Anti-dsDNA | Negative |
| ANCA (c-ANCA, p-ANCA) | Negative |
| Anti-GBM antibody | Negative |
| Complement (C3, C4) | Normal |
| Serum IgE | Elevated (3× upper limit of normal) |
| Serum protein electrophoresis | No monoclonal band |
| HIV, Hepatitis B surface antigen, Anti-HCV | Negative |
| Blood cultures ×2 | Negative |
Imaging
Renal Ultrasound
- Right kidney: 11.4 cm | Left kidney: 11.1 cm (mildly enlarged, consistent with edema)
- Increased bilateral cortical echogenicity — reflects interstitial inflammation and edema
- No hydronephrosis, no nephrolithiasis, no renal masses
- Normal Doppler waveforms; resistive index mildly elevated (0.74)
Ultrasound findings are neither sensitive nor specific for ATIN but help exclude obstruction and structural causes. Renal volume can increase up to 100% in ATIN due to interstitial edema and inflammatory infiltration. — Brenner and Rector's The Kidney
Renal Biopsy
Indication: Unexplained AKI with eGFR 14 mL/min/1.73 m², no spontaneous improvement at 5 days after drug withdrawal, biopsy needed to confirm diagnosis and guide steroid therapy.
Light Microscopy (H&E stain)

Renal biopsy (H&E stain): Diffuse interstitial edema with a mononuclear inflammatory infiltrate comprising T lymphocytes, plasma cells, and macrophages, with scattered eosinophils. Tubulitis is evident as lymphocytes infiltrating tubular epithelium. Glomeruli appear relatively preserved with no proliferative or necrotizing lesions.
Histologic Findings Summary
| Compartment | Finding |
|---|---|
| Interstitium | Diffuse edema; dense mononuclear infiltrate (lymphocytes, macrophages, plasma cells) |
| Eosinophils | Scattered within interstitium ✓ |
| Tubulitis | Lymphocytes breaching and disrupting tubular epithelium ✓ |
| Glomeruli | Normal — no crescents, no endocapillary proliferation, no necrosis |
| Vessels | No vasculitis |
| Granulomas | Absent |
Immunofluorescence
- Negative for IgG, IgA, IgM, C3, C1q, fibrin — no immune complex deposits
Electron Microscopy
- No dense deposits
- Foot process effacement absent (no concurrent minimal change disease)
Histologic hallmarks of ATIN: interstitial inflammatory cellular infiltrate, variable tubular injury, interstitial edema, and tubulitis. — Brenner and Rector's The Kidney
Etiology Classification

Figure 319-2: Etiologic categories of acute tubulointerstitial nephritis. — Harrison's Principles of Internal Medicine, 22e
Differential Diagnosis
| Diagnosis | Evidence For | Evidence Against |
|---|---|---|
| ATIN — drug-induced (omeprazole/clarithromycin) ✓ | Temporal drug exposure, fever, rash, eosinophilia, WBC casts, eosinophiluria, biopsy findings, elevated IgE | — |
| Acute pyelonephritis | Fever, pyuria, CVA tenderness | Negative urine/blood cultures, no nitrites, no bacteria on microscopy, biopsy non-purulent |
| Acute tubular necrosis (ATN) | AKI, FeNa > 1% | No hemodynamic insult, no granular casts, eosinophiluria and rash present, biopsy shows mononuclear infiltrate not tubular necrosis |
| ANCA-associated interstitial nephritis | AKI, hematuria | ANCA negative, no glomerular crescents on biopsy |
| Lupus nephritis | AKI, female excluded but considered | ANA/anti-dsDNA negative, no immune deposits on IF, complement normal |
| Multiple myeloma / cast nephropathy | Elderly male, AKI | Normal SPEP, no monoclonal casts on biopsy |
| Prerenal AKI | Reduced urine output | FeNa 2.8%, BUN/Cr ratio 12.4, no volume depletion on exam |
Diagnosis
Acute Allergic Tubulointerstitial Nephritis (ATIN), drug-induced — most likely attributable to omeprazole (proton pump inhibitor)
The clinical triad of fever, rash, and eosinophilia — present in this patient — occurs in only approximately 5–10% of unselected ATIN cases and should not be relied upon as a required criterion. Most patients present with subacute kidney function decline with or without this triad. — Brenner and Rector's The Kidney
Pathophysiology
Drugs secreted into the tubular lumen can covalently bind to tubular cell cytoplasmic or extracellular components, creating immunogenic neoantigens. The resultant immune injury is mediated by:
- Type I hypersensitivity (IgE-mediated): explains eosinophilia, elevated serum IgE, and skin rash
- Type IV hypersensitivity (T cell–mediated): drives the mononuclear interstitial infiltrate, tubulitis, and tubular injury
The idiosyncratic nature of the reaction (not dose-dependent), the latent period of 1–4 weeks from exposure, and recurrence on re-exposure are hallmarks of an immune-mediated mechanism. — Robbins & Kumar Basic Pathology
Management
Step 1 — Remove the Offending Agent (Immediate)
- Discontinue omeprazole immediately. Drug withdrawal is the cornerstone of treatment and can be sufficient for mild cases.
- Switch acid suppression to famotidine (H₂-blocker) — different drug class, no cross-reactivity with PPI-induced ATIN.
- Document omeprazole (and class) as an adverse drug reaction in the medical record.
Step 2 — Corticosteroid Therapy
Given persistent AKI (eGFR 14 mL/min/1.73 m²) and biopsy confirmation with no spontaneous improvement at 5 days:
- Prednisone 1 mg/kg/day (max 60 mg/day) orally for 4 weeks
- Taper over an additional 4 weeks (total 8-week course)
- Corticosteroids are supported by immunologic rationale and observational data; the extensive T-cell inflammatory infiltrate on biopsy is the basis for immunosuppressive therapy — Brenner and Rector's The Kidney
Step 3 — Supportive Care
| Problem | Intervention |
|---|---|
| Hyperkalemia (K⁺ 5.6 mEq/L) | Low-potassium diet; patiromer or kayexalate if persistent |
| Metabolic acidosis (HCO₃⁻ 14) | Oral sodium bicarbonate supplementation (target HCO₃⁻ ≥ 20) |
| Hypertension (148/90 on losartan) | Continue losartan with close monitoring of K⁺ and creatinine |
| Hyperphosphatemia | Dietary phosphate restriction; consider binder if persistent |
| Volume status | Careful IV NS if clinically hypovolemic; avoid overhydration |
Step 4 — Monitoring and Follow-up
- Daily creatinine, electrolytes, and urine output during acute hospitalization
- Weekly creatinine for 4 weeks after discharge
- Creatinine targets: return toward baseline within 4–12 weeks in responsive patients
- Ophthalmology referral not needed in this case (no ocular symptoms), but note: bilateral red eyes + AKI should prompt evaluation for TINU syndrome (tubulointerstitial nephritis and uveitis)
- Avoid all PPI agents permanently; document allergy/ADR
Prognosis
Most patients with drug-induced ATIN recover kidney function following drug withdrawal, though recovery may take several months. Older patients and those with delayed diagnosis carry higher risk of incomplete recovery. Persistent tubular dysfunction (impaired concentrating ability, tubular acidosis) may outlast the acute phase. — Harrison's Principles of Internal Medicine, 22e; Robbins & Kumar Basic Pathology
Teaching Points
- The classic triad (fever + rash + eosinophilia) is present in fewer than 10% of ATIN cases — its absence does not exclude the diagnosis.
- PPIs are now among the most common causes of drug-induced ATIN, alongside NSAIDs, synthetic penicillins, fluoroquinolones, and cephalosporins.
- WBC casts and eosinophiluria on urine microscopy are highly suggestive; a cytocentrifuged, Giemsa-stained preparation optimally demonstrates T lymphocytes, eosinophils, and plasma cells.
- Kidney biopsy is the gold standard for diagnosis and guides the decision to initiate corticosteroids.
- FeNa > 1% in the setting of oliguria points to intrinsic renal injury (not prerenal), narrowing the differential.
- Hyperchloremic normal anion gap metabolic acidosis reflects tubular dysfunction (impaired H⁺/NH₄⁺ secretion) — a key distinguishing feature from glomerular disease.
- Immunofluorescence negative distinguishes ATIN from immune complex glomerulonephritis.
Sources:
- Harrison's Principles of Internal Medicine, 22e (2025), Chapter 319
- Brenner and Rector's The Kidney, Chapter 35
- Robbins & Kumar Basic Pathology, Chapter 12
Make a little shorter and leave the references in this and sources
Here is the condensed version of the clinical case:
Clinical Case: Acute Tubulointerstitial Nephritis (ATIN)
Patient Presentation
Patient: 67-year-old male, retired mechanic
Setting: Emergency Department
Chief Complaint: Progressive fatigue, decreased urine output, and bilateral flank discomfort for 10 days.
History of Present Illness
Mr. J.V. was diagnosed with H. pylori-associated peptic ulcer disease 4 weeks ago and started on triple therapy (omeprazole 40 mg twice daily, amoxicillin, clarithromycin). He completed antibiotics 2 weeks ago but continued omeprazole. Twelve days ago he developed fatigue, bilateral flank aching, reduced urine output, nocturia (3–4×/night), low-grade fever (~37.9 °C), and a pruritic maculopapular rash on the trunk and arms.
He denies dysuria, gross hematuria, recent NSAID use, or prior kidney disease.
Medications:
- Losartan 50 mg/day (hypertension, 3 years)
- Rosuvastatin 10 mg/night
- Omeprazole 40 mg PO twice daily — started 4 weeks ago ← offending agent
Allergies: Penicillin (childhood rash)
Physical Examination
| Parameter | Finding |
|---|---|
| Temperature | 38.3 °C |
| Blood pressure | 148/90 mmHg |
| Heart rate | 94 bpm |
| SpO₂ | 97% room air |
- Skin: Diffuse maculopapular erythematous rash — trunk and upper arms
- Abdomen: Soft; bilateral CVA tenderness on deep palpation
- Eyes: Clear; no photophobia or conjunctival injection
Laboratory Results
Complete Blood Count
| Test | Result | Reference |
|---|---|---|
| WBC | 10.2 × 10³/µL | 4.5–11.0 |
| Eosinophils | 14% → 1.43 × 10³/µL | < 0.5 ↑ |
| Hemoglobin | 11.8 g/dL | 13.5–17.5 ↓ |
Metabolic Panel
| Test | Result | Reference |
|---|---|---|
| Serum Creatinine | 4.2 mg/dL | 0.7–1.3 ↑↑ |
| BUN | 52 mg/dL | 7–20 ↑↑ |
| eGFR | 14 mL/min/1.73 m² | >60 |
| Potassium | 5.6 mEq/L | 3.5–5.0 ↑ |
| Bicarbonate | 14 mEq/L | 22–29 ↓ |
| Chloride | 110 mEq/L | 98–107 ↑ |
| Anion gap | 12 mEq/L | (normal) |
Hyperchloremic normal anion gap metabolic acidosis → reflects distal tubular dysfunction (impaired H⁺/NH₄⁺ secretion).
Urinalysis & Urine Microscopy
| Test | Result |
|---|---|
| Specific gravity | 1.007 ↓ (impaired concentrating ability) |
| Protein | 2+ |
| Leukocyte esterase | 3+ |
| Nitrites | Negative |
| WBC casts | Present ✓ |
| Eosinophiluria (Hansel stain) | Present ✓ |
| Bacteria | Absent |
| Urine culture | No growth |
A cytocentrifuged, Giemsa-stained urine preparation best demonstrates T lymphocytes, eosinophils, and plasma cells — the most characteristic cell types in ATIN. — Harrison's Principles of Internal Medicine, 22e
FeNa: 2.8% (intrinsic renal injury, not prerenal) | Urine β₂-microglobulin: elevated (proximal tubular dysfunction)
Serology
ANA, anti-dsDNA, ANCA, anti-GBM — all negative. Complement normal. Serum IgE elevated (3× ULN). Blood cultures ×2 negative.
Imaging — Renal Ultrasound
- Bilateral kidneys mildly enlarged (right 11.4 cm, left 11.1 cm)
- Increased cortical echogenicity bilaterally — consistent with interstitial edema
- No hydronephrosis, no stones, no masses
Renal volume can increase up to 100% in ATIN due to inflammatory infiltration and interstitial edema; imaging findings are not specific but exclude obstruction. — Brenner and Rector's The Kidney
Renal Biopsy
Indication: Confirmed AKI with eGFR 14 mL/min/1.73 m²; no spontaneous improvement at 5 days after drug withdrawal.
Histology (H&E)

| Compartment | Finding |
|---|---|
| Interstitium | Diffuse edema; dense infiltrate of lymphocytes, macrophages, plasma cells |
| Eosinophils | Scattered within interstitium ✓ |
| Tubulitis | Lymphocytes infiltrating and disrupting tubular epithelium ✓ |
| Glomeruli | Normal — no crescents, no necrosis |
| Immunofluorescence | Negative (IgG, IgA, IgM, C3, C1q) |
ATIN is characterized by interstitial inflammatory infiltrate, variable tubular injury, interstitial edema, and tubulitis. — Brenner and Rector's The Kidney
Differential Diagnosis
| Diagnosis | For | Against |
|---|---|---|
| Drug-induced ATIN (omeprazole) ✓ | Drug exposure, fever, rash, eosinophilia, WBC casts, biopsy | — |
| Acute pyelonephritis | Fever, pyuria, CVA tenderness | Negative cultures, no bacteria on biopsy |
| Acute tubular necrosis | AKI, FeNa > 1% | No hemodynamic insult, no granular casts, eosinophiluria present |
| ANCA-associated nephritis | AKI, hematuria | ANCA negative, no crescents on biopsy |
| Prerenal AKI | Oliguria | FeNa 2.8%, no volume depletion |
Diagnosis
Acute Allergic Tubulointerstitial Nephritis — drug-induced, attributed to omeprazole (proton pump inhibitor)
The classic triad of fever + rash + eosinophilia occurs in only 5–10% of unselected ATIN cases and should not be required for diagnosis. — Brenner and Rector's The Kidney
Pathophysiology
Omeprazole is secreted into the tubular lumen, where it covalently binds to tubular cell components creating immunogenic neoantigens. Resultant injury involves:
- Type I (IgE-mediated): eosinophilia, elevated IgE, skin rash
- Type IV (T cell–mediated): mononuclear interstitial infiltrate and tubulitis
The reaction is idiosyncratic (not dose-dependent), with a latent period of 1–4 weeks from exposure. — Robbins & Kumar Basic Pathology

Figure 319-2: Etiologic categories of acute tubulointerstitial nephritis. — Harrison's Principles of Internal Medicine, 22e
Management
1. Remove the offending agent — Discontinue omeprazole immediately. Switch to famotidine (H₂-blocker, no cross-reactivity). Document as ADR.
2. Corticosteroids — Given biopsy-confirmed ATIN with no improvement at 5 days after withdrawal:
- Prednisone 1 mg/kg/day (max 60 mg/day) × 4 weeks, then taper over 4 weeks
- Rationale: the extensive T-cell interstitial infiltrate supports immunosuppressive therapy — Brenner and Rector's The Kidney
3. Supportive care:
| Problem | Intervention |
|---|---|
| Hyperkalemia (K⁺ 5.6) | Low-K⁺ diet; patiromer if persistent |
| Metabolic acidosis (HCO₃⁻ 14) | Oral sodium bicarbonate (target ≥ 20 mEq/L) |
| Hyperphosphatemia | Dietary restriction; phosphate binder if needed |
| Hypertension | Continue losartan; monitor K⁺ closely |
4. Monitoring: Daily creatinine/electrolytes during admission; weekly creatinine for 4 weeks post-discharge. Most patients recover kidney function following drug withdrawal, though recovery may take several months. Older patients and those with delayed diagnosis are at higher risk for incomplete recovery. — Harrison's Principles of Internal Medicine, 22e; Robbins & Kumar Basic Pathology
Key Teaching Points
- The classic triad (fever + rash + eosinophilia) is present in < 10% of ATIN cases — do not rely on it.
- PPIs are among the most common causes of drug-induced ATIN today.
- WBC casts + eosinophiluria on cytocentrifuged Giemsa-stained urine are the most suggestive urinary findings.
- Normal anion gap metabolic acidosis signals tubular dysfunction, distinguishing ATIN from glomerular disease.
- Negative IF on biopsy excludes immune complex glomerulonephritis.
- Kidney biopsy is the gold standard and guides the decision to initiate corticosteroids.
Sources:
- Harrison's Principles of Internal Medicine, 22e (2025), Chapter 319
- Brenner and Rector's The Kidney, Chapter 35
- Robbins & Kumar Basic Pathology, Chapter 12
Can you make a pptx
Checking Date & Time
Reading File
Reading File
Reading File
Reading File
Running Command
Running Command
Running Command
Writing File
Running Command
Running Command
Editing File
Running Command
The presentation was built successfully. Here it is:
Acute Tubulointerstitial Nephritis
Presentation · PPTX
The presentation contains 12 slides with a dark navy + teal clinical theme:
| # | Slide |
|---|---|
| 1 | Title Slide — Clinical case cover |
| 2 | Patient Presentation — Demographics, HPI, medications (offending drug highlighted) |
| 3 | Physical Examination — Vital signs cards + findings |
| 4 | Laboratory Results — CBC & Metabolic Panel with color-coded abnormal values |
| 5 | Urinalysis & Tubular Function — WBC casts, eosinophiluria, FeNa, β₂-microglobulin, serology |
| 6 | Imaging — Renal ultrasound findings |
| 7 | Renal Biopsy — Embedded H&E histology image + findings table |
| 8 | Etiology & Final Diagnosis — Embedded etiology diagram from Harrison's + diagnosis callout |
| 9 | Differential Diagnosis — Table with evidence for/against each dx |
| 10 | Pathophysiology — 5-step mechanism (tubular secretion → neoantigen → Type I/IV hypersensitivity → tubular dysfunction) |
| 11 | Management — Drug withdrawal → corticosteroids → supportive care → prognosis |
| 12 | Key Teaching Points — 6 numbered highlights |
This is a shared conversation. Sign in to Orris to start your own chat.